 |
 |
 |
| |
BEYOND PAIN: PRESCRIPTION OPIOID USE IN THE WOMEN'S INTERAGENCY HIV STUDY
|
| |
| |
...use has doubled, WLWH had 56% increased chronic prescription opioid use....increased mortality...sexual minority women had 70% increased use
Why do HIV+ women’s issues get so little broad discussion & attention. Jules
Adam W . Carrico1, Lorie Benning2, Kathleen Weber3, Anjali Sharma4, Michael Plankey5, Deborah Jones Weiss1, Mirjam-Colette Kempf6, Bradley Aouizerat7, Tracey Wilson8, Joel Milam9, Adaora Adimora10, Gina Wingood11, Mardge Cohen12 1University of Miami, Miami, FL, USA, 2John H Stroger Jr Hospital of Cook County, Chicago, IL, USA, 3Hektoen Institute of Medicine/Cook County Health and Hospitals System, Chicago, IL, USA, 4Albert Einstein College of Medicine, Bronx, NY, USA, 5Georgetown University, Washington, DC, USA, 6University of Alabama at Birmingham, Birmingham, AL, USA, 7New York University, New York City, NY, USA, 8State University of New York Downstate Medical Center Downstate Medical Center, Brooklyn, NY, USA, 9University of Southern California, Los Angeles, CA, USA, 10University of North Carolina at Chapel Hill, Chapel Hill, NC, USA, 11Columbia University, New York, NY, USA, 12Cook County Health and Hospitals System, Chicago, IL, USA
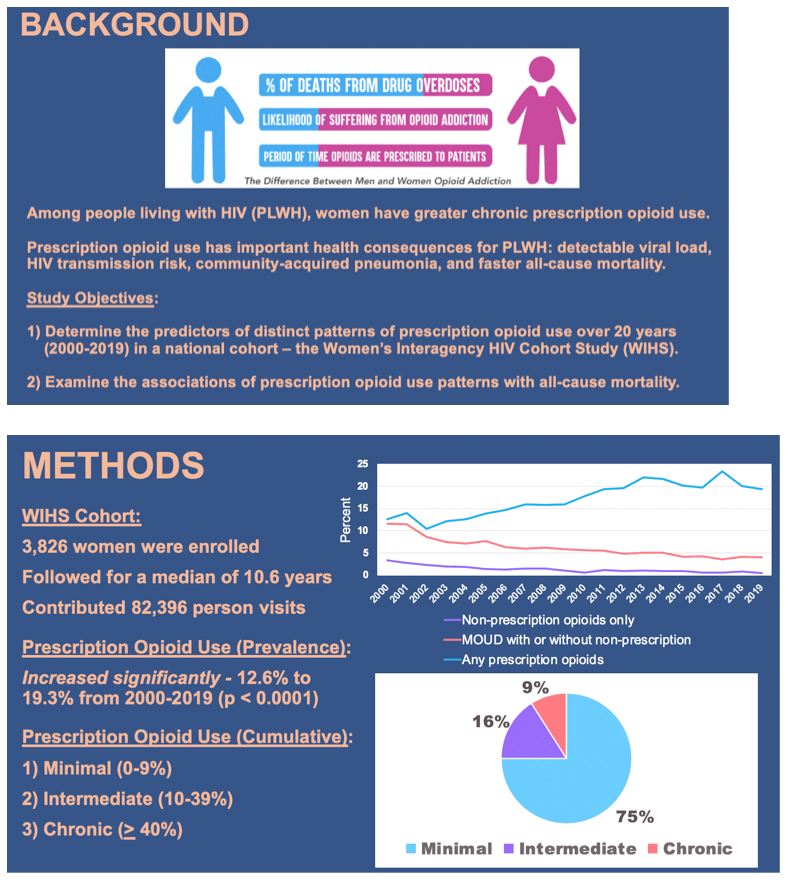
Background: Women are more likely than men to experience chronic pain and use prescription opioids. Less is known about predictors and consequences of prescription opioid use among women living with HIV (WLWH).
Methods: 3,826 WLWH or women without HIV enrolled in the Women's Interagency HIV Study (WIHS) and completed bi-annual self-report prescription opioid use assessments from 2000-2019. Cumulative proportion of visits with prescription opioid use was categorized as: minimal (0-9%); intermediate (10- 39%); and chronic (40% or greater). Logistic regression examined independent predictors and proportional hazards regression estimated the unadjusted hazard of all-cause mortality, comparing intermediate and chronic prescription opioid use to minimal use.
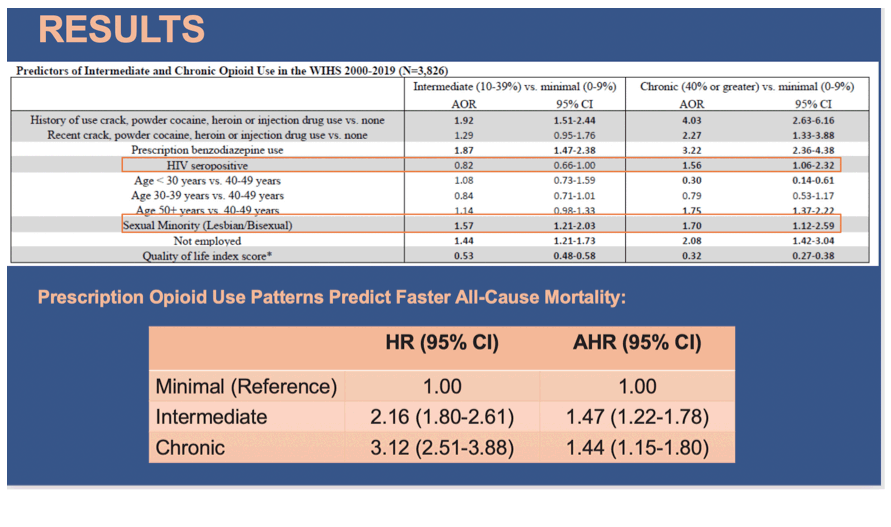
Results: At index visit, most participants were Black (64%), with mean age of 38.9 years and a median annual income of < $12,000. Women contributed 82,396 person-visits over a median of 10.6 [interquartile range (IQR) = 5.0-17.2] years. The annual prevalence of prescription opioid use significantly increased from 12.6% to 19.3% from 2000-2019 (p < 0.0001). Prescription opioid use was classified as minimal in 75%, intermediate in 16%, and chronic in 9% of women. WLWH had 56% higher odds of chronic prescription opioid use compared to women without HIV. Even after adjusting for quality of life scores that included ratings of pain, women with intermediate prescription opioid use had greater odds of being sexual minorities (lesbian or bisexual), unemployed, and were more likely to report benzodiazepine and non-prescription substance use compared to those with minimal use. Similar results were found when comparing chronic to minimal opioid use, but with generally greater magnitude than those observed with intermediate versus minimal use (see Table). Intermediate and chronic prescription opioid use were respectively associated with a 2-fold and 3-fold increased risk of all-cause mortality.
Conclusion: Despite federally mandated changes in opioid prescribing guidelines, prescription opioid use in the WIHS significantly increased from 2000-2019. Findings underscore the need for non-opioid and non- pharmacologic interventions for chronic pain in sexual minorities and WLWH. Concurrent use of benzodiazepines and non-prescription drugs should also be addressed and treated to reduce risk of mortality.

|
| |
|
 |
 |
|
|