 |
 |
 |
| |
HEPATITIS B SEROPROTECTION AMONG YOUNG ADULTS LIVING WITH PERINATALLY ACQUIRED HIV
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Florence Bada1, Patrick Ryscavage1
1University of Maryland, Baltimore, MD, USA
Background: The development of protective antibodies against hepatitis B virus (HBV) following vaccination is variable across the HIV population, and has been studied primarily in older adults. HBV seroprotection among young adults with perinatally-acquired HIV has not been examined. We sought to describe HBV seroprotection among young adults with both perinatally acquired HIV (PHIV) and non-perinatally acquired HIV (NPHIV).
Methods: We conducted a retrospective chart review of HBV vaccination history and HBV serology results among young adults (≥18 years) with both perinatally acquired HIV and non-perinatally acquired HIV. Bivariable analysis was conducted using Pearson's chi-square, Fisher's exact and t-tests as appropriate to compare the distribution of covariates between PHIV and NPHIV. Multivariable logistic regression was used to determine the odds of having a reactive HBV surface antibody (HBsAb) in PHIV as compared to NPHIV adjusted for CD4 nadir, HIV RNA proximate to the HBsAb test and documentation of HBV vaccination. HBV seroprotection was defined as a documented HBsAb ≥10 mIU/ mL. Patients with evidence of current or past HBV infection were excluded from the analysis.
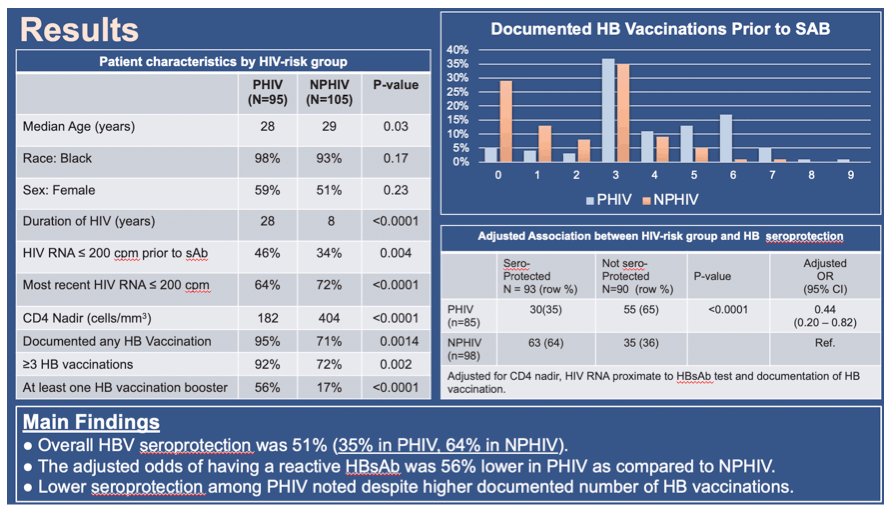
Results: Two hundred individuals (N=95 PHIV, N=105 NPHIV) aged 18-36 years had a recorded HBV serology result (Table 1). The cohort was predominantly Black (96%) and female (55%). PHIV were significantly younger (median age 28 vs. 29 years), had been HIV-infected for longer (28 vs 8 years), had a lower median CD4 nadir (182 vs 404 cells/mm3), and were more likely to have achieved HIV viral suppression prior to HBsAb test. In addition, PHIV received more documented HBV vaccine boosters, and were more likely to have documented completion of a 3 shot series (mean # HBV vaccinations: 4.4 among PHIV, 3.1 among NPHIV). Overall HBV seroprotection was 51%, and was lower among PHIV (37.9%) compared to NPHIV (65%). By multivariable logistic regression, the adjusted odds of having a reactive HBsAb was 60% lower in PHIV adults as compared to NPHIV adults (OR .40, 95% CI 0.20-0.82).
Conclusion: Hepatitis B seroprotection was low in this cohort of young adults with HIV infection. Adults with perinatally-acquired HIV were less likely to achieve seroprotection despite a high number of total documented vaccinations across time. Providers should assess HBV seroprotection in all HIV-infected young adults, with vigilant attention to seroresponse among PHIV. Novel approaches to HBV immunization should be sought in this population.



|
| |
|
 |
 |
|
|