 |
 |
 |
| |
HIV-1, INSUFFICIENT SLEEP, AND ENDOTHELIAL VASODILATOR FUNCTION
|
| |
| |
CROI 2021 March 6-10 Reported by jules Levin
Kelly A . Stockelman1, Anthony R. Bain2, Cindy S. Firnhaber3, Jared J. Greiner1, Brian L. Stauffer3, Elizabeth Connick4, Christopher A. DeSouza1
1University of Colorado Boulder, Boulder, CO, USA, 2University of Windsor, Windsor, Ontario, Canada, 3University of Colorado Anschutz Medical Campus, Aurora, CO, USA, 4University of Arizona, Tucson, AZ, USA
Background: The increased risk and incidence of cardiovascular disease (CVD) in adults living with HIV-1 is not solely due to worsening of traditional CVD risk factors, but also involves ill-defined factors related to the virus and/or its therapies. More than 70% of adults living with HIV-1 report sleep problems, the most common malady being short nightly sleep duration (<7 h/night). Short nightly sleep duration is associated with increased CVD risk and events. An underlying mechanism for the sleep-related increase in CVD is a profound worsening in vascular endothelial function. The influence of insufficient sleep on vascular endothelial function in HIV-1-seropositive adults is unknown. We tested the hypotheses that: 1) short nightly sleep duration is associated with lower nitric oxide (NO)-mediated endothelium-dependent vasodilation in antiretroviral (ART)-treated adults living with HIV-1; and 2) the short sleep- related reduction in endothelial vasodilator function is due, at least in part, to increased oxidative stress.
Methods: Thirty-two sedentary, middle-aged HIV-1-seropositive adults on stable antiretroviral therapy were studied: 16 with normal nightly sleep duration (12M/4F; age: 50±2 yr; BMI: 25.4±0.7 kg/m2; sleep: 7.8±0.3 h/night) and 16 with short nightly sleep duration (14M/2F; 51±2 yr; 25.4±0.8 kg/m2; 5.6±0.3 h/night). Forearm blood flow (FBF) responses to intra-arterial infusion of acetylcholine (ACh), in the absence and presence of the endothelial NO synthase inhibitor NG-monomethyl-L-arginine (L-NMMA) and the antioxidant vitamin C were determined by venous occlusion plethysmography.
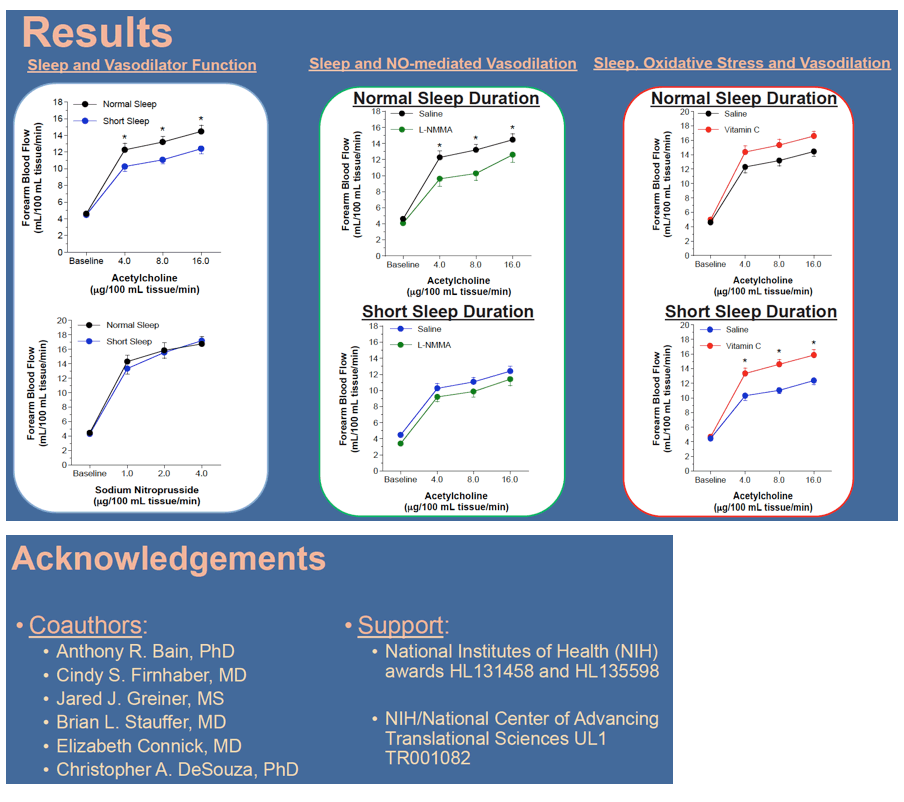
Results: FBF responses to ACh were significantly lower (∼20%) in the short sleep (from 4.5±0.3 to 12.4±0.6 mL/100 mL tissue/min) vs normal sleep adults (from 4.7±0.3 to 14.5±0.7 mL/100 mL tissue/min). L-NMMA significantly reduced (∼15%) the FBF response to ACh in the normal sleep but not the short sleep group; whereas, vitamin C significantly increased (∼30%) the vasodilator response to ACh in short sleep but not the normal sleep group.
Conclusion: Habitual short sleep duration is associated with lower endothelium-dependent vasodilation in adults living with HIV-1 due, in part,
to increased oxidative stress. Reduced NO-mediated endothelium-dependent vasodilation may increase the CVD risk in adults living with HIV-1 who sleep < 7h/night.


|
| |
|
 |
 |
|
|