| |
Cross-sectional study of correlates and prevalence [high rates] of functional and high-risk multimorbidity in an academic HIV practice in New York City at Cornell-Weill HIV Clinic
|
| |
| |
Download the PDF here
Eugenia Siegler ,1 Jerad Moxley ,1 Elizabeth Mauer ,2,3 Marshall Glesby
----------------------------------
Eugenia Siegler, MD, on Functional and High-Risk Comorbidities in PLWH: Geriatricians are taught to think functionally, and I was struck by how often people had difficulty walking and doing daily tasks. Study notes that age, longer time with an HIV diagnosis, and Black race was associated with high-risk comorbidities, while age, being a cisgender woman, Hispanic ethnicity, and longer time with an HIV diagnosis was associated with a higher number of functional comorbidities. Multimorbidity often leads to polypharmacy, and reducing medication burden is often very difficult. Reviewing the medication list and asking which medications can be discontinued is essential. Finding the time as a clinician to ask the patient how he or she feels about aging is challenging, but in my experience, it is a worthwhile investment, even for PLWH who are in their 50s or 60s.
For people living with HIV (PLWH), comorbidities account for a large part of their disease burden and, therefore, their management plans. However, the focus of these comorbidities by researchers often fails to include sufficient consideration for functional comorbidities. To provide well-rounded care for PLWH, health care providers must consider the impact of both high-risk and functional comorbidities over the course of their patients' lives.
Many people have multiple comorbidities, also known as multimorbidity. It can be frustrating for a patient who is already taking multiple medications for their hypertension, diabetes, and hyperlipidemia to hear that you want to investigate whether they have other comorbidities. But taking a functional approach helps-asking, for example, if they are having difficulty hearing, seeing, climbing stairs, maintaining their balance, dealing with pain, or concentrating. It enables you to address the comorbidities that underlie these impairments. It also encourages the patient to talk about aging concerns.
https://www.consultant360.com/exclusive/infectious-diseases/hiv-management/eugenia-siegler-md-functional-and-high-risk
--------------------------
Functional & High Risk Comorbidities Common in all age groups Increasing with Age. "High-Risk" Comorbidities (high impact on mortality) associated with aging & more years with HIV, being African-American, Hispanic, cisgender female.
Conclusions Comorbidities with functional impact increase with age in parallel to those with a more direct impact on mortality and should be assessed and monitored, especially as the population with HIV ages.
• Number of comorbidities, as expected, increased with age, starting with a median of 1 (IQR=0-3) for those under 50 and increasing to a median of 5 (IQR=4-7) in the 75+ age group.
• Comorbidities of each classification were common, with slightly more high-risk than functional comorbidities in each age category. Although some participants had no comorbidities, the maximum number of comorbidities was 13 inclusive, with 8 in the high risk and 7 in the functional categories.
• All PWH >75 had at least one comorbidity but look in table 1 you see 74% of the <50 had a comorbidity & 98% of those 65-74.
• Different comorbidities showed different patterns with age. Some, like cardiovascular disease (CVD), genitourinary disease and hypertension (HTN), demonstrated marked increase in risk with increasing age. Other comorbidities like gastrointestinal disease or cancer demonstrated a weaker link. Mental health problems were highly prevalent in all age groups, slightly more so in older patients. Obesity, although common, showed no relationship to age.
Results Median age was 52 years (IQR 43-59). Cisgendered women comprised 24.6% of the sample, and 31.7% were African-American. Both functional and high-risk comorbidities were common and risk increased with age. Among those 75 and older, median number of both functional and high-risk comorbidities was 3 (IQR 2-4). High-risk comorbidities were associated with age (p<0.001), more years with an HIV diagnosis (p<0.001) and being an African-American (p<0.001). Associated with a higher number of functional comorbidities were age (p<0.001), being a cisgender female (p<0.001), being Hispanic (p=0.01) and more years with an HIV diagnosis (p<0.001). Conclusions Comorbidities with functional impact increase with age in parallel to those with a more direct impact on mortality and should be assessed and monitored, especially as the population with HIV ages.
The study was conducted at HIV Clinic, the Centre for Special Studies at the Weill Cornell Campus of New York Presbyterian Hospital. The significant burden of functional multimorbidity described in this study highlights the importance of acknowledging and addressing this burden. Median age was 52. Racially diverse 29% hispanic, 31% African-American. More than half of those 65 & older were former smokers. The most common risk factor for HIV was MSM (57%) with unprotected heterosexual sex being 2nd. Medical number of years with HIV was 19. It is based on automated extraction of ICD-10 codes and labs from an EHR; neither patient interview nor note review was possible to add missing data, making it likely that some comorbidities, particularly arthritis, were underestimated.23 Geriatric syndromes like frailty or social stressors like loneliness are rarely coded as ICD-10 diagnoses and are also missing from the analysis. In addition, ICD-10 codes were extracted from the past medical history, surgical history and problem list, and these are only as accurate as the providers maintaining them.
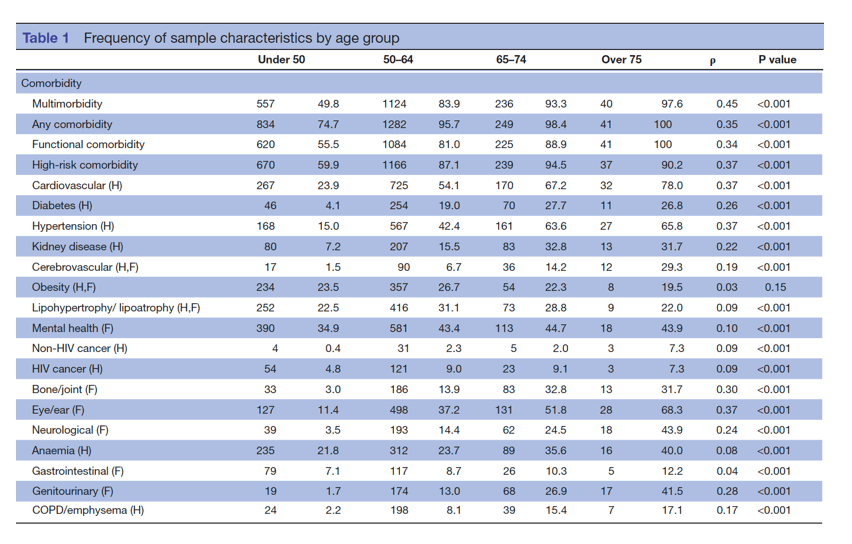
HIGH RISK Comorbidities (Table 1): cardiovascular, hypertension, kidney disease, cerebrovascular, lipohypetrophy/lipoatrophy, non-HIV cancer, bone/joint, neurological, gastrointestinal, COPD, emphysema.
NEUROLOGIC DISEASE: 3.5% <50 had this; 14% of 50-64; 24% of 65-74; 43% of >75.
KIDNEY DISEASE: 32% of 65-74.
MENTAL HEALTH: 34% <50; 44% 65-74.
HIGH-RISK Comorbidity: 59% <50; 94% 65-74
Functional comorbidity: 55% <50 had this; 81% of 50-64; 89% of 65-74; 100% of >75 years old.
Conclusions
In our large sample of adults with HIV, we found significant burdens of functional multimorbidity in addition to high-risk comorbidities. Diseases that have an impact on function are highly prevalent and increase with age; they likely are additive to the more commonly recognised comorbidities seen in this population and may have a significant impact on quality of life. Future research is needed to better define and catalogue functional comorbidities, understand how they cluster and who is at highest risk for them, and assess their impact on people ageing with HIV.
Comorbidities were classified in several ways. We first used a very inclusive definition, including all of the comorbidities that were in the original database. We also used more specific measures, one focused on diseases that had a high impact on mortality, termed 'high-risk' and the other focused on diseases that had a higher impact on functional impairment (eg, walking or carrying out tasks of daily living), termed 'functional'. In the absence of a literature to categorise them, these comorbidities were grouped by consensus of two of the study authors (ELS, MJG) prior to the analysis. The classification for each of the comorbidities is presented in abbreviated fashion in table 1. More detail is provided in online supplemental digital content table 2. Three of the comorbidities (cerebrovascular disease, lipohypertrophy/lipoatrophy and obesity) were felt to have significant high-risk and functional implications, and were included in both groups.
Functional comorbidities
Associated with a higher number of functional comorbidities were age (p<0.001), being a cisgender female (p<0.001), being a transgender FTM (p<0.001), being Hispanic (p<0.01) and having more years with an HIV diagnosis (p<0.001). No variables were associated with having fewer number of functional comorbidities.
The clinic population is large and diverse, and our findings are generalisable to the larger population with HIV: The significant burden of functional multimorbidity described in this study highlights the importance of acknowledging and addressing this burden.
Guaraldi et al2 evaluated people treated at Modena University and included five comorbidities: CVD (combining myocardial infarction, stroke, coronary artery bypass surgery, angioplasty and angina into one category), HTN, diabetes mellitus (DM), renal disease and fractures, and found that the prevalence of multimorbidity was 46.9% in people with HIV over 60 years of age.
Wong et al20 examined the NA-ACCORD population and restricted their comorbidity list to HTN, DM, chronic kidney disease, hypercholesterolemia, end-stage liver disease and non-AIDS-related cancers, and found a prevalence of multimorbidity in people with HIV 60 and older in 2009 to be 53%.
Maggi et al16 evaluated eight categories (CVD events, DM, HTN, dyslipidaemia, hepatitis C antibody positive, psychiatric illness, osteopenia/osteoporosis and renal impairment), and found that 77.1% of people 60 and older with HIV had multimorbidity.
our study also investigated other, highly prevalent functional comorbidities that have significant impact on quality of life.
Multimorbidity, frailty and mortality are interrelated.21 Multimorbidity can be studied to elucidate prognosis as well as aetiology of disease. Multimorbidity has been used to predict mortality and functional decline22 23;
It is not surprising that in our study age was the strongest driver of most individual comorbidities and multimorbidity.
Our findings that women had higher multimorbidity burdens than men are also consistent with the literature26 27 although this seemed to hold only for functional multimorbidity; a recent study also found thatwomen had poorer physical function than men, lending credence to our findings of high functional burden in this group.28
The risk of individual comorbidities and multimorbidity is higher in people with HIV than in their counterparts without HIV,2-5 and the impact of this higher prevalence is not fully understood. In this study, we have used the electronic record of a university-based practice caring for a large, diverse population with HIV and demonstrated that: (1) Comorbidities with primarily functional consequences had a prevalence as high as those with a direct impact on mortality; (2) Different comorbidities had different relationships to age and (3) Although age and number of years with an HIV diagnosis were associated with both high-risk and functional comorbidities as a group, being Hispanic, cisgender female and FTM transgender were associated with functional comorbidities.
Cross-sectional study of correlates and prevalence of functional and high-risk multimorbidity in an academic HIV practice in New York City
Eugenia Siegler ,1 Jerad Moxley ,1 Elizabeth Mauer ,2,3 Marshall Glesby
Abstract
Objectives People with HIV have high levels of multimorbidity, but studies often focus on high-risk comorbidities such as hypertension or coronary artery disease. We examined both high-risk and functional comorbidities in an ethnically diverse clinic population to compare the prevalence of comorbidities and different patterns of multimorbidity.
Design Retrospective cross-sectional study.
Setting University-based primary care HIV clinic with two locations in New York City.
Participants Patients who had been seen by a physician at least once between 1 June 2016 and 31 May 2017.
Primary and secondary outcome measures Data regarding demographics, diagnoses and lab values were downloaded in a one-time data import from the electronic medical record. Comorbidities were classified as high-risk (with major impact on mortality) or functional (with major impact on function), and multimorbidity was determined for both classes in the total sample of 2751. Factors associated with high-risk and functional multimorbidity were determined first through bivariate analysis and then through multivariable median regression in 2013 patients with complete data.
Results Median age was 52 years (IQR 43-59). Cisgendered women comprised 24.6% of the sample, and 31.7% were African-American. Both functional and high-risk comorbidities were common and risk increased with age. Among those 75 and older, median number of both functional and high-risk comorbidities was 3 (IQR 2-4). High-risk comorbidities were associated with age (p<0.001), more years with an HIV diagnosis (p<0.001) and being an African-American (p<0.001). Associated with a higher number of functional comorbidities were age (p<0.001), being a cisgender female (p<0.001), being Hispanic (p=0.01) and more years with an HIV diagnosis (p<0.001).
Conclusions Comorbidities with functional impact increase with age in parallel to those with a more direct impact on mortality and should be assessed and monitored, especially as the population with HIV ages.
Strengths and limitations of this study
• It examines both functional and high-risk multimorbidity in older people with HIV.
• The study population is large and diverse.
• It distinguishes between age-related and non-age-related comorbidities in this population.
• It is from a single academic medical centre in New York City.
• It is based on extraction of data from an electronic health record.
Introduction
With the advent of effective anti-retroviral medication, people are living with HIV as a chronic disease. Although many people with HIV can live to near-normal life spans,1 they are at higher risk than their HIV negative counterparts for comorbidities2-5 like heart disease,6 bone disease7 and neuropsychiatric illnesses like depression,8 as well as geriatric syndromes like falls and frailty.9 Geriatric assessment, which evaluates the impact of medical and psychosocial factors on individual's function, has been proposed as a way to help optimise care of people with HIV as they age.10 WHO supports this focus on function, defining healthy ageing as 'the process of developing and maintaining the functional ability that enables well-being in older age'.11
Multimorbidity, which has been defined as the presence of two or more chronic conditions,12 is increased in the population with HIV.13 14Multimorbidity has been assessed in a wide variety of ways, with instruments measuring anywhere from 4 to 102 different conditions.15Recent studies have identified multimorbidity clusters16 as a way of generating hypotheses regarding disease aetiology and risk. The focus of these studies has largely been on illnesses with significant impact on mortality. In ageing populations in particular, mortality impact is insufficient; it is important to examine multimorbidity in terms of functional impact, as well.
Many of the studies documenting multimorbidity have been conducted as prospective cohorts using very selective populations. The advent of the electronic health record (EHR) has enabled providers to maintain a more comprehensive past medical history and problem list, and despite its drawbacks,17 has provided opportunities to expand study populations to a more representative sample of people with HIV in the community who are receiving medical care. We took advantage of such a system to study the characteristics of the patients who attended a dedicated HIV Clinic, the Centre for Special Studies at the Weill Cornell Campus of New York Presbyterian Hospital. This clinic, which dates from the early days of the AIDS epidemic, provides care for approximately 3000 people who have HIV throughout the New York City metropolitan area. This enables the study of a large, diverse group of people with HIV without the selection bias associated with studies of voluntary study participants. Our objectives for this study were to examine the prevalence of various comorbidities in a real-world sample, and to evaluate the relationship between functionally important and high-risk comorbidities, HIV parameters and age.
Results
All comorbidities
Associated with a higher number of comorbidities were age (p<0.001), being a cisgender female (p=0.04), being a transgender FTM (p=0.04), more years with an HIV diagnosis (p<0.001), being a Hispanic-American (p=0.03), and being an African-American (p<0.001). Associated with fewer comorbidities were having the risk factors of MSM (p<0.001) and USWOS (p=0.009). Note in this analysis and for the other comorbidities following, the FTM effect was statistically significant in all three analyses, but there was only one person in the smaller sample.
High-risk comorbidities
Associated with a higher number of high-risk comorbidities were age (p<0.001), being a transgender FTM (p=0.04), more years with the diagnosis (p<0.001) and being an African-American (p<0.001). Associated with fewer comorbidities were having the risk factors of MSM (p<0.001) and IDU (p=0.007). The interaction of age and being a former smoker was also significant (p=0.001) and positive, indicating that the risk from being a former smoker increased with age.
Functional comorbidities
Associated with a higher number of functional comorbidities were age (p<0.001), being a cisgender female (p<0.001), being a transgender FTM (p<0.001), being Hispanic (p<0.01) and having more years with an HIV diagnosis (p<0.001). No variables were associated with having fewer number of functional comorbidities.
Discussion
The risk of individual comorbidities and multimorbidity is higher in people with HIV than in their counterparts without HIV,2-5 and the impact of this higher prevalence is not fully understood. In this study, we have used the electronic record of a university-based practice caring for a large, diverse population with HIV and demonstrated that: (1) Comorbidities with primarily functional consequences had a prevalence as high as those with a direct impact on mortality; (2) Different comorbidities had different relationships to age and (3) Although age and number of years with an HIV diagnosis were associated with both high-risk and functional comorbidities as a group, being Hispanic, cisgender female and FTM transgender were associated with functional comorbidities.
Multimorbidity is simple in its fundamental definition, that is, two or more chronic comorbidities, but complex in its meaning. Prevalence of multimorbidity is highly variable and depends on the number of comorbidities under study. For example, Guaraldi et al2 evaluated people treated at Modena University and included five comorbidities: CVD (combining myocardial infarction, stroke, coronary artery bypass surgery, angioplasty and angina into one category), HTN, diabetes mellitus (DM), renal disease and fractures, and found that the prevalence of multimorbidity was 46.9% in people with HIV over 60 years of age. Wong et al20 examined the NA-ACCORD population and restricted their comorbidity list to HTN, DM, chronic kidney disease, hypercholesterolemia, end-stage liver disease and non-AIDS-related cancers, and found a prevalence of multimorbidity in people with HIV 60 and older in 2009 to be 53%. Maggi et al16 evaluated eight categories (CVD events, DM, HTN, dyslipidaemia, hepatitis C antibody positive, psychiatric illness, osteopenia/osteoporosis and renal impairment), and found that 77.1% of people 60 and older with HIV had multimorbidity. As with these studies, our sample demonstrated high levels of multimorbidity, given the inclusiveness of our definition. Of note, these studies focused largely on high-risk comorbidities (except osteoporosis/fractures and mental health); our study also investigated other, highly prevalent functional comorbidities that have significant impact on quality of life.
Multimorbidity, frailty and mortality are interrelated.21 Multimorbidity can be studied to elucidate prognosis as well as aetiology of disease. Multimorbidity has been used to predict mortality and functional decline22 23; in these analyses, individual comorbidities are chosen based on impact and are usually assigned weights, the sum of which provides an assessment of risk. Multimorbidity studies have also examined the relationships between comorbidities. In these cases, comorbidities can be grouped together through common etiologies (eg, linkage to obesity),24 or used to identify unexpected clusters.16 25
It is not surprising that in our study age was the strongest driver of most individual comorbidities and multimorbidity. We did note that while age had a strong influence on both functional and high-risk multimorbidity, individual comorbidities demonstrated different age-related patterns. It is likely that obesity and mental health burdens did not change substantially with age as they showed high prevalence in all ages.
Our findings that women had higher multimorbidity burdens than men are also consistent with the literature26 27 although this seemed to hold only for functional multimorbidity; a recent study also found that women had poorer physical function than men, lending credence to our findings of high functional burden in this group.28 We cannot rule out diagnostic bias as a reason why women did not have a higher prevalence of high-risk multimorbidity in our population.
EHR data are incomplete,29 30 and there are biases in choosing to evaluate complete records rather than being more inclusive and analysing all records.31 We chose to feature those with complete demographic and HIV-related data because of the importance of these variables. In general, other risk factors for each type of multimorbidity were similar in both the partial and full samples.
Certain findings are surprising. In the high-risk multimorbidity sample, we found that IDU, like MSM, was associated with fewer comorbidities. We do not know if this is related to unknown confounders or biases such as earlier death in the most vulnerable; we also do not know the duration of IDU. This inverse association with IDU did not hold true for functional multimorbidity. In addition, we found that current tobacco use was not associated with greater numbers of both high-risk and functional comorbidities, although having quit was associated with increased risk in the full sample. We do not know how many pack-years patients in this cohort have smoked, or when they quit. There was an interaction between having quit and age for those with high-risk multimorbidity, and we suspect that older smokers may have been more likely to quit because of poor health. This may explain the paradoxical finding that having quit smoking correlated with high-risk comorbidity. Rather, those who are older may not have benefited from having quit smoking and yet may still carry the risk of many years of tobacco use.
We were interested in comorbidity as encountered by the clinician, not as a predictive measure. Overall comorbidity burden has an impact on both mortality and function,23 and our decision to divide comorbidities into those with mortality and functional impact was not designed for prognostic purposes; instead it was designed from the clinician's perspective, in directing attention and resources to patients and subpopulations. The clinic population is large and diverse, and our findings are generalisable to the larger population with HIV: The significant burden of functional multimorbidity described in this study highlights the importance of acknowledging and addressing this burden.
There are a number of limitations to this study. It is from a single academic medical centre in New York City, but its size and the diversity of its population compensate to a large degree. It is based on automated extraction of ICD-10 codes and labs from an EHR; neither patient interview nor note review was possible to add missing data, making it likely that some comorbidities, particularly arthritis, were underestimated.23 Geriatric syndromes like frailty or social stressors like loneliness are rarely coded as ICD-10 diagnoses and are also missing from the analysis. In addition, ICD-10 codes were extracted from the past medical history, surgical history and problem list, and these are only as accurate as the providers maintaining them. Because of this, there is no method to determine if a problem was resolved or considered active. Another limitation of this study is the lack of literature classifying comorbidities; for this reason, the authors determined which comorbidities would fall into the functional and high-risk classification groups; while these were determined a priori, there may be some unknown bias in the choices. There were insufficient data about socioeconomic status to add these data to the analysis, and this may have resulted in unknown confounding. Finally, we cannot rule out diagnostic bias as a reason for differences in morbidity prevalence in different demographic groups.
Conclusions
In our large sample of adults with HIV, we found significant burdens of functional multimorbidity in addition to high-risk comorbidities. Diseases that have an impact on function are highly prevalent and increase with age; they likely are additive to the more commonly recognised comorbidities seen in this population and may have a significant impact on quality of life. Future research is needed to better define and catalogue functional comorbidities, understand how they cluster and who is at highest risk for them, and assess their impact on people ageing with HIV.
|
|
| |
| |
|
|
|