| |
"I'm Just Forgetting and I Don't Know Why": Exploring How People Living With HIV-Associated Neurocognitive Disorder View, Manage, and Obtain Support for Their Cognitive Difficulties - study interviewing 25 PLWH average age 51 diagnosed with HAND (HIV-associated neurocognitive disorder)
|
| |
| |
Download the PDF here
"The term cognition refers to the high-level functions of the brain, such as speaking, seeing, calculating, processing information, remembering, planning and problem-solving. When these processes are reduced, experts use the term neurocognitive impairment, or NCI."
from long-time HIV+ Maggie Atkinson's story - see below
The clinical characteristics of HAND have been well-documented in neuropsychological studies, which show that HAND may be associated with changes in learning, memory, attentional, and executive processes affecting health, quality of life, dulled senses, and work productivity. Despite clinical knowledge of the disorder, the lived experience of HAND has received little attention.
Here is a study reported at the European AIDS Conference in October 2021
EACS: A fog that impacts everything: understanding quality of life in people living with HIV and cognitive impairment - poor mental & physical function - (11/06/21) 25 PLWH describe their cognitive impairment & impact on quality of life ....affects on sigma, self-esteem, memory, poor concentration, poor physical & metal function - This study described broad impacts on QOL across physical, psychological, and social functioning. In addition, the direct effects of their cognitive symptoms, experiences associated with living with HIV, and perceived control, along with acceptance of health conditions emerged as important factors impacting on QOL experiences.
https://www.natap.org/2021/HIV/112121_01.htm
- older PLWH report forgetting appointments & taking medications & meals, fear of revealing cognitive difficulties to anyone or their doctors, internalized stigma feeling stupid. Many older people with & without HIV do not want to hear the term aging nor cognitive impairment, these terms can have a lot of stigma attached that people do not want to feel the terms apply to them. Many older or elderly PLWH can get very defensive if one suggests they could get cognitive impairment. But in reality all people, with or without HIV, age & many have mild cognitive function decline, the mildest form is called "asymptomtic - (signs of impairment on neuropsychological tests but no loss of function in day-to-day life) to mild (signs of impairment in both tests and daily living) to the most severe form, HIV-associated dementia (HAD).
Abstract
HIV-associated neurocognitive disorder (HAND) is common, but the lived experience of HAND is not well-understood. In this descriptive qualitative study, we explored how adults with HAND view, manage, and obtain support for cognitive difficulties. We interviewed 25 participants (20% female; median age = 51 years) who were diagnosed with HAND using neuropsychological assessment and a clinical interview. Semistructured interviews, co-developed with community members living with HIV, focused on how cognitive difficulties manifested and progressed, impacted well-being, and were discussed with others. We analyzed interview transcripts using a team-based, thematic approach. Participants described concentration, memory, and multitasking difficulties that fluctuated over time, as well as potential risk factors, management strategies, and psychosocial consequences. They reported they seldom discussed cognitive impairment with health care professionals, and that receiving a HAND diagnosis was validating, informative, yet somewhat disconcerting. Conversations between health care professionals and people living with HIV about HAND may provide opportunities for education, assessment, and support.
In this study, participants expressed not only relief and validation but also shock and doubt, in response to their HAND diagnosis...... our participants reported concentration, multitasking, and memory difficulties that varied in degree depending on factors such as stress, sleep, and mood, and produced negative emotional reactions including frustration, embarrassment, and worry.
Many participants recollected missing or forgetting meals, medication, and medical appointments. As one participant with MND described, "I had an appointment, a hearing test, a while ago . ."My memory problems interfere with my remembering to take pills, for example, and my remembering to eat." Most participants recalled one or more instances when their cognitive difficulties interfered with their health behaviors.......Participants often indicated they rarely discussed their cognitive difficulties with their primary care physicians and HIV specialists.
Participants indicated that they had minimal discussions about their cognitive functioning with primary care physicians and HIV specialists. The development or identification of brief screening tools for HAND is necessary to increase access to cognitive screening and identify those who may benefit from further assessment and/or intervention.
---------
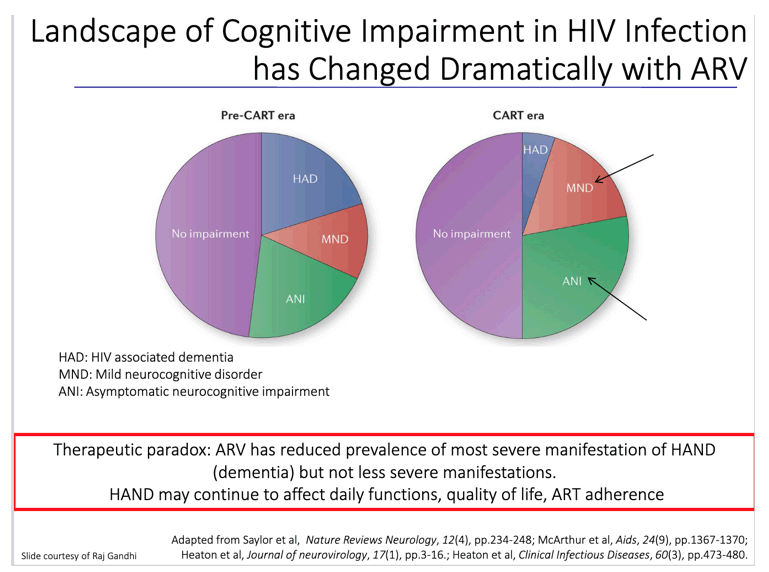
HIV-associated neurocognitive disorder (HAND) is increasingly recognized as a concern among people living with HIV. HAND comprises three diagnostic categories, namely, asymptomatic neurocognitive impairment (ANI; characterized by mild cognitive impairments that do not interfere with daily functioning), HIV-associated mild neurocognitive disorder (MND; where cognitive impairments have a mild but noticeable or significant impact on daily functioning), and HIV-associated dementia (HAD; characterized by moderate to severe deficits that cause marked impairment in performing day-to-day tasks. Despite the decline of HAD with the advent of HIV treatment, milder forms of HAND remain common. Approximately 50% of people living with HIV are estimated to experience HAND (Clifford & Ances, 2013; Woods et al., 2009), making it an important health condition to examine in the context of HIV.
Notably, past research suggests that HIV stigma can be a barrier to conversations with family, friends, and health care professionals about health problems and behaviors. A novel finding in this study, and contribution to the literature, was that conducting a comprehensive, "gold standard" neurocognitive assessment for the diagnosis of HAND, particularly ANI and MND, and sharing the results and implications of the assessment with participants, was favorably received and an important intervention to reduce worry and rumination.
Enacted stigma
Participants described criticism they had received from others in response to their attentional and memory lapses. A man with MND said his children think, "When dad forgets, he's stupid." A woman in her early 50s with MND recalled, [M]y daughter criticized me about the way, you know, I behave. I behave like I'm not in my sound mind or I can't remember things. They treat me like I'm not competent enough to be with their children alone or for me to take them out . . . It's not like I'm out with the kids on the subway and then suddenly I remember "Oh, you're with me." That doesn't happen.
Participants often indicated they rarely discussed their cognitive difficulties with their primary care physicians and HIV specialists. When asked if he had spoken to a health care professional about his cognitive challenges, a man with MND responded, "I don't think so, no. That's sort of something I've always thought I'd have to take on myself." Those who reported having the conversations about cognitive difficulties indicated that the conversations were limited. As a man in his late 40s recounted, "[M]y family doctor . . . might be the only person I would have talked to about memory, but nothing extensive or anything." Alternatively, another man with MND recalled saying to his health care professional, "I have . . . lost some valuable things and I don't know why . . . I just want to know if it's HIV."
The clinical characteristics of HAND have been well-documented in neuropsychological studies, which show that HAND may be associated with changes in learning, memory, attentional, and executive processes affecting health, quality of life, and work productivity. Despite clinical knowledge of the disorder, the lived experience of HAND has received little attention.

With advances in HIV research, our understanding of the effects of HIV on the brain has become more nuanced. Now, experts often speak of HIV-associated neurocognitive disorders (HAND). This umbrella term covers a range of disorders of increasing severity- from asymptomatic (signs of impairment on neuropsychological tests but no loss of function in day-to-day life) to mild (signs of impairment in both tests and daily living) to the most severe form, HIV-associated dementia (HAD).
https://www.natap.org/2017/IDWeek/Mukerji_IDweek_2017.pdf
I first noticed a slight reduction in my ability to think clearly in 1993, when my CD4+ cell count fell below 200. I just didn't feel as sharp.
A year later, when I got PCP, the life-threatening pneumonia that is a hallmark of AIDS, my handwriting deteriorated so much that I had to concentrate to write legibly. About five years ago, I started having trouble remembering names of famous people. Over the next couple of years, these memory lapses progressed to the names of colleagues and then friends, which was awkward, to say the least.
I also began to have difficulty finding words. It started with complex words. My brain would substitute another similar-sounding or simpler word. My sentences began to be filled with "thing" or "stuff" or "you know." As it got worse, I forgot everyday words.
As an AIDS activist, I used to speak in public regularly. Gradually, I began to shy away from those activities because it was embarrassing to be fumbling for words. I was acting like a stereotypical geriatric, not a 40-something lawyer.
Fortunately, about two years ago, I found some strategies that helped and I've gotten much, but not all, of my functioning back. Based on my personal experience and some additional research, here is what I learned about protecting the brain.
Experts are still not sure how common NCI is. Since the advent of highly active antiretroviral therapy (HAART), rates of the severe form-HAD-have declined dramatically in the developed world, from about 50 percent down to as low as 2 percent. University of Alberta's Dr. Chris Power, one of North America's leading neurologists, has estimated that about 7 percent of the more than 3,000 patients in the HIV clinics in Calgary and Edmonton have HAD.
Milder forms of NCI may be more common, and researchers in the United States are taking an in-depth look at this issue in the CHARTER (CNS HIV Antiretroviral Therapy Effects Research) study. Their results, released this past summer, indicate that the rate of NCI was 52 percent among 1,555 middle-aged HIV-positive volunteers-with 21 per-cent having mild impairment, 29 percent moderate and 2 percent severe.
Similar findings have been made by Dr. Sean B. Rourke, a neuropsychologist, scientist and the director of research in the Mental Health Service at St. Michael's Hospital in Toronto. Having done neuropsychological testing on more than 500 people with HIV/AIDS (PHAs), he found NCI preva-lence ranging from about one-quarter to one-third among people with HIV and up to 50 percent in people with AIDS, excluding those with conditions that can also cause NCI (such as depression or a history of traumatic brain injury). Dr. Rourke notes that his data are slightly biased because he sees patients who have been referred for cognitive problems.
There is not yet a general consensus on these data, but it is clear that NCI-especially its milder, subtler forms-may be touching a large proportion of PHAs.
What Causes NCI ?
HIV enters the brain early on in the course of infection. Although it doesn't infect brain nerve cells (neurons), HIV damages them both directly and indirectly. Proteins from HIV-infected cells cause the release of certain chemical messengers (neurotransmitters), which, in turn, cause inflammation, excitation and even cell death. In a less direct fash-ion, HIV infects other cells in the brain that cause a release of toxins that dam-age that organ.
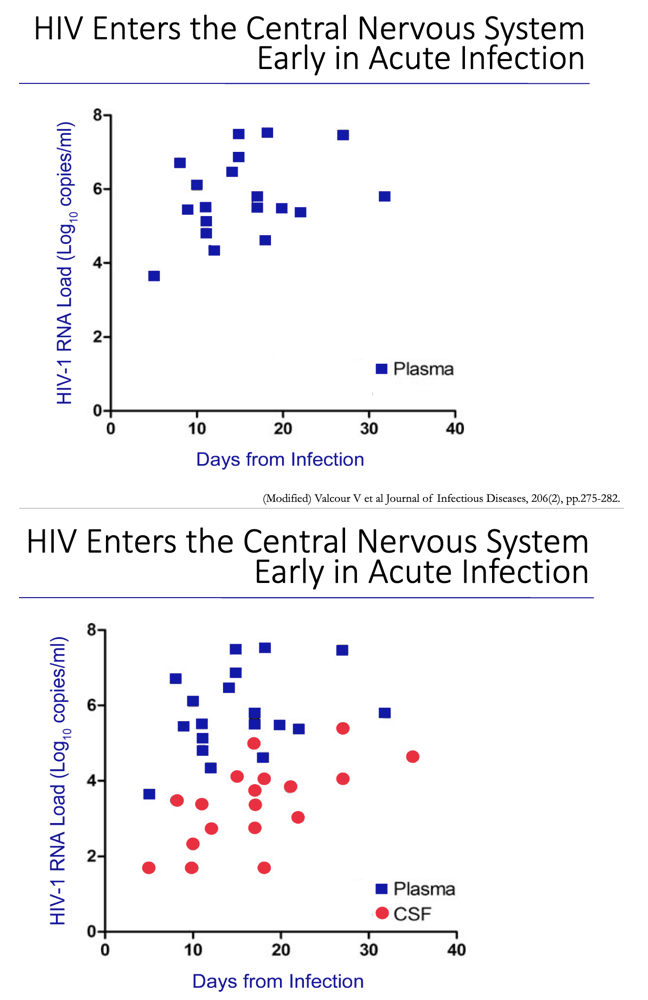
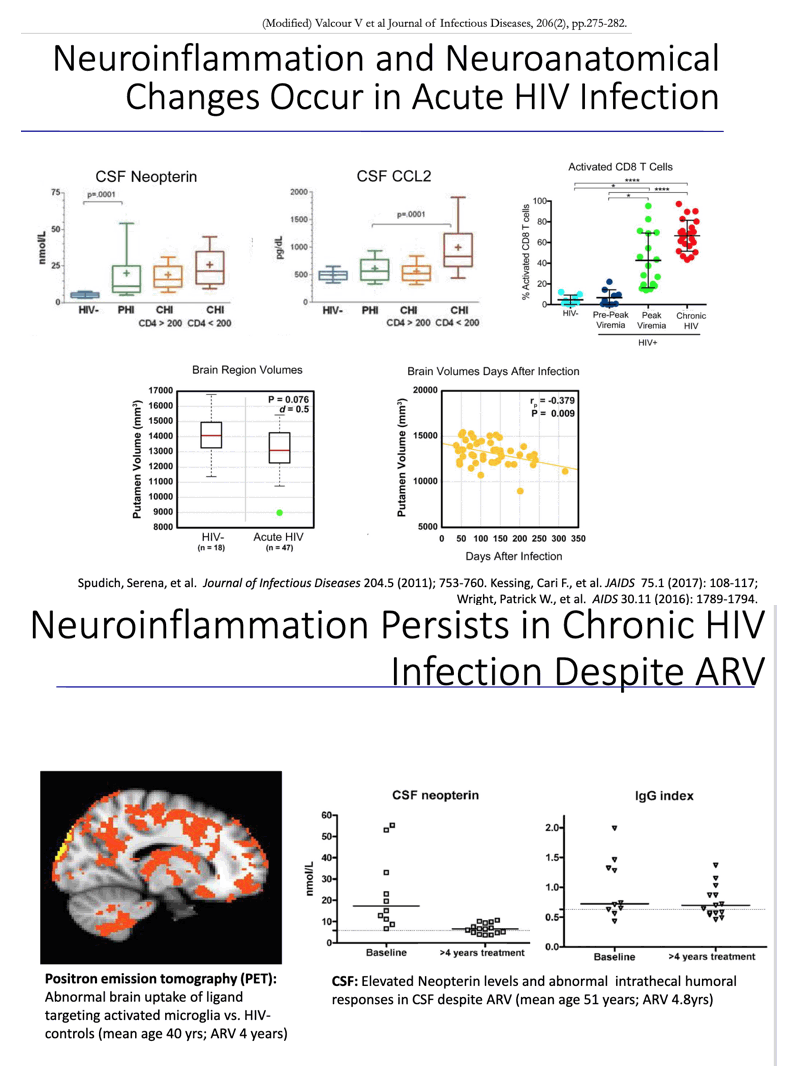

HAD is associated with advanced HIV disease, and although rates of HAD are declining, the milder forms of NCI are not necessarily follow-ing suit, says Dr. Ian Everall, a professor of psychiatry at the University of California, San Diego. He speculates that while HAD may be caused by the direct toxicity of HIV in the brain, milder forms of NCI are caused by secondary processes brought on by low-level presence of the virus: "HAD is a product of uncontrolled viral replication and immune sup-pression, so when we control replication with HAART, we get less HAD. But perhaps we are still living with low-grade infection and inflammation, which is subtly affecting the neurons and causing mild neurocognitive disorder."
Along with HIV and aging (see next section), there are many other factors that can cause or contribute to NCI, depending on their severity, including: depression, concus-sion, learning disabilities, alcohol or other substance-use disorders, non-HIV-related neurologic conditions (such as epilepsy and multiple sclerosis), systemic diseases (such as high blood pressure, diabetes, asthma and thyroid disease), hepatitis C virus and vitamin B1 and B12 deficiencies.
Aging & NCI
Aging affects the structure and function of the brain, slowing it down, making it less accurate and reducing its capacity to store and retrieve memories. Again, scientists have a range of terms for the severity of this decline, begin-ning with age-related cognitive decline, which is associated with normal aging. Mild cognitive impairment, evidenced by poorer memory and performance on neuropsychological testing, is seen in about 20 percent of those over 70. Thmost severe impairment is dementia, one common cause of which is Alzheimer's disease. This irreversible illness severely and progressively affects cognition, behavior and motor functions and day-to-day living. Most often found in people over 65, its incidence doubles about every five years from then. Approxi-mately 50 percent of HIV-negative people over 80 have Alzheimer's.
"It is a concern that with the aging of the HIV population we may be seeing additional effects of age [on NCI]," says Dr. Power. He hasn't seen much Alzheimer's in HIV-positive patients until they're in their 70s, but some studies have shown signs of Alzheimer's disease in the brains of PHAs much earlier. In a small substudy of brain samples from HIV-positive people over 55, Dr. Everall and his colleagues from the National NeuroAIDS Tissue Consortium found beta amyloid plaques, a characteristic of Alzheimer's disease, in 35 out of 36 brains.
For years, doctors and PHAs have suspected that HIV causes accelerated aging of the body. It wouldn't be sur-prising if the virus had this effect on the brain, too. In a recent small study, the blood flow in the brains of PHAs appeared similar to that of HIV-negative people who are 15 to 20 years older. Dr. Rourke says that with neuropsycho-logical testing "in those [HIV-positive people] with mild neu-rocognitive disorder, I am seeing an accelerated aging, like 10, 15 or even 20 years older.
Do you have HAND?
If you suspect that you have a problem with your cognition, the first step is to see your doctor. He or she may refer you to a specialist for further testing. Diagnosis of HAND involves neuropsychological testing that evaluates differ-ent parts of brain functioning. If you have signs of mild neurocognitive disorder, your doctor will take a full history and perform tests to determine the conditions that might be causing the impairment.
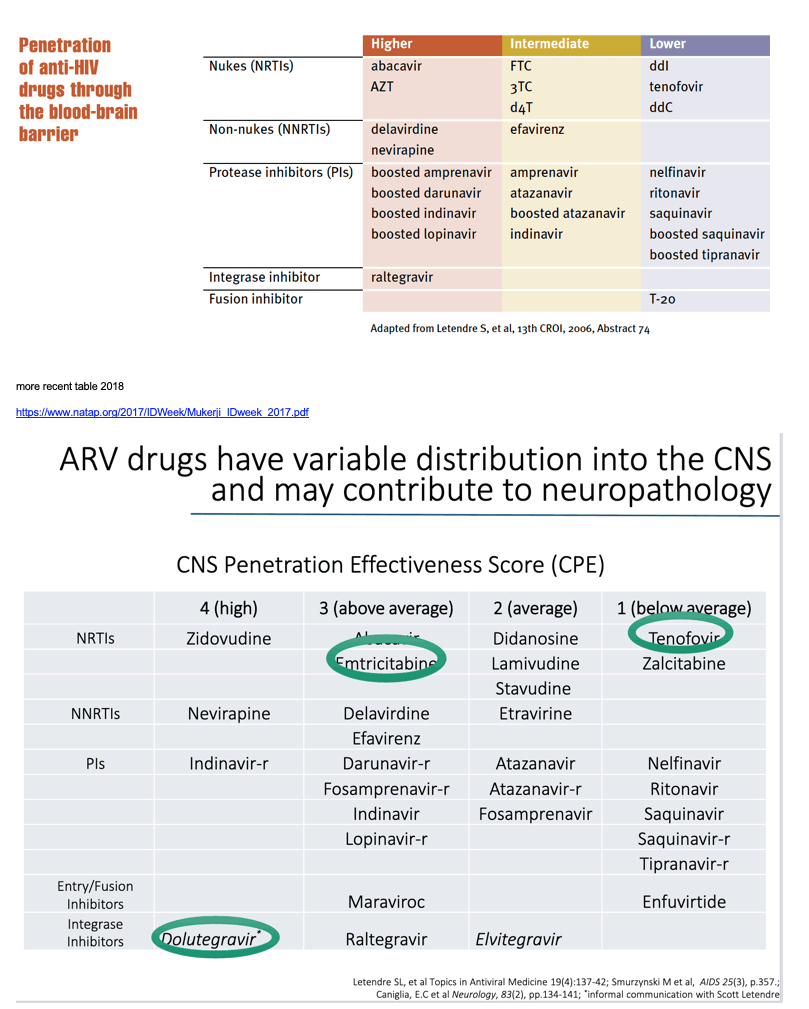
Of course now Dolutegravir and perhaps Bictegravir would be added but here is recent study:
High CNS Penetration Increased HIV Dementia
Its best to discuss with a neurologist & your doctor knowledgeable about these issues and when & If switching to a new ART regimen with better penetration is for you.
more recent table 2018
Fitness for the Brain
A couple of years ago, I saw Dr. Norman Doidge, Toronto psychiatrist and researcher, speak about his book, The Brain that Changes Itself. He explained how the brain is plastic and therefore can change based on what you do and think. He also mentioned the success of the Brain Fitness Program (BFP) in improving the memory of healthy seniors. I went online and read about the early impressive results of the IMPACT study (Improve-ments in Memory with Plasticity-based Adaptive Cogni-tive Training), a randomized, double-blinded prospective study of the Brain Fitness Program by researchers from the Mayo Clinic and the University of California, San Francisco. Among 524 HIV-negative seniors, those using the BFP had a 131 percent increase in brain processing speed. Their memory improved to that of individuals 10 years younger on average. Their neuropsychological test performance was significantly better than the active con-trols. And 75 percent of participants self-reported positive changes.
full pdf story attached
|
|
| |
| |
|
|
|