 |
 |
 |
| |
CROI 2021 Highlights
|
| |
| |
By Christina K. Psomas, M.D.
European Hospital Marseille, Marseille, France
Caterina Prelli Bozzo (Ulm University Medical Center) inaugurated the SARS-CoV-2 vs host session, explaining how the interferon-induced transmembrane (IFITM) protein family who are known viral restriction factors (influenza, HIV, zika, corona pseudotypes), may promote SARS-CoV-2 entry in cells (Abstract 112). Indeed, even if overexpressed IFITMs blocked SARS-CoV-2 infection in transduced HEK293T cells in a dose-dependent manner, endogenous expression of IFITMs in Calu-3 (lung cell line) and SAEC (primary small airway epithelial cells) promoted genuine SARS-CoV-2 infectionoV-2 entry. Moreover, IFITMs interacted directly with the SARS-CoV-2 spike and antibodies directed against the intramembrane region of the IFITMs or IFITM-derived peptides could inhibit SARS-CoV-2 replication and thus IFITMs can be novel targets for SARS-CoV-2 inhibition.
http://www.croiwebcasts.org/console/player/48131?mediaType=slideVideo&
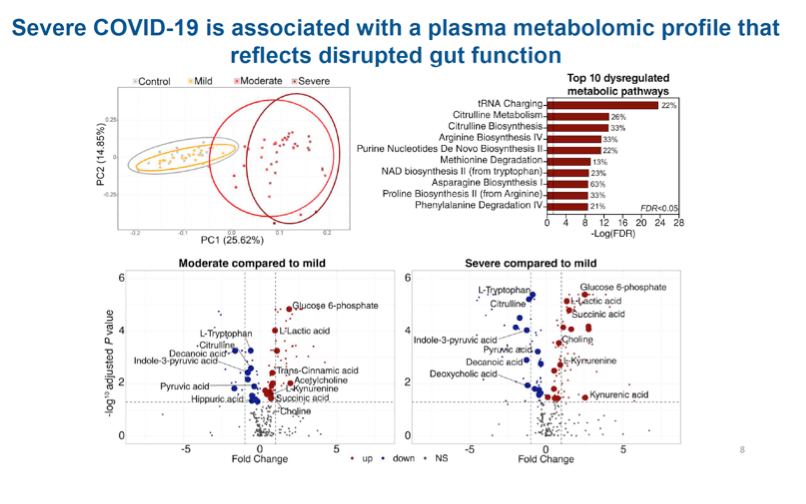
Leila B. Giron (The Wistar Institute, Philadelphia, PA, USA) explored if a vicious cycle exists between lung, gut, and inflammation (Gut-Lung Axis) contributing to COVID-19 severity (Abstract 114). Researchers compared 60 SARS-CoV-2 positive vs 20 age-matched SARS-CoV-2 negative subjects first concluding that COVID-19 severity was associated with tight junctions' permeability (higher levels of zonulin). Zonulin is both a marker and a driver of gut permeability, because it is the only non-physiological regulator of intestinal tight junctions. In this cohort COVID-19 severity was also associated with LPS-binding protein (LBP) and beta-glucan plasma levels respectively expressing microbial and fungal translocation, as well as soluble CD14 (sCD14) and MPO levels expressing monocyte/neutrophil inflammation. Markers of intestinal barrier integrity strongly correlated with many markers of inflammation and immune activation, including IL-6, CRP and D-dimers. Moreover, severe COVID-19 was associated with a plasma metabolomic profile reflecting disrupted gut function, because dysregulated metabolic pathways were all related to amino-acid metabolism. More specifically, citrulline (marker of intestinal function and absorption) exposed reduced plasma levels, while markers of microbial dysbiosis (succinic acid and kynurenine/tryptophane ratio) increased in the plasma of the moderate and severe group. All these markers were also associated with systemic inflammation (positive correlation with succinic acid and kynurenine/tryptophane ratio, negative correlation with citrulline). Severe COVID-19 was also associated with disrupted plasma lipidome and glycome in a manner compatible with gut dysfunction, even if a causal relationship between them was not yet established.
http://www.croiwebcasts.org/console/player/48133?mediaType=slideVideo&
Minami Tokuyama (Icahn School of Medicine at Mount Sinai, New York, NY, USA) tried to collect evidence of in vivo SARS-CoV-2 intestinal infection in 29 participants undergoing clinically indicated endoscopic procedures and having a concurrent or past diagnosis of COVID-19 (Abstract 115). The average age of the recruited participants was 51.5 years (+/- 19.9) and 19 (65%) of these patients were male. The average number of days from last positive nasopharyngeal swab was 51 (+/- 44.8) days and the average number of days from symptom onset to procedure was 56.6 (+/- 54.72) days. Seven (24.1%) out of the 29 patients were PCR+ within 3 days of the procedure. Most of these patients had mild disease during their acute COVID-19 illness (18 patients or 62.1%), 6 (20.7%) of them had severe disease and 8 (27.6%) of them had COVID-19 associated gastro-intestinal symptoms. SARS-CoV-2 antigen and presumptive viral particles were identified by immunofluorescence in small intestinal biopsies from 12/25 COVID-19 patients. At the stage examined, large number of cells with detectable antigen appeared to be intestinal goblet cells (MUC2+), but the type of cell infected may be stage dependent. Despite the detection of viral products, inflammation was mild or undetectable in most cases. Detection of viral products did not correlate with GI symptoms in the acute setting in this cohort. Finally, viral antigen could continue to be detected in intestinal tissue up to 7 months following symptom resolution.
http://www.croiwebcasts.org/console/player/48134?mediaType=slideVideo&
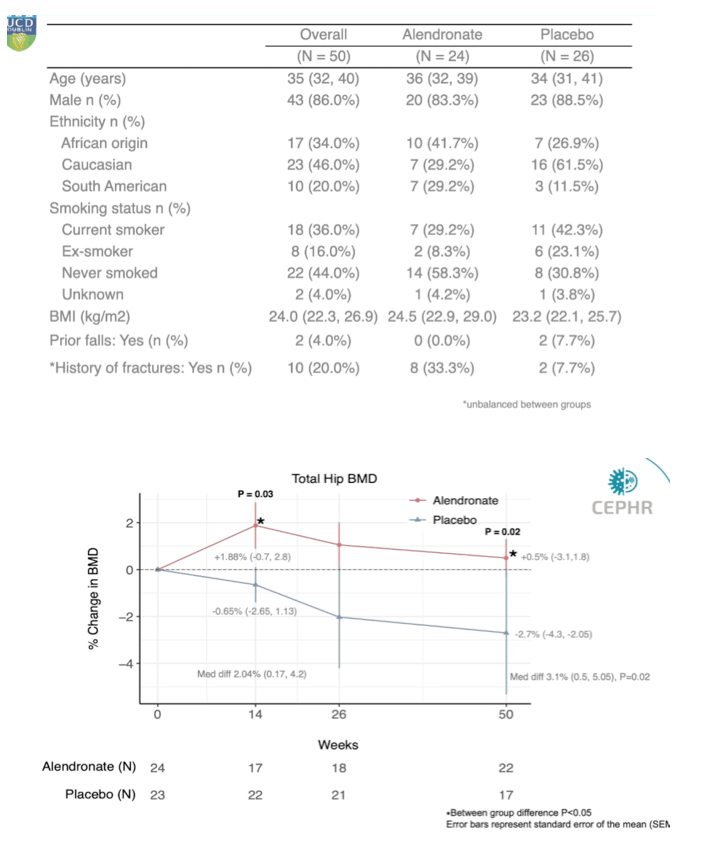
Tara McGinty (University College Dublin) introduced the complications of HIV session, presenting a clinical trial about how short-course alendronate could prevent ART-associated bone loss on behalf of the APART study group (Abstract 96). Knowing that ART initiation has consistently been associated with 2-6% loss of bone mineral density (BMD) in the first 48 weeks post-ART initiation, the study's primary aim was to determine if short-course generic oral alendronate could prevent bone loss associated with ART initiation in ART-naive PWH. The APART study was a multicenter, prospective, randomized, double-blind, placebo-controlled phase IV trial comparing generic oral alendronate vs placebo for a total of 14 weeks. 50 participants were well matched with no significant differences in demographics and the majority of participants were initiated with an InSTI as their third agent. It is worth noting that there were more current or former smokers in the placebo group. There was no difference regarding the BMD at either side between the groups at baseline. When examining the primary endpoint of percentage change in BMD at week 50 at total hips between the groups, they found that participants receiving alendronate had an 0.5 % gain in total hip BMD compared to a 2.7% loss in the placebo arm, resulting in a significant difference of 3.1% between the groups in total hip BMD at week 50. At the lumbar spine region participants receiving alendronate had a significantly higher BMD at week 14 and 26 (respectively 2.4% and 3.1%) but preserved lumbar spine BMD did not persist till week 50. Although the alendronate arm had a smaller decline in lumbar spine BMD compared to the placebo group, the difference in BMD of 2.3% between the two groups was not statistically significant. Alendronate was overall well tolerated during the study. Despite limitations regarding the small sample size, limited female representation and lack of alternative non InSTIs 3d agents, generic alendronate seemed to be an easily accessible option particularly in resource limited settings.
http://www.croiwebcasts.org/console/player/48015?mediaType=slideVideo&
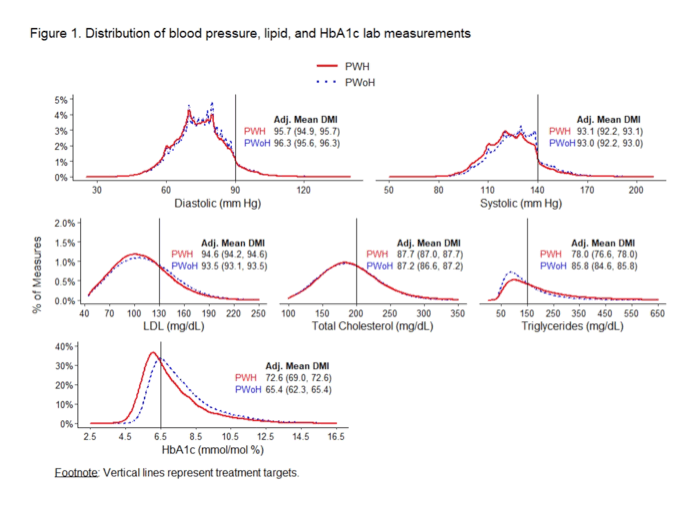
Michael J. Silverberg (Kaiser Permanente Northern California) presented results about prevention of cardiovascular disease in persons with and without HIV (Abstract 97). Researchers first measured the management below treatment targets of hypertension, dyslipidemia and diabetes mellitus. Disease Management Index (DMI) is a measure of how effectively a condition is managed, considering both time and level of control. Participants of this cohort study included Kaiser Permanente (KP) members with HIV (N=8,285) (PWH) and age-, sex-, race/ethnicity-matched members without HIV (N=170,517) (PWoH), excluding individuals with prevalent CVD. Regarding risk factor management, similar dyslipidemia, hypertension and diabetes control were observed by HIV status, while there was evidence for slightly worse triglycerides and better HbA1c control for PWH. Regarding CVD risk, PWH had 26% higher CVD risk when there was no history of dyslipidemia, hypertension and diabetes, and there was no difference in CVD risk by HIV status among those with adequate dyslipidemia and diabetes control. Finally, CVD risk was 35% higher when PWH had adequate hypertension control, and 91% higher in PWH with inadequate hypertension control (specifically systolic blood pressure).
http://www.croiwebcasts.org/console/player/48016?mediaType=slideVideo&
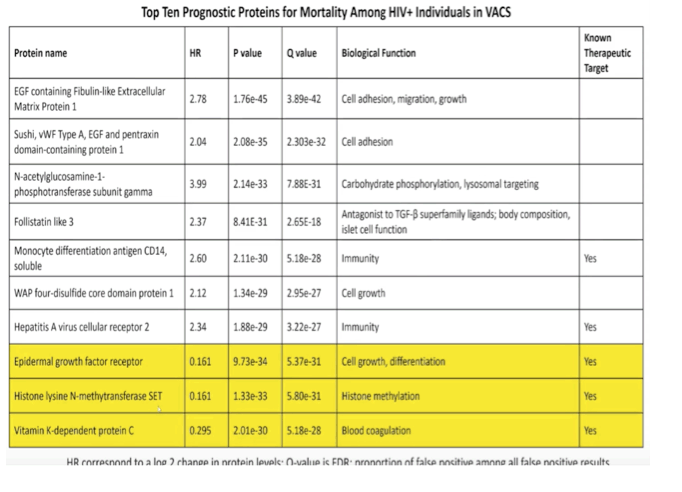
Priscilla Hsue (University of California San Francisco) used large-scale proteomics to identify novel protein biomarkers that were associated with total mortality events in PWH, compared to HIV-related factors, inflammatory and coagulation markers and components of VACS Index (Abstract 99). They performed a longitudinal prospective observational study of 1525 PWH and 853 uninfected Veterans within the time period of 2005-2019. Novel unique proteins were identified that were negatively or positively associated with mortality in PWH. A risk score based on 10 proteins provided moderately good discriminatory accuracy, despite heterogeneous causes of death in this population. Proteins remained predictive of mortality despite addition of HIV-associated characteristics, of traditionally measured inflammatory/coagulation markers and of VACS Index components.
http://www.croiwebcasts.org/console/player/48018?mediaType=slideVideo&
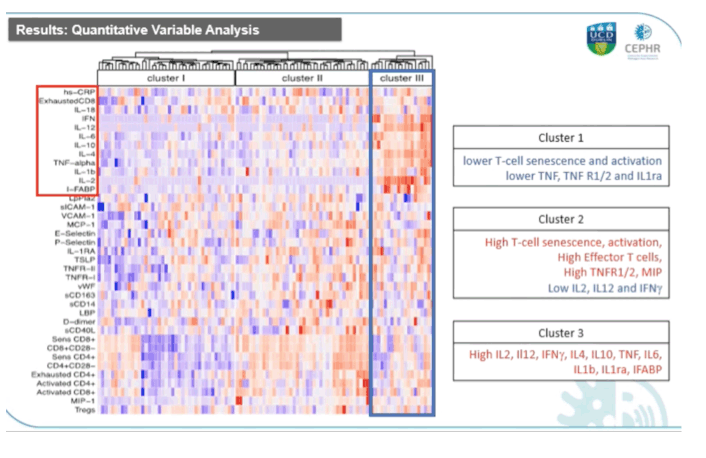
Padraig McGettrick (University College Dublin) presented results of the HIV UPBEAT CAD substudy about the inflammatory profile associated with subclinical Coronary Artery Disease (CAD) (Abstract 100). 101 participants were enrolled in the substudy of which 51 were PWH, and the two groups were globally matched apart from the rate of statins' use and level of HDL cholesterol that were statistically different. Following unsupervised hierarchical clustering analysis 3 biomarker derived distinct inflammatory clusters were identified: cluster I was characterized by overall lower T-cell senescence, activation and systemic inflammation markers, cluster II was characterized by high T-cell senescence, activation and inflammation markers and low Th1 driven biomarkers, and cluster III was characterized by increased systemic inflammatory and microbial translocation markers. Cluster demographics were overall similar with the exception of HIV status, because PWH were significantly over-represented in cluster II and under-represented in cluster I. Associations of inflammatory clusters with the radiological endpoints showed that overall, 36% of participants had evidence of subclinical CAD on CCTA imaging. In the unadjusted analysis cluster II and III displayed a stronger association with partially calcified plaque and mixed plaque and a weaker association with any coronary plaque and calcified plaque. Cluster III was the only cluster associated with both CAC Agatston and Calcium volume scores.
Adjustment by HIV status did not significantly alter the associations seen between clusters and CAD, suggesting that it is rather the inflammatory rather than the HIV status that drives these associations.
http://www.croiwebcasts.org/console/player/48025?mediaType=slideVideo&
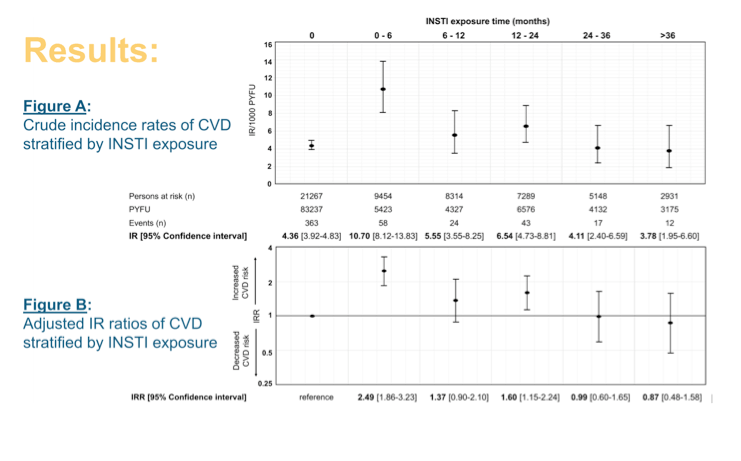
Bastian Neesgaard (CHIP, Dept of Infectious Diseases, Rigshospitalet, Copenhagen, Denmark) and the RESPOND study group assessed if exposure to integrase strand transfer inhibitors (INSTIs) was associated with an increased incidence in cardiovascular disease (CVD) (Abstract 488). RESPOND participants were INSTI naive followed from baseline (1st of January 2012) to the earliest of first CVD event, last follow-up or 1st of October 2018. Exposure to INSTIs was calculated following the D:A:D methodology and models adjusted for CVD risk factors, HIV characteristics and ARVs previously associated with CVD. Logistic regression examined odds of starting an INSTI (raltegravir [RAL], elvitegravir [EVG/c] and dolutegravir [DTG]) by D:A:D 5-year risk score. More than 21,000 individuals were included in this analysis of whom 46% (9,782) were exposed to an INSTI during follow-up. Overall, the majority of participants were white, of male gender and Western European origin, with MSM being the most frequent risk of HIV transmission. During a median of 6.3 years of follow-up (IQR 3.5-6.7) corresponding to 106,870 PYFU, 517 CVD events occurred giving an overall incidence rate of 4.9/1000 PYFU (CI 95%, 4.5-5.3). Myocardial infarctions were the most frequent occurring event (210 MIs, 162 strokes and 145 ICPs). Looking at the population stratified by those that did not experience an event vs those that did, the latter were older with a larger proportion of CVD risk factors at baseline, and a higher 5-year estimated D:A:D CVD risk score (46% vs 12%, p<0.001). When examining the odds of starting an INSTI by baseline 5-year estimated D:A:D CVD risk and compared to those with low risk, the odds of starting INSTIs were higher for higher risk score categories (moderate risk (1 - <5%): 1.11 [1.00-1.21], high risk (5 - <10%): 1.19 [1.05-1.35], very high risk (>10%): 1.05 [0.89-1.25]). Figure A shows the results regarding the crude unadjusted incidence rates of CVD stratified by INSTI exposure, demonstrating the increase in the IR of those who never exposed to those having 0-6 months exposure, while thereafter IR declined to the levels of those who were never exposed. In figure B are shown the IR ratios after adjustment for confounding factors, confirming the 2.5 times greater incidence of CVD within the first 6 months of INSTI exposure when compared to non-exposed group, regardless of underline CVD risk and HIV characteristics. Due to limited statistical power, there was no focus on individual INSTI drugs and ART-naive individuals. Due to the observational nature of the study, we cannot exclude the potential for channeling bias or residual confounding, the authors said.
http://www.croiwebcasts.org/console/player/47532?mediaType=slideVideo&
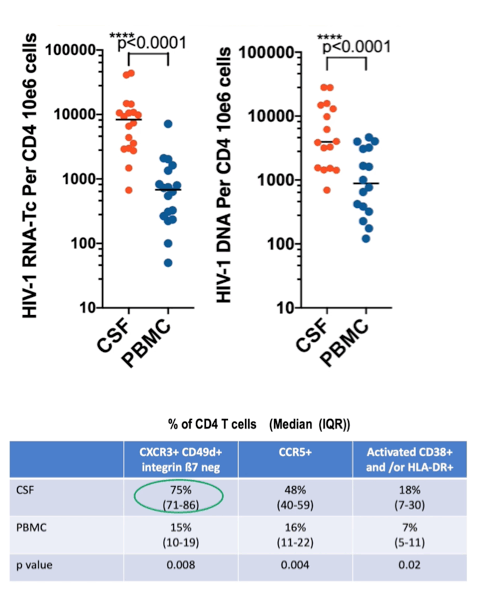
Kazuo Suzuki (St Vincent's Hospital, Sydney) presented data of his group about physio pathogenesis of HIV-associated neurocognitive disorders (HAND) despite prolonged suppressive ART (Abstract 162). Researchers tried to investigate if HAND is related to active HIV-1 transcription from the CNS reservoir without production of whole virions in 20 paired CSF and blood samples from virally suppressed patients in plasma (<50 cp/mL) and CSF (<80 cp/mL) enrolled in a prospective study of HIV-1 CNS latency biomarkers. Patients had a median age of 62 years, they were all male, and had a median nadir CD4 T cell count of 202 cells/mm3, and a median CD4+ T cell count at the time of analysis of 656 cells/mm3. Using the double-R assay (targeting the R region of LTR section) they detected cell-associated HIV transcription activity (ongoing reservoir activity) despite ART and this assay was 27 times more sensitive than real-time assay that detects cell-free virus in plasma and CSF.
HIV-1 RNA transcripts and HIV-1 DNA levels in CSF cells were significantly higher than in PBMC even after normalization of HIV-1 copy number by number of cells infected, suggesting that CSF is an HIV reservoir with high transcription activity despite ART. CSF cells were mainly represented by CD4- and CD8-T cells that were 20 times higher than monocytes cells. HIV-1 transcripts were quantified in CSF cells of 18/20 patients (90%), while HIV-1 DNA was quantified in cells of 16/20 patients (80%). Interestingly, HIV-1 transcript expression in CSF cells was highly correlated with HIV transcript levels in PBMC. Most of the CSF cells were memory CD4+ T cells expressing CXCR3, CD49d (integrin alpha 4) but lack for integrin beta 7 and this type of cells were highly enriched in CSF compared to PBMC. Most of these memory cells were activated CCR5+ and were likely the source of HIV-1 RNA transcripts, while monocytes seemed to be less important. Although there were insufficient data for correlation analysis of HIV-1 RNA transcript levels in CSF CD4+ T cells and neuropsychological tests, it seemed to be an inverse correlation between HIV-1 transcripts and neuronal integrity reflected by brain metabolites (FWM-NAA and PCC-NAA) in the MRI/S analyses.
http://www.croiwebcasts.org/console/player/48343?mediaType=slideVideo&
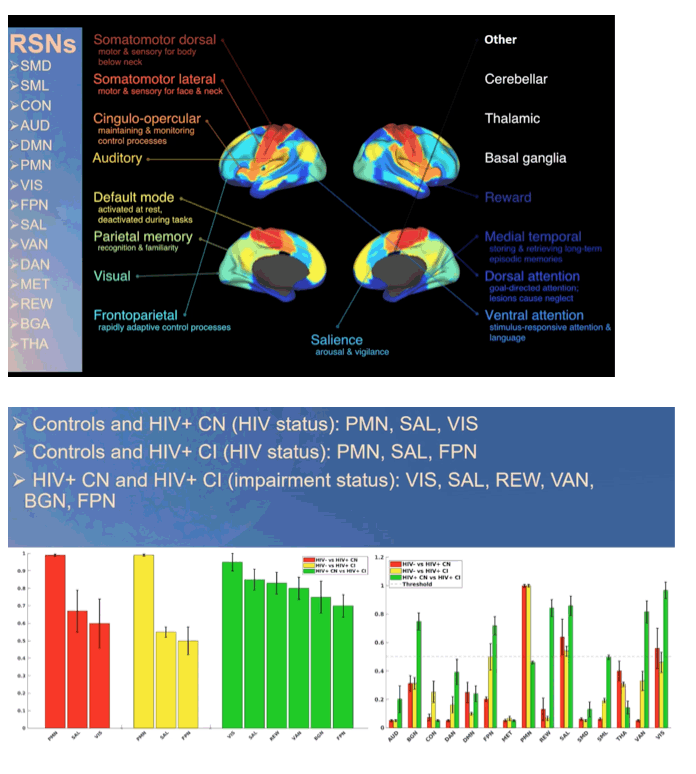
Patrick Luckett (Department of Neurology, Washington University School of Medicine, Saint Louis, MO, USA) presented data about effect of HIV and aging on resting state networks (Abstract 164). The aims of this study were to i) utilize machine learning based feature selection to identify resting networks being the strongest predictors of HIV status and of cognitive impairment and ii) to utilize deep learning to analyze voxelwise maps of the networks identified by feature selection and therefore analyze topological differences. Researchers used resting state functional MRIs that allowed studying neuronal brain activity by measuring the Blood Oxygen Level Dependence (BOLD) signal over time. BOLD signal reflects brain activity via oxygen usage and can be used to identify unique brain networks as well as to evaluate the functional organization of the brain (hierarchy, topological boundaries, communicating signals). A total of 1806 participants were included in this study, of which 297 were HIV positive virogically suppressed (viral load < 200 cp/mL) and matched for age, sex and education with control participants. Cognitive impairment was assessed in the learning, memory, executive, motor and language domains. A total of 15 resting state networks were evaluated in HIV + participants with or without cognitive impairment and in controls. Salience network was a strong predictor for all three groups in all age groups. Parietal memory network was a strong predictor of HIV status but not cognitive impairment status. The frontal parietal network was a strong predictor when comparing controls to HIV+ cognitive impaired and HIV cognitive normal to HIV+ cognitive impaired, but not controls to HIV+ cognitive normal, suggesting that cognitive impairment was associated with both cortical and subcortical regions. Strong predictors were strong in all age groups.
http://www.croiwebcasts.org/console/player/48345?mediaType=slideVideo&
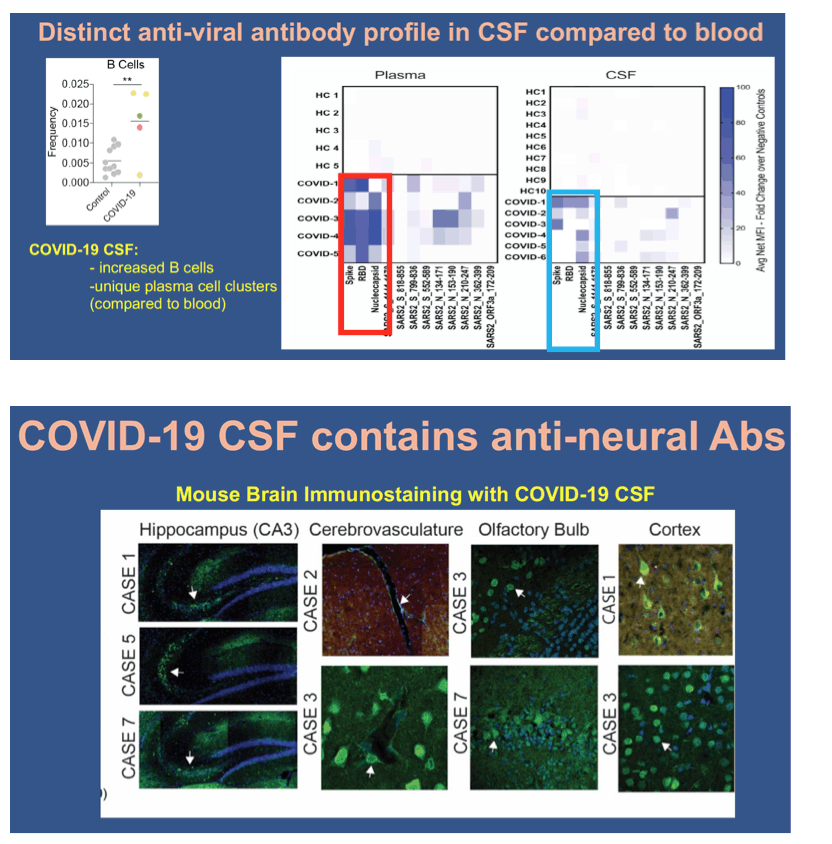
Shelli F. Farhadian (Yale School of Medicine) described divergent and self-reactive immune responses in the CNS of COVID-19 patients (Abstract 165). Neurological symptoms concern about a 1/3 of patients hospitalized with acute COVID-19. Other respiratory viruses like RSV and influenzae cause neurological sequelae through many different paths, including direct neuro-invasion and/or through para-infectious processes including exuberant immune responses within the CNS. Autopsy studies of patients who have died with COVID-19 suggest that viral neural invasion does occur in some patients with COVID-19, but likely does not explain the degree of neuropathology seen in some cases. Researchers evaluated here whether neural immune processes may contribute to neurological sequelae during COVID-19 using paired blood and CSF samples from COVID-19 patients and healthy uninfected controls in order to compare immune profiles in blood and CSF from the same patients. In 6 acute COVID-19 patients with neurological symptoms (seizures, encephalopathy or intractable headache) they demonstrated divergent T cell responses in CSF and plasma, namely upregulated CSF Th1, Th2 and effector CD8 T cells during COVID-19, with activated Il-1 and Il-12 pathways only in CSF. Moreover, B cells were also increased in the CSF, and presented different anti-SARS-Cov-2 antibody profile in CSF compared to the blood of the same patients (e.g., anti-RBD antibodies were rare in the CSF but uniformly present in the plasma). Finally, cloning individual monoclonal antibodies (mAbs) from clonally expanded B cell receptor sequences in the CSF and blood, they concluded that unique CSF-derived mAbs target spike protein, while all others mAbs had anti-neural immunoreactivity. In sum, intrathecal antibodies were reactive to SARS-CoV-2 antigen, self-antigen or both and CNS symptoms during COVID-19 were likely multifactorial and may be due in part to CNS-specific immune responses.
http://www.croiwebcasts.org/console/player/48346?mediaType=slideVideo&
|
| |
|
 |
 |
|
|