| |
Assessing the health status and mortality of older people over
65 with HIV - greater mortality, more comorbidities
|
| |
| |
Download the PDF here
November 5, 2020
Gina TurriniID1*, Stephanie S. Chan1, Pamela W. KleinID2, Stacy M. CohenID2,
Antigone DempseyID2, Heather Hauck2, Laura W. Cheever2, Andre R. ChappelID1
1 U.S. Department of Health and Human Services, Office of the Assistant Secretary for Planning and Evaluation, Office of Health Policy, Washington, DC, United States of America, 2 Division of Policy and Development, U.S. Department of Health and Human Services, Health Resources and Services Administration, HIV/AIDS Bureau, Rockville, Maryland, United States of America
HHS Study: "Increasing access to care and improving health outcomes for people with HIV is a critical goal of the National HIV/AIDS Strategy 2020. It is important for clinicians and policymakers to be aware that despite significant advances in the treatment and care of people with HIV, older people with HIV have a higher odds of having multiple chronic conditions at any point in time, a higher incidence of new diagnoses of these conditions over time, and a higher hazard of mortality than Medicare beneficiaries without HIV.
These results showed that Medicare beneficiaries living with HIV have a significantly higher hazard of mortality compared to older people without diagnosed HIV (3.6 times the hazard).
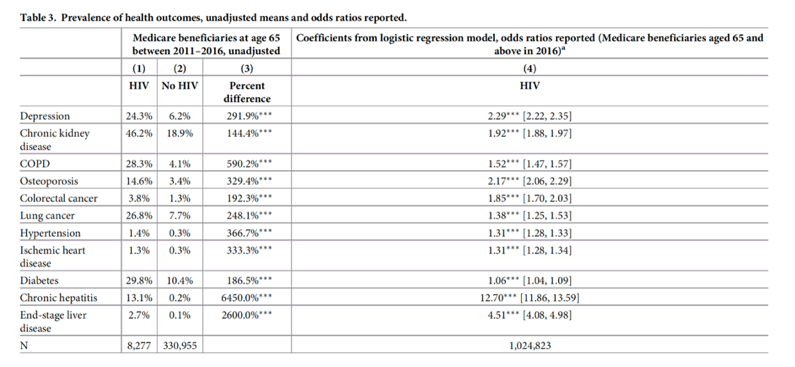
This paper analyzed a large, nationally representative sample of Medicare beneficiaries aged 65 and older from 2011 to 2016 to compare the health and survival status of older people with HIV to an older US population not living with HIV. Prior research has found that older people with HIV have high adherence to treatment which results in high levels of viral suppression [25, 26]. Adherence to treatment and viral suppression are both associated with better health outcomes [51]. Nonetheless, we found that older people with HIV have a higher overall hazard of mortality as well as a higher odds of having depression (2.7times higher), chronic kidney disease 2.3 times higher), COPD(1.67 times higher), osteoporosis (2.6 times higher), colorectal cancer, lung cancer, hypertension, ischemic heart disease (60% higher), diabetes (25% higher), chronic hepatitis, and end-stage liver disease compared to those without HIV, [look at table 5 below] even after adjusting for demographic characteristics. Some of these differences were quite large in magnitude, particularly for hepatitis and end-stage liver disease. Finally, we found that the incidence of diagnosis over time of every condition analyzed is higher for people with HIV, after accounting for the competing and differential risk of mortality.
After adjusting for other demographic and geographic characteristics in the Cox proportional hazard model, an HIV diagnosis was associated with a hazard ratio (HR) of all-cause mortality that was approximately 3.6 times the HR of older adults without diagnosed HIV (column 1 of Table 2). The HR was even higher when we included an interaction with exposure time (years since age 65) to address non-proportional hazards (HR = 5.90), although this ratio decreased by approximately 1% for each year of exposure (column 2). Beneficiaries who are male, non-Hispanic Blacks, rural, or dually enrolled in Medicaid all had higher HRs in every specification of the model. The primary result—the mortality hazard was higher for people with HIV than for people without HIV—was robust across all specifications of the model."
WHY: There are a number of potential reasons why older people with HIV may have different baseline health statuses or trajectories than older people without HIV, and the reasons likely differ by condition. First, HIV itself leads to chronic inflammation, which in turn is associated with systemic chronic immune activation and a higher likelihood of a number of diseases [7-10]. Second, the long-term toxicity of antiretroviral therapies (ARTs) may directly affect the body and may also interact with other medications [11]. Although newer treatment regimens cause fewer side effects than those used in the past, long-term use of ART is associated with increased risk of heart disease and heart attack; use of ART in general may lead to a number of health problems, including liver toxicity, pancreatitis, neuropathy, and impaired glucose metabolism [12, 13]. A third issue is that older people who are newly diagnosed with HIV tend to have more advanced disease due to delayed diagnosis, leading to more advanced immunodeficiency and an increased likelihood of blunted immune response to ART due to immune senescence [14]. This may be partly the result of barriers to early testing and diagnosis for older individuals, such as a lack of awareness of how risk factors may be different for older adults compared to younger individuals, as well as an underestimation of the risk of HIV infection at older ages both by patients and providers [14-18]. Delays in HIV diagnosis are associated with negative health outcomes, decreased life expectancy, and increased HIV transmission [19]. Finally, rates of HIV infection are higher in certain populations that tend to have poorer long-term health outcomes generally, including among men who have sex with men, transgender women, racial and ethnic minorities, and people experiencing poverty [20, 21]. Recently, the prevalence of HIV among people living in rural areas has been increasing, and these individuals are more likely to have delayed diagnosis and to face additional barriers to accessing health care, in general, and from providers with experience treating HIV, in particular [22]. In addition, a range of other adverse health behaviors, such as smoking, are disproportionately common among people with HIV [23, 24].
Abstract
Background
Nearly half of people with HIV in the United States are 50 years or older, and this proportion is growing. Between 2012 and 2016, the largest percent increase in the prevalence rate of HIV was among people aged 65 and older, the eligibility age for Medicare coverage for individuals without a disability or other qualifying condition. Previous work suggests that older people with HIV may have higher rates of chronic conditions and develop them more rapidly than older people who do not have HIV. This study compared the health status of older people with HIV with the older US population not living with HIV by comparing: (1) mortality; (2) prevalence of certain conditions, and (3) incidence of these conditions with increasing age.
We used a sample of Medicare beneficiaries aged 65 and older from the Medicare Master Beneficiary Summary File for the years 2011 to 2016, including 100% of individuals with HIV (N = 43,708), as well as a random 1% sample of individuals without diagnosed HIV (N = 1,029,518). We conducted a survival analysis using a Cox proportional hazards model to assess mortality and to determine the need to adjust for differential mortality in our analyses of the incidence of certain chronic conditions. .
These results showed that Medicare beneficiaries living with HIV have a significantly higher hazard of mortality compared to older people without diagnosed HIV (3.6 times the hazard).
We examined the prevalence of these conditions using logistic regression analysis and found that people with HIV have a statistically significant higher odds of depression, chronic kidney disease, chronic obstructive pulmonary disease (COPD), osteoporosis, hypertension, ischemic heart disease, diabetes, chronic hepatitis, end-stage liver disease, lung cancer, and colorectal cancer.
To look at the rate at which older people are diagnosed with conditions as they age, we used a Fine-Gray competing risk model and showed that for individuals without diagnosis of a given condition at age 65, the future incidence of that condition over the remaining study period was higher for people with HIV even after adjusting for differential hazard of mortality and for other demographic characteristics. Many of these results also varied by personal characteristics including Medicaid dual enrollment, sex, and race and ethnicity, as well as by condition..
Conclusions
Increasing access to care and improving health outcomes for people with HIV is a critical goal of the National HIV/AIDS Strategy 2020. It is important for clinicians and policymakers to be aware that despite significant advances in the treatment and care of people with HIV, older people with HIV have a higher odds of having multiple chronic conditions at any point in time, a higher incidence of new diagnoses of these conditions over time, and a higher hazard of mortality than Medicare beneficiaries without HIV.
|
|
| |
| |
|
|
|