 |
 |
 |
| |
ASSOCIATION BETWEEN NEWER ANTIRETROVIRALS
AND INCREASE IN BODY MASS INDEX IN RESPOND
|
| |
| |
CROI 2021 March 6 Reported by Jules Levin
Loveleen Bansi-Matharu, for RESPOND
University College London, London, UK
Background: Weight gain has been related to use of tenofovir alafenamide (TAF) and integrase inhibitor (InSTIs), particularly dolutegravir (DTG). However, the independent effects of individual contemporary antiretrovirals (ARVs) on weight gain are not fully understood. We investigated associations between pre-specified clinically significant increase (>7%) and extreme increase (>30%) in body mass index (BMI) and contemporary ARV use.
Methods: For all ARVs received on/after RESPOND study entry (median 2013), BMI changes from pre-ARV BMI levels (baseline) were considered at each BMI measured whilst on the ARV. The effect of each ARV was isolated by assuming each ARV was independent of other ARVs being received concomitantly. Logistic regression using generalised estimating equations to account for clustering was used to identify individual ARVs that were associated with first occurrence of >7% and >30% increase in BMI from pre-ARV BMI. Analyses were adjusted for time on ARV, pre-ARV BMI, demographics, geographical region, CD4 count, viral load, smoking status, diabetes, dyslipidaemia, hypertension, viral hepatitis, and clinical events at baseline. Analyses were also stratified according to receiving DTG with/without TAF and TAF with/without DTG.
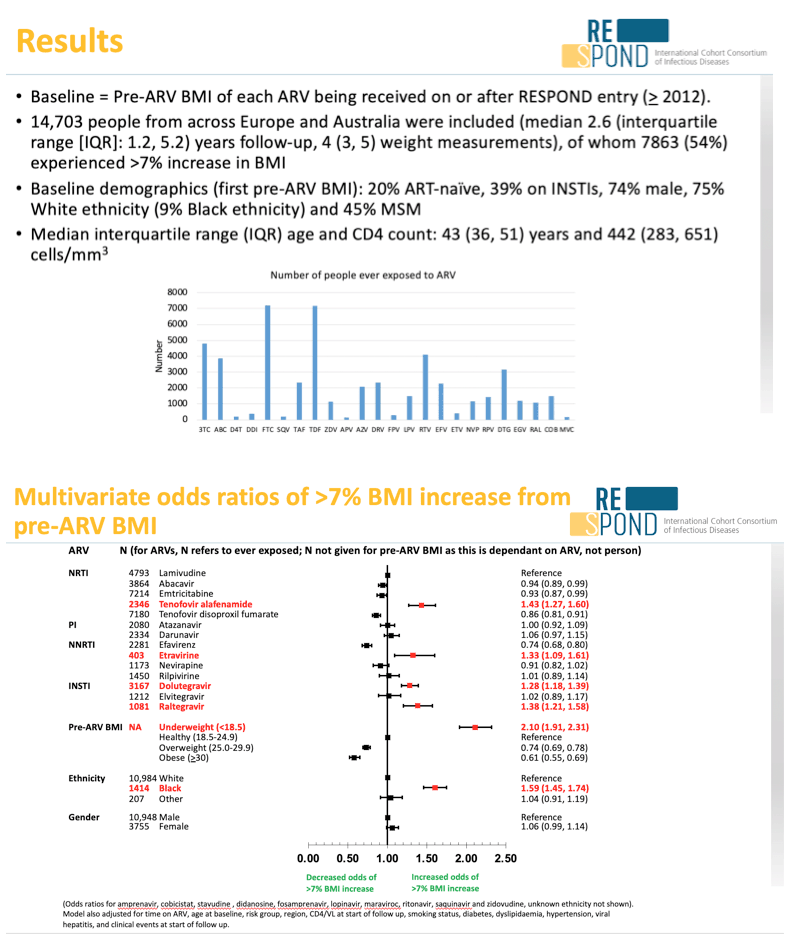
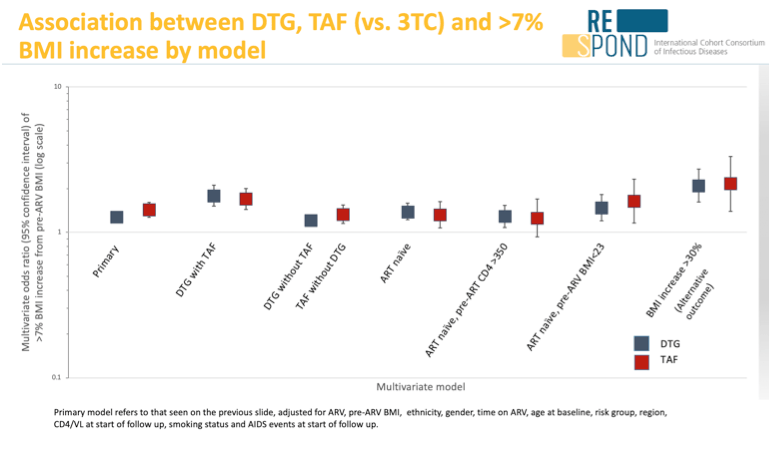
Results: 14703 people were included (median 2.6 years follow-up), of whom 7863 (54%) had >7%, and 749 (5%) >30%, BMI increase. At baseline 20% were ARV-naïve, 39% on InSTIs, 74% were male, 75% of white ethnicity and 45% MSM. Multivariate odds ratios (ORs) are shown in Figure 1. Use of DTG, raltegravir (RAL) and TAF, low pre-ARV BMI and black ethnicity were significantly associated with >7% BMI increase. ORs for people on both DTG and TAF (DTG 1.73 [1.47, 2.04], TAF 1.63 [1.38, 1.93] vs. lamivudine (3TC)) were higher than those taking DTG without TAF (1.20 [1.09, 1.31]) or TAF without DTG (1.30 [1.12, 1.50]). Both ARVs were independently associated with >30% BMI increase (DTG 2.02 [1.55, 2.62], TAF 2.09 [1.35, 3.22] vs. 3TC). When restricting to the 1476 naïve patients with pre-ART CD4 count>350, compared to 3TC, DTG was associated with >7% BMI increase (DTG 1.32 (1.11, 1.57)), but TAF was not (1.30 (0.96, 1.76)).
Conclusion: Low pre-ARV BMI was the strongest independent predictor of >7% BMI increase. Use of DTG, RAL and TAF were associated with significant BMI increase compared to 3TC independent of pre-ARV BMI and time on ARVs. Combined rather than individual use of TAF and DTG was associated with greater risk of BMI increase.


|
| |
|
 |
 |
|
|