| |
A NOVEL APPROACH TO MEASURE PrEP UPTAKE AMONG POPULATIONS WITH PERSISTENT HIV RISK
|
| |
| |
CROI 2021 March 6-10 Reported by Jules Levin
Preeti Pathela1, Saba Qasmieh2, Monica Gandhi3, Elliot Rozen1, Harris Goldstein4, Hideaki Okochi3, Kelly Jamison1, Addie Crawley1, Joan Berman4, Betsy Herold4, Denis Nash2
1New York City Department of Health and Mental Hygiene, Long Island City, NY,
USA, 2City University of New York, New York, NY, USA, 3University of California San Francisco, San Francisco, CA, USA, 4Albert Einstein College of Medicine, Bronx, NY, USA
Background: Persons with sexually transmitted infections (STIs) are prime PrEP candidates, but the accuracy of using self-report to determine PrEP use
is unknown. We used a novel approach to objectively measure PrEP use in a sentinel population largely representative of New York City (NYC) residents diagnosed with STIs, providing information about PrEP uptake and the accuracy of self-report.
- [Why do the assay as part of a study like this? This work confirmed two important things. 1. It is feasible to monitor PrEP drug levels using remnant specimens in a sexual health clinic setting where STIs are diagnosed; and 2. Client self-report of PrEP use correlates very well with actual PrEP use. Before this study, the feasibility was not known, and the extent to which self-report information would be accurate was unknown. One can think of reasons why it would be more or less accurate, including things like prep-related stigma. But it looks as if the vast majority felt comfortable sharing their actual PrEP status. It is not yet totally clear why there was a small level of disagreement, but there could be lots of reasons including that people may not have always been paying attention when answering routine questions as part of medical history, data entry error, and recent PEP use.
In terms of the big picture as to why it is important to have reliable info on PrEP status (self report or biomarker), from a public health standpoint, we have historically been able to rely on trends in STI rates to reflect HIV risk in the population (and identify areas/groups for whom there may be gaps in the HIV prevention 'safety net'). However, in PrEP era, it may no longer be possible to use the STI data for this purpose, especially for men where PrEP uptake is higher and a new STI by definition does not mean increased risk of HIV acquisition. For this reason, it is important for STI programs to have reliable info on PrEP use among those diagnosed with an STI, making it possible to monitor STI trends in individuals who are not on PrEP (which will continue to reflect potential HIV risk).
Why do the assay going forward, given that we found a high level of agreement? We found high agreement between self-report and drug levels among people with newly diagnosed STIs in NYC sexual health clinics. but for reasons of stigma, normalization and other contextual factors, other jurisdictions may find something different. Moreover, things could change with time in NYC making this kind of biomarker approach important. for example if LAI PrEP becomes the norm, or of people use prep more intermittently as opposed to daily.] -
Methods: We systematically accrued remnant serum samples from the following HIV-negative patients screened for syphilis at NYC Sexual Health Clinics (January-June 2019): men who have sex with men (MSM) and women with chlamydia (CT), gonorrhea (GC), and /or early syphilis (ES). Samples were tested for tenofovir/emtricitabine (detected vs. not detected) using a validated liquid chromatography-mass spectrometry (LC-MS) assay. Pairing test results with medical records, we assessed: 1) PrEP use on the day of STI diagnosis, 2) agreement of LC-MS assay with self-reported PrEP, and 3) correlates of PrEP use among MSM with rectal CT/GC or ES.
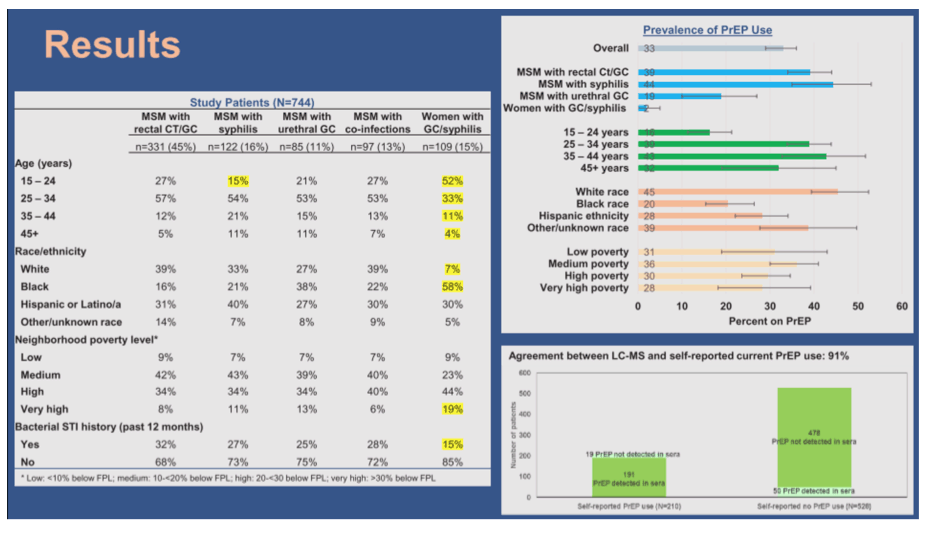
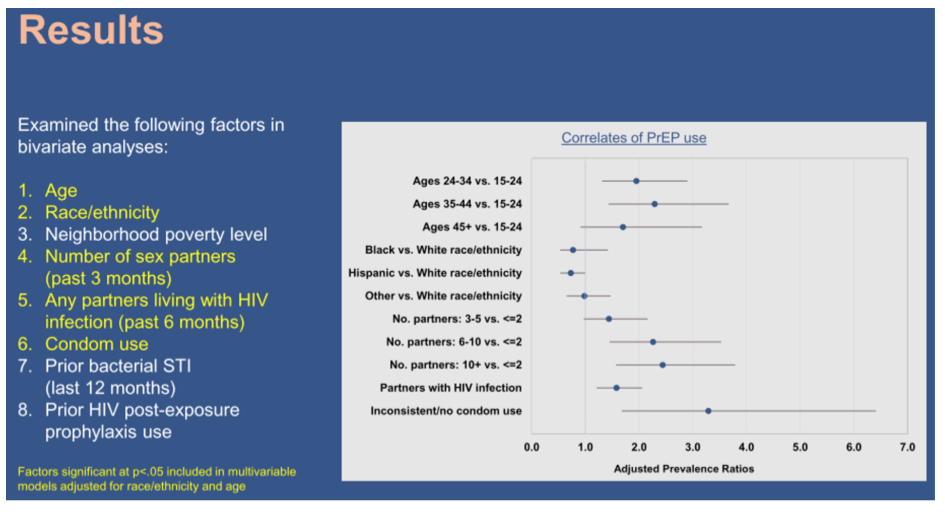
Results: PrEP use among 744 patients (331 MSM with rectal CT/GC, 122 MSM with ES, 85 MSM with urethral GC, 109 MSM with co-infections, 97 women with GC/ES) was 32.8% (95% CI, 29.4%-36.3%). PrEP use was highest among White patients (45%) and MSM with ES (44%), and lowest among Black patients (20%) and women (2%). Agreement between LC-MS and self-reported PrEP use was 91%. Among MSM with rectal CT/GC or ES, PrEP use was associated with age [adjusted prevalence ratio (aPR)=1.6 (95% CI, 1.0-2.5) for ages 25-34 and aPR=2.0 (1.2-3.4) for ages 35-44, vs. 15-24 years]; number of recent sex partners [aPR=2.1 (1.3-3.4) for 6-10 partners and aPR=2.0 (1.2-3.3) for >10 partners, vs. <2 partners]; having sex/needle-sharing partners with HIV [aPR=1.4 (1.0-1.8)]; and inconsistently vs. always using condoms [aPR=3.1 (1.5-6.3)]. Race/ethnicity and past-year history of CT/GC/ES diagnoses or post-exposure prophylaxis were not associated.
Conclusion: This is the first study to analyze routinely collected remnant samples from STI clinics for a PrEP biomarker. Although the accuracy of self- reported PrEP was high, only 1 in 3 people with a newly diagnosed STI was on PrEP. PrEP use was associated with most measured HIV risk factors, but it is critical to increase use in racial minority populations and women. Surveillance studies using remnant samples can assess the accuracy of self-reported PrEP use in other settings and evaluate the success of interventions to increase PrEP uptake in high-risk populations.


|
|
| |
| |
|
|
|