 |
 |
 |
| |
Survey of Consumers, Clinicians and Service Providers about Needs of Long-Term Survivors and People Aging with HIV in New York State
|
| |
| |
International Workshop on HIV and Aging, September 23-24, 2021
from Jules: I will add that many older, aging & elderly PWH are not satisfied with the care they receive. And many do not realize their care is inadequate. They may not have a high standard to compare with what they currently receive so many may not even realize what good & adequate care is. But in fact many realize & express dissatisfaction with 15-20 minute visits the current care system allows with doctors, care providers, this limited time is dictated by bottom line costs & profits to the hospital or clinic. Insurers restrict payments to low flat fees the amount of reimbursement they pay for a visit, and thus the hospital or clinic limits time of a visit to maximize their income so they can see more patients. The patients end up suffering & often many doctors feel exploited too. Some doctors express also they feel rushed & unable to provide the time & attention they used to & would like to, they are working under harsh & extreme circumstances too. For elderly, aging PWH with many care needs, with multi-comotbidities (heart disease, diabetes, bone disease, depression, etc) who need more time & attention with their HIV doctors & with specialists 20 minute visits & the rush job they get to get in & out of the visit - this does NOT meet their needs. We need flexible time to visit with HIV doctors, the doctors MUST NOT feel rushed to get through the visit, as they all are currently, PWH are tired of the doctor sitting & staring at the computer to input data instead of real interaction with the PWH learning about what is really going on with them. In terms of referrals to specialists the same "rushed" system does not give the PH what they need. The specialist such as for example a referral to a cardiologist has the same 15 minute limit, often does not know much or anything about HIV, there is too little or NO communication between the HIV primary care doctor & the specialist & too little or no explanation to the PWH about their condition (there should be a 3-way telehealth, communication including th PWH to make sure the PWH fully understands their diagnosis, condition & treatment). Mental health is completely ignored all too often for PWH, frailty & physical function & cognitive function are completely absent. There is no connection between the PWH & the primary care HIV doctor anymore, very little personal relationship like there was for many 10 years ago. There is a need for sensitivity training for HIV primary care doctors regarding ageism & aging & cultural issues. These are not theoretical concerns, some older & elderly PWH are prematurely getting strokes, heart attacks or dying because they are not getting the care they require & need, and because they are not educated about aging & comorbidities. They do not understand their higher risk for stroke or heart attack & the need for better diet & exercise, they are not receiving education about this. Many aging pWH do not even know or understand they are subject to premature aging & earlier onset for Comorbidities conditions like a heart attack or stroke, their doctors never informed them of this perhaps because they did not feel they had enough time to do that or because they did not for some reason feel the need to inform the patient, perhaps the doctors themselves need to be better educated about premature aging & earlier onset for Comorbidities conditions for aging PWH.
Maria Teresa Brown, PhD1; John Wikiera2; Angie Partap3; Marz Albarran4; Courtney Ahmed, BA2; Sheridan Beard, BS2; Victoria Brock, BS2; Thomas Heslop5; Eugenia Siegler, MD5 1Syracuse University, 2NYS DOH AIDS Institute, 3Stony Brook Medicine, 4Albany Damien Center, 5 Weill Cornell Medical College
Background: As the number of long-term survivors (LTS) and older people with HIV (OPH) continues to increase, there is no consensus on how to meet their practical needs.
Materials & Methods: The HIV+ Aging and LTS Subcommittee of the NYS Quality of Care Consumer Advisory Council held town halls for consumers and providers across the state in August 2020. Based on themes identified in these town halls, Syracuse University launched a statewide survey in June 2021 using Qualtrics™. The survey was open to consumers aged 18 and over who were LTS or OPH, and clinicians and social service providers working with them. For each theme, respondents were asked to choose the 3 most important barriers and recommendations. Consumers also answered questions about HIV and comorbidities; all answered questions about demographics. Themes included: clinical care and coordination, telemedicine/telehealth, medication and pharmacy services, aging and long-term care, mental health and social support, barriers during COVID-19, health equity and stigma, transportation and food, housing, and financial support. Responses were characterized using basic descriptive statistics.
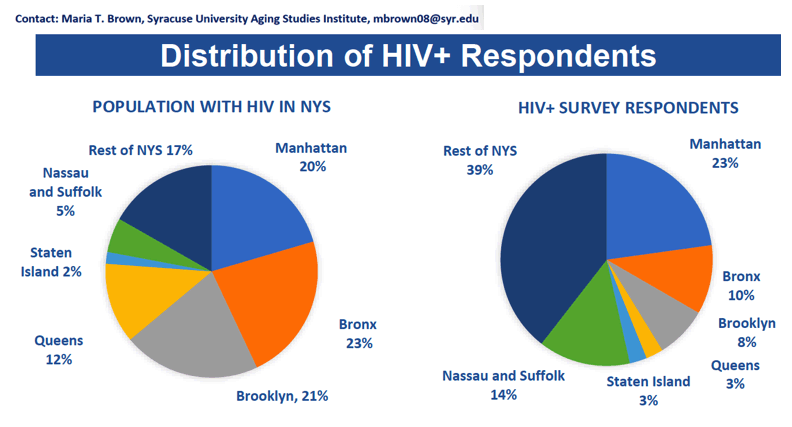
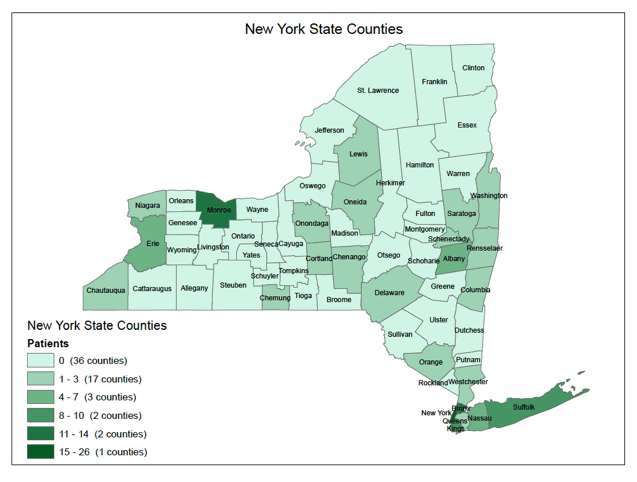
Results: 132 people completed the survey: 124 consumers from 26 counties and 44 providers (20 clinicians, 24 social service providers). On average, consumers were 56 years old, and had been living with their HIV+ diagnosis for 27 years; 39% were cis gender women, and 28% were African American. Almost half (46%) were from the New York City Region and 13% were from each of the Long Island and Finger Lakes Regions. Consumers reported 4 additional health conditions, most commonly anxiety (27%), depression (30%), hypertension (27%), and being overweight (26%). The barriers endorsed most by consumers and providers were related to housing, clinical care and coordination, telehealth, and mental health and social support.
The most endorsed recommendations to address these barriers were: for housing, build more housing and make more housing available to low-income populations; for clinical care and coordination, integrate HIV care with other specialties; for telehealth, mandate annual in-person visits to ensure that PLWHA needs are being met; and for mental health and social support, hire counselors and mental health professionals that represent the communities they serve. In contrast with greater consumer concern about catching potential medication interactions, providers expressed concern about medication delivery services and lack of sensitivity training for pharmacy staff. All 3 groups reported that consumers were unable to see people or attend support groups in person due to COVID-19 and recognized consumers' financial strains and recommended that CPWs make regular check-in calls to PLWHA during COVID-19 and that the state provide more funding to assist OPH and LTS in housing, food, and transportation.
Conclusions: Survey respondents in NYS are most concerned with coordination of clinical care, unmet housing needs, cultural representation in mental health services, and financial support of older people living with HIV/AIDS (PLWHA) and long-term survivors of HIV. Consumers, clinicians, and service providers shared many of the same impressions of barriers and recommendations.



|
| |
|
 |
 |
|
|