 |
 |
 |
| |
CARDIOMETABOLIC HEALTH IN HIV+ AND HIV- PREGNANT SOUTH AFRICAN WOMEN
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Angela Bengtson1, Hlengiwe Madlala2, Zandile Maqwatini2, Azetta Fisher2, Landon Myer2
1Brown University, Providence, RI, USA, 2University of Cape Town, Cape Town, South Africa
Background: HIV and antiretroviral therapy (ART) frequently influences cardiometabolic health, including obesity, glucose metabolism, lipids, and blood pressure (BP), but there are few data on the cardiometabolic impact of HIV and ART in pregnancy.
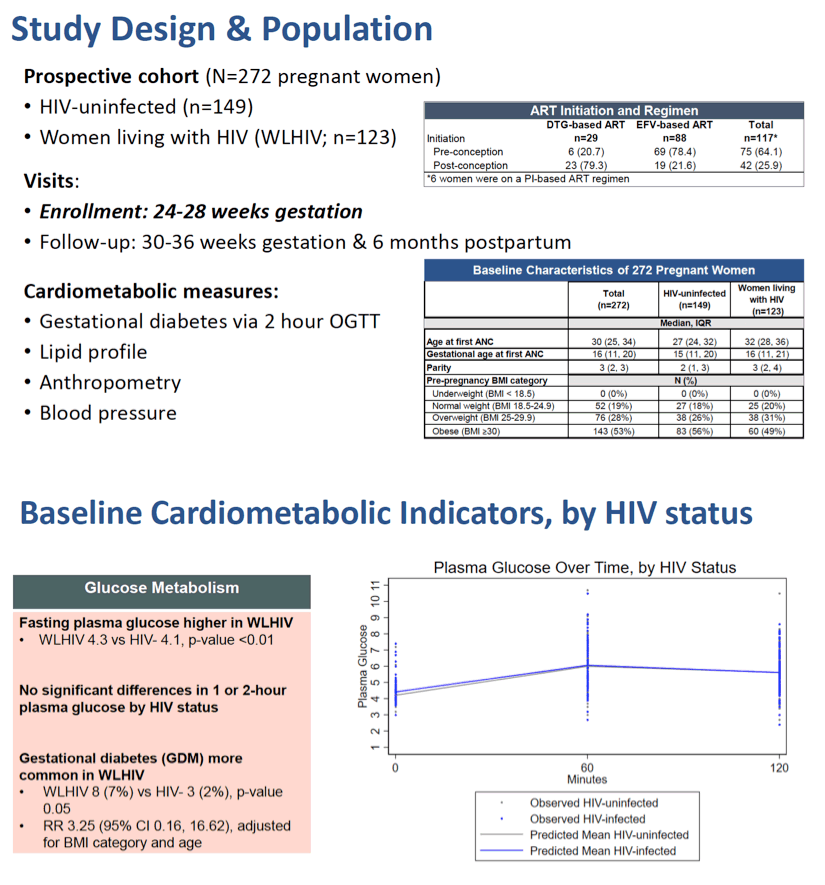
Methods: We consecutively enrolled HIV+ and HIV- women in routine antenatal care at 24-28 weeks' gestation in Cape Town. At enrollment, women underwent a fasted 2-hour oral glucose tolerance test for gestational diabetes (GDM), diagnosed via WHO guidelines (fasting plasma glucose (PG) ≥5.1 mmol/l, 1-hour PG ≥ 10.0 or 2-hour PG ≥8.5). Fasted blood samples were used to evaluate triglycerides, total cholesterol (TC), high-density lipoprotein (HDL) cholesterol, and low-density lipoprotein (LDL) cholesterol. BP and anthropometry was assessed by trained research staff. Self-reported pre- pregnancy weight was used to estimate pre-pregnancy body mass index (BMI; obesity = pre-pregnancy BMI ≥ 30). Hypertension was defined as ≥130/80 mmHg. All HIV+ women were on TDF 300mg+3TC 300mg/FTC 200mg+EFV 600mg pre (n=76) or post (n=6) conception.
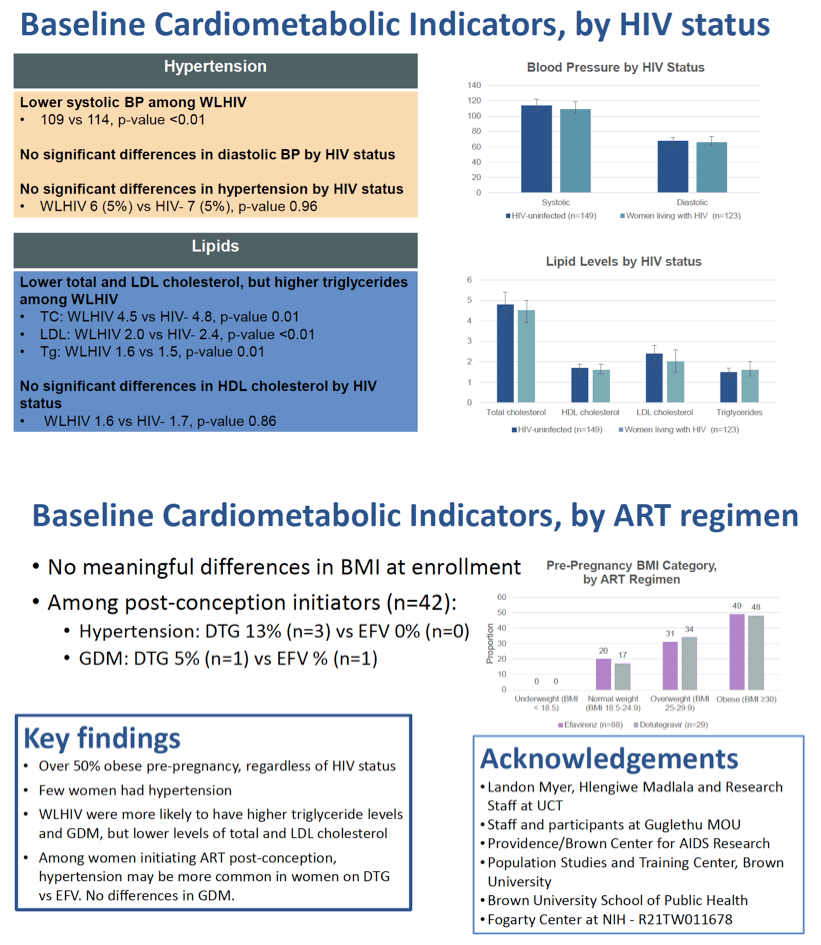
Results: Among 231 women (82 HIV+, 149 HIV-), the median gestational age at first antenatal care was 15 weeks (IQR 11, 20), 18% were primigravida (4% HIV+ vs 26% HIV-, p-value <0.01), and 54% were obese pre-pregnancy (HIV+ 50% vs HIV- 56%, p-value 0.50; Table). Systolic BP was higher among HIV- vs HIV+ women (114 vs 109, p-value <0.01) but the prevalence of hypertension was similar (5% vs 2%, p-value 0.39). Compared to HIV- women, HIV+ women had slightly higher median triglyceride levels (1.6 mmol/l vs 1.5, p-value 0.03), but lower TC (4.5 vs 4.8, p-value 0.01) and LDL cholesterol (1.9 vs 2.4, p-value <0.01) and similar HDL cholesterol (1.7 vs 1.7, p-value 0.34). HIV+ women had slightly higher fasting (4.3 mmol/l vs 4.1, p-value 0.05), 1-hour (6.2 vs 6.0, p-value 0.07), and 2-hour (5.7 vs 5.6, p-value 0.25) PG levels and GDM (7% vs 2%, p-value 0.05), compared to HIV- women. Adjusted for pre-pregnancy BMI and parity, HIV was marginally associated with GDM (RR 4.02, 95% CI 0.78-20.70, p-value 0.10).
Conclusion: In this cohort of pregnant HIV- and HIV+ women on EFV-based ART, over 50% were obese pre-pregnancy. HIV+ women were more likely to have higher triglyceride levels and GDM, but lower levels of TC and LDL cholesterol. These novel data indicate the burden of cardiometabolic risk factors in HIV+ pregnant women and point to the need to strengthen services to diagnose and manage cardiometabolic health in HIV+ women.

|
| |
|
 |
 |
|
|