 |
 |
 |
| |
MATERNAL WEIGHT AND ADVERSE PREGNANCY OUTCOMES AMONG WOMEN ON ART AT CONCEPTION
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Rebecca Zash1, Ellen Caniglia2, Modiegi Diseko3, Gloria Mayondi3, Judith Mabuta3, Rebecca Luckett1, Justus Hofmeyr4, Chelsea Morroni5, Doreen Ramogola- Masire4, Paige L. Williams6, Chloe Zera1, Joseph Makhema3, Shahin Lockman7, Roger Shapiro6
1Beth Israel Deaconess Medical Center, Boston, MA, USA, 2New York University Langone Medical Center, New York, NY, USA, 3Botswana Harvard AIDS Institute Partnership, Gaborone, Botswana, 4University of Botswana, Gaborone, Botswana, 5University of Liverpool, Liverpool, UK, 6Harvard TH Chan School of Public Health, Boston, MA, USA, 7Brigham and Women's Hospital, Boston, MA, USA
Background: Antiretrovirals such as dolutegravir (DTG) and tenofovir alafenamide (TAF) have been associated with excessive weight gain, but the impact of weight and weight gain on pregnancy outcomes is poorly described among women on antiretroviral treatment (ART).
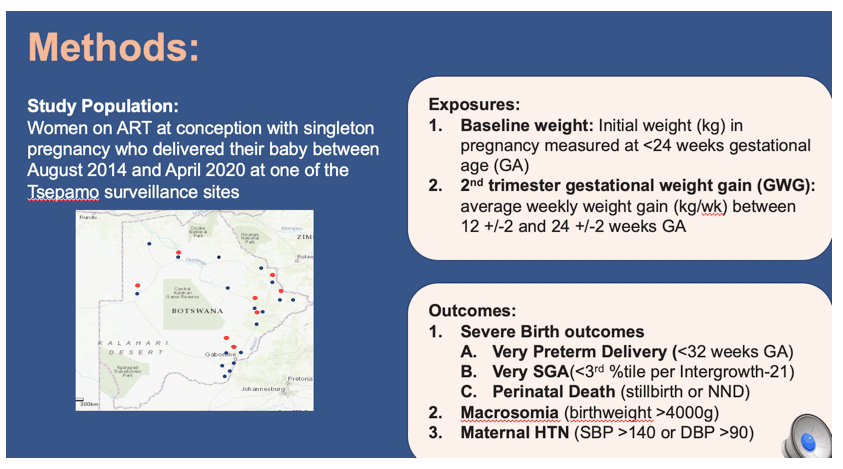
Methods: Using data from the Tsepamo birth outcomes surveillance study in Botswana, we evaluated the relationship between maternal weight (and weight gain) and severe birth outcomes (very preterm delivery <32weeks, very small for gestational age <3rd percentile, perinatal death), macrosomia (birthweight >4000g) and maternal hypertension. We estimated the relative risk of each outcome by baseline weight (first weight in pregnancy <24 weeks) and second trimester average weekly weight gain (kg/week from 12 +/-2 to 24 +/-2 weeks) using log binomial regression and evaluated effect modification by ART regimen (DTG vs. Efavirenz [EFV]).
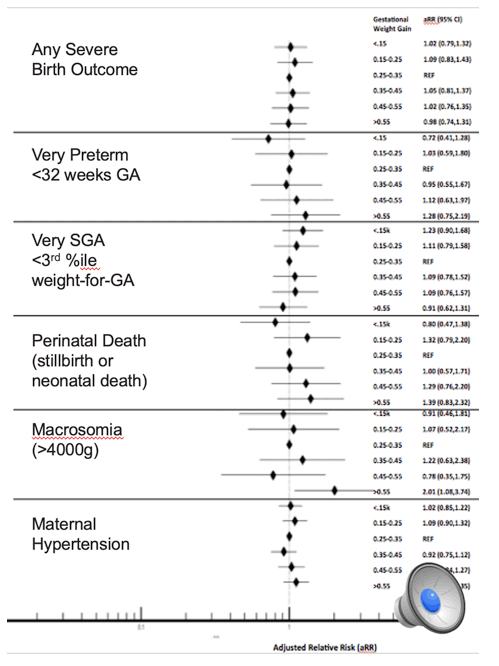
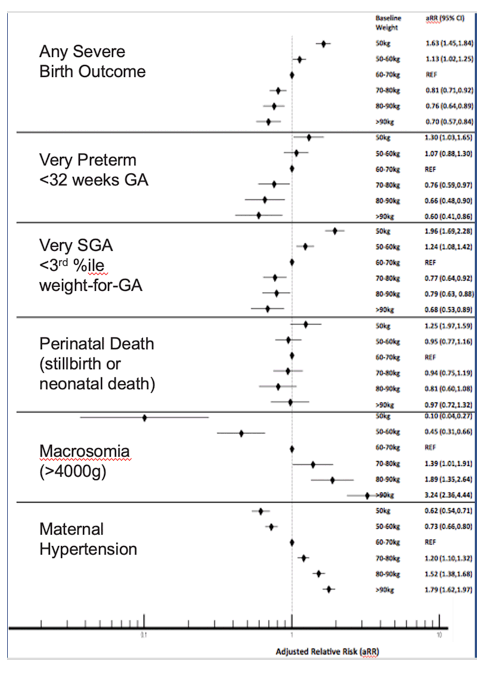
Results: Of 22,828 women on ART at conception with singleton deliveries between August 2014-April 2020, 16,300 (71.4%) had a documented weight measured at <24 weeks gestation (baseline weight) and 4437 (19.2%) had documented weight measured both at 12 (+/-2) weeks and 24 (+/-2) weeks, allowing gestational weight gain calculation. Compared to women with baseline weight 60-70kg, low baseline weight (<50kg) was associated with increased risk of very preterm delivery (aRR 1.30, 95% CI 1.03,1.65) and very small for gestational age (aRR 1.96, 95% CI 1.69,2.28). High baseline weight (>90kg) was associated with increased risk of macrosomia (aRR 3.24, 95% CI 2.36,4.44) and maternal hypertension (aRR 1.79, 95% CI 1.62,1.97)(Figure 1). Baseline weight was not associated with perinatal death. For all outcomes, gestational weight gain showed weaker associations than did baseline weight. Duration of pre-pregnancy ART (years) was associated with higher baseline pregnancy weight for DTG but not for EFV, and the risk of maternal hypertension by baseline weight category was higher for DTG than EFV for all strata.
Conclusion: ART regimens associated with weight gain may reduce the percentage of low weight women at risk for certain severe adverse pregnancy outcomes but increase the number at risk of maternal hypertension. Further research is needed to determine whether weight-based ART treatment strategies could improve maternal and child health.



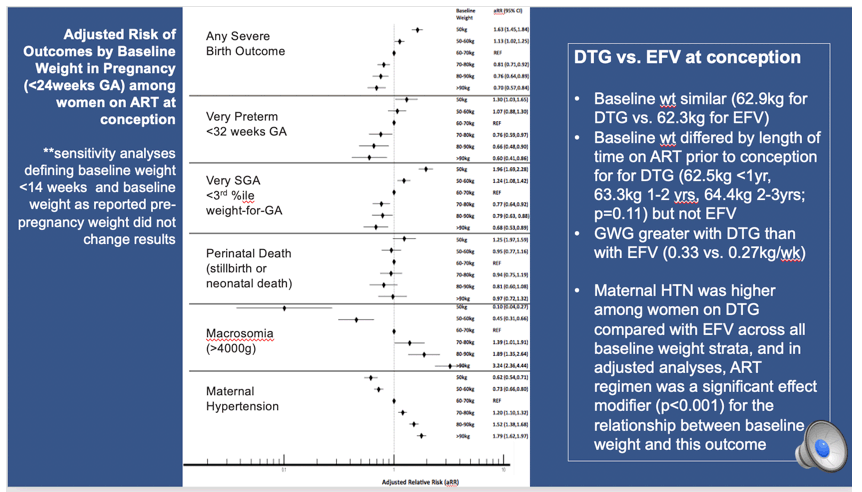
In contrast, here are our results of the association of baseline weight and outomes. You can see that women with lower baseline weight had increased risk of any sever birth outcomes, and specifically very preterm and very SGA. While women with higher baseline weight had increased risk of fetal macrosomia and hypertension. Perinatal death was fairly similar across baseline weight strata. When we did a sensitivty analysis defining baseline weight <14 weeks and baseline weight as reported pre-pregnancy weight, these results did not change.
We also looked at differences in weight with DTG and EFV. We found that the baseline weight did not differ between these two groups, though baseline weight increased by the number of years on DTG prior to conception, but not with EFV.
GWG was greater with DRG than EFV and maternal hypertension was higher.
|
| |
|
 |
 |
|
|