 |
 |
 |
| |
COVID-19 HOSPITALIZATION AMONG PEOPLE WITH HIV OR SOLID ORGAN TRANSPLANT IN THE US
|
| |
| |
CROI 2021 March 6-10 reported by Jules Levin
Jing Sun1, Rena Patel2, Vithal Madhira3, Amy L. Olex4, Evan French4, Jessica Y. Islam5, Richard Moffitt6, Nora Franceschini5, Roslyn B. Mannon7, Gregory D. Kirk1, for the National COVID Cohort Collaborative
1The Johns Hopkins Bloomberg School of Public Health, Baltimore, MD, USA, 2University of Washington, Seattle, WA, USA, 3Palila Software, Reno, NV, USA, 4Virginia Commonwealth University, Richmond, VA, USA, 5University of North Carolina at Chapel Hill, Chapel Hill, NC, USA, 6Stony Brook University, Stony Brook, NY, USA, 7Nebraska Medical Center, Omaha, NE, USA
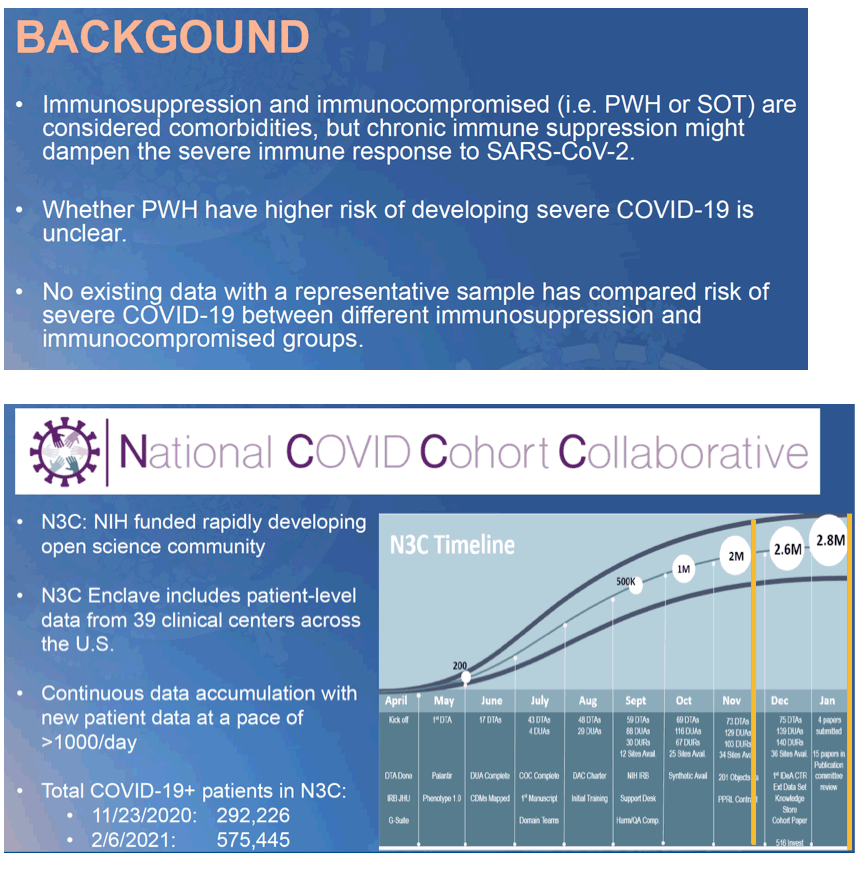
Background: The role of immunosuppression/compromise (ISC) in risk of severe COVID-19 is unknown. While ISC could reduce control of SARS-CoV-2 viremia, it might also dampen the severe immune response to the virus; data comparing ISC groups is limited.
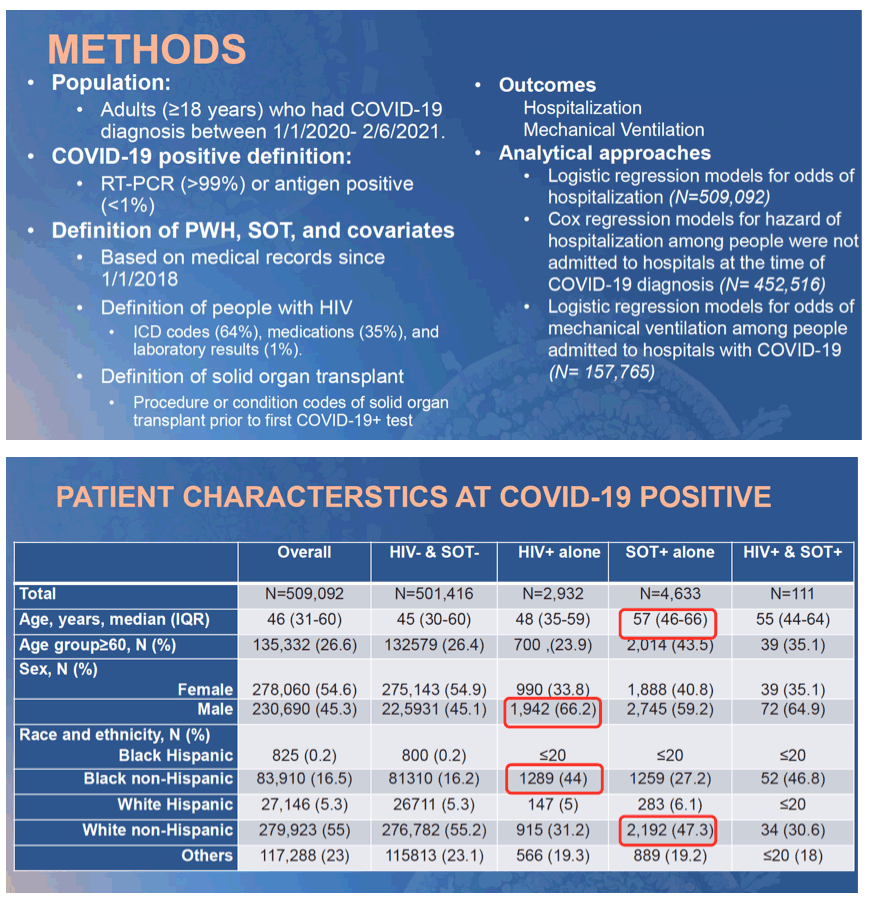
Methods: Using patient-level data from 34 sites in the U.S. National COVID Cohort Collaborative (N3C), we compared risk of COVID-19 hospitalization amongst COVID-19 patients in 3 ISC groups (1,300 persons with HIV [PWH]; 2,142 solid organ transplant [SOT] patients; 41 PWH with SOT) to 288,743 COVID-19 patients without HIV or SOT (HIV-/SOT-). COVID-19+ was defined by RT-PCR, antibody test, or diagnostic codes. HIV infection, SOT and comorbidities were defined by conditions/diagnostic codes within 2 years prior to first COVID-19+. Hospitalization was defined by inpatient care between 14 days prior to 45 days after the first COVID-19+. Odds ratios of hospitalization were estimated using multivariable logistic regression models adjusting for demographics, study site, and comorbidities (severe liver disease, diabetes, cancer, kidney disease, and total comorbidities [0, 1, 2, ≥3]).
Results: Of 292,226 COVID-19+ patients, the median age was 41 years (IQR: 25-58), 46% male, 47% non-Hispanic white (NHW), and 17% non-Hispanic black (NHB). PWH and SOT patients, respectively, were more likely to be older (median: 50 & 56), male (70% & 60%), and had ≥ 3 comorbidities than overall N3C patients (30% & 64% vs. 8%). PWH were more likely to be NHB (50%)
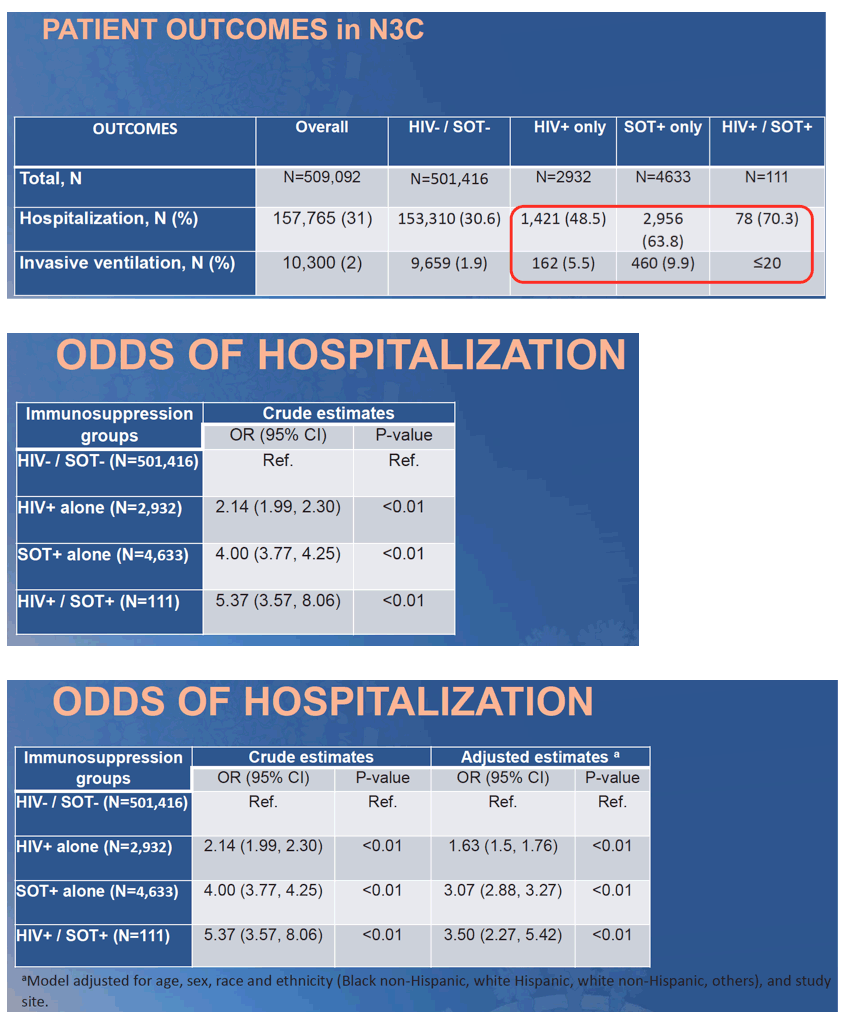
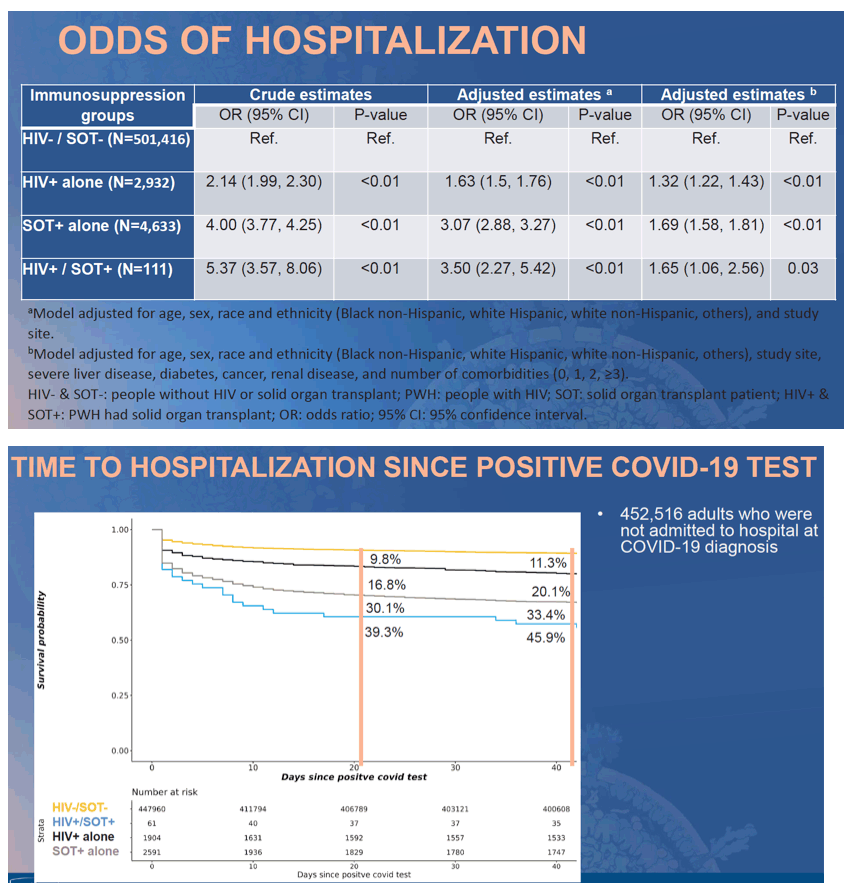
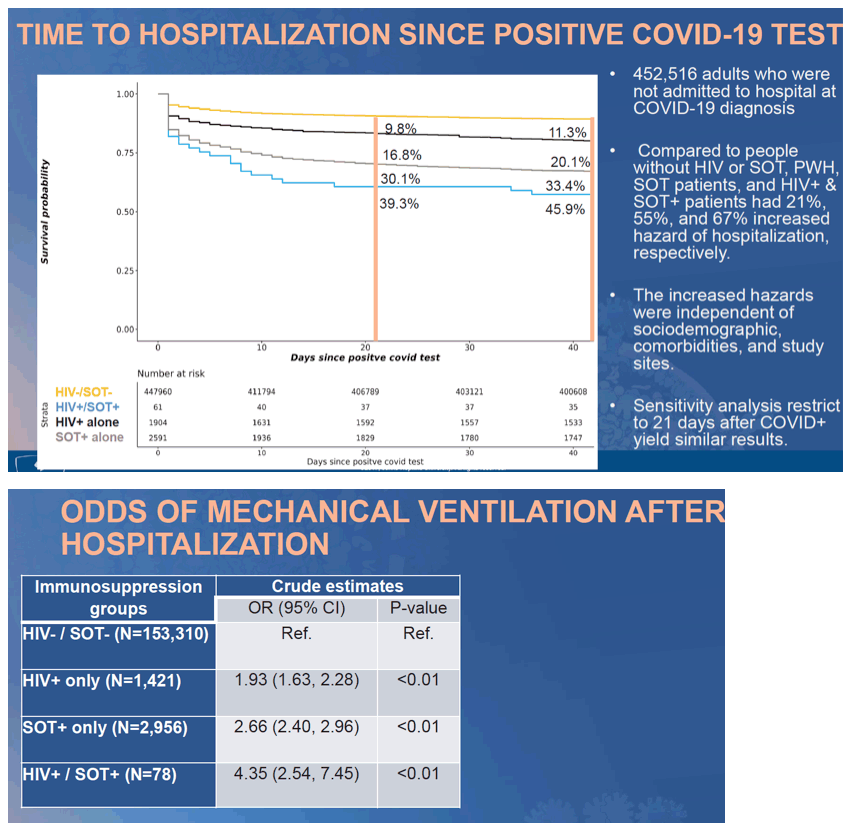
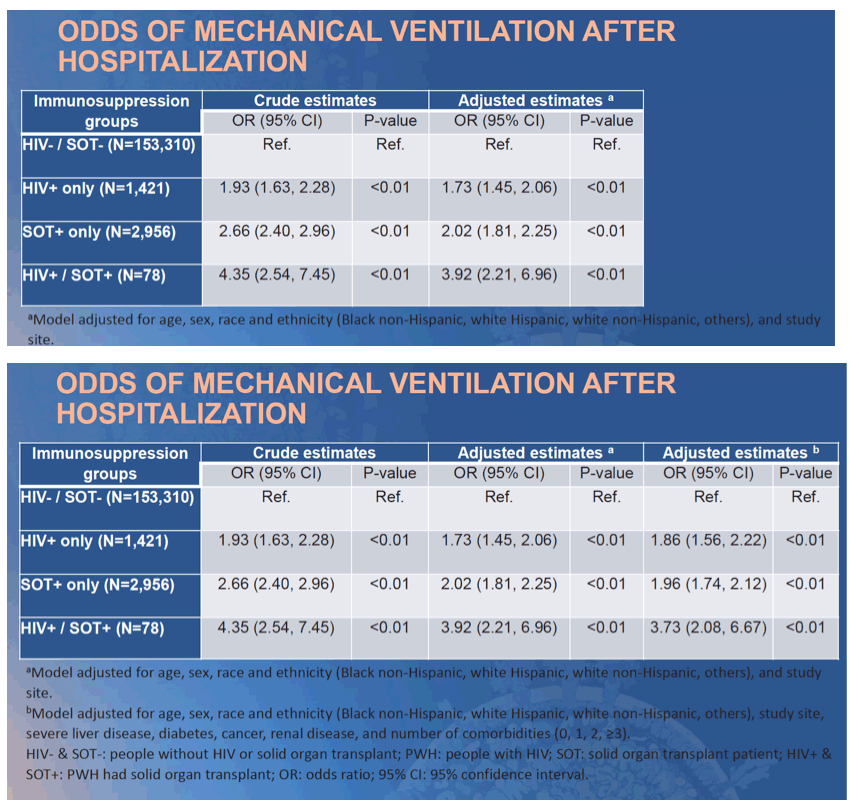
and SOT patients were more likely to be NHW (41%). Overall, 26% of HIV-/SOT- COVID-19 patients were hospitalized. In crude analyses with HIV-/SOT- as the referent group (Table), COVID-19 patients with HIV, SOT or both had a 2.3, 4.4, or 6.9-fold increased odds of hospitalization, respectively. After adjustment for demographics and site, the risk was attenuated but remained statistically significant (Model a). Sequential adjustment for the type and number of comorbidities obviated the estimated risk among PWH, while SOT patients had persistently increased odds of hospitalization (Model b).
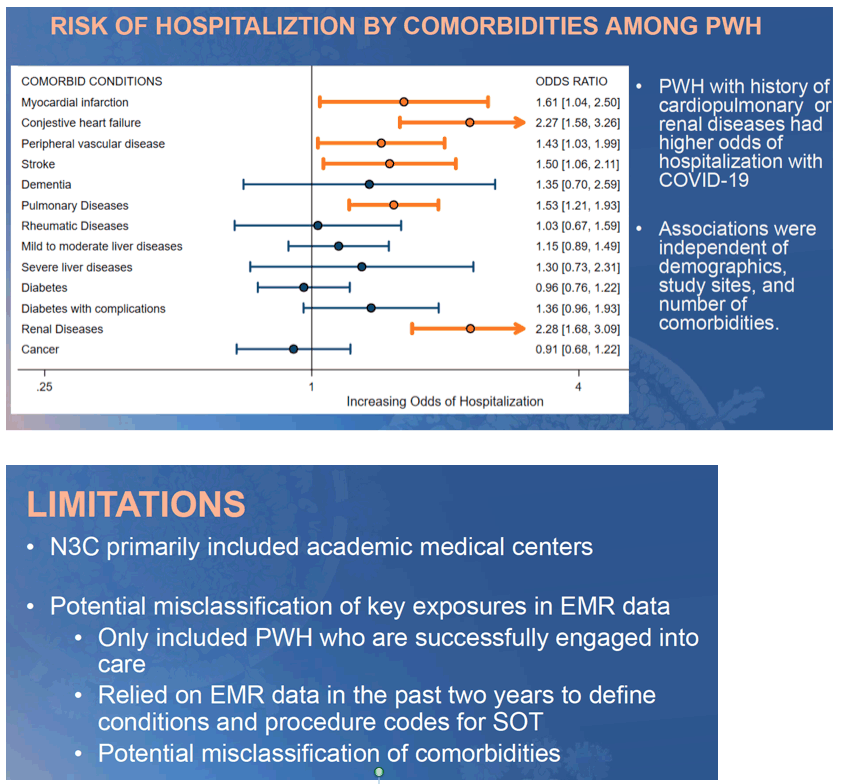
Conclusion: ISC patients (PWH and SOT) are more likely to be hospitalized with COVID-19 independent of demographics. However, this increased hospitalization risk was driven mainly by the high burden of comorbidities in both groups.
Only SOT patients had an independent risk of hospitalization after adjusting for comorbidities. Ongoing analyses will examine the impact of ISC on additional COVID-19 outcomes (i.e. ventilation use, death).


|
| |
|
 |
 |
|
|