| |
Brief Report: Switching From TDF to TAF in HIV/HBV-Coinfected Individuals With Renal Dysfunction-A Prospective Cohort Study
|
| |
| |
Download the PDF here
JAIDS 2020 -Bernard Surial, MD,a Charles Beguelin, MD,a Jean-Philippe Chave, MD,b Marcel Stockle, MD,c Noemie Boillat-Blanco, MD,d Thanh Doco-Lecompte, MD,e Enos Bernasconi, MD,f Jan Fehr, MD,g,h Huldrych F. Gunthard, MD,g,i Patrick Schmid, MD,j Laura N. Walti, MD,a Hansjakob Furrer, MD,a Andri Rauch, MD,a Gilles Wandeler, MD,a,k and the Swiss HIV Cohort Study
Presented in part at the 17th EACS conference; November 6-9, 2019, Basel, Switzerland
Abstract
Background:
Whereas tenofovir disoproxil fumarate (TDF) can lead to renal adverse events, tenofovir alafenamide (TAF) has a more favorable renal safety profile. However, the impact of replacing TDF with TAF on renal function and liver parameters among HIV/hepatitis B virus (HBV)-coinfected individuals with renal dysfunction remains unclear.
Methods:
We included all participants from the Swiss HIV Cohort Study with an HIV/HBV coinfection who switched from TDF to TAF and had an estimated glomerular filtration rate (eGFR) <90 mL/min/1.73 m2 and a suppressed HIV viral load (<200 cp/mL). We assessed changes in eGFR, urine protein-to-creatinine ratio, and alanine aminotransferase (ALT) after 1 year using mixed-effect models with interrupted time series.
Results:
Among 106 participants (15.1% women, median age 53 years), eGFR was 60-89 mL/min/1.73 m2 in 84 (79.2%) and <60 mL/min/1.73 m2in 22 (20.8%) individuals at the time of switch. One year after the switch from TDF to TAF, individuals with an eGFR between 60 and 89 mL/min/1.73 m2 experienced increases in eGFR of 3.2 mL/min/1.73 m2 (95% confidence interval [CI] 1.2 to 5.2), whereas those with an eGFR <60 mL/min/1.73 m2 experienced improvements of 6.2 mL/min/1.73 m2 (95% CI 2.4 to 10.0). Urine protein-to-creatinine ratio decreased overall (-6.3 mg/mmol, 95% CI -10.0 to -2.7), and ALT levels declined in patients with elevated baseline levels (-11.8 IU/L, 95% CI -17.3 to -6.4) 1 year after replacing TDF with TAF.
Conclusions:
Switching from TDF to TAF among HIV/HBV-coinfected individuals with renal impairment led to improvements in eGFR, a decline in proteinuria, and to ALT normalization in those with elevated ALT levels.
Changes in eGFR and Urine Protein-To-Creatinine Ratio
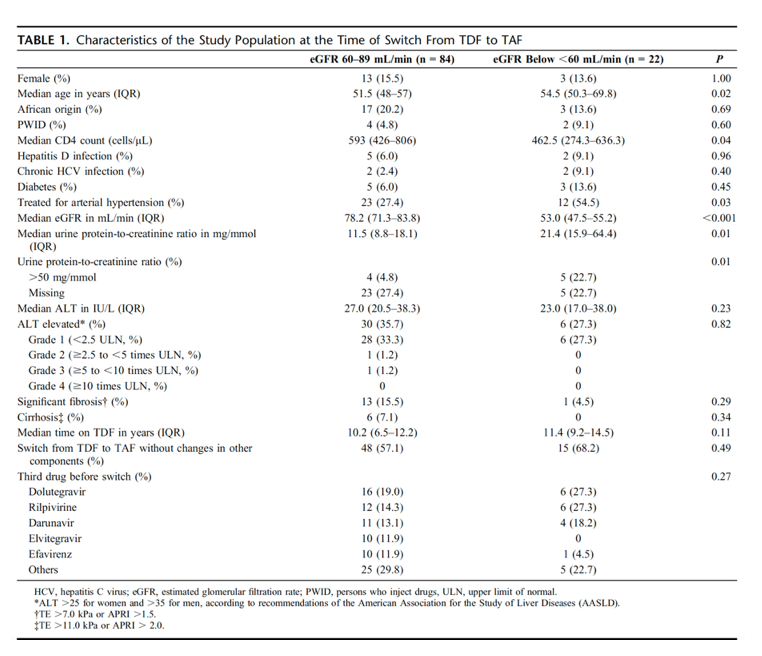
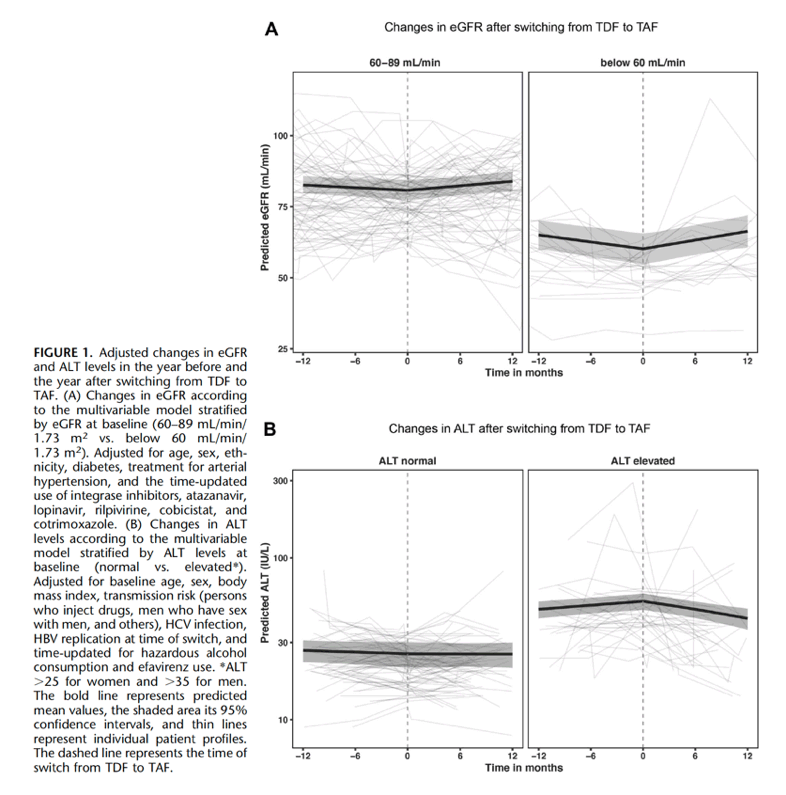
Adjusted mean changes in eGFR are shown in the Figure 1A. Individuals with an eGFR between 60 and 89 mL/min/1.73 m2 experienced changes in eGFR of -1.9 mL/min/1.73 m2 in the last year on TDF [95% confidence interval (CI) -3.3 to -0.5], which increased to 3.2 mL/min/1.73 m2 1 year (95% CI 1.2 to 5.2) after switching to TAF (P value for slope difference 0.001). The use of TDF in individuals with an eGFR below 60 mL/min/1.73 m2 led to a decline in eGFR (-4.9 mL/min/1.73 m2 in the year before switch, 95% CI -7.5 to -2.2), and switching to TAF was associated with improvements in eGFR (6.2 mL/min/1.73 m2 1 year after the switch, 95% CI 2.4 to 10.0, P value for slope difference <0.001).
One year after switching to TAF, 58 (54.7%) individuals had urine protein-to-creatinine ratio values available, and the main demographic and clinical characteristics, including eGFR at baseline, were similar between the group with and without follow-up data. After adjusting for covariates, the use of TDF was associated with a change in urine protein-to-creatinine ratio of 0.9 mg/mmol in the last year before switch (95% CI -2.5 to 4.3), and switching to TAF led to a change in urine protein-to-creatinine ratio of -6.3 mg/mmol 1 year after the switch (95% CI -10.0 to -2.7, P-value for slope difference 0.01). Changes in urine protein-to-creatinine ratio after 1 year did not correlate with changes in eGFR over the course of time (correlation coefficient -0.02, P = 0.91). Our findings on eGFR and urine protein-to-creatinine ratio remained similar after restricting the analyses to individuals who had the replacement of TDF by TAF as the only ART change (see Table S1, Supplimental Digital Content, http://links.lww.com/QAI/B499).
In this study switching to TAF was associated with improvements in renal function, which was most pronounced in individuals with a baseline eGFR below 60 mL/min/1.73 m2. Changes in eGFR were not correlated with improvements in urinary protein-to-creatinine ratios because switching from TDF to TAF led to reductions in proteinuria irrespective of the eGFR at baseline.
|
|
| |
| |
|
|
|