 |
 |
 |
| |
Sex work in the wake of SARSCoV2 in Zimbabwe: A qualitative study
|
| |
| |
Presented at the HIVR4P, Virtual, 27-28 January and 3-4 February 2021
Presenter
Fortunate Machingura
Authors
F. Machingura * (1), G. Jamali (1), M. Makamba (1), J. Busza (2), F.M Cowan (3)
Institutions
(1) Centre for Sexual Health and HIV/AIDS Research Zimbabwe (CeSHHAR Zimbabwe), Key Populations, Harare, Zimbabwe, (2) London School of Hygiene and Tropical Medicine, Centre for Evaluation, London, United Kingdom, (3) Liverpool School of Tropical Medicine, Department of International Public Health, Liverpool, United Kingdom
BACKGROUND: Female sex workers (FSW) in Zimbabwe have an HIV prevalence (58%) four times higher than women of reproductive age in the general population, making tailored prevention and treatment services critical. Recent SARSCoV2 lockdowns may have affected both sex work and FSW's risk behavior and engagement with HIV prevention and care. We aimed to investigate the impact of SARSCoV2 lockdowns on the dynamics of sex work in Zimbabwe.
METHODS: Between April 6 and July 21, 2020, we conducted 42 semi-structured telephone interviews with FSW from 24 sites across Zimbabwe's nationally scaled HIV prevention programme for FSW. We report evolving dynamics in sex work, access to HIV prevention services and perceptions of SARSCoV2 risk.
RESULTS: All the women reported decreases in demand for sex with reduced client numbers. Clients were reported to fear contracting SARSCoV2 and experience logistic difficulties meeting with FSW due to travel and socialising restrictions. Closure of the informal economic sector reportedly reduced clients' income and therefore capacity to pay for sex. Where sexual exchange happened, clients preferred rear-entry sex positions and refused kissing or oral sex to minimise contact perceived to increase chances of contracting SARSCoV2. Costs per sex act plummeted from an average of US$5 to US$1 per 'short time'. 'I go as low as US$0.50c, clients are fewer...' FSWs reported willingness to have sex on credit, condomless (anal) sex, or exchanging sex for food to alleviate financial and food insecurity. Women fear hunger, inability to pay rent and returning to rural homes to face stigma and ostracization more than SARSCoV2. 'I would rather die of COVID than see my children go to bed hungry...' FSWs who rely on mobile clinics (unable to operate during the first phase of lockdown) struggled to access HIV tests, PrEP refills, STI treatment, and family planning needs.
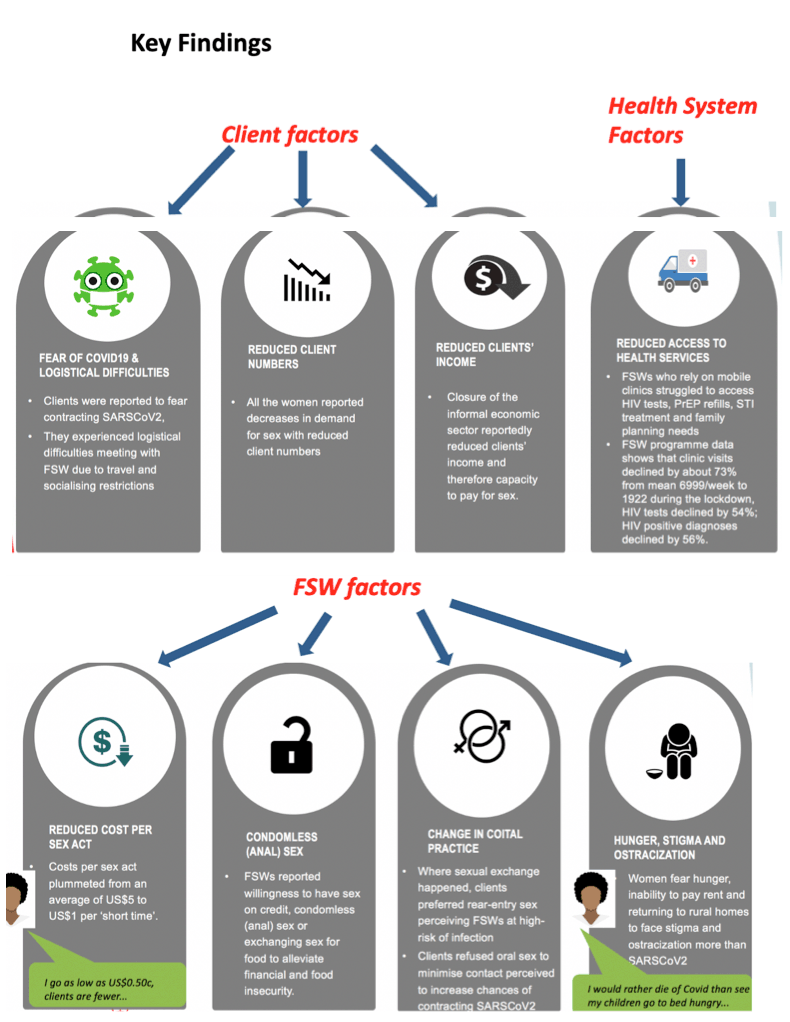
CONCLUSIONS: Reduced demand for and cost of commercial sex compounded existing income and food insecurity, making already vulnerable FSWs increasingly desperate and therefore willing to take greater risks with clients, including contracting SARSCoV2, HIV, and STIs. FSWs who live in precarious conditions, with little social protection, face difficult choices that potentially undermine HIV prevention investments.
|
| |
|
 |
 |
|
|