 |
 |
 |
| |
HIV Immune Response to COVID – 2 studies: 1- Robust SARS-CoV-2-specific serological and functional t-cell immunity in PLWHIV, 2 - SARS-Cov-2 immunity in COVID-19 convalescent individuals living with HIV: bulk immune profiling and SARS-CoV-2 specific humoral and cellular immune responses
|
| |
| |
Robust SARS-CoV-2-specific serological and functional t-cell immunity in PLWHIV
IAS 2012 July 18-22
Presenter: Juan Tiraboschi
Authors: L. Donadeu (1,2}, J. Tiraboschi • (3,2}, A Fava (1,2), S. Scevola (3,2), D. Podzamczer (3,2), 0. Bestard (1,2}
Institutions: (1) Bellvitge University Hospital, Translational Nephrology and Transplantation Laboratory, L"Hospitalet de Llobregat, Spain, (2) IDIBELL, L"Hospitalet de Llobregat, Spain, (3) Bellvitge University Hospital, HIV Unit, Infectious Disease Service, L"Hospitalet de Llobregat, Spain
Abstract:
BACKGROUND: While description of protective humoral and T-cell immune responses has been reported among immunocompetent (IC) individuals, its characterization among PLWHIV remains uncertain.
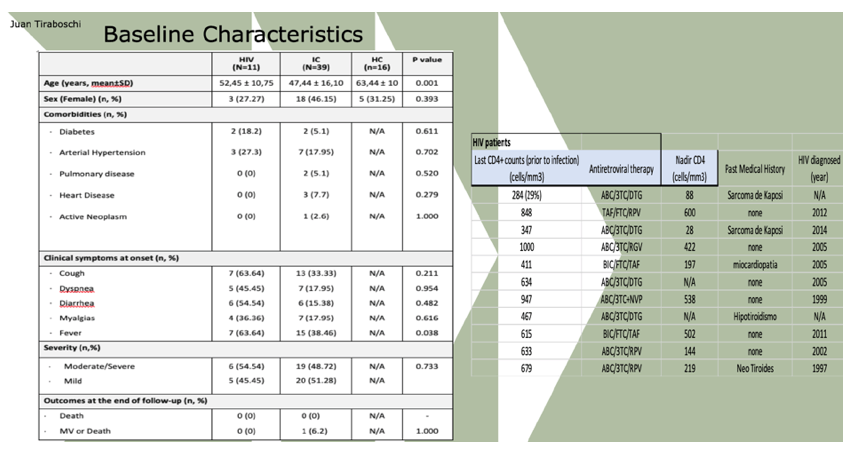
METHODS: SARS-CoV-2-specific serological and functional T-cell immune responses against main immunogenic antigens were assessed in 11 HIV-positive patients at three (T1) and six months (T2) following confirmed-SARS-CoV-2-infection, and compared to a cohort of 34 immunocompetent (IC) individuals developing mild (outpatient, n=21) and severe (inpatient, n=13) disease. Also, SARS-CoV-2 (Spike)-specific memory B cells responses were investigated A healthy non-infected group of 16 patients whose PBMC (peripheral blood mononuclear cells) had been bio-banked before COVID-19 pandemic (2018) were also analyzed.
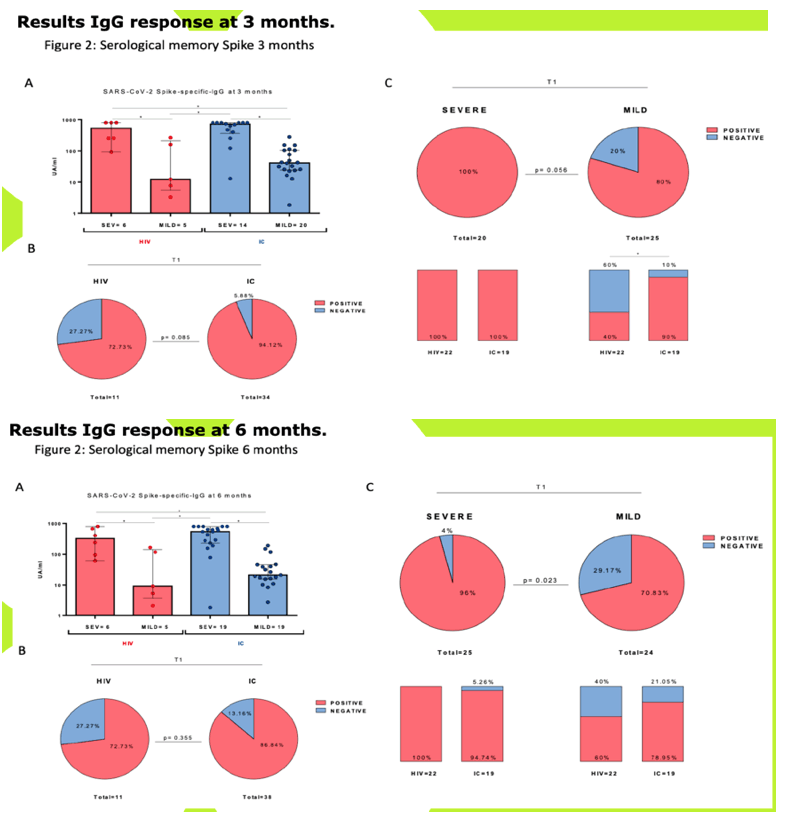
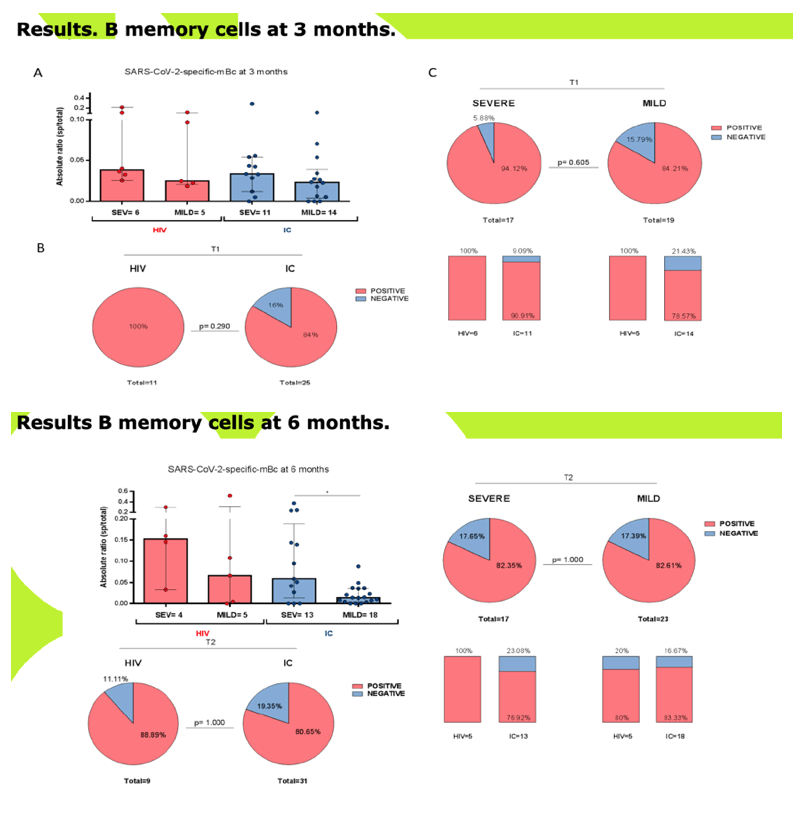
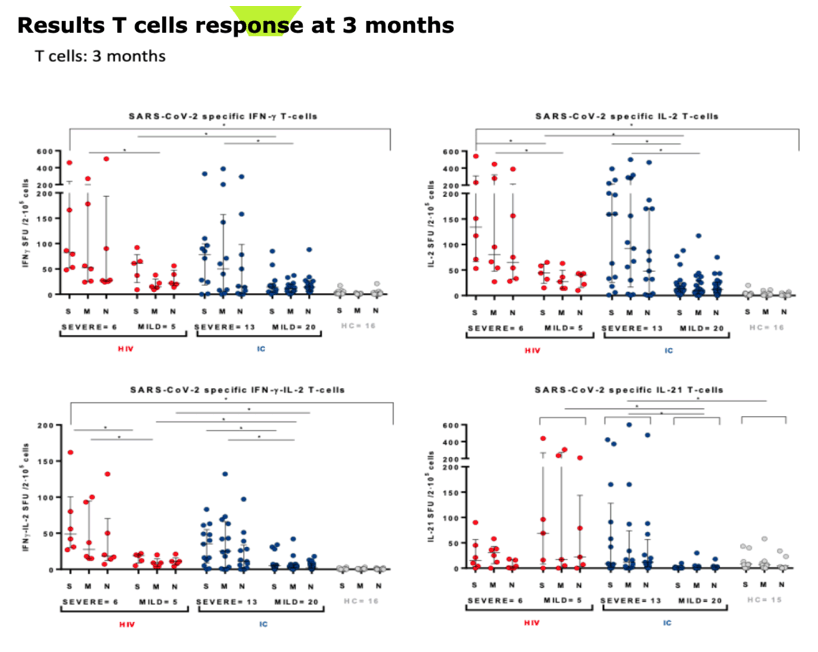
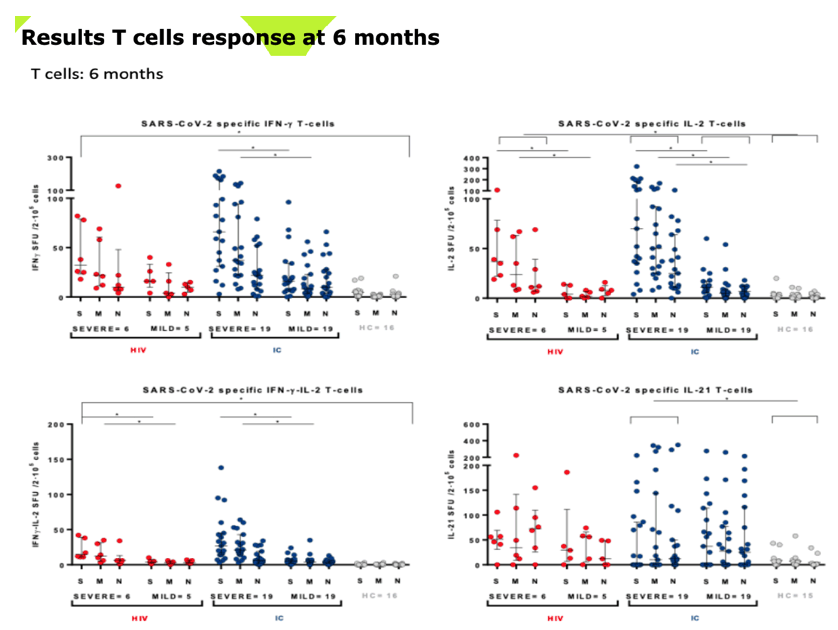
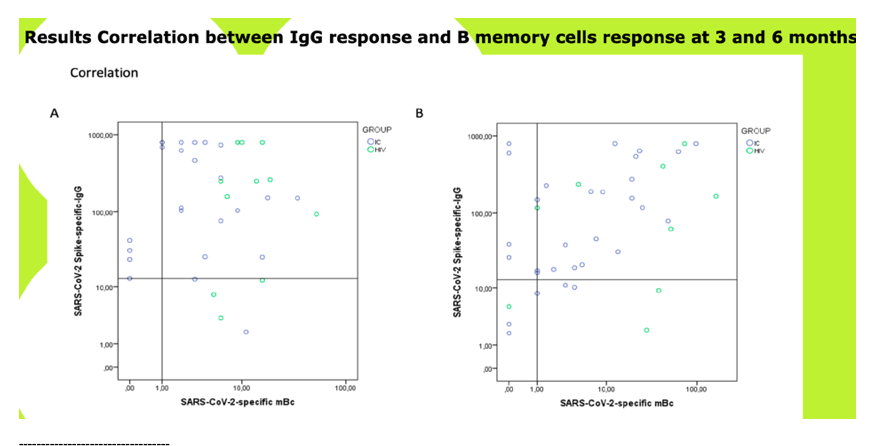
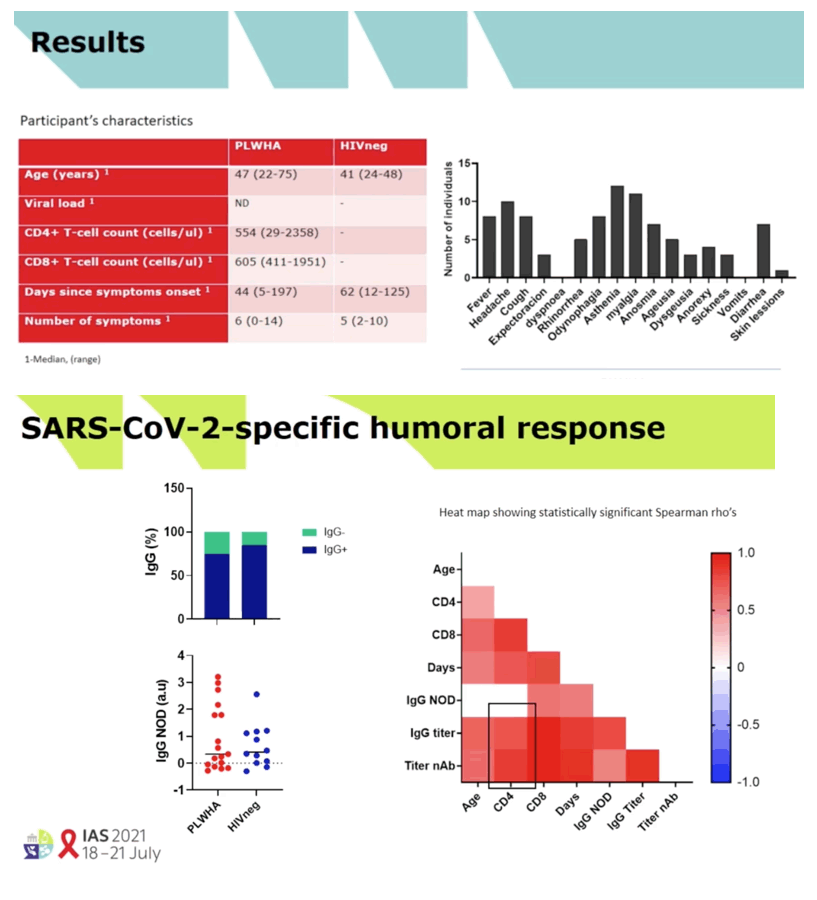
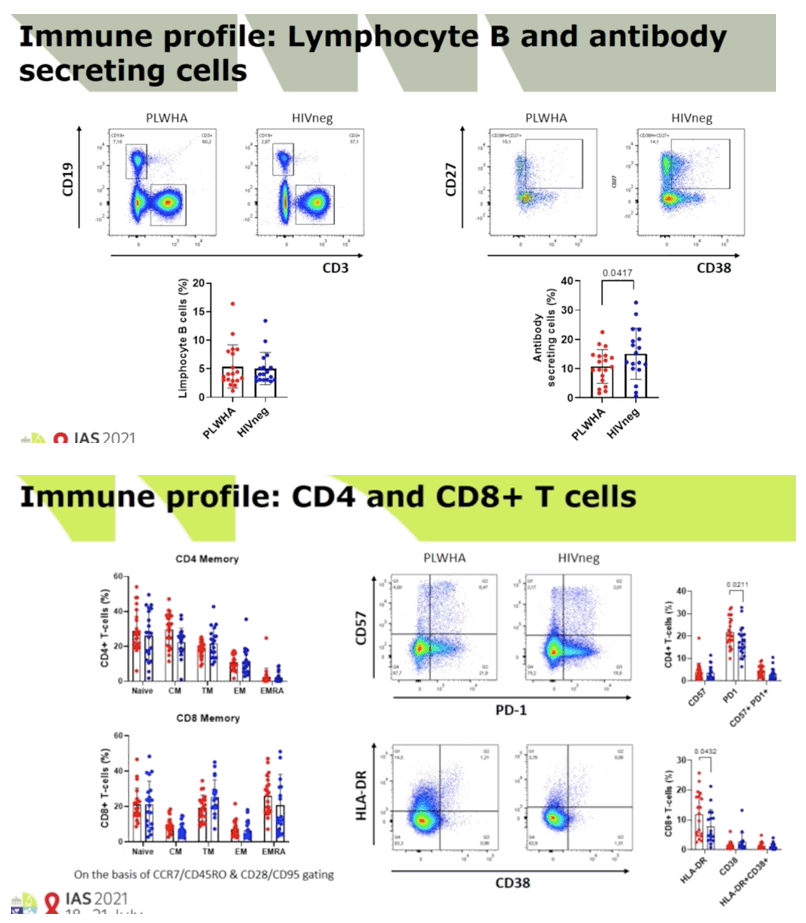
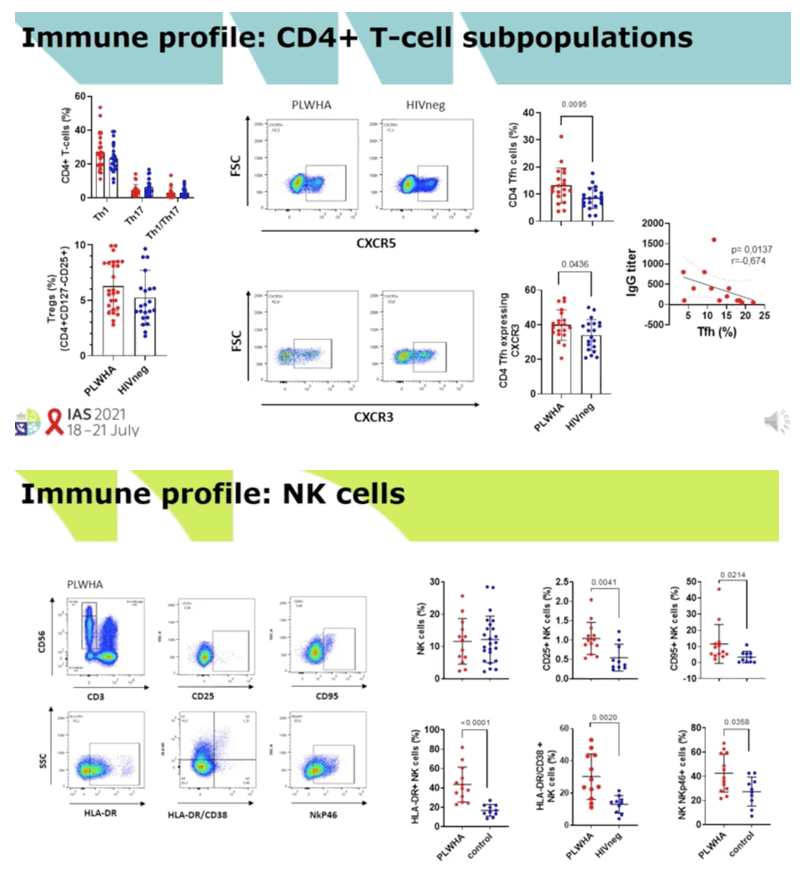
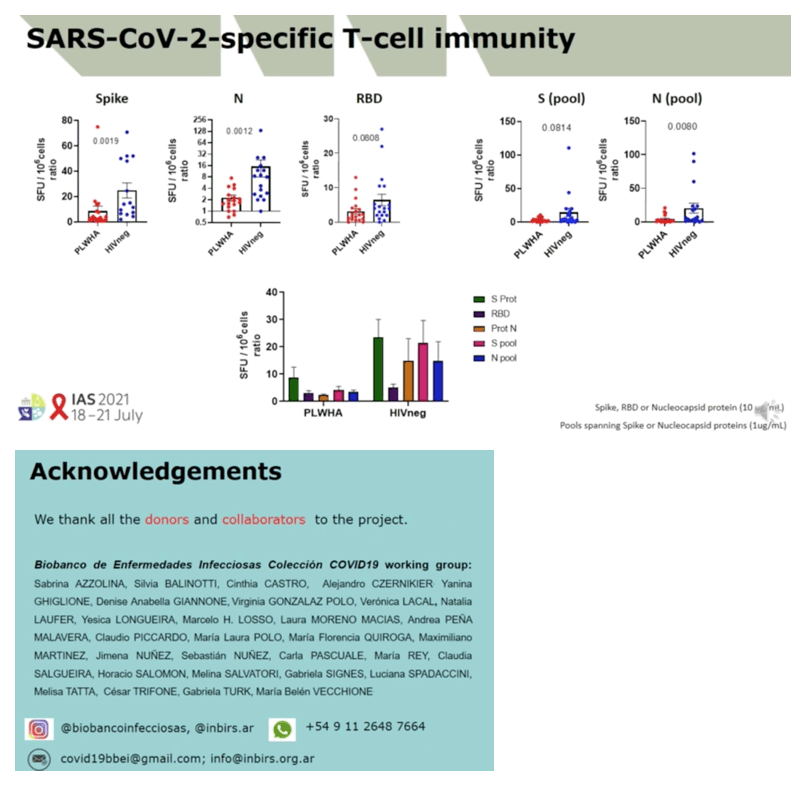
RESULTS: Median (range) age was 51 (33-67); nadir and current T-CD4 cell count was 219 cells/ml (28-600) and 633 cells/ml (284-1000) respectively. Only 5/11 patients needed hospital admission and one of them required ICU. Patients displayed similar IFN-i3, IL2 and polyfunctional IFN-f3/IL2 producing T-cell frequencies than IC with mild symptoms at three and six months after infection. IC patients with more severe COVID-19 infection exhibited the highest T-cell immune responses (Figure 1). However, all (14/14) severe, 7/11 (63%) HIV and 3/18 (16.7%} mild IC patients showed lgG seropositivity at 6 months (p<0.005} (Figure 2). Interestingly, a broad range of SARS-CoV-2 (Spike)-specific memory 8-cell responses in the majority of HIV patients, despite the absence of SARS-CoV-2-specific lgG antibodies at three (4/4) and six (2/4) months (Figure 3).
CONCLUSIONS: Our data suggest a comparable natural immunization among chronic HIV, similar to that of IC convalescent patients developing similar COVID-19 disease severity. Notably, functional B and T-cell assessment may more reliably detect immunized patients with robust immune memory responses as compared to serological memory assessment during mid-term convalescence.




|
| |
|
 |
 |
|
|