 |
 |
 |
| |
T-CELL IMMUNE DYSREGULATION AND MORTALITY IN WOMEN WITH HIV
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Brandilyn A. Peters, Jee-Young Moon, David B. Hanna, Olaf Kutsch, Margaret Fischl, Caitlin Moran, Adaora A. Adimora, Stephen Gange, Nadia R. Roan, Katherine G. Michel, Michael Augenbraun, Anjali Sharma, Alan Landay, Seema Desai, Robert C. Kaplan
Background
Dysregulation of adaptive immunity is a hallmark of HIV infection that persists even on antiretroviral therapy (ART), and may contribute to higher risk of non-HIV-related diseases in people with HIV compared to people without HIV. Yet few large, prospective studies with long follow-up have examined associations of adaptive immunity deficits with mortality in HIV.
Methods
Multiparameter flow cytometry was applied to peripheral blood mononuclear cells from 612 women with HIV in the Women’s Interagency HIV Study (WIHS). Samples were collected from 2002-2005, and underlying cause of death ascertained from the National Death Index up to 2018. Using competing risk regression, we examined associations of CD4+ and CD8+ T-cell activation (%CD38+HLADR+), senescence (%CD57+CD28-), exhaustion (%PD-1+), and co-stimulation (%CD57-CD28+) with natural cause (i.e. all causes except overdose and other external causes), HIV-related, and non-HIV-related mortality. We developed nested models to serially adjust for age, demographic, and behavioral characteristics, cardiometabolic factors, and HIV-related factors.
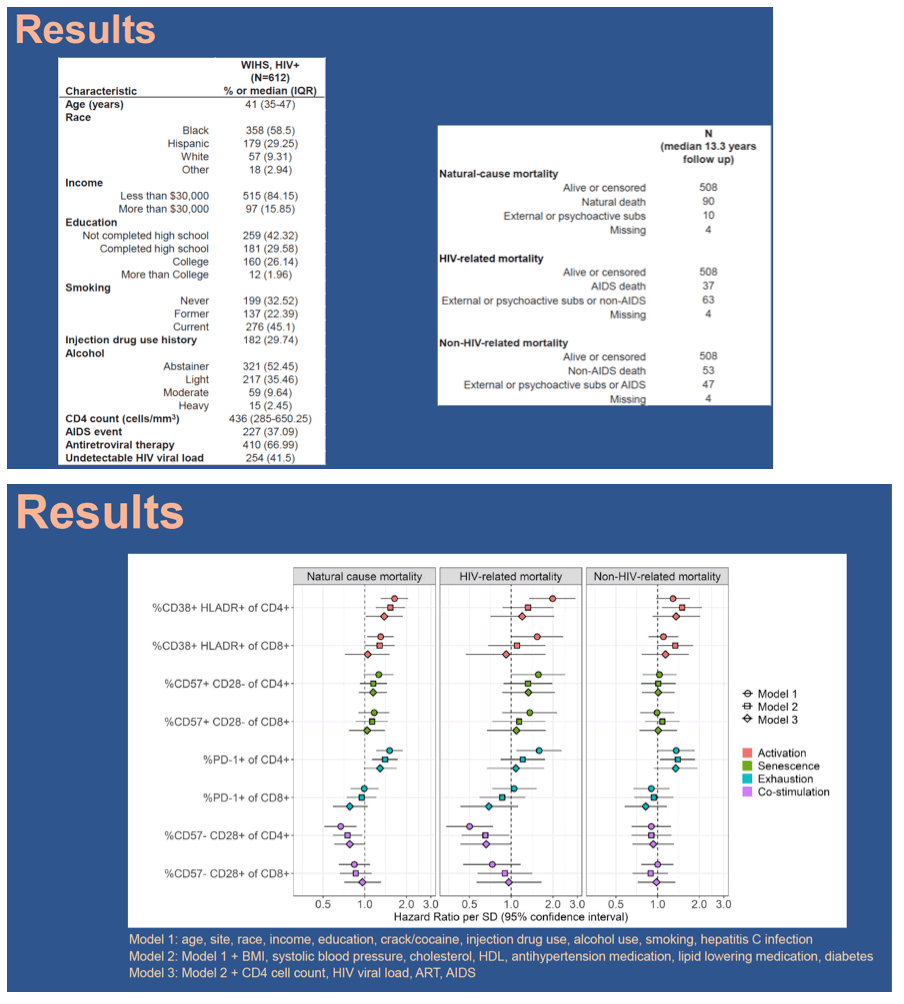
Results
At baseline, participants ranged in age from 35 to 47 (median: 41) and 67% were on ART. Among 104 deaths during median 13.3 years follow-up, 90 were due to natural causes (53 non-HIV-related, 37 HIV-related), 10 to external causes, and 4 were missing cause. Higher activation, senescence, and exhaustion of CD4+ T-cells, activation of CD8+ T-cells, and lower co-stimulation of CD4+ T-cells, were significantly associated with natural cause mortality, adjusting for age, demographic, and behavioral characteristics (Figure 1). Adjustment for cardiometabolic and HIV-related factors attenuated these associations. This pattern of associations was consistent for HIV-related mortality. For non-HIV-related mortality, only activation and exhaustion of CD4+ T-cells were marginally associated with the outcome, and these were not attenuated by further adjustment. Associations of CD4+ T-cell activation, exhaustion, and co-stimulation with natural cause mortality tended to be stronger in women with uncontrolled HIV (detectable viral load or CD4 cell count <500 cells/mm3) vs. controlled HIV, though interactions were not significant.
Conclusions
Consistent with HIV pathogenesis, dysregulation in multiple CD4+ T-cell subsets is associated with HIV-related mortality. Activation and exhaustion of CD4+ T-cells may also be involved in non-HIV-related mortality, independent of cardiometabolic or HIV-related factors.


|
| |
|
 |
 |
|
|