 |
 |
 |
| |
SEX MODIFIES THE ASSOCIATION BETWEEN INFLAMMATION
AND VASCULAR EVENTS IN TREATED HIV
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Samuel R . Schnittman1, Gabriele B. Beck-Engeser1, Judy K. Shigenaga1, Haelee Ahn1, Robin M. Nance2, Vanessa York1, Joseph A. Delaney3, Susan Heckbert2, David Tirschwell2, Felicia C. Chow1, Fran Aweeka1, Carl Grunfeld1, Heidi Crane2, Peter W. Hunt1, for the CFAR Network of Integrated Clinical Systems (CNICS) Network 1University of California San Francisco, San Francisco, CA, USA, 2University of Washington, Seattle, WA, USA, 3University of Manitoba, Winnipeg, Canada
Background: Inflammation persists in people with HIV (PWH) despite antiretroviral therapy (ART) and predicts morbidity and mortality. The specific inflammatory pathways associated with myocardial infarction (MI), ischemic stroke, and venous thromboembolism (VTE), and whether these pathways are modified by sex, have yet to be fully described.
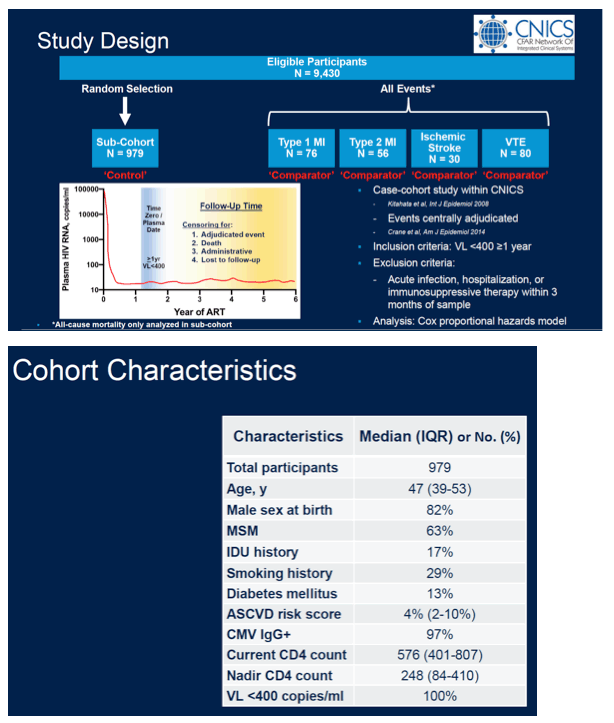
Methods: Using a case-cohort design, we randomly sampled all CNICS participants with available plasma after 1 year of ART-mediated viral suppression (the cohort), and from the same timepoint, all participants who were subsequently diagnosed with an incident type 1 or 2 MI (T1MI, T2MI), ischemic stroke, or VTE (all centrally adjudicated). Composite cardiovascular disease (CVD) event included T1MI and ischemic stroke. The relationship between 11 plasma biomarkers normalized to the cohort interquartile range (IQR) and subsequent event risk was assessed by logistic regression, adjusting for age, natal sex, nadir CD4, and other potential confounders (smoking, IDU, ASCVD risk score, and HCV history).
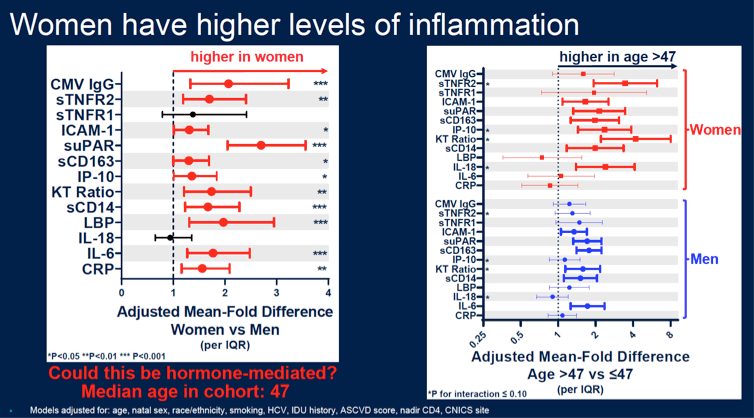
"Clear interaction between age & inflammation for women"
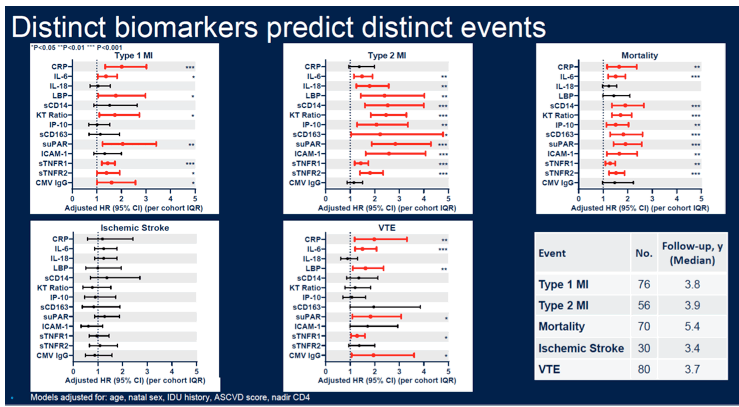
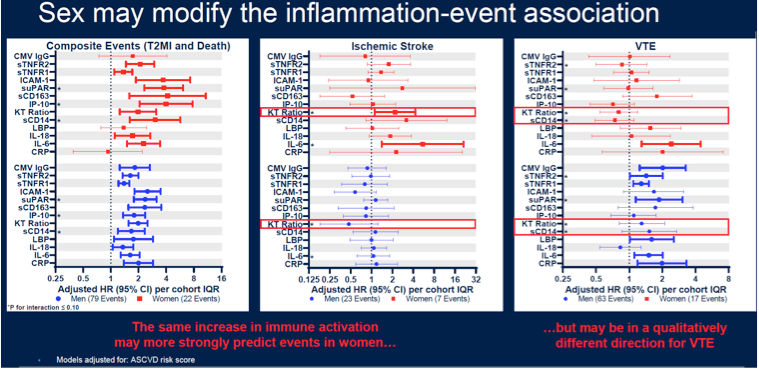
Results: We sampled a random sub-cohort of 979 (of 9430 eligible) participants and 103 CVD (75 T1MI, 30 ischemic stroke), 56 T2MI, and 80 VTE cases. In the sub-cohort, median age was 47, 82% were men, and 17% had a history of IDU. Median ASCVD risk was 4% and median current and nadir CD4 were 576 and 248, respectively. After adjustment, women had a 1.4-2.5 fold IQR higher CRP, LBP, sCD14, suPAR, ICAM-1, and CMV IgG than men (P<0.03 for all). Higher CRP, sCD14, and sTNFR2 were associated with subsequent T1MI (1.3-1.6 fold higher odds per IQR increase, P<0.01 for all), while higher CRP, suPAR, and ICAM-1 were associated with VTE (1.5-1.7 fold higher odds per IQR increase, P<0.01 for all). All biomarkers except CRP, LBP, and CMV IgG were associated with incident T2MI (1.4-2.8 fold greater odds per IQR increase, P<0.001 for all). Inflammatory markers tended to be associated with CVD events more strongly among women compared to men (KT ratio and sCD14 P for interaction = 0.005 and 0.08) but tended to be associated with VTE events more strongly in men than women (sCD14 and sTNFR2 P for interaction = 0.02 and 0.10).
Conclusion: Discrete pathways of inflammation independently predict CVD and VTE events in treated HIV, and many of these pathways are modified by sex. As inflammation predicts CVD events more strongly in women than in men, representation of women in clinical studies of immune-based interventions in treated HIV infection is critical.



|
| |
|
 |
 |
|
|