 |
 |
 |
| |
HIV AND COVID-19 INPATIENT OUTCOMES: A MATCHED RETROSPECTIVE MULTICENTRE ANALYSIS
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Ming J . Lee1, Colette Smith2, Sarah Fidler3, Lynsey C. Goodwin4, Lisa Hamzah5, Sarah Lawrence4, Rebecca Marchant5, Adrian Palfreeman6, Manish Pareek6, Kyle Ring7, Luke Snell8, John Thornhill9, Marie Williamson9, Achyuta Nori1, for RECEDE- C19 STUDY GROUP
1Guy’s and St Thomas’ NHS Foundation Trust, London, UK, 2University College London, London, UK, 3Imperial College London, London, UK, 4The Pennine Acute Hospitals NHS Trust, Manchester, UK, 5St George's University Hospital NHS Foundation Trust, London, UK, 6University Hospitals of Leicester NHS Trust, Leicester, UK, 7Imperial College Healthcare NHS Trust, London, UK, 8King's College London, London, UK, 9Barts Health NHS Trust, London, UK
Background:
Clinical outcomes for people living with HIV (PLWH) hospitalized with COVID-19 infections have shown mixed outcomes. We conducted a multicentre, UK retrospective matched cohorts' analysis.
Methods:
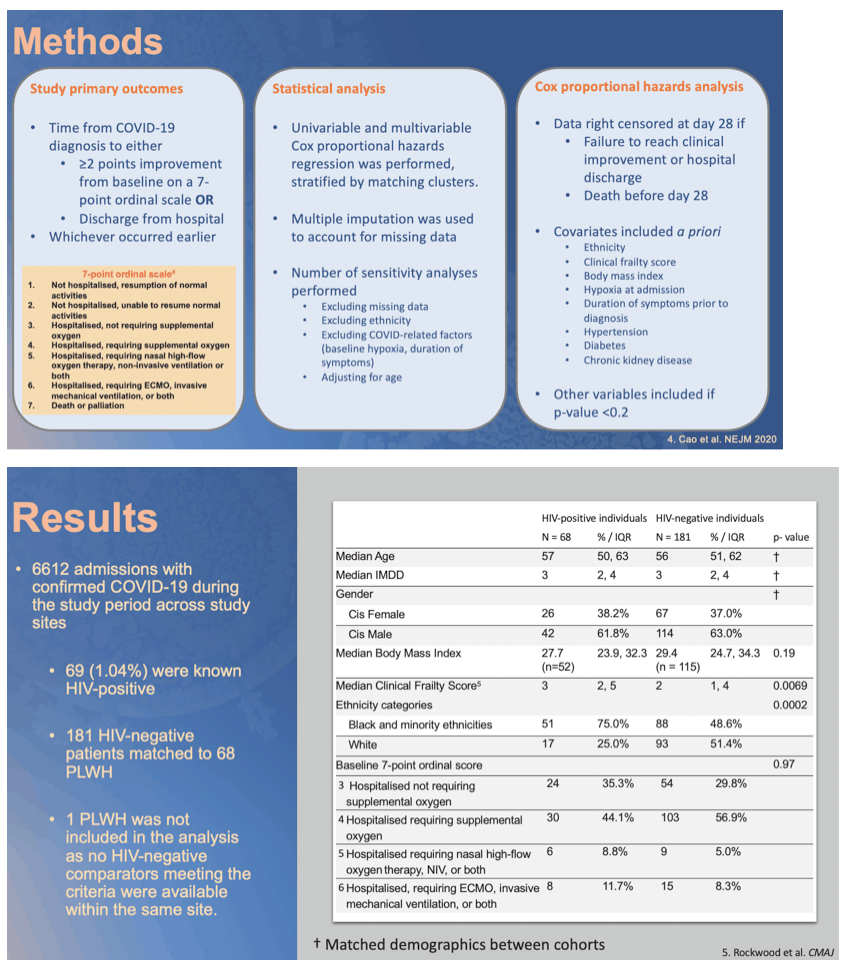
Index cases were HIV+ COVID-19 PCR+ patients hospitalized between dates 1st February - 31st May 2020. HIV-negative patients were matched to PLWH up to a 3:1 ratio across 6 sites in England, by hospital site, test date +/- 7 days, age +/- 5 years, gender, index of multiple deprivation decile (IMDD) +/- 1. The primary outcome was patients achieving ≥2-point improvement on a 7-point ordinal scale or discharge from hospital by day 28, whichever was earlier. Follow up was right-censored at day 28 for patients still in hospital. Baseline characteristics and outcomes were analysed by Cox-proportional hazards regression stratified by matching clusters using multiple imputation for missing data. The model adjusted for ethnicity, clinical frailty score, body mass index, baseline hypoxia, duration of symptoms, hypertension, diabetes, malignancy, cardiac, lung and renal disease.
Results:
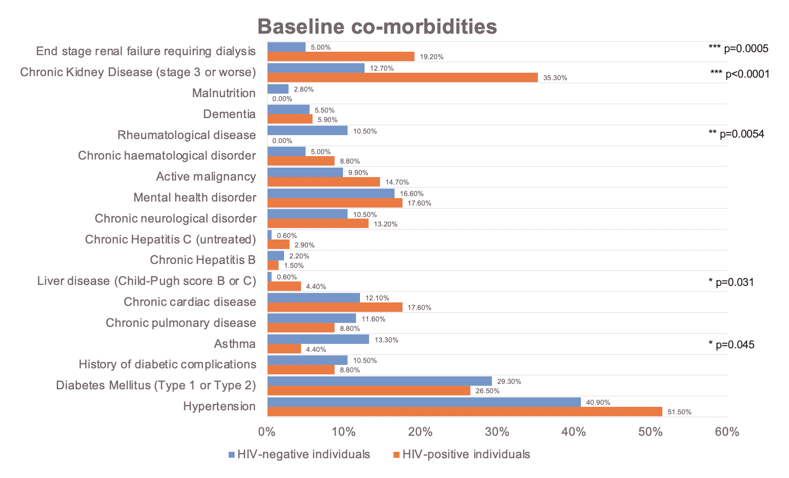
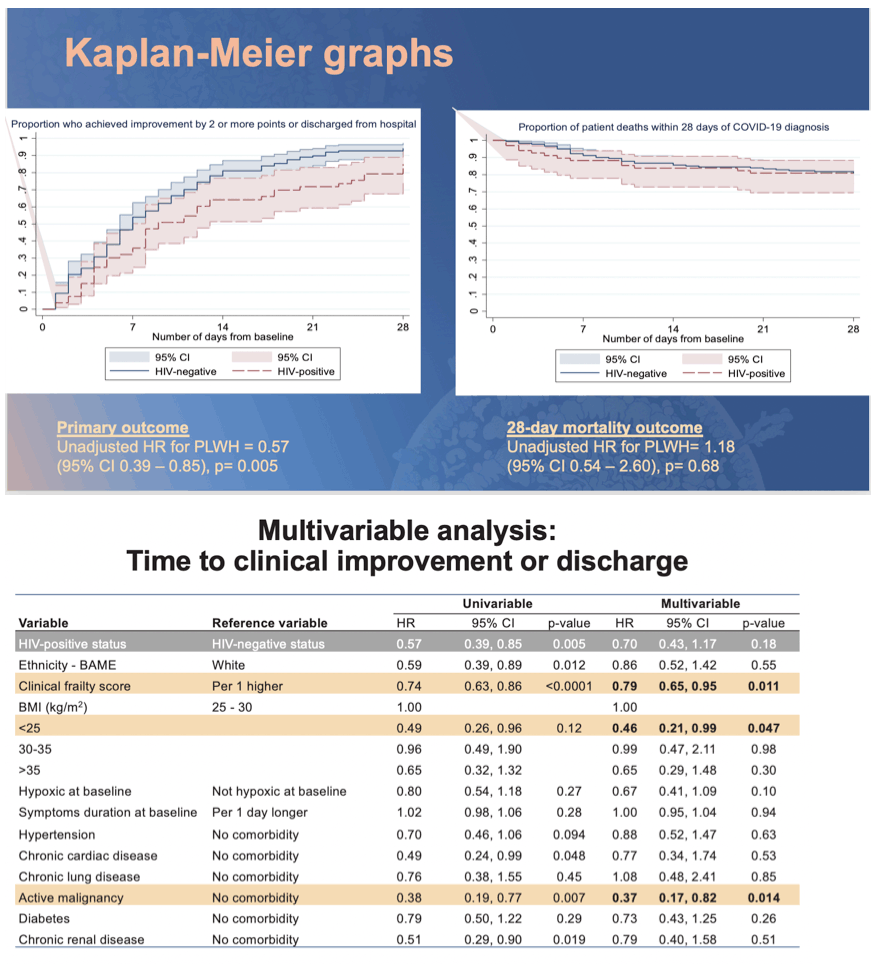
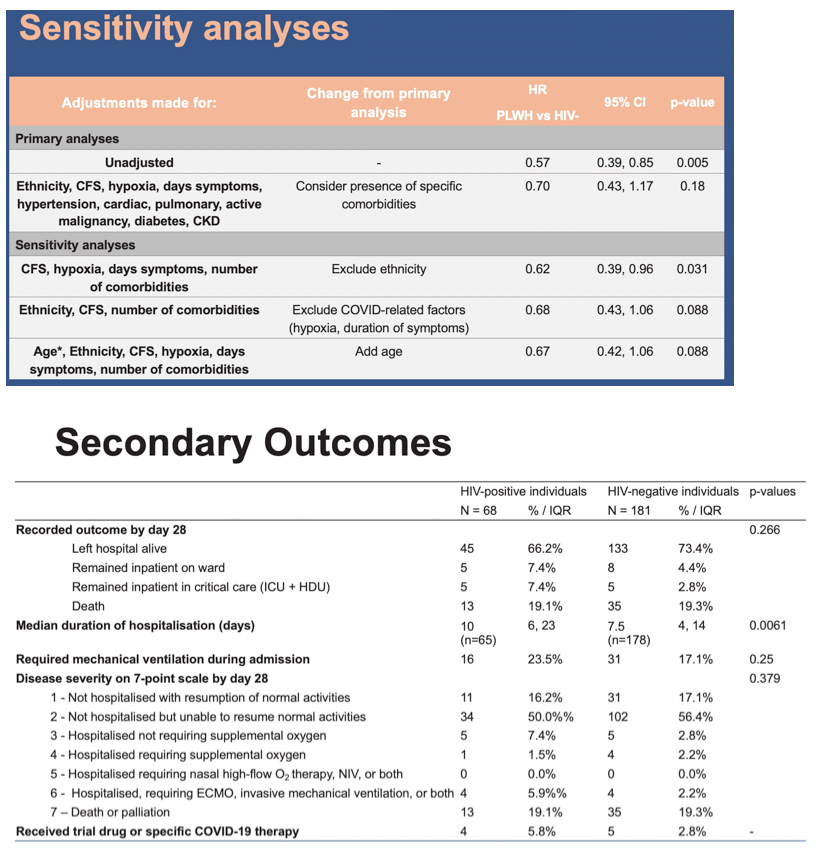
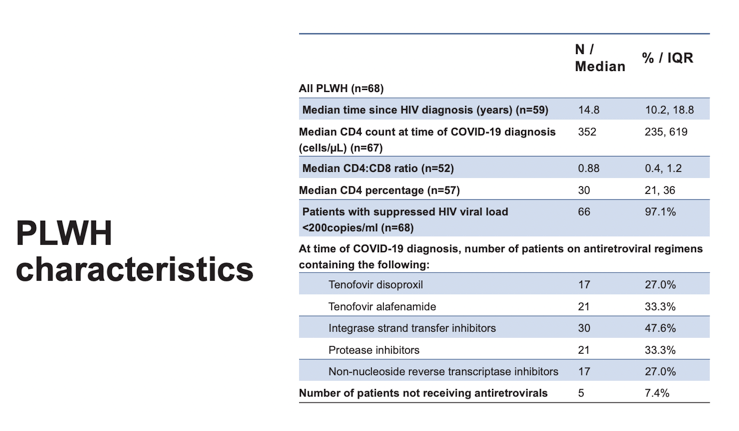
68 PLWH and 181 HIV-negative patients were included. PLWH had an HR of 0.57 (95%CI 0.39, 0.85; p=0.005) of achieving 2-point improvement or discharge compared to HIV-negative patients. The effect size of HIV-status was attenuated (aHR 0.70; 0.43, 1.17; P=0.18) after adjustment in the multivariable model (Table 1), with baseline frailty (aHR=0.79; 95%CI 0.65, 0.95; p=0.011 ), malignancy (aHR=0.37; 95%CI 0.17, 0.82; p=0.014) having a greater impact on the primary outcome. Proportion of deaths (19.1% vs 19.3%, p=0.266) and patients requiring ventilation (23.5% vs 17.1%, p=0.25) were similar between PLWH and HIV-negative patients. Sensitivity analyses adjusting for age and excluding missing data, remained consistent with main findings. PLWH were frailer (median clinical frailty score 3 vs 2, p=0.0069), and had higher proportion of malignancies (14.7% vs 9.9%, p=0.29) although not statistically significant. Number of non-HIV co-morbidities (2 vs 2, p=0.16) and median BMI (27.7 vs 29.4, p=0.19) were similar. The median CD4 count of PLWH was 352cells/ μL (IQR 235, 619), and 63/68 (92.3%) were taking antiretroviral therapy.
Conclusion:
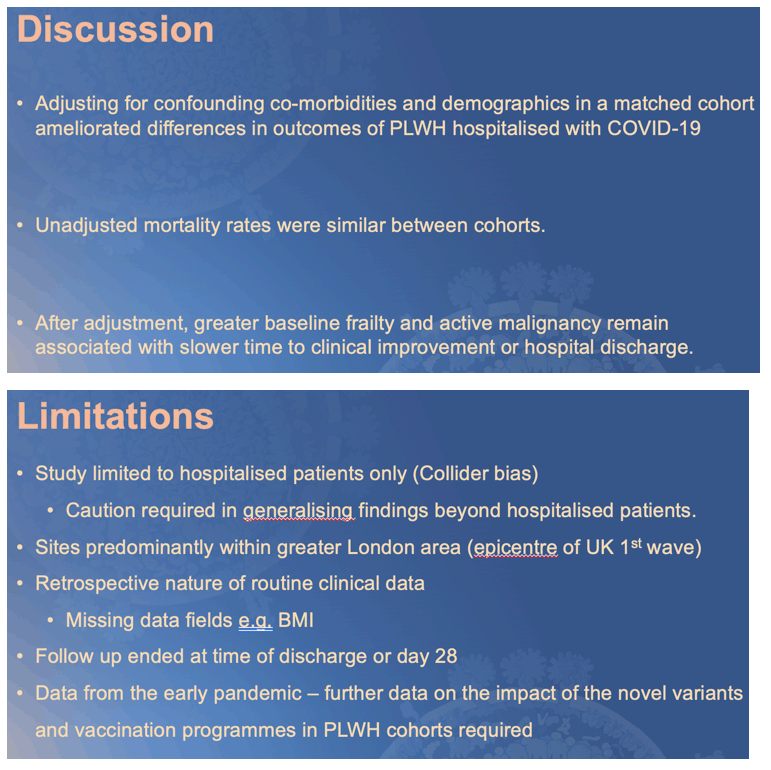
Although PLWH were less likely to achieve improvement or discharge, after adjustment the effect of HIV-status was attenuated. Increased baseline frailty and active malignancies remain associated with poorer COVID-19 outcomes.




|
| |
|
 |
 |
|
|