 |
 |
 |
| |
DEMENTIA INCIDENCE AMONG ART-TREATED PEOPLE WITH HIV IN A PRIMARY CARE SETTING
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Jennifer O . Lam1, Paola Gilsanz1, Catherine Lee1, Craig E. Hou2, Wendy Leyden1, Derek D. Satre3, Jason Flamm4, William J. Towner5, Michael A. Horberg6, Michael J. Silverberg1
1Kaiser Permanente Northern California, Oakland, CA, USA, 2Kaiser Permanente Northern California, South San Francisco Medical Center, South San Francisco, CA, 3University of California San Francisco, San Francisco, CA, USA, 4Kaiser Permanente Northern California, Sacramento Medical Center, Sacramento, CA, USA, 5Kaiser Permanente Southern California, Pasadena, CA, USA, 6Kaiser Permanente Mid- Atlantic States, Rockville, MD, USA
Background: People aging with HIV may be at increased risk for dementia. However, few studies have compared the incidence of dementia between people with HIV (PWH) on antiretroviral therapy (ART) and people without HIV (PWoH) in primary care.
Methods: We conducted a cohort study of individuals aged ≥50 years who were members of Kaiser Permanente health plans in Northern California, Southern California, and Mid-Atlantic States (Maryland, Virginia, Washington D.C.) between 2000 and 2016. PWH and PWoH were frequency-matched 1:10 by age, sex, race/ethnicity, medical facility, and calendar year at baseline. We excluded PWH without an ART prescription fill in the year before baseline. Incident all-cause dementia diagnoses were identified in electronic health records using International Classification of Diseases codes confirmed via chart review in ∼300 randomly selected patients. Dementia incidence was evaluated by HIV status using Poisson regression models adjusted for period (2000-2004, 2005-2009, 2010-2014, 2015-2016), age (50-59, 60-69, ≥70 years), sex, race/ ethnicity (White, Black, Hispanic, Other), and healthcare utilization (outpatient visit frequency in the year before baseline). An overall model adjusted for all covariates. Subsequent adjusted models were stratified by period, age, sex, and race/ethnicity.
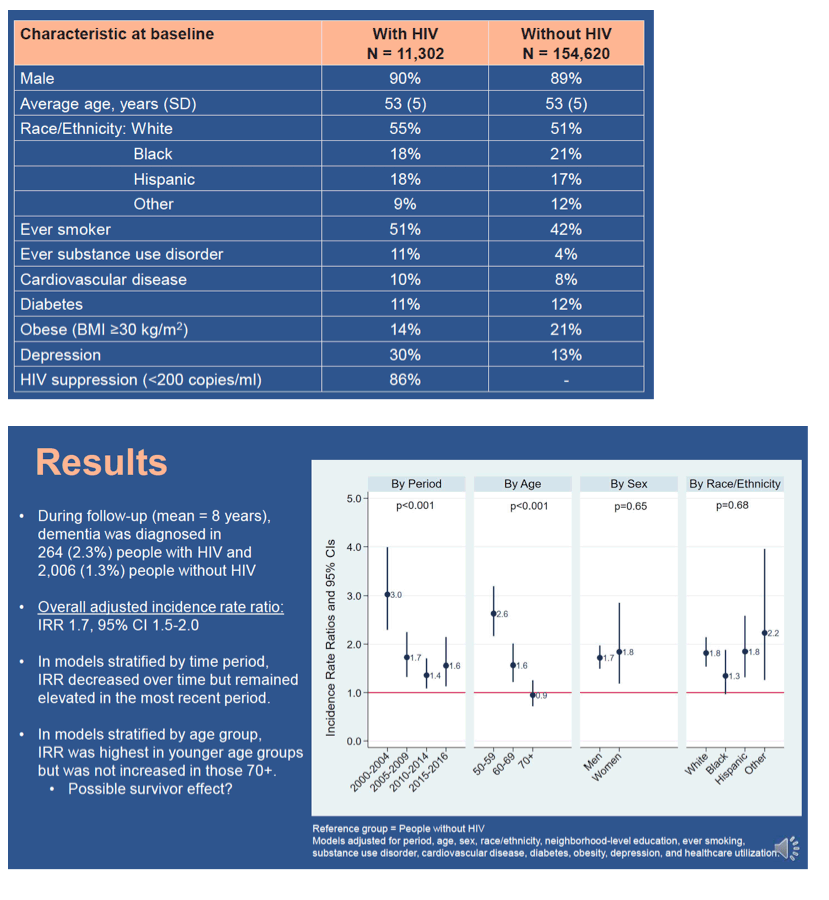
Results: The study included 11,302 PWH and 154,620 uninfected individuals (mean baseline age=53 years, 11% female; 82% of PWH with HIV RNA<200 copies/ml). During follow-up (mean=8 years), 264 PWH and 2,006 PWoH developed dementia.
Crude incidence of dementia was 4.4 (95% CI=3.9-4.9) and 2.1 (95% CI=2.0-2.2) per 1,000 person-years in PWH and PWoH, respectively (incidence rate ratio [IRR]=2.0, 95% CI=1.8-2.3).
After covariate adjustment, incidence remained higher in PWH (IRR=1.9, 95% CI=1.7-2.2). In models stratified by age, IRR was highest in younger age groups (age 50-59, IRR=3.3, 95% CI=2.7-3.9; age 60-69, IRR=1.7, 95% CI=1.3-2.1) but normalized in those age ≥70 (IRR=1.0, 95% CI=0.7-1.3) - could be due to survival affect or that new diagnoses occurs at younger ages, people >70 " Ould have a greater burden of dementia in older age because of their younger age at diagnosis". In models stratified by period, IRR decreased over time but remained elevated among PWH in the most recent (2015-2016) period (IRR=1.7, 95% CI=1.2-2.3). There were no significant differences in incidence across sex and race/ethnicity strata.
Conclusion: Despite ART use, dementia incidence is higher among PWH compared with PWoH and is diagnosed at younger ages. Further research is needed to determine factors contributing to age-specific patterns and continued elevated dementia incidence among ART-treated PWH.


|
| |
|
 |
 |
|
|