| |
Increased brain-predicted aging in treated HIV disease in COBRA
|
| |
| |
Download the PDF here
James H. Cole, Jonathan Underwood, Matthan W.A. Caan, Davide De Francesco, Rosan A. van Zoest, Robert Leech, Ferdinand W.N.M. Wit, Peter Portegies, Gert J. Geurtsen, Ben A. Schmand, Maarten F. Schim van der Loeff, Claudio Franceschi, Caroline A. Sabin, Charles B.L.M. Majoie, Alan Winston, Peter Reiss, David J. Sharp
First published March 3, 2017
James H. Cole, PhD Jonathan Underwood, MBBS, BSc, Matthan W.A. Caan, PhD, Davide De Francesco, MSc, Rosan A. van Zoest, MD, Robert Leech, PhD Ferdinand W.N.M. Wit, PhD, Peter Portegies, PhD Gert J. Geurtsen, PhD Ben A. Schmand, PhD Maarten F. Schim van der Loeff, PhD, Claudio Franceschi, PhD Caroline A. Sabin, PhD Charles B.L.M. Majoie, MD, PhD Alan Winston, MD, PhD Peter Reiss, MD, PhD David J. Sharp, PhD On behalf of the COBRA
Abstract
Objective: To establish whether HIV disease is associated with abnormal levels of age-related brain atrophy, by estimating apparent brain age using neuroimaging and exploring whether these estimates related to HIV status, age, cognitive performance, and HIV-related clinical parameters.
Methods: A large sample of virologically suppressed HIV-positive adults (n = 162, age 45-82 years) and highly comparable HIV-negative controls (n = 105) were recruited as part of the Comorbidity in Relation to AIDS (COBRA) collaboration. Using T1-weighted MRI scans, a machine-learning model of healthy brain aging was defined in an independent cohort (n = 2,001, aged 18-90 years). Neuroimaging data from HIV-positive and HIV-negative individuals were then used to estimate brain-predicted age; then brain-predicted age difference (brain-PAD = brain-predicted brain age - chronological age) scores were calculated. Neuropsychological and clinical assessments were also carried out.
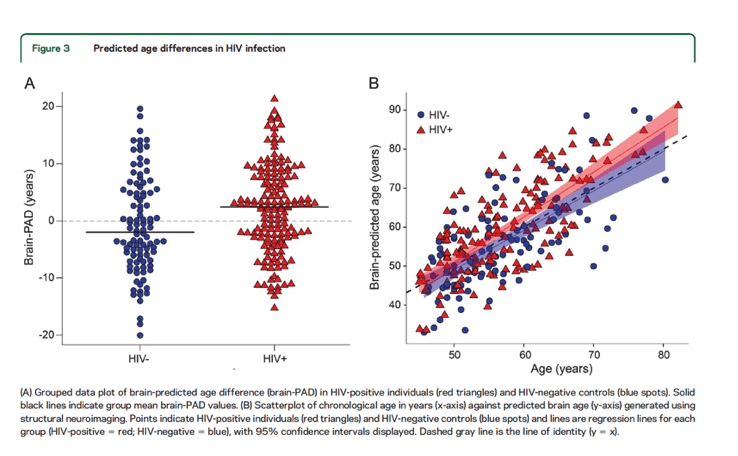
Results: HIV-positive individuals had greater brain-PAD score (mean ± SD 2.15 ± 7.79 years) compared to HIV-negative individuals (-0.87 ± 8.40 years; b = 3.48, p < 0.01). Increased brain-PAD score was associated with decreased performance in multiple cognitive domains (information processing speed, executive function, memory) and general cognitive performance across all participants. Brain-PAD score was not associated with age, duration of HIV infection, or other HIV-related measures.
Conclusion: Increased apparent brain aging, predicted using neuroimaging, was observed in HIV-positive adults, despite effective viral suppression. Furthermore, the magnitude of increased apparent brain aging related to cognitive deficits. However, predicted brain age difference did not correlate with chronological age or duration of HIV infection, suggesting that HIV disease may accentuate rather than accelerate brain aging.
We observed lower brain volumes in HIV-positive individuals, presumably due to atrophy. Our model allows us to quantify this change and relate it to brain structure in healthy individuals. HIV-positive individuals had brains that resembled individuals 2.15 years older. We interpret this as increased brain aging, although one must be cautious in interpreting the results in this way. Brain atrophy does not necessarily mean aging per se. For example, neurologic insults (e.g., stroke, focal lesions from a traumatic brain injury, encephalitis) can result in brain tissue loss that is not primarily due to aging. However, our participants were free from a history of cerebral infections or focal neurologic injury. Hence, gross insults are unlikely to be driving the results. The observed brain tissue loss is likely to be the result of historical damage or the gradual buildup of deleterious factors, such as persistent neuroinflammation. It is unclear whether the biological mechanisms underlying brain tissue loss in HIV are the same as the mechanisms involved in brain aging. However, what is evident at the macroscopic level we have studied (i.e., volumetric MRI) is that the HIV brain appears prematurely aged.
Also, we did not investigate other HIV-related factors not directly associated with the virus that could also affect brain aging, such as antiretroviral toxicity, lifestyle, and cardiovascular disease.38
Participants.
The study included 162 HIV-positive individuals and 105 HIV-negative controls who had highly similar demographic and lifestyle characteristics (table 1). These participants comprised the test set in the machine-learning analysis. Participants were recruited from 2 sites, London and Amsterdam, as part of the Comorbidity in Relation to AIDS (COBRA) collaboration. Exclusion criteria for COBRA were as follows: age under 45 years, current major depression (Patient Health Questionnaire-9 score of ≥15), confounding neurologic diseases, previous severe head injury (loss of consciousness ≥30 minutes), previous cerebral infections (including AIDS-defining CNS diseases), self-reported IV drug use within the last 6 months, daily use of recreational drugs (with the exception of cannabis), excess alcohol intake (>48 units per week), severe psychiatric disease, or MRI contraindications. All HIV-positive participants were required to be on cART and to have had undetectable plasma HIV RNA (<50 copies/mL) for ≥12 months prior to enrollment.
Increased levels of age-associated changes to brain structure were evident in HIV-positive individuals with suppressed plasma HIV viremia, compared to a highly comparable HIV-negative group. The magnitude of increased brain aging (i.e., brain-PAD score), derived from structural neuroimaging, related to neuropsychological test scores. Individuals with older brain-predicted ages, relative to chronological age, showed deficits in information processing speed, executive function, memory, and global cognitive performance. Brain-PAD score did not correlate with chronological age or duration of infection, suggesting that HIV disease does not accelerate the rate of age-associated brain atrophy.
Increased brain-PAD was associated with poorer cognitive performance in multiple domains. The characteristic pattern of age-related cognitive decline is associated with impairments in processing speed, executive function, and memory, while vocabulary and general knowledge are thought to be relatively stable.26 The largest effect sizes for a relationship with brain-PAD score were found for memory, executive function, and processing speed, similar to the expected pattern of typical cognitive aging. However, at least borderline effects were seen in all domains and the strength of these associations was relatively modest. This means that we cannot definitively conclude whether changes in brain-PAD score relate specifically to cognitive aging or more general cognitive impairment. Moreover, cognitive performance between domains is likely to be interrelated, potentially driven by information processing speed,27 or general intelligence.
Interestingly, the relationship between brain-PAD and cognitive performance was seen in both HIV-positive and HIV-negative groups, despite observing greater cognitive impairment in HIV-positive individuals. This implies that brain-PAD reflects a general relationship between brain structure and cognition. HIV is potentially accentuating these age-related changes in brain structure, which then drives deficits in cognitive performance. That the damage to the brain in HIV relates to that seen in normal aging agrees with previous work that has reported a spatial overlap between HIV-associated brain regions and regions associated with aging and cognitive performance in both HIV-positive and HIV-negative individuals.11 Hence, it is plausible that chronic HIV disease could be driving atrophy in brain regions that commonly change with advancing age, resulting in deficits in cognitive performance......We observed lower brain volumes in HIV-positive individuals, presumably due to atrophy.
Neuroimaging-based age predictions may represent a biomarker of the aging process. Such measures could potentially track neurodegeneration in the aging HIV-positive population and identify those at greater risk for poor cognitive outcomes. Cellular and molecular markers of biological aging have also indicated age-like increases in HIV, using telomere length, markers of CD8 T-cell senescence and DNA methylation levels.31,-,35 Our findings generally concur with these reports, which suggests that individuals with chronic HIV disease also experience increased accumulation of the cellular damage associated with aging, resulting in age-like brain atrophy. HIV-positive individuals were on average more than 3 years older compared to the control group. This is a lower estimate compared to age predictions from the epigenetic clock, where brain tissue and blood resulted in 7.4 and 5.2 years of increased aging, respectively.32
|
|
| |
| |
|
|
|