 |
 |
 |
| |
CSF MARKERS OF AD-RELATED PATHOLOGY AND MEMORY DEFICITS IN OLDER PEOPLE WITH HIV
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Judith D . Lobo1, Erin E. Sundermann1, Mark W. Bondi1, Ben Gouaux1, Cristian L. Achim1, Scott Letendre1, David J. Moore1
1University of California San Diego, La Jolla, CA, USA
Background: Older people with HIV (PWH) are at-risk for Alzheimer's disease (AD) and its precursor, amnestic mild cognitive impairment (aMCI). Identifying aMCI among PWH is challenging because memory impairment is also common in HIV-associated neurocognitive disorders (HAND). The neuropathological hallmarks of aMCI/AD are amyloid-42 (Aβ42) plaque and phosphorylated tau (p-tau) accumulation. We assessed whether the AD pathology markers of lower Aβ42 levels and higher p-tau and p-tau/Aβ42 ratio levels in the cerebrospinal fluid (CSF) could help identify early stages of aMCI among older PWH with high rates of HAND. We assessed the relationship of these AD CSF biomarkers to learning and memory performance versus other neurocognitive domains that are more commonly-impaired in HAND than in aMCI (motor and speed of information processing).
Methods: Participants included 31 PWH aged 50-68 years (84% male, 58% White) from the National NeuroAIDS Tissue Consortium (NNTC). CSF Aβ42 and p-tau were measured by commercial immunoassay. The analyzed neurocognitive domains included: learning and memory (Hopkins Verbal Learning Test-Revised and Brief Visuospatial Memory Test-Revised), speed of information processing (WAIS-III Digit Span) and motor (Grooved Pegboard Test). Linear regressions examined the relationship between neurocognitive scores and levels of CSF p-tau, Aβ42, and p-tau/Aβ42 ratio while adjusting for demographics, apolipoprotein-E ε4 genotype, HIV disease characteristics (nadir CD4, antiretroviral treatment status) and clinical comorbidities (e.g., substance use disorders).
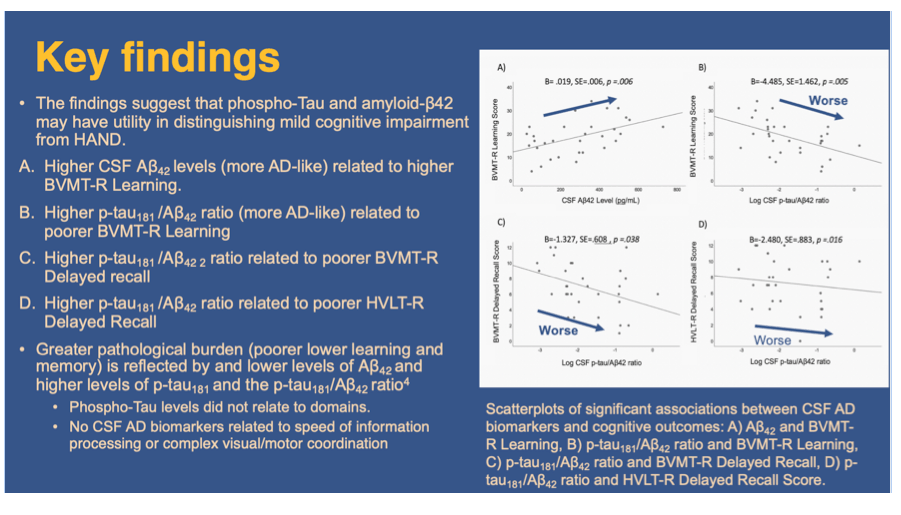
Results: Forty-five percent of participants were diagnosed with HAND. Lower CSF Aβ42 levels related to poorer BVMT-R Learning (p=.006; Figure 1). Higher CSF p-tau/Aβ42 ratio related to poorer BVMT-R Learning, and BVMT-R and HVLT-R Delayed Recall (ps<.05). CSF p-tau levels did not relate to neurocognitive test scores. Motor and speed of information processing were not significantly related to AD CSF biomarkers.

Conclusion: The specificity of the relationship between CSF AD biomarkers and learning/memory performance suggests that these biomarkers, particularly p-Tau/Aβ42 ratio, have utility in identifying aMCI/AD-related cognitive deficits amid a background of HAND. Additional research is needed to fully identify, among PWH, who is at greatest risk for aMCI/AD and whether there is increased risk for aMCI/AD among PWH as compared to those without HIV.

|
| |
|
 |
 |
|
|