 |
 |
 |
| |
WEIGHT GAIN AMONG PWH WHO SWITCH TO ART-CONTAINING InSTIs OR TAF
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Frank Palella1, Qingjiang Hou2, Jun Li3, Jonathan Mahnken4, Kimberly J. Carlson2, Marcus Durham3, Douglas Ward5, Jack Fuhrer6, Ellen M. Tedaldi7, Richard Novak8, Kate Buchacz3
1Northwestern University, Chicago, IL, USA, 2Cerner Corporation, Kansas City, MO, USA, 3Centers for Disease Control and Prevention, Atlanta, GA, USA, 4University of Kansas Medical Center, Kansas City, KS, USA, 5Dupont Circle Physicians Group, Washington, DC, USA, 6Stony Brook University, Stony Brook, NY, USA, 7Temple University, Philadelphia, PA, USA, 8University of Illinois at Chicago, Chicago, IL, USA
Background: ART-associated weight changes among persons with HIV (PWH) whose first InSTI exposure is via an ART switch regimen require further long- term study in routine HIV care.
Methods: We analyzed 2007-2018 medical records data of patients who were InSTI-naive and virally suppressed (VS) for ≥ 1 year on non-InSTI-based ART, switched ART and remained VS. Patients were prescribed InSTI- or non-InSTI- based ART for ≥ 6 months, had ≥ 2 body mass index (BMI) values in the year before switch and ≥ 1 after. We analyzed weight change (BMI, presuming height was stable) before and after switch using generalized linear mixed effects models (GLMM), and estimated relative contribution of InSTI- and TAF- containing ART to BMI gain by contrasting GLMM-estimated slopes.
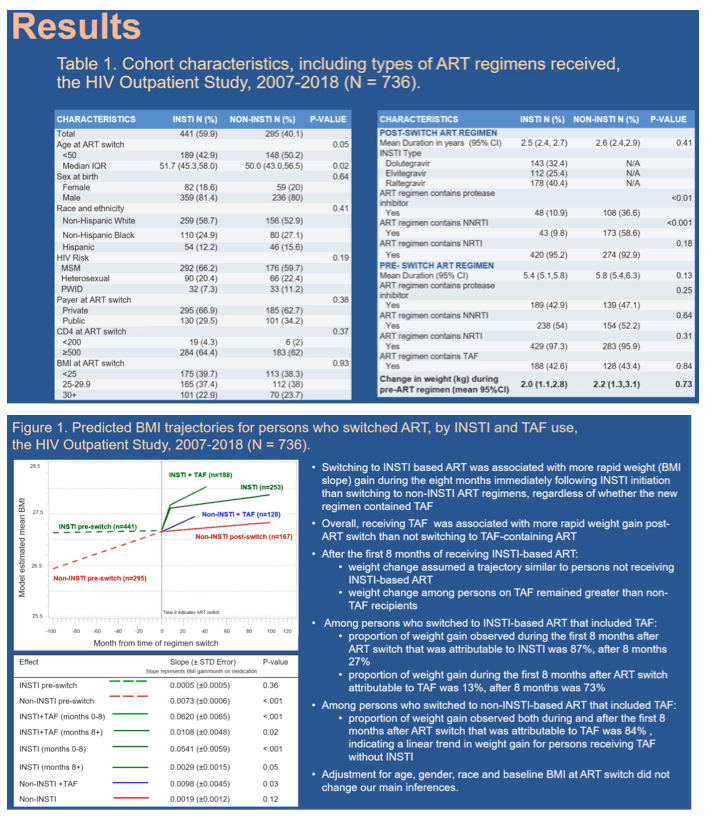
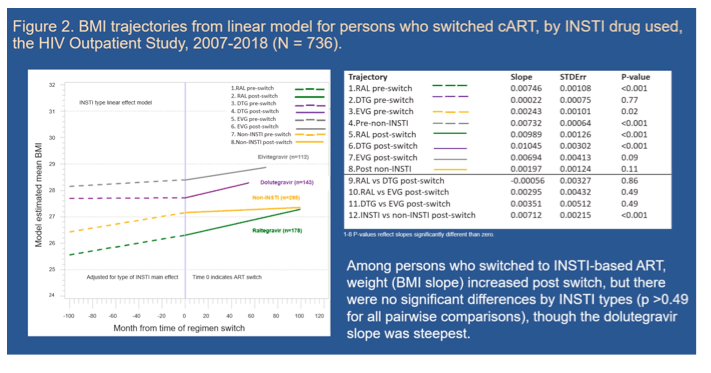
Results: Among 736 persons (with 5,316 person-years of observation), 441 (60%) switched to InSTI-based ART. Proximal to time of switch, both groups (InSTI vs non-InSTI) had similar CD4 cell count (634 vs. 626 cells/μL, P=0.85) and median BMI (23.0 vs. 24.0 kg/m2, P=0.62). Of InSTI-based ART regimens, 236 (54%) included raltegravir, 112 (25%) elvitegravir, and 143 (32%) dolutegravir. In GLMM, monthly rate of BMI increases post-switch was faster for InSTI-based than non-InSTI based ART (rate difference ± stderr: 0.0525 ± 0.006, p<0.001) [0.041, 0.064 95% CI]. There was an inflection point for BMI changes at 8 months post switch and the slopes were similar according to TAF use (Table 1). Among persons receiving InSTI-based ART with TAF, during the first 8 months 87% of weight gain (BMI change) was associated with InSTI and 13% with TAF; after 8 months post-ART switch, these estimated contributions were 27% and 73%, respectively. For non-InSTI TAF-based ART, 84% of weight gain was associated with TAF both during and after the first 8 months post switch. Older age and higher baseline BMI but not sex or race/ethnicity were associated with more rapid weight gain. BMI changes were not statistically different post-switch by type of InSTI.
Conclusion: Among VS persons who switched ART, both InSTI and TAF use were independently associated with weight gain. During the first 8 months post-switch, the rate of weight gain was greatest and mostly associated with InSTI use; after that, continued gradual weight gain was mostly associated with TAF use. These data help define the individual contribution, magnitude, and duration of effect upon weight gain of InSTI and TAF use.

|
| |
|
 |
 |
|
|