| |
HCV Innovative Payment Models, Eliminating HCV
|
| |
| |
Download the PDF here
From Jules - my comment is - why is not the federal government bearing full responsibility for full HCV screening & treatment model implementation? These are programs that could & should be carefully constructed by federal agencies & funded by Congress & the White House. the White House announced on May 19 2021 they would eliminate viral hepatitis but we have NOT heard one word since then, dead silence. The CDC gets a mere $39 million a year from Congress for all hepatitis'. The CDC estimates $400 mill year for a time-limited number of years, perhaps 6 years ($2.5 billion), could eliminate HCV, remember HCV is curable with safe, tolerable short-term treatment by diet-actbg antivirals (DAAs) which have shown in studies to be 95%+ effective in curing HCV. The billions of dollars that could be saved by spending a mere $2.5 billion - we would save many more billions in healthcare costs, loss of productivity not to mention the lives & health of many millions of people and their families with HCV. Don't forget HCV affects the most vulnerable in our society. African-Americans, Latinos and the poor are disproportionately affected by HCV. We have had these DAAs for 10-15 years now, that's how long we've known we could cure HC, yet despite this we have continued to only receive $39 million a year from Congress, they have refused to fund this effort. we need routine & mandated HCV screening for all, we need
- We need routine & I think mandated screening for all. Screening is very underutilized in the USA, it is NOT being implemented, without full fledged large-scale commitment to screening we can't eliminate HCV.
- We need culturally apporopriate screening for all affected groups including incarcerated and vulnerable marginalized groups like drug users and their partners, immigrant, homeless.
- We need full public awareness programs that appeal to people from all walks of life including injection drug users & their community; that tries to destigmatize HCV.
- We need adequate & expansion of syringe exchange programs & harm reduction programs, and that provide complete care & services.
- We need HCV treating clinicians that are willing and able to treat injection drug users. There is a big lack of adequate numbers of such clinicians.
- Telehealth can & should be part of the solution. We need to better utilize & expand use of mobile vans for telehealth for HCV treatment, screening & services.
- We need to expand HCV screening & treatment and colocate with Methadone Programs and with Opioid Use Disorder Treatment Programs. We need a national network of infrastructure that provides all this.
- We need to develop rapid (15 minute) point of care testing that can be reliable & accurate.
- we need A Ryan White Care Act -type program for HCV could be a short-term project time limited to 6-7 years. We need an infrastructure & the necessary funding & commitment. If we had a cure for HIV or diabetes or cancer would we NOT provide the infrastructure to offer the cure to all? I do not think so. Its the stigma of drug users associated with HCV that prevents the commitment. HCV is curable with short term treatment by daily pills with 95% cure rates, a great medical milestone.

Sept 2021
INNOVATIVE PAYMENT MODELS: AN ANALYSIS
OF THE PROMISE AND PRACTICE OF NOVEL HCV MEDICATION PROCUREMENT STRATEGIES IN THE U.S.
HEPATITIS C VIRUS (HCV) INFECTIONS continue to be a public health threat in the United States. Several states have invested in innovative payment models to help eliminate cost and access barriers to HCV treatment for people on Medicaid and people in state-operated correctional systems. So far, Louisiana and Washington have implemented innovative payment models for treatment, and Michigan is currently taking steps to implement its model.
However, early analysis shows that they fall short of optimizing the potential benefits achievable when an innovative payment model is utilized. As more states such as Michigan implement HCV innovative payment models, it is important to carefully assess the varied applications of these types of models, progress to-date at increasing HCV treatment rates, and how the plans currently being implemented are impacting access to treatment.
EXISTING INNOVATIVE PAYMENT
MODELS (IPMs)
IPMs are novel drug procurement strategies that secure large quantities of DAA medication to treat the people with HCV who receive state-covered health care through Medicaid or while incarcerated in state correctional facilities at minimal cost. Through IPMs, state health authorities negotiate agreements with pharmaceutical companies for an annual expenditure ceiling. Once
this ceiling is met, each subsequent unit is offered at heavily discounted prices to maintain a nominal net cost throughout the contract period.
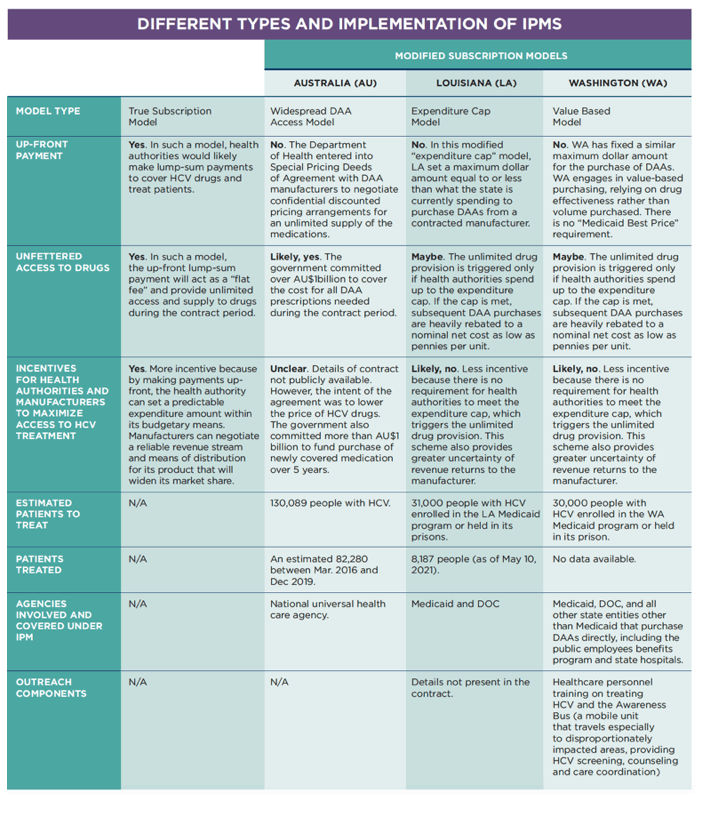
LOUISIANA "EXPENDITURE CAP" MODEL
Louisiana was the first state to implement an innovative payment model to acquire HCV medication. Louisiana's modified payment model set an annual maximum dollar amount (an annual expenditure cap) that the state would pay towards the purchase of DAAs from a contracted manufacturer. Under this expenditure cap agreement, the state purchases DAAs for its Medicaid program from the manufacturer at a negotiated price that utilizes only the federal drug rebates. Drugs for use within the state Department of Corrections would be purchased utilizing 340B rebates to discount the cost.
WASHINGTON'S
VALUE-BASED MODEL
Washington's value-based model allows the state to utilize supplemental rebates to negotiate a low DAA price for the Medicaid program with a manufacturer. Value-based purchasing relies on drug effectiveness rather than volume, and allows the state to negotiate with the manufacturer on terms such as utilization period and outcomes-based benchmarks. Washington's proposal sought to negotiate a guaranteed net per
unit price (GNUP) for the state Medicaid program, the Department of Corrections, and all state entities that purchase DAAs directly, including the public employees benefits program, state hospitals, and workers covered by the state's worker's compensation system.
EMERGING IPM IMPLEMENTATION
IN MICHIGAN
Building upon existing arrangements in Louisiana and Washington with expenditure caps, Michigan entered into an agreement with AbbVie to use Mavyret as the state's preferred HCV medication. Effective April 1, 2021, Michigan Medicaid removed all prior authorizations to prescribe Mavyret for HCV treatment, but prior authorization is required to prescribe a person a different DAA.
IPM PROGRESS TO DATE
Public health interventions of such significant scale should make their data publicly available, as public access to outcomes data can improve community investment and support, garner additional support from important stakeholders, and help hold the agency accountable. However, despite both plans being in Year 2 of implementation, there is a significant difference in the availability of publicly available data on the ongoing progress for Louisiana and Washington's IPM initiatives.
THE FUTURE OF IPMs AND HCV TREATMENT: LOOKING AHEAD
Existing models fall short of achieving true potential. In the absence of strong motivating fiscal incentives for both contracting parties to optimize care-which is the intent of true subscription models-the benefit these models lend to improving HCV treatment outcomes is substantially lessened.
Payment models can be a beneficial tool in a comprehensive elimination strategy. HCV elimination cannot occur unless existing cases are identified, treated, and cured. Greater access to DAAs will not yield the benefit of increasing the number of people cured if no resources exist to inform people of their risk of HCV and to get them screened and enrolled into Medicaid if they are eligible.
| |
| |
| |
|
|
|