 |
 |
 |
| |
HBV and HCV are Each Associated with Adverse Pregnancy
Complications: a 7-year Nationwide Inpatient Sample Study
|
| |
| |
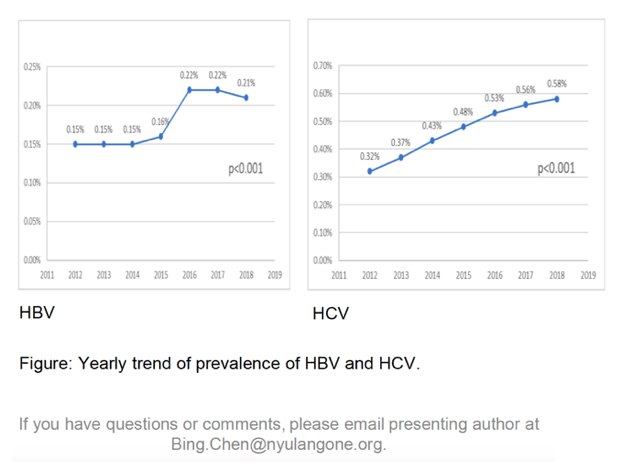
- There was a rising prevalence of chronic hepatitis B and chronic hepatitis C over time among pregnant women. (HCV almost doubled since 2012)
- hepatitis B was associated with a significantly higher rate of GDM and chronic hepatitis C was associated with a significantly higher rate of preterm labor and all-cause in-hospital maternal mortality during pregnancy.
--------------------------------------
AASLD: CIRRHOSIS IS ASSOCIATED WITH SIGNIFICANT ADVERSE PREGNANCY COMPLICATIONS: A 7-YEAR NATIONWIDE INPATIENT SAMPLE STUDY - (11/12/21)
AASLD: HDV seropositivity was common amongst HBsAg+ women enrolled in WIHS. 26 (22%) of the 117 HBsAg+ women were HDV seropositive - (11/12/21)
-----------------------------------
AASLD 2021 Nov 12-16
Bing Chen MD1, Yichen WangPic turMe1.Dpng2 , Tatyana Kushner MD, MSCE3
1. Department of Medicine, NYU Langone Hospital-Brooklyn, New York; 2. Mercy Internal Medicine Service, Trinity Health of New England, Massachusetts;
3. Division of Liver Diseases, Icahn School of Medicine at Mount Sinai, New York

abstract
Background: There is conflicting data regarding association of chronic hepatitis B (HBV) and chronic hepatitis C (HCV) with adverse pregnancy outcomes during pregnancy. We sought to evaluate trends over time of diagnosis of HBV/HCV in pregnant women and evaluate prevalence of associated adverse pregnancy outcomes in a national U.S. based database
Methods: We performed a retrospective study utilizing National Inpatient Sample database from 2012-2018. Previously validated ICD-9 and ICD-10 codes for pregnancy-related admissions were utilized to identify all pregnant women. Patients with acute liver disease were excluded. Patients with a diagnosis of HBV, and HCV were identified; we performed a longitudinal analysis to assess their trends over time. We evaluated pregnancy-related complications include rates of C-section, preeclampsia/eclampsia, preterm labor, and gestational diabetes (GDM), as well as all-cause in-hospital mortality, length of stay, and total cost of the hospital stay.
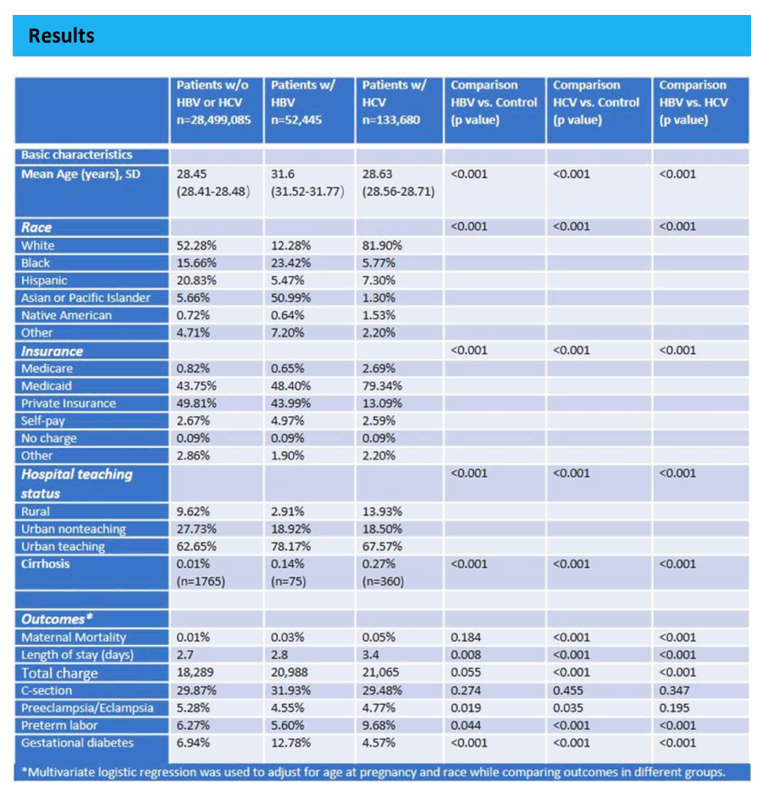
Results: A total of 28.68 million pregnancy-related admissions which met our eligibility criteria were identified; 52,445 with HBV, and 133,680 with HCV.
Over the 7-year period, prevalence of HBV and HCV each increased, from 0.15% to 0.21% (p<0.001), and 0.32% to 0.58% (p<0.001) respectively. Compared to patients without viral hepatitis, patients with HBV were more likely to be Asian or Pacific Islander (50.99% vs. 5.66%, p<0.001); pregnant patients with HCV were more likely to be white (81.90% vs. 52.28, p<0.001); patients with HCV were more likely to be white (81.90% vs. 52.28%, p<0.001). In comparison to pregnant patients without viral hepatitis, patients with HBV had significantly higher GDM (12.78% vs. 6.94%, p<0.001)(Table 1); HCV had a significantly higher rate of preterm labor (9.68% vs. 6.27%, p<0.001), all-cause mortality (0.05% vs. 0.01%, p<0.001), and longer length of stay (3.4 days vs. 2.7 days, p<0.001).
Conclusion: There was a rising prevalence of chronic hepatitis B and chronic hepatitis C over time among pregnant women. Compared to the uninfected control group, chronic hepatitis B was associated with a significantly higher rate of GDM and chronic hepatitis C was associated with a significantly higher rate of preterm labor and all-cause in-hospital maternal mortality during pregnancy. Given current recommendations for universal screening for both HBV and HCV in pregnancy, these findings should inform counseling of women who are found to have HBV or HCV during pregnancy regarding risk of adverse pregnancy outcomes.

|
| |
|
 |
 |
|
|