 |
 |
 |
| |
PHASE 1 PK, SAFETY, AND ACCEPTABILITY STUDY OF 3-MONTH DAPIVIRINE VAGINAL RINGS
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Albert Liu1, Clara Dominguez Islas2, Holly Gundacker3, Craig Hoesley4, Ariane Van der Straten5, Craig Hendrix6, May Beamer7, Cindy Jacobson7, Tara McClure8, Tanya Harrell3, Katherine Bunge9, John Steytler10, Jeremy Nuttall10, Jeanna PIper11, Mark Marzinke6
1San Francisco Department of Public Health, San Francisco, CA, USA, 2Fred Hutchinson Cancer Research Center, Seattle, WA, USA, 3Statistical Center for HIV/AIDS Research and Prevention, Seattle, WA, USA, 4University of Alabama at Birmingham, Birmingham, AL, USA, 5RTI International, Berkeley, CA, USA, 6The Johns Hopkins University School of Medicine, Baltimore, MD, USA, 7Magee-Womens Research Institute, Pittsburgh, PA, USA, 8FHI 360, Durham, NC, USA, 9Magee-Womens Hospital of UPMC, Pittsburgh, PA, USA, 10International Partnership For Microbicides, Silver Spring, MD, USA, 11National Institute of Allergy and Infectious Diseases, Rockville, MD, USA
Background: Vaginal rings (VRs) are a promising approach to long-acting HIV prevention. Extended duration VRs may reduce user burden and cost, streamline follow-up, and encourage adherence. We evaluated the safety, pharmacokinetics, adherence, and acceptability of two 3-month dapivirine (DPV) VRs compared with the monthly DPV VR.
Methods: MTN-036/IPM-047 enrolled 49 HIV-negative participants into a Phase 1, multi-site, randomized (1:1:1) trial comparing two extended duration (100 or 200 mg DPV) VRs used continuously for 13 weeks to a monthly 25 mg DPV VR. DPV concentrations were quantified in plasma, cervicovaginal fluid (CVF), and cervical tissue, at nominal timepoints. Geometric means ratios (GMRs) relative to the comparator ring were estimated using a fixed-effects model on log-transformed outcomes. Used rings were analyzed for residual DPV levels.
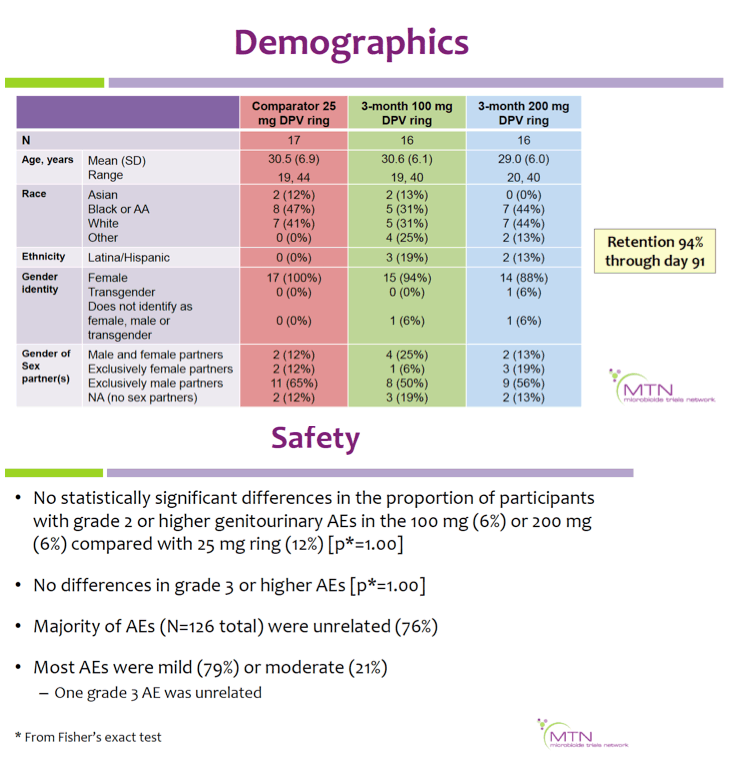
Safety was assessed by adverse events (AEs), acceptability and adherence by self-report.
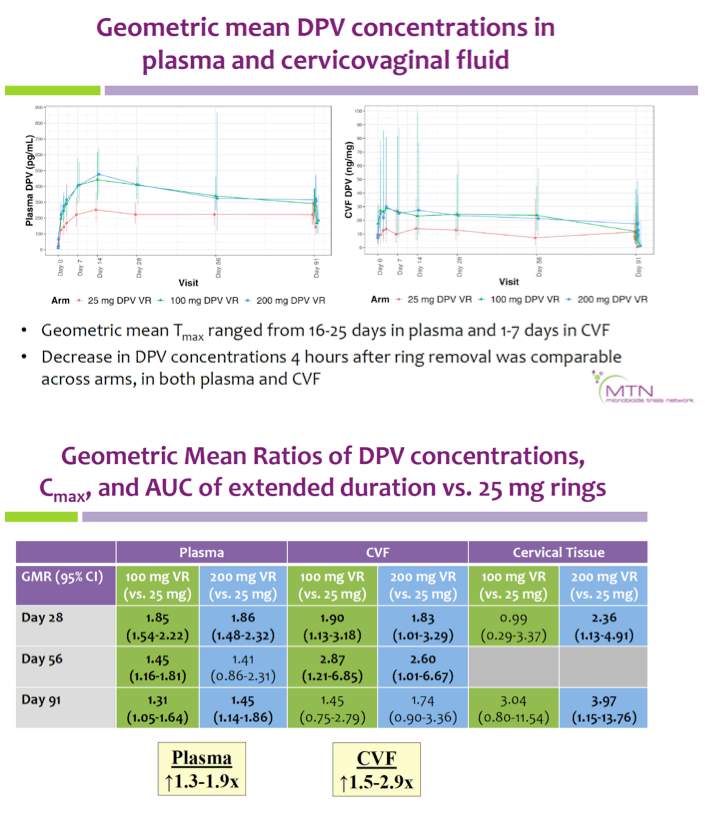
Results: Mean age was 30.0 (range 19-44) years; 41% were Black, 39% white, 8% Asian, and 12% of other race. Retention was 94% through day 91. There were no differences in the proportion of participants with grade ≥2 genitourinary AEs or grade ≥3 AEs in the extended duration vs. monthly VR arms (p=1.0). Across timepoints, plasma and CVF DPV concentrations were higher in the 100 and 200 mg VR arms compared with the 25 mg arm (Table).
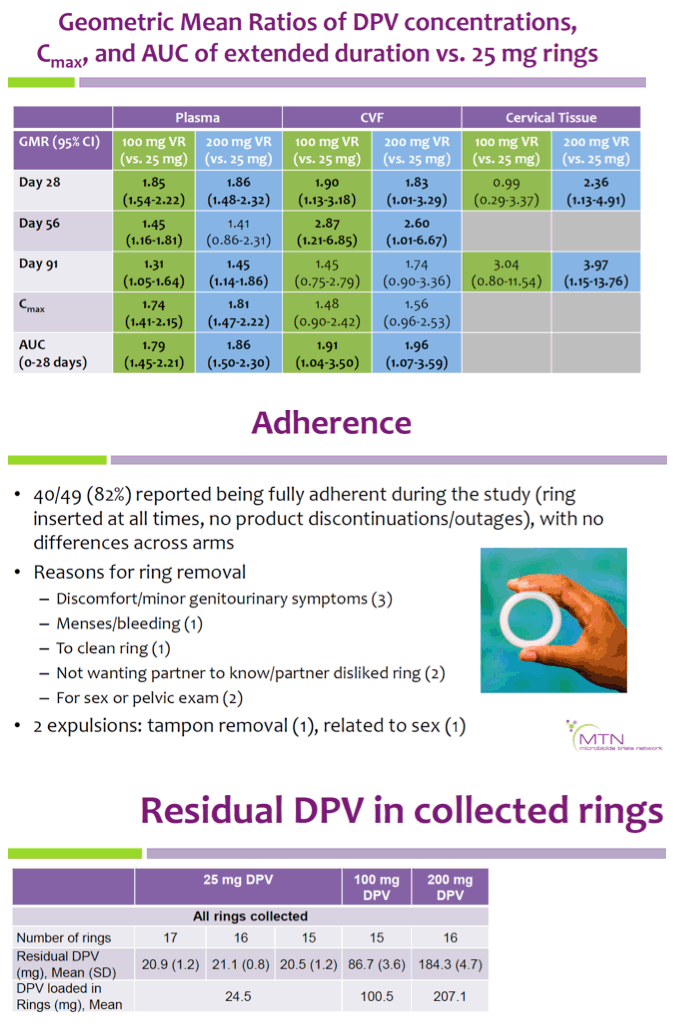
Additionally, the peak concentration (Cmax) and Area Under the Concentration- Time Curve (AUC) for 0-28 days were 1.5 to 2 times higher for the extended duration VRs vs. monthly VR. Cervical tissue concentrations were consistently higher in the 200 mg VR (GMRs 2.36-3.97) and higher in the 100 mg VR at day 91 (GMR 3.04). A majority of participants (82%) reported being fully adherent, with no statistically significant differences between groups. Most participants reported liking the VRs (median (IQR): 8 (6-10) on 10-point Likert scale) and reported they were likely to use the VR if effective (median (IQR): 9 (7-10) on a 10-point Likert scale of future VR use). Based on manufacturer-reported DPV loads, the mean total DPV released over 13 weeks was estimated to be 11.2 mg for the 25 mg VR, 14.2 mg for the 100 mg VR, and 22.8 mg for the 200 mg VR.
Conclusion: The extended duration DPV VRs were well-tolerated and achieved higher DPV concentrations compared with the monthly DPV VR, likely translating into at least equal efficacy. These findings support further evaluation of 3-month DPV VRs for HIV prevention in women.





|
| |
|
 |
 |
|
|