 |
 |
 |
| |
TREATMENT WITH BULEVIRTIDE IMPROVES PATIENT REPORTED OUTCOMES IN PATIENTS WITH CHRONIC HEPATITIS DELTA (CHD): AN INTERIM EXPLORATORY ANALYSIS AT WEEK 24
|
| |
| |
AASLD 2021 Nov 12-16
Heiner Wedemeyer1, Soo Aleman2, Vladimir Chulanov3, Gudrun Hilgard4, Jenya Antonova5, Ankita Modi Kaushik5, Andrew Lloyd6, Dmitry Manuilov5, Vithika Suri5, Tram T. Tran5, Anu O Osinusi7, Pietro Lampertico8, Viacheslav Morozov9, Olga Sagalova10, Tatyana Stepanova11 and Maria Buti12, (1) Medizinische Hochschule Hannover, Germany, (2)Karolinska Universitetssjukhuset, Karolinska Institutet, Stockholm, Sweden, (3)Central Research Institute of Epidemiology, Moscow, (4)Universitätsklinikum Essen, Germany, (5) Gilead Sciences, (6)Acaster Lloyd Consulting Ltd, (7)Gilead Sciences, Inc., Foster City, CA, USA, (8)Fondazione Irccs Ca' Granda Ospedale Maggiore Policlinico, CRC "a.M. and a. Migliavacca" Center for Liver Disease, Università Degli Studi Di Milano, Italy, (9)Hepatolog, LLC, Samara, Russian Federation, (10)Southern Ural State Medical University, Chelyabinsk, Russian Federation, (11)Clinic of Modern Medicine, Moscow, (12)Liver Unit. Hospital Universitario Valle Hebron, Barcelona, Spain

Background: Chronic hepatitis delta (CHD) is the most severe form of viral hepatitis, causing rapid progression to cirrhosis, decompensation, or hepatocellular carcinoma. Until recently, there were no approved treatments options. In 2020, European Medicines Agency conditionally approved bulevirtide (BLV 2mg) as the first treatment for CHD. This abstract reports exploratory interim analysis of health-related quality of life (HRQOL) benefits of the 24-week treatment with approved BLV-2mg dose in CHD patients within an ongoing Phase 3 trial.
Methods: In MYR301-a randomized, open-label, parallel-group, multicentre Phase 3 clinical trial-CHD patients were randomised (1:1:1) to and started receiving three treatments (BLV 2mg or 10mg or delayed-treatment [DT]) for a total of 3 years). The BLV 10mg data are not reported as not regulatory approved. DT patients received no active treatment until week 48. Prior to initiating study-visit activities, patients completed the Hepatitis Quality of Life Questionnaire (HQLQTM, including SF-36 and 15 supplemental items) at baseline (BL) and Week 24 (W24) with subsequent periodic intervals throughout the study.
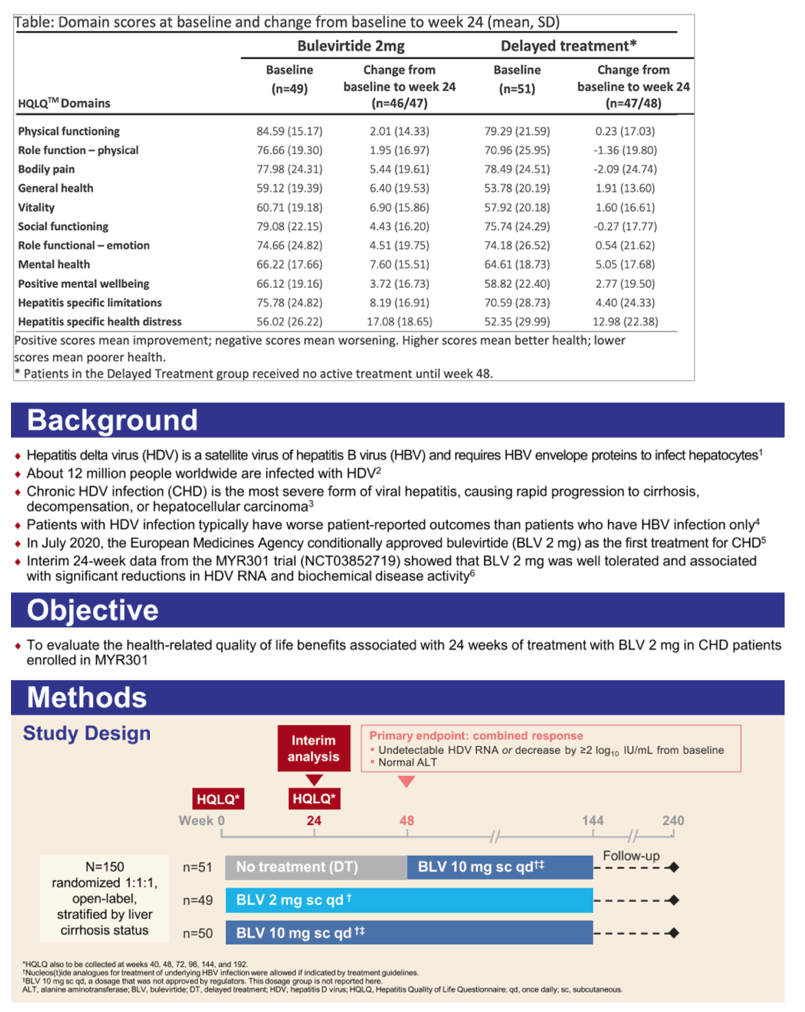
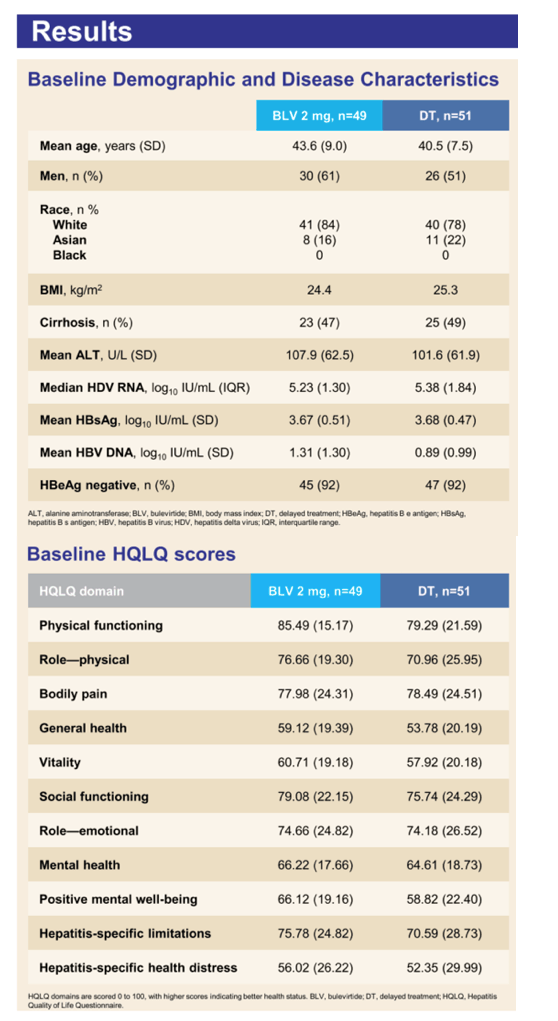
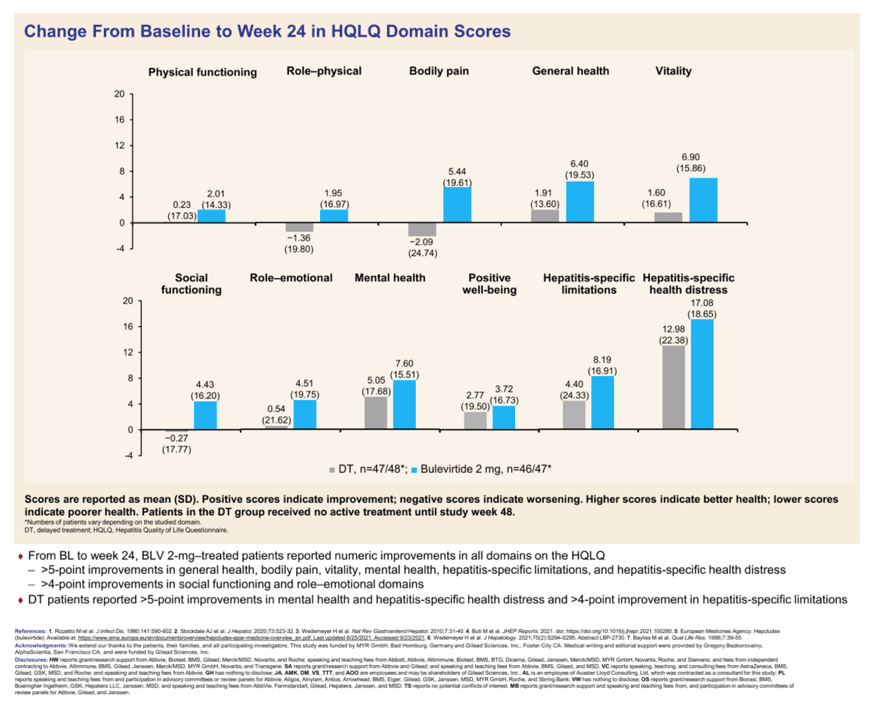
Results: At BL, the subjects receiving BLV 2mg (n=49, mean±SD age 43.6 (±9.0), BMI 24.4 (kg/m²), 61.2% male, 48% with cirrhosis) and DT (n=51, reported mean±SD age 40.5 (±7.5), BMI 25.26 (kg/m²), 51% male, 51% with cirrhosis) reported varying levels of HRQoL (Table). From BL to W24, BLV 2mg-treated patients reported improvements in all domains on the HQLQTM, notably >5-point improvements in general health, bodily pain, vitality, mental health, hepatitis-specific (HS) limitations, and HS health distress and >4 points in social functioning and role functioning-emotional domains. The DT patients reported >5-point improvements in mental health and HS health distress and > 4-points on HS limitations.
Conclusion: Both BLV 2mg and DT groups reported improvements from BL to W24 in HRQoL measured by HQLQTM, most notably in HS limitations, HS health in distress, and mental health. However more domain improvements were observed with BLV 2mg most notably in general health, bodily pain, vitality, social functioning, and role functioning-emotional than with the DT arm. Further research is needed to understand the discrepancies in the baseline data, the burden of illness, the course of the disease, and the long-term effect of treatment.


|
| |
|
 |
 |
|
|