 |
 |
 |
| |
HBV Nuc Withdrawal -Cautionary Study Results at AASLD 2021
|
| |
| |
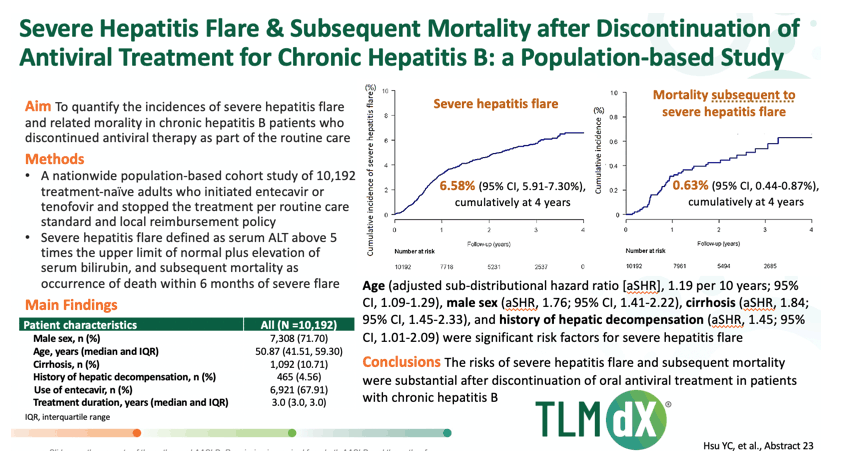
AASLD: Severe Hepatitis Flare and Subsequent Mortality after Discontinuation of Oral Antiviral Treatment in Patients with Chronic Hepatitis B: a Population-based Study- (11/15/21)
AASLD: Nucleos(t)ide analogue withdrawal in chronic hepatitis B patients leads to limited sustained remission in the absence of HBsAg loss: Results from the RETRACT-B study Response after End of Treatment with Antivirals in Chronic Hepatitis B (RETRACT-B Study) - (11/13/21)
------------------------------------
SEVERE ACUTE EXACERBATION AFTER CESSATION OF NUCLEOS(T)IDE ANALOGS FOR CHRONIC HEPATITIS B: A
REAL-WORLD STUDY OF ROUTINE PRACTICE
AASLD 2021 Nov 12-15
Jia-Ling Wu1, Cheng-Hao Tseng2,3, Mindie H. Nguyen4,5, Tzu-Haw Chen6, Ying-Nan Tsai3, Chih Wen Lin2,7, Yi-Chun Tsai8, Chih-Lung Hung9, Chun-Ying Wu10,11 and Yao-Chun Hsu2,6,11, (1)Department of Public Health, National Cheng Kung University, College of Medicine, (2)School of Medicine, College of Medicine, I-Shou University, (3)Division of Gastroenterology and Hepatology, E-DA Cancer Hospital, (4)Division of Gastroenterology and Hepatology, Stanford University Medical Center, (5)Department of Epidemiology and Population Health, Stanford University Medical Center, (6) Gastroenterology and Hepatology, E-DA Hospital, (7)Division of Gastroenterology and Hepatology, E-Da Dachang Hospital,(8)Department of Information Technology, E-Da Healthcare System, (9)Administrative Center, E-Da Healthcare System, (10)Gastroenterology and Hepatology, Taipei Veterans General Hospital, (11)Institute of Biomedical Informatics, National Yang Ming Chiao Tung University
Background: Finite nucleos(t)ide analog (NA) therapy has been proposed as an alternative strategy in the management of chronic hepatitis B (CHB). However, data reporting the risk of clinical adverse events in large cohorts of CHB patients who discontinued NA therapy as part of their routine care and were monitored in real-world practice is limited. We aimed to quantify the risk of severe acute exacerbation (SAE, defined as elevation of serum alanine aminotransferase >200 U/L plus hyperbilirubinemia >2 mg/dL) and subsequent occurrences of acute on chronic liver failure (defined as serum bilirubin >5 mg/dL and international normalized ratio >1.5 in addition to clinical complications) and death in real-world CHB patients after stopping NA therapy.
Methods: We screened all CHB patients who discontinued NA at three clinical centers in Taiwan from April 1, 2004 to October 8, 2020. Those with serious comorbidity, malignancy or receiving immunosuppressive therapy were excluded.
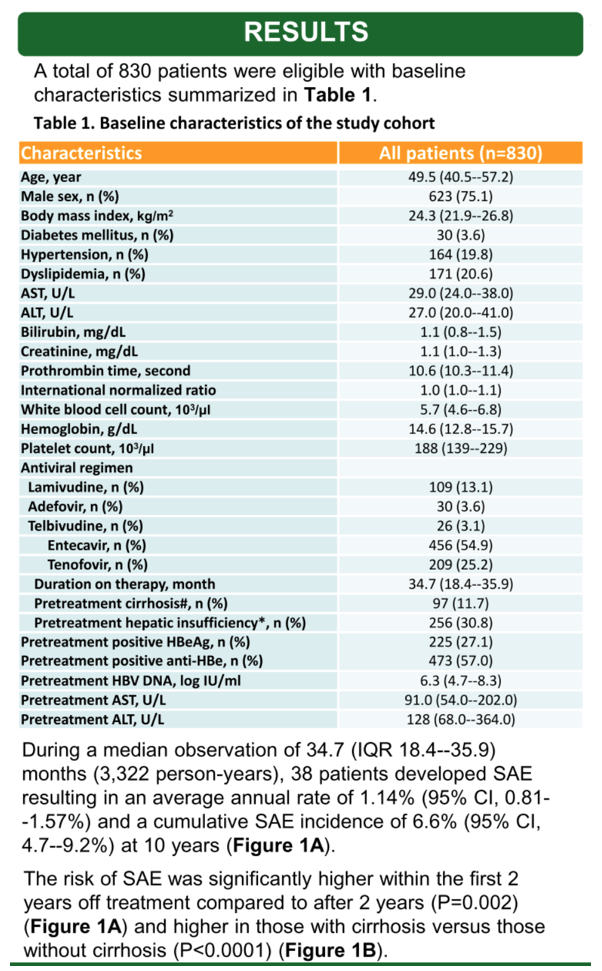
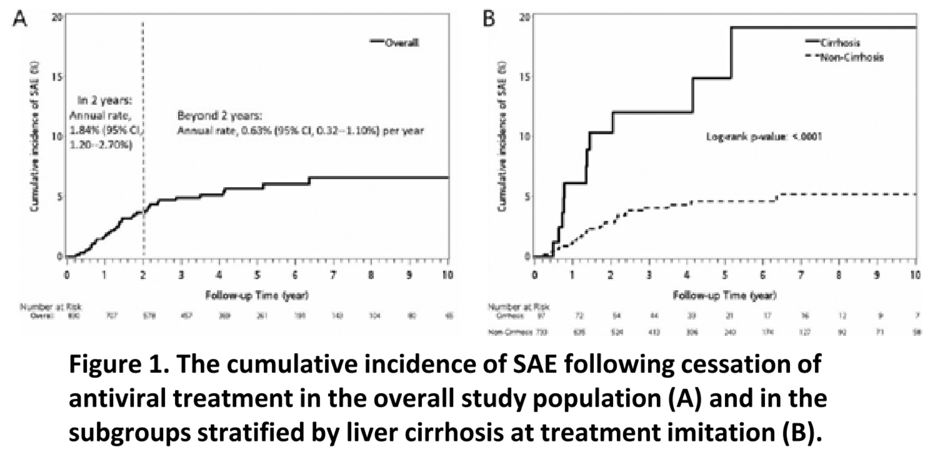
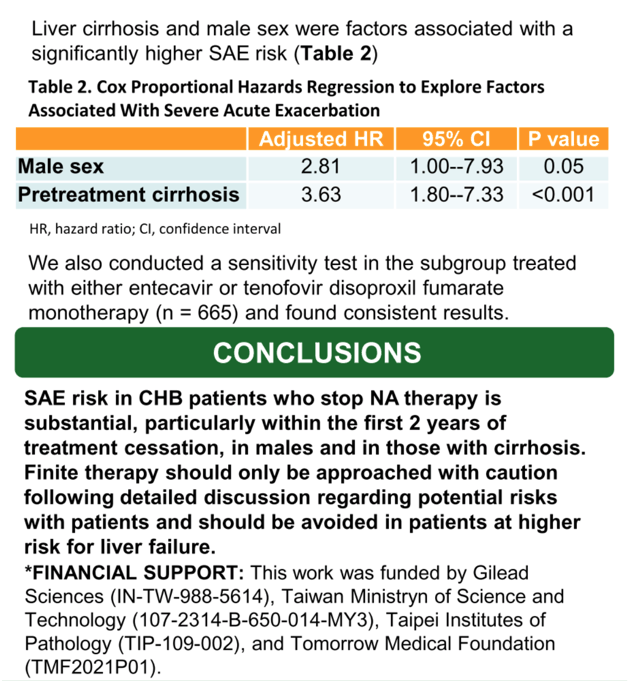
Results: We enrolled 830 patients (median age, 49.5 years; 75.1% male; 11.7% cirrhosis) who discontinued NA after a median duration of 2.9 years, mostly due to loss of reimbursement coverage. During a median post-treatment follow-up of 3.6 years, 38 patients developed SAE resulting in an average annual rate of 1.14% (95% confidence interval [CI], 0.81--1.57%) and a cumulative SAE incidence of 6.6% (95% CI, 4.7--9.2%) at 10 years (Figure 1A). The risk of SAE was significantly higher within the first 2 years off treatment compared to after 2 years (P=0.002) (Figure 1A) and higher in those with cirrhosis versus those without cirrhosis (P<0.0001) (Figure 1B). On multivariable Cox regression analysis, independently associated factors for SAE were liver cirrhosis at treatment initiation (hazard ratio, 3.63; 95% CI, 1.80--7.33; P<0.001) and male sex (hazard ratio, 2.81; 95% CI, 1.0--7.93; P=0.05). Seven of the 38 SAE cases (18.4%) progressed to liver failure and three (7.9%) subsequently died.
Conclusion: SAE risk in CHB patients who stop NA therapy is substantial, particularly within the first 2 years of treatment cessation, in males and in those with cirrhosis. Finite therapy should only be approached with caution following detailed discussion regarding potential risks with patients and should be avoided in patients at higher risk for liver failure.




|
| |
|
 |
 |
|
|