 |
 |
 |
| |
Hepatitis D-Associated Hospitalizations in the United States: 2010-2018
|
| |
| |
AASLD 2021 Nov 12-15

Paul Wasuwanich (Univ of Florida College of Medicine); Catherine W. Striley; Saleem Kamili; Eyasu H. Teshale; Eric C. Seaberg; Wikrom Karnsakul
program abstract
Background: Globally, hepatitis D is an important burden of liver disease, estimated to be responsible for 18% of cirrhosis among those with hepatitis B. However, the burden of hepatitis D is not clearly known in the United States, and with the recent approval of bulevirtide in Europe and anticipated approval by the US Food and Drug Administration, there is need for measuring the burden of this disease. We aim to estimate the incidence of hepatitis D-associated hospitalizations in the United States and describe the clinical, demographic, and geographic characteristics.
Methods: We utilized hospitalization data from the 2010-2018 National Inpatient Sample from the Healthcare Cost and Utilization Project. All hospitalizations with hepatitis D, and hepatitis B without hepatitis D, were identified by ICD-9/ICD-10 codes. Demographic, geographic, and clinical data including cirrhosis, portal hypertension, ascites, thrombocytopenia, and mortality, were extracted. Frequencies were compared using χ2 test; risk factors for mortality were evaluated using logistic regression.
Results:
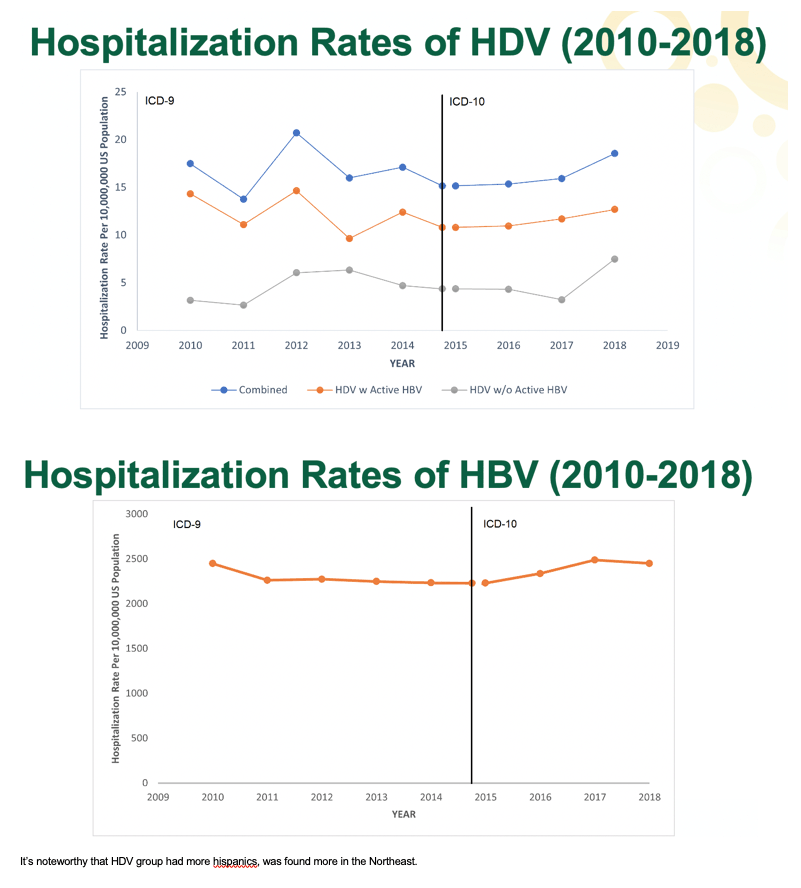
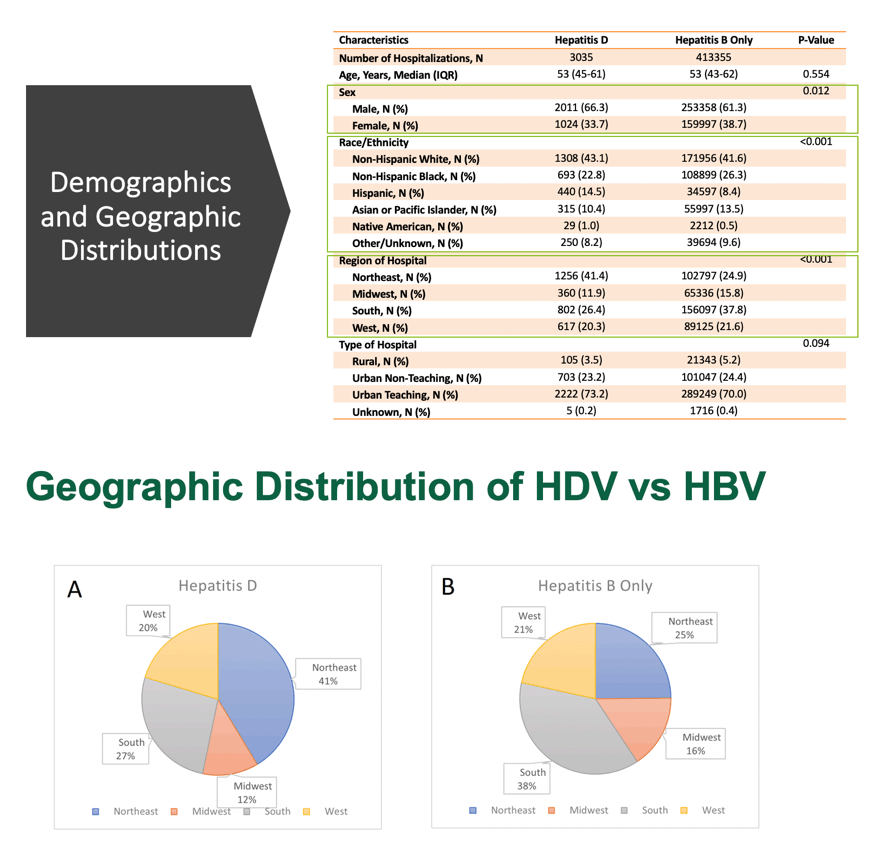
We identified 3,825 hepatitis D-associated hospitalizations with median age of 53 (IQR: 45-61) years. Average annual hospitalization rate of hepatitis D was 16.7 per 10,000,000 between 2010-2015 (ICD-9) and 7.4 per 10,000,000 between 2015-2018 (ICD-10) (Figure 1). Prevalence of hepatitis D among those hospitalized with hepatitis B was 0.6%. Compared to hepatitis B alone, the hepatitis D cohort had more males (66.3% vs 61.3%; P=.012), Hispanic persons (14.5% vs 8.4%; P<.001), and hospitalizations in the Northeast (41.4% vs 24.9%; P<.001). The hepatitis D cohort had greater frequencies of liver failure (6.5% vs 4.5%; P=.018), non-alcoholic cirrhosis (20.5% vs 15.2%; P<.001), portal hypertension (12.9% vs 6.8%; P<.001), ascites (16.5% vs 10.8%; P<.001), and thrombocytopenia (22.0% vs 18.0%; P=.012).Although overall mortality of hepatitis D was similar to that of hepatitis B alone (3.7% vs 3.7%; P=.995), within the hepatitis D cohort, being over 65 years of age (OR=3.79; P=.020) and having a diagnosis of alcoholic cirrhosis (OR=3.37; P=.044) increased the odds of mortality.
Conclusion: While hepatitis D-associated hospitalizations are uncommon, they are associated with severe complications. Early detection by routine testing of persons with hepatitis B for co-infection with hepatitis D could slow disease progression and avoid severe outcomes as hepatitis D-specific treatments are emerging.






|
| |
|
 |
 |
|
|