 |
 |
 |
| |
SIMULTANEOUS HEPATITIS B AND C SCREENING IN AN
EMERGENCY DEPARTMENT: A BROAD LINKAGE TO CARE STRATEGY
|
| |
| |

AASLD 2021 Nov 12-15
Jordi Llaneras1,2, Ana Barreira-Diaz1, Ariadna Rando3, Juan Bañares1, Beatriz Meza2, Lourdes Ruíz2, Joana-Rita Marques2, Arnau Monforte2, Olimpia Orozco2, Mar Riveiro Barciela1,4, Fernando Velasquez5, Francisco Rodríguez-Frías6, María Arranz2, Rafael Esteban-Mur1,4 and Maria Buti1,4, (1)Liver Unit, Internal Medicine Department, Hospital Universitari Vall D'hebron, Barcelona, Spain, (2)Emergency Department, Hospital Vall D'hebron, (3)Vall D'hebron Institut De Recerca (VHIR). Barcelona, Spain, (4)Centro De Investigación Biomédica En Red, Enfermedades Hepáticas y Digestvas (CIBERehd), Instituto De Salud Carlos III, Madrid, Spain, (5)Virology Unit, Microbiology Department, Hospital Universitari Vall D'hebron, (6)Liver Pathology Unit, Biochemistry and Microbiology Departments, Hospital Universitari Vall d'Hebron, Barcelona, Spain
Background: The estimated current prevalence of viral hepatitis in Spain is 0.2-1.69% for hepatitis B virus (HBV) and 0.22% for hepatitis C virus (HCV). There are still a significant percentage of people with hepatitis B and C virus who are unaware of their infection, especially among the vulnerable population with scarce contact with the health system. The emergency department (ED) is the access point to the health system for the majority of this vulnerable population not linked to formal care. The aim of the study was to perform a universal screening for HBV and HCV infection at the ED and link positive cases to care.
Methods: Prospective, single-centre study in an academic hospital involving screening and linkage to care of hepatitis B and C cases. Simultaneous HBsAg and anti-HCV antibodies were performed in individuals >16 years who require phlebotomy for medical reasons. Reflex viral load was performed in all anti-HCV+ patients and hepatitis D antibodies in HBsAg+ patients. Patient characteristics were analyzed in relation to HBV and HCV infection and linkage to care.
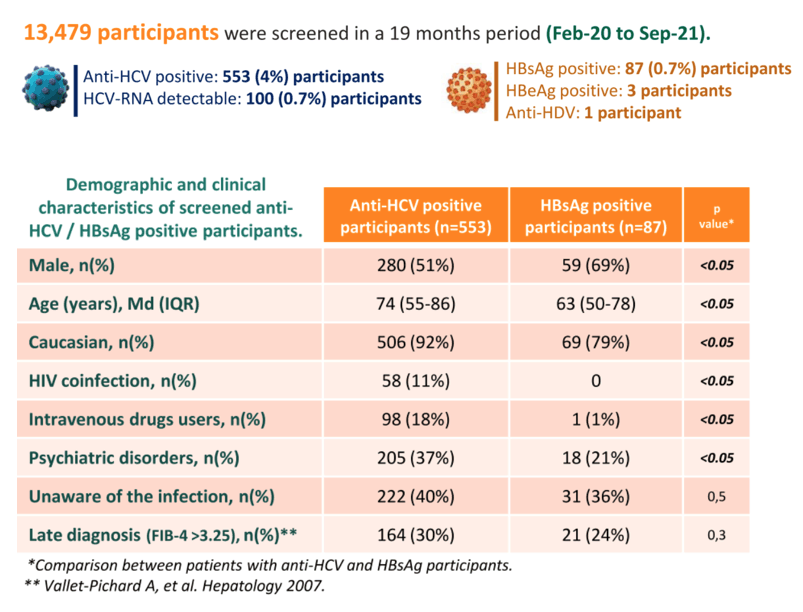
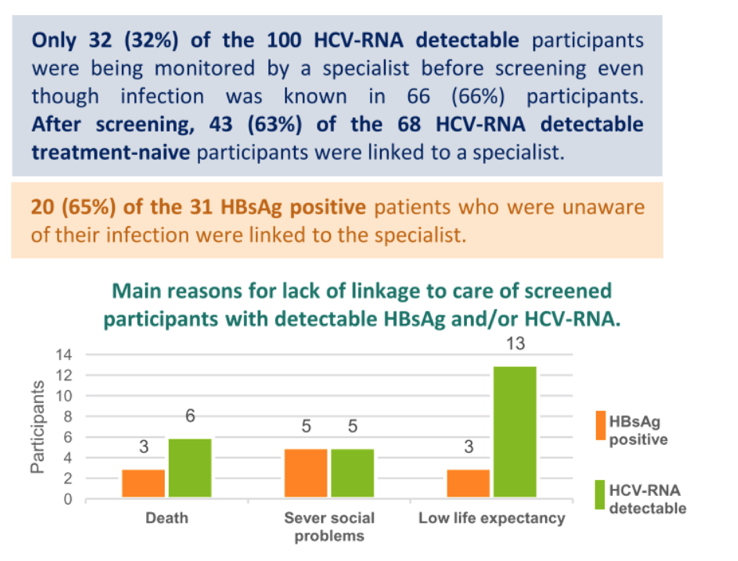
Results: 7,259 patients were screened in a one-year period (Feb-20 to Feb-21) in the ED. HBsAg was detected in 43 (0.6%) subjects, and anti-HCV in 293 (4%), 51 (0.7%) of them had detectable HCV-RNA. HBsAg+ patients were younger (median age 64) and mainly males (67%) than anti-HCV+ subjects (median age 72, 50% male). 81% and 95% of HBsAg and anti-HCV individuals were Caucasian. 35% of HBsAg+, 40% of anti-HCV+ and 27% of HCV-RNA+ patients were unaware of the infection. Risk factors for HBV were observed in<5% of HBsAg+ patients while roughly 85% of anti-HCV+ had some associated risk factor, with the most frequent being HIV co-infection, substance use (alcohol and intravenous drugs) and psychiatric disorders. A case of HBV and HCV co-infection was detected but no cases of hepatitis D. 22 (51%) patients with known HBV were already linked. 10/43 (23%) HBsAg+ patients and 22/51 (43%) HCV-RNA+ patients were linked to a specialist. Main reasons for the lack of linkage were severe cognitive impairment, low life expectancy or severe social problems.
Conclusion: Simultaneous testing of hepatitis B and C infection showed a prevalence of HBV of 0.6% and active HCV infection of 0.7%, almost three times higher than that reported in the general population. Screening for HBV and HCV infection in emergency departments can be a useful strategy to identify patients with unknown viral hepatitis and ensure appropriate management.

|
| |
|
 |
 |
|
|