 |
 |
 |
| |
A SURVEY-BASED PILOT STUDY TO ASSESS
THE EFFECTS OF COVID-19 ISOLATION ON OLDER PLWH
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Lauren Smith1, Hannah Walsh1, Jennifer Chiarella1, Julian Weiss1, Serena S. Spudich1, Shelli F. Farhadian1
1Yale University, New Haven, CT, USA
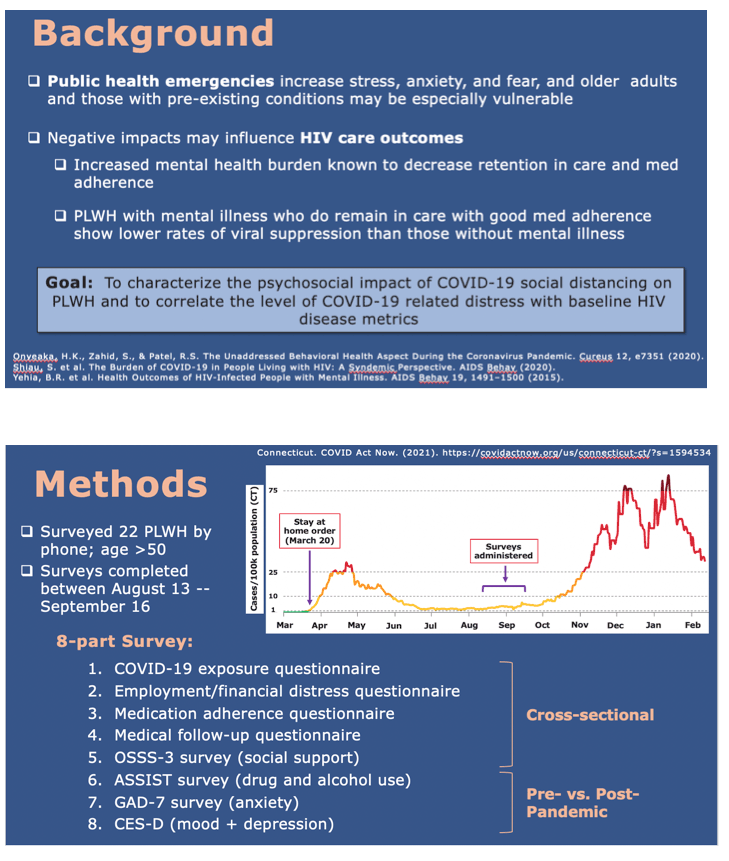
Background: Public health emergencies increase stress, anxiety, and fear, and older adults and those with pre-existing conditions may be especially vulnerable. We used a survey-based pilot study to explore the psychosocial impact of COVID-19 on older PLWH and correlate the level of COVID-19 related distress with baseline HIV disease metrics.
Methods: Participants were PLWH > age 50 who had previously (2017-2020) enrolled in the HARC HIV biorepository study at Yale. 48 PLWH were contacted and 22 participated in this study, conducted Aug-Sep 2020. An 8-part survey was administered to inquire about COVID-19 exposure, financial distress, medication adherence/medical follow-up, social support, substance use, and mood symptoms (Table 1). Cross-sectional analysis was performed on results at the time of survey administration, and longitudinal analysis was performed to compare anxiety (GAD-7), alcohol/drug use (ASSIST), and depression (CES-D) to baseline values obtained pre-pandemic (median 1.3 years prior).
Results: Participant demographics are reported in Table 1. 2 participants reported having been diagnosed with COVID-19, 1 of whom had a known COVID-19 positive contact. 68% of participants were retired and reported no changes to their work due to COVID-19, and most reported moderate (4.1 on scale of 0-7) financial distress. Most reported excellent medication adherence, with 77% reporting no missed doses. 95% stated they felt "very well supported" by their primary HIV care providers, with 18% saying their care was improved during COVID-19. Only 18% felt their care was "somewhat worse." Most participants also scored highly on the social support scale, with an average score of 11 out of 14. There were no significant differences between pre-pandemic and current scores for anxiety, alcohol/drug use, and depression, and there was no correlation between baseline HIV metrics and current level of distress. However, there was an association between COVID-19-associated worsening in GAD-7 score and a history of substance use disorder (p = 0.02).
Conclusion: These results suggest that overall, most participants were doing well with excellent medication adherence and no significant changes in scores for anxiety, depression, and substance use, but that older PLWH with a history of substance use disorder had a greater risk for increased anxiety during COVID- 19. These findings can help identify groups who may be the most at-risk to experience distress from a second wave of COVID-19 and put support measures in place.


|
| |
|
 |
 |
|
|