 |
 |
 |
| |
RISK FACTORS FOR HOSPITALIZATION IN PEOPLE WITH HIV AND COVID-19
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Lauren K . Barbera1, Kevin F. Kamis2, Mona H. Abdo1, Katie A. Kozacka1, Edward M. Gardner3, Samantha MaWhinney1, Sarah E. Rowan2, Kristine Erlandson1 1University of Colorado Anschutz Medical Campus, Aurora, CO, USA, 2Denver Public Health, Denver, CO, USA, 3Denver Health Medical Center, Denver, CO, USA
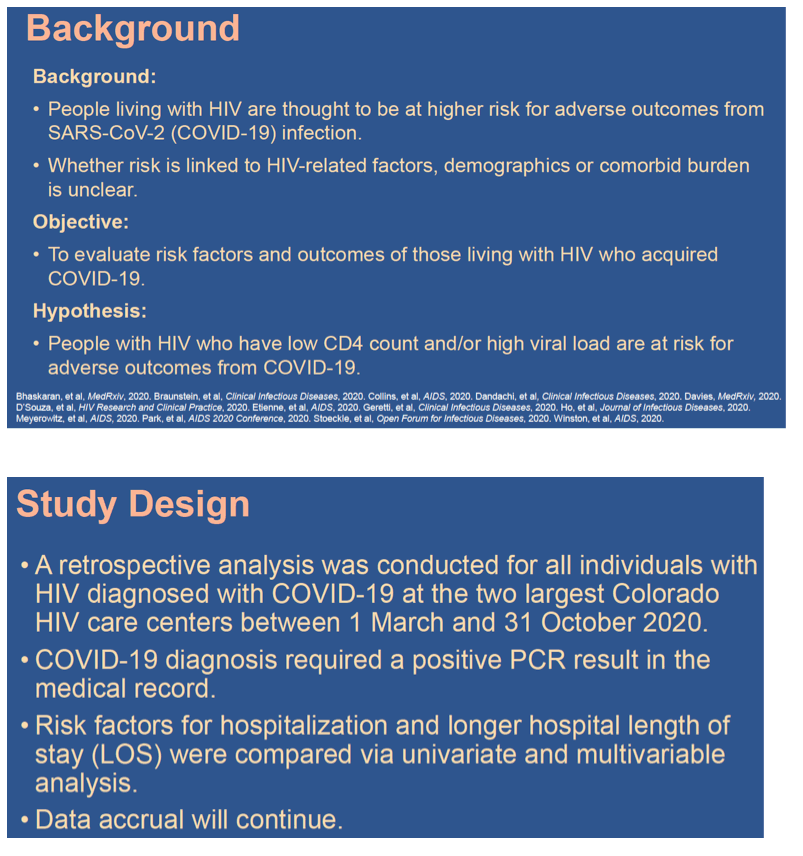
Background: People living with HIV are thought to be at higher risk for poor outcomes (including higher hospitalization and mortality rates) from SARS-CoV-2 (COVID-19) infection. Whether risk is linked to HIV-related factors, demographics or comorbid burden is unclear. We examine risk factors and outcomes of those living with HIV who acquired COVID-19 and received care within two large healthcare systems in Denver, CO.
Methods: A retrospective analysis was conducted for all individuals with HIV diagnosed with COVID-19 at the two largest Colorado HIV care centers between 1 March and 31 October 2020. COVID-19 diagnosis required a positive PCR result; HIV diagnosis was extracted from the medical record. Risk factors for hospitalization and longer hospital length of stay (LOS) were examined and compared via univariate and multivariable analysis.
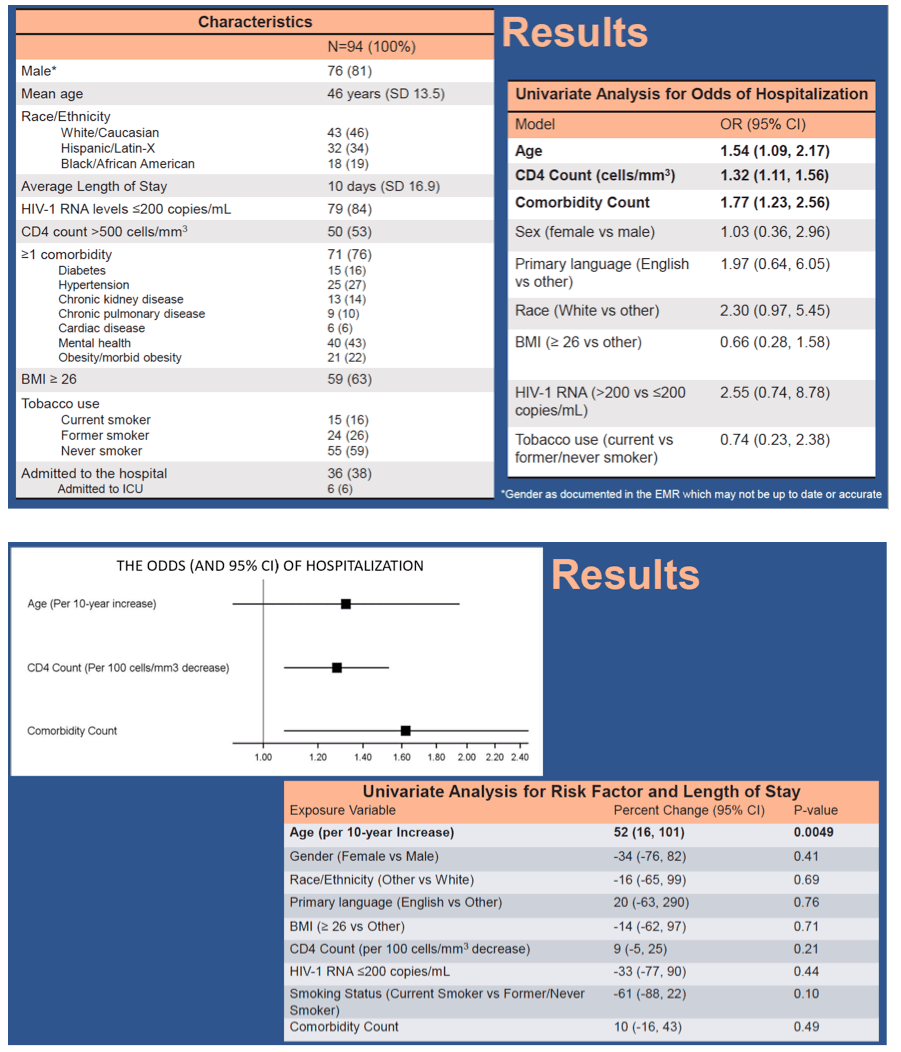
Results: Among 94 patients, 81% were male, with a mean age of 46 (SD 13.5) years. The majority had HIV-1 RNA levels <50 copies/mL (87%) and CD4 count >500 cells/mm3 (55%). Most (75%) had ≥1 comorbidity; 64% were overweight or obese. 39% of patients were admitted to the hospital (17% to intensive care). Increased odds of hospitalization were associated with increased age, lower CD4 count, and increased number of comorbidities (including diabetes, hypertension, chronic kidney disease, chronic pulmonary disease, cardiac disease, mental health concerns, and obesity) (Table). In multivariable analyses, only lower CD4 count (OR 1.28) and comorbidity count (OR 1.62) remained significant. Among hospitalized patients, longer LOS was univariately associated with age (52% longer LOS per 10 year age increase [95% CI 16,101%], p=0.004) but not CD4 count (-8%, [95% CI -18, 5%] % change in LOS per 100 cell/mm3 increase, p=0.21), HIV-1 viral load ≥200 copies/mL (-33% [95% CI -77, 90%], p=0.44), or comorbidity count (10% [95% CI -17, 43%] change in LOS per additional comorbidity, p=0.49). Sensitivity analyses excluding 9 patients hospitalized for non-COVID reasons provided similar findings.
Conclusion: Lower CD4 count was associated with an increased risk of hospitalization among patients with concurrent HIV and COVID-19, suggesting that successful HIV treatment remains a key component to decreasing HIV- related morbidity.

|
| |
|
 |
 |
|
|