 |
 |
 |
| |
Burden of Illness and Economic Impact of Nonalcoholic Steatohepatitis (NASH) in the United States According to the Presence of Obesity
|
| |
| |
AASLD 2021 Nov 12-15
Zobair M. Younossi1, 2, 3, James M. Paik1,2,3, Linda Henry3, Joe Yang4, Gail Fernandes4, Maria Stepanova5, Fatema Nader5
1. Betty and Guy Beatty Center for Integrated Research, Inova Health System, Falls Church, VA, United States
2. Center for Liver Disease, Department of Medicine, Inova Fairfax Medical Campus, Falls Church, VA, United States
3. Inova Medicine, Inova Health System, Falls Church, VA, United States
4. Merck & Co., Inc., Kenilworth, NJ, USA
5. Center for Outcomes Research in Liver Diseases, Washington DC, United States

Abstract
Background: NASH is driven by the growing global prevalence of obesity. We aimed to model clinical and economic burden of NASH in the US, stratified by presence or absence of obesity.
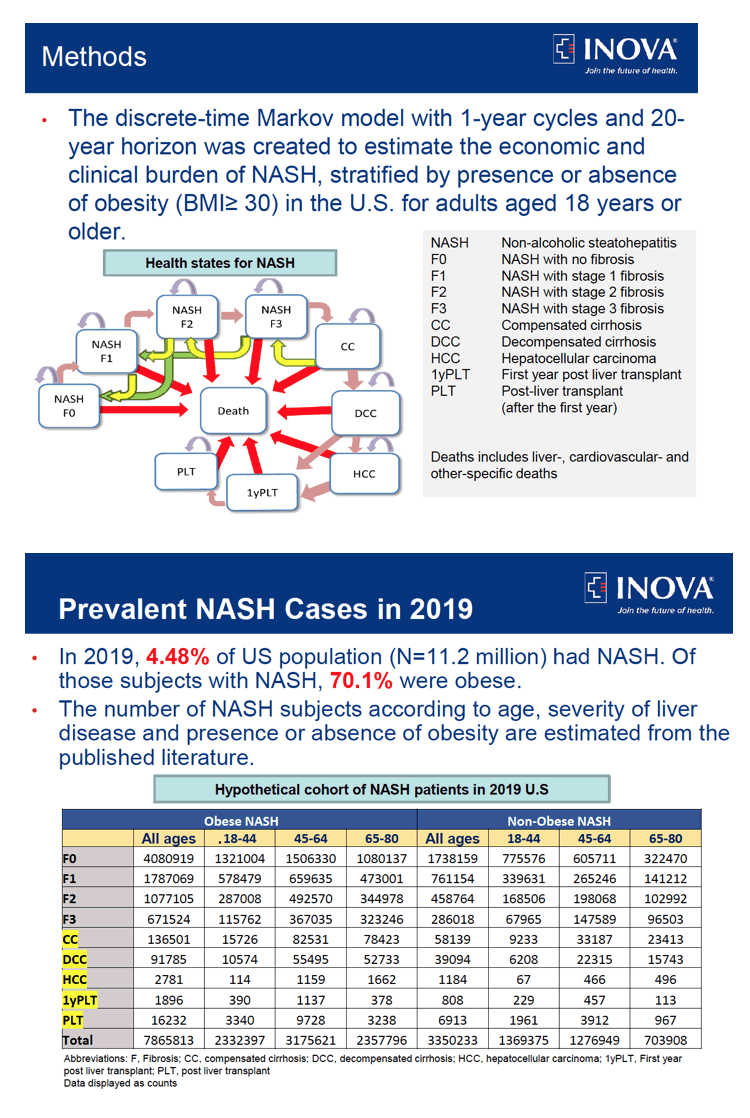
Methods:
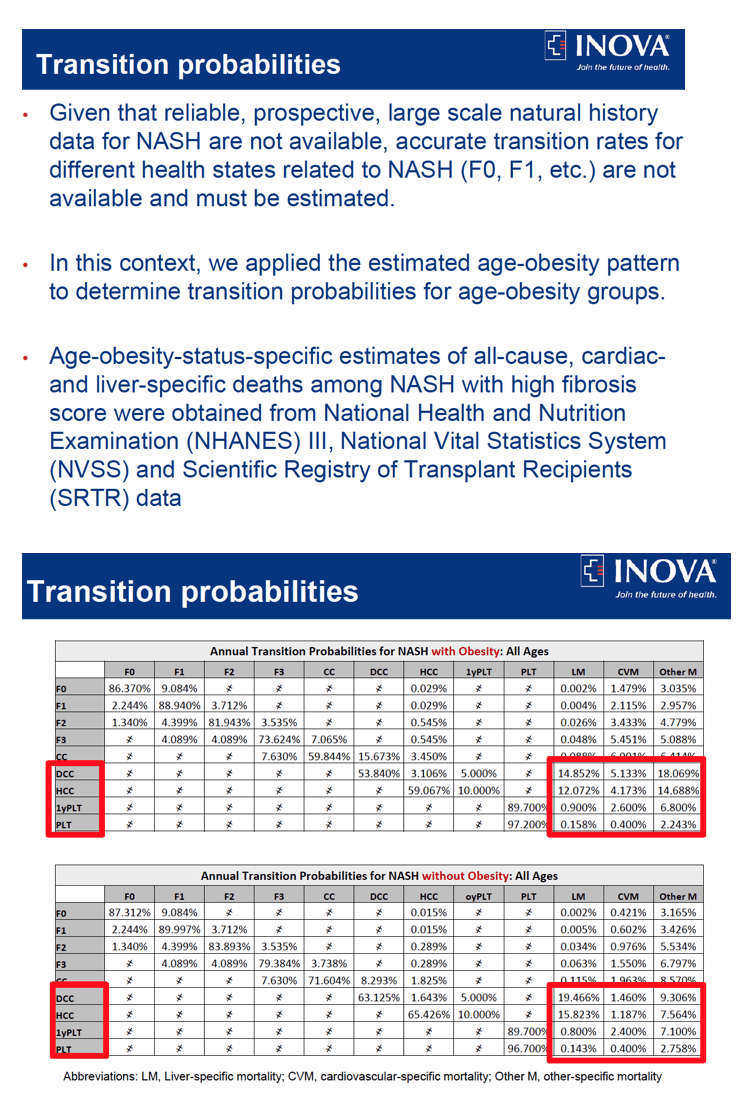
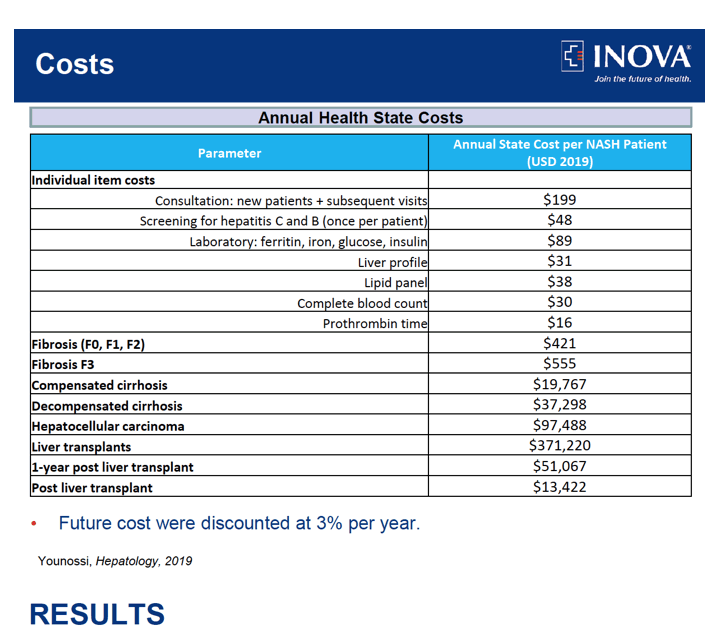
We used a discrete-time Markov model to simulate 20-year outcomes for hypothetical cohort of NASH patients in the U.S. We stratified cohorts by age and presence of obesity using the U.S. population projections data for 2019-2040 and published literature. The Markov model included 9 health states and 3 absorbing death states in each year with defined transition probabilities (TPs). The estimated age-obesity impact on all-cause, cardiac- and liver-specific deaths among NAFLD with high fibrosis scores were obtained from the National Health and Nutrition Examination (NHANES) III, National Vital Statistics System (NVSS) and Scientific Registry of Transplant Recipients (SRTR) data. These data were used to adjust TPs from health states to death. The TPs between health states were then rescaled to sum to one at each state. We then split all TPs for NASH with all ages into the age-obesity group using information from the literature. Costs included inpatient, outpatient, professional services, emergency department, and drug costs, which were obtained from the Center for Medicare and Medicaid Services Fee Schedule 2019 and published data. 95% uncertainty interval (UIs) were calculated as the 25th and 975th ranked values across all 1,000 simulations. Costs were reported in 2019 US dollars and a discount rate of 3% was used. Main outcomes were Cardiac- and Liver-specific deaths, Liver transplants (LT), years of decompensated cirrhosis (DCCy), years of hepatocellular carcinoma (HCCy) and costs.
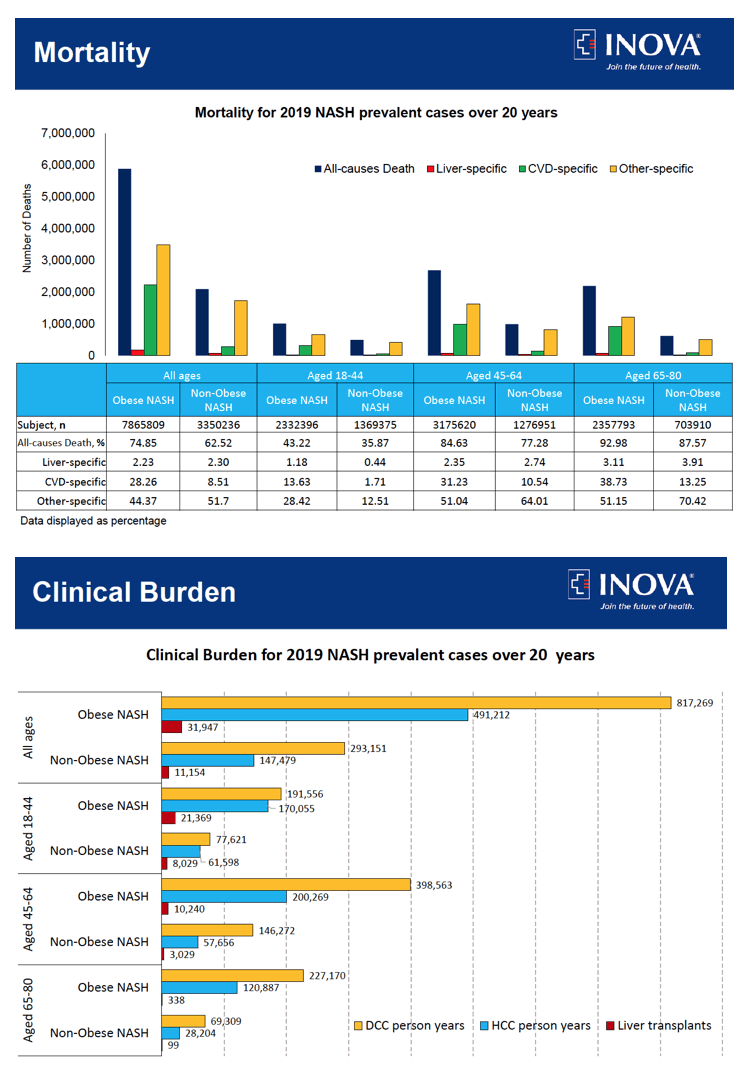
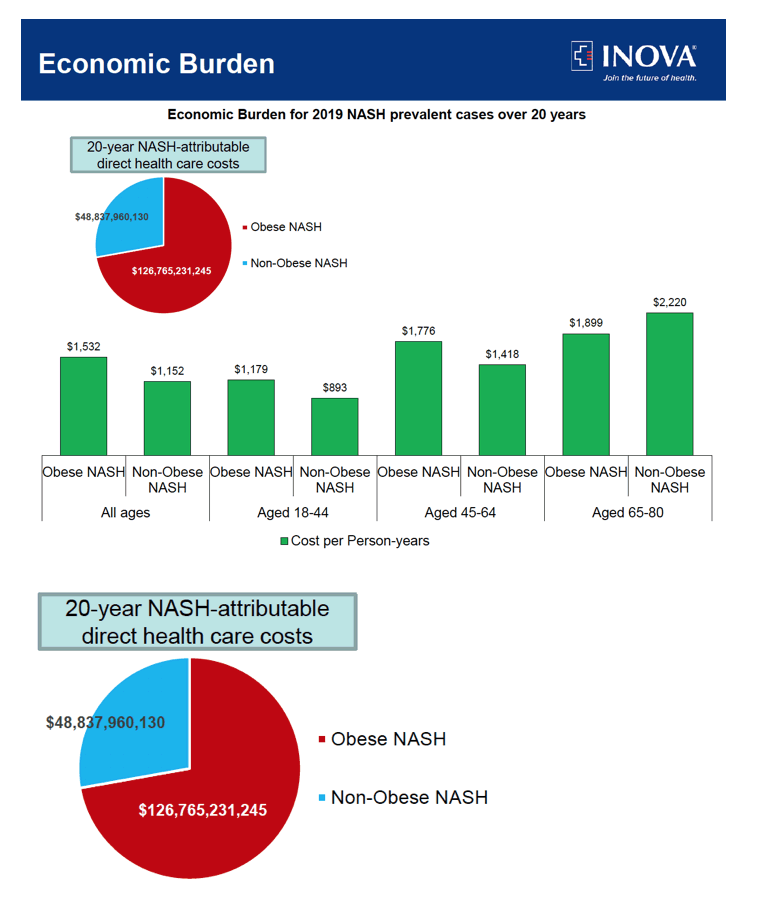
Results: In 2019, 4.48% of the U.S. population (N=11.2 million) was estimated to have NASH. Of those with NASH, 80.1% were obese. Over 2 decades (2019-2040), we estimated that obese NASH will have higher all cause (74.1% vs 59.1%), cardiac (26.4% vs 7.4%) and liver-specific mortality (2.7% vs. 2.3%) compared to non-obese NASH. During this period, we estimated that the obese NASH cohort will experience 48,855 LT (48,692-49,018), 1,138,665 DDCy (1,137,750-1,139,694) and 743,833 HCCy (742,738-745,009). In contrast, non-obese NASH will have 8,332 LT (8,259-8,413), 193,988 DCCy (193,215-194,569) and 103,795 HCCy (103,414-104,250). Finally, the expected costs for obese NASH and the non-obese NASH cohorts were estimated to be $161.91B (161.77B-$162.05B) and $30.99B ($30.94B-$31.05B), respectively.
Conclusion: The growing prevalence of obesity and related NASH will have a major clinical and economic impact in the U.S. These data should inform policy makers and other stakeholders to address the growing burden of NASH in the U.S.

|
| |
|
 |
 |
|
|