 |
 |
 |
| |
MILD NAFLD IS COMMON IN SEVERELY OBESE ADOLESCENTS
AND IMPROVES SIGNIFICANTLY FOLLOWING BARIATRIC SURGERY
|
| |
| |
AASLD 2021 Nov 12-15
Miriam Ben Abdallah1, Thomas H Inge2, Emily Cooper3, Kristen Nadeau4, Megan Kelsey4, Kaci Pickett3 and Shikha S. Sundaram5,6, (1)Pediatrics, Children's Hospital Colorado, (2) Surgery, Children's Hospital Colorado, (3)Center for Research in Outcomes for Children's Surgery, University of Colorado School of Medicine, (4)Children's Hospital Colorado, (5) Digestive Health Institute, Children's Hospital Colorado, (6)Section of Gastroenterology, Hepatology and Nutrition, Department of Pediatrics and the Digestive Health Institute, Children's Hospital of Colorado and University of Colorado School of Medicine
Background: Non-alcoholic fatty liver disease (NAFLD) is a common co-morbidity of pediatric obesity. Little is known about the response of NAFLD to metabolic bariatric surgery (MBS) in severely obese adolescents.
Objectives: To examine prevalence/severity of NAFLD longitudinally in severely obese adolescents before and after MBS. Methods: Retrospective study of adolescents who underwent MBS between November 2017 and April 2020, with at least 12 months of follow up. All had a liver biopsy during MBS.
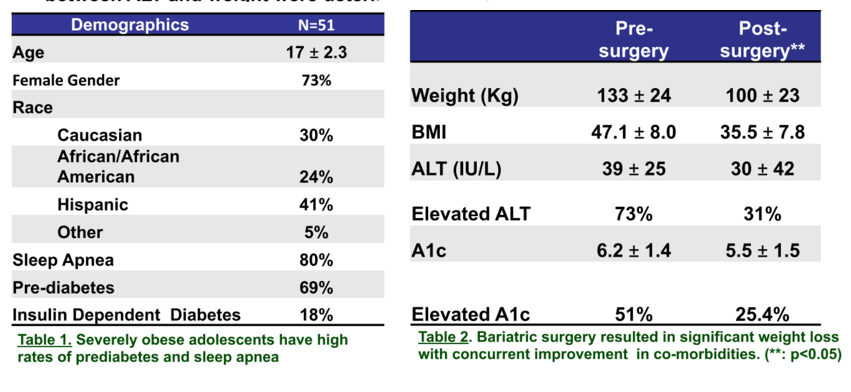
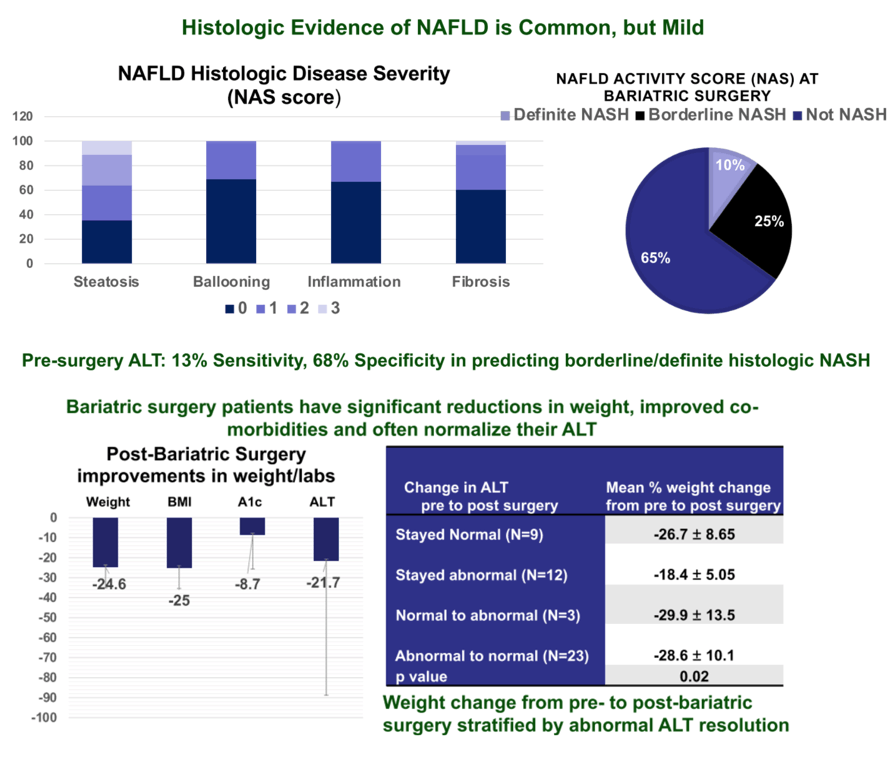
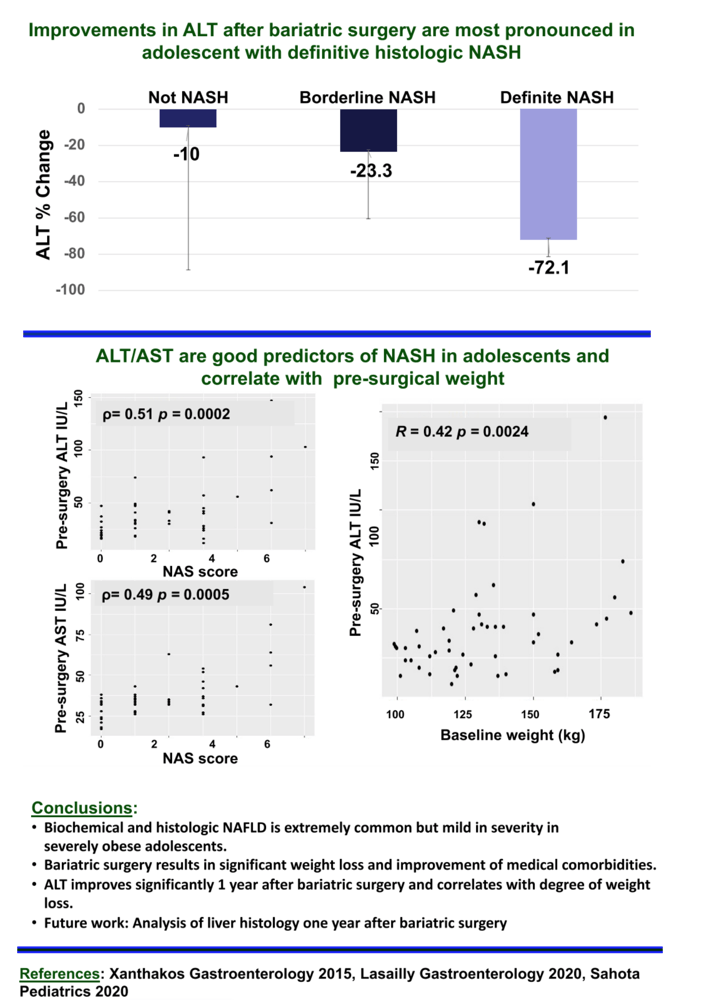
Results: 51 adolescents (mean age 17 ± 2.3 years, 73% female, 41% Hispanic, 30% Caucasian, 24% African American) underwent MBS (98% vertical sleeve gastrectomy). Mean (±SD) pre-surgical weight was 133 ± 24.1 kg (range 99-186) and BMI was 47.1 ± 8.0 kg/m2. Mean pre-surgical ALT was 39 ± 25 IU/L (range 12-147), which correlated with weight (Ρ:=0.42, 95% CI: 0.14- 0.62; p= 0.002). An elevated ALT occurred in 73% of subjects (≥ 26 in males; ≥ 22 IU/L in females). The mean NAS score at baseline was 1.8 ± 1.7, with 10% definite NASH (NAS ≥ 5), 25% borderline NASH (NAS 3-4) and the majority (65%) without NASH (NAS 0-2). Most (60%) had no hepatic fibrosis, 38% with stage 1-2 and 2% stage 3 hepatic fibrosis. The sensitivity of an abnormal ALT in predicting borderline/definite histologic NASH was 13% and the specificity was 68%. However, a strong relationship was found between histologic disease severity (NAS score) and pre-surgical ALT (Ρ:=0.5, 95% CI: 0.25-0.70;p=0.0002). Following MBS, mean BMI decreased to 35.5 ± 7.8 kg/m2 (a 23 ± 10.4% reduction). Mean ALT decreased to 30 ± 42 IU/L (a 21.7 ± 67.1%) reduction. In addition, following MBS, ALT remained elevated in only 33% of subjects. Greater weight loss (28.6 ± 10.1%) was seen in those in whom an abnormal ALT reverted to normal after bariatric surgery compared to 18.4 ± 5.0% weight loss in those whose ALT remained abnormal (p=0.003). The largest % ALT decrease (72 ± 9%) occurred in those with definite NASH at baseline as compared to borderline NASH (23 ± 37%) and not NASH (10 ± 78%) following MBS (p=0.009).
Conclusion: Biochemical and histologic NAFLD is extremely common but mild in severity in severely obese adolescents. ALT improves significantly after bariatric surgery and correlates with degree of weight loss. Liver histology is also likely to improve or normalize with this treatment option. Future directions include analysis of follow-up liver biopsy data to confirm these findings.




|
| |
|
 |
 |
|
|