 |
 |
 |
| |
HIGHER COMORBIDITY BURDEN PREDICTS
WORSENING NEUROCOGNITION IN PEOPLE WITH HIV
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Ronald J . Ellis1, Emily W. Paolillo1, Rowan Saloner2, Scott Letendre2, David J. Moore1, Robert K. Heaton2
1University of California San Diego, La Jolla, CA, USA, 2University of California San Diego, San Diego, CA, USA
Background: Comorbidities linked to aging such as diabetes mellitus, visceral adiposity and renal dysfunction accumulate at a faster rate in people with HIV (PWH) than in the general population. We evaluated whether the Charlson Index, a global comorbidity scale comprising 17 variables that has been validated in previous studies, predicted neurocognitive trajectories in PWH.
Methods: Neurocognition was measured by averaging scaled scores from all assessments in a comprehensive neuropsychological battery. Multilevel modeling was used to examine between- and within-person predictors of global neurocognition. At the between-person level, average Charlson Index (averaged within each person across all their visits) was examined as a predictor of neurocognitive change over time, covarying for the effect of HIV disease characteristics (proportion of visits virally suppressed, average CD4). At the within-person level, Charlson Index was used to predict fluctuations in global neurocognition at the same and next visit, covarying for visit-specific effects of viral load detectability and current CD4 count.
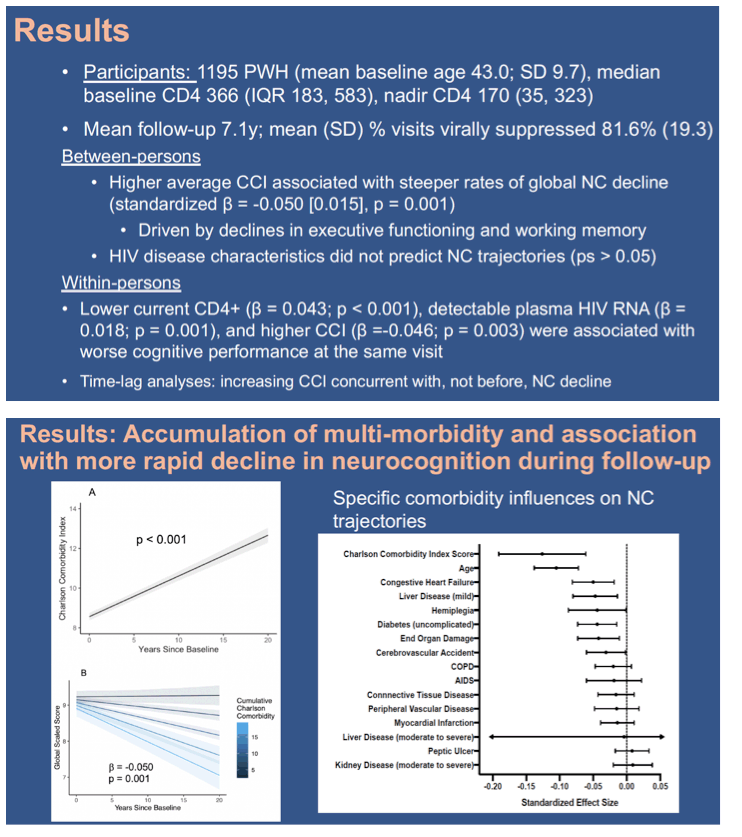
Results: Participants were 1195 PWH (mean age at baseline = 43.0; SD 9.7) followed for an average of over 7.1 years (SD = 5.0; range = 0.5 to 20.5 years). Between persons, higher average Charlson index scores were associated with faster rates of global neurocognitive decline (standardized β = -0.50 [0.015], p = 0.001). This global effect was driven by significant decline in the domains of executive functioning (p = 0.001) and working memory (p = 0.007). The Figure shows the contributions of individual components of the Charlson. HIV disease characteristics did not predict trajectories of neurocognitive change (ps > 0.05). At the within-person level of the model, lower current CD4+ lymphocytes (β
= 0.043 [0.009]; p < 0.001), detectable plasma HIV RNA (β = 0.018 [0.006]; p = 0.001), and higher Charlson Index score (β = -0.046 [0.015]; p = 0.003) related to worse concurrent global neurocognitive performance at the same visit. Time-lag analyses demonstrated that increasing comorbidities occurred concomitant with, not before, neurocognitive decline.
Conclusion: The impact of comorbidities on trajectories of neurocognitive decline was greater than that of HIV disease factors. Although correlative, the temporal relationship between accumulating comorbidities and neurocognitive decline suggests that interventions to prevent or ameliorate a variety of comorbidities may improve neurocognitive prognosis for PWH.


|
| |
|
 |
 |
|
|