 |
 |
 |
| |
Unsuppressed plasma HIV-RNA is associated with
worse COVID-19 outcomes among people living with HIV.
|
| |
| |
IAS 2021 July 18-22
Authors: Daniel Kwakye Nomah, MD1,2,, Juliana Reyes-Urueña, MD, PhD1,3,4,, Yesika Diaz, MSc1,4, Sergio Moreno, MSc1,4, Jordi Aceiton, BSc1,4, Andreu Bruguera, MD1,3,4, Rosa M. Vivanco-Hidalgo, MD, PhD5, Josep M. Llibre, MD, PhD6, Pere Domingo, MD, PhD7, Vicenç Falco, MD, PhD8, Arkaitz Imaz, MD, PhD9, Cristina Cortés, MD, PhD10, Lluis Force, MD, PhD11, Emili Letang, MD, PhD12,13, Ingrid Vilaro, MD14, Jordi Casabona, MD, PhD1,2,3,4, Jose M. Miro, MD, PhD15 and the PISCIS cohort group.
1. Centre Estudis Epidemiològics sobre les Infeccions de Transmissio Sexual i Sida de Catalunya (CEEISCAT), Dept Salut, Generalitat de Catalunya, Badalona, Spain
2. Departament de Pediatria, d'Obstetricia i Ginecologia i de Medicina Preventiva i de Salut Publica, Universitat Autònoma de Barcelona, Bellaterra, Spain
3. CIBER Epidemiologia y Salud Pública (CIBERESP), Barcelona, Spain
4. Institut d'Investigacio Germans Trias i Pujol (IGTP), Barcelona, Spain
5. Agencia de Qualitat i Avaluacio Sanitàries de Catalunya
6. Hospital Universitari Germans Trias i Pujol, Badalona, Spain
7. Hospital de la Santa Creu i Sant Pau, Barcelona, Spain.
8. Vall d'Hebron Research Institute (VHIR), Hospital de Vall d'Hebron, Barcelona, Spain.
9. HIV and STI Unit. Department of Infectious Diseases, Hospital Universitari de
Bellvitge-(IDIBELL), L'Hospitalet de Llobregat, Spain.
10. Hospital Moises Broggi-Consorci Sanitari Integral, L'Hospitalet de Llobregat, Spain
11. Hospital de Mataro, Mataro, Spain
12. Hospital del Mar, Barcelona, Spain.
13. ISGlobal, Barcelona Institute for Global Health, Hospital Clinic-University of Barcelona, Barcelona, Spain
14. Hospital de Vic, Vic, Spain
15. Hospital Clinic-Institut d'Investigacions Biomediques August Pi i Sunyer, University of Barcelona, Barcelona, Spain
ABSTRACT
Background
Information about the relationship between HIV-associated immune suppression and COVID-19 outcomes is scarce. We characterized the sociodemographic and clinical features, and impact of immunosuppression on COVID-19-related outcomes among persons living with HIV (PLWH).
Methods
PISCIS is a population-based cohort of PLWH aged ≥16 years in care at 16 Catalan hospitals, which collects sociodemographic and clinical data between 01/01/1998 and 15/12/2020. We linked PISCIS data with the Public Data Analysis for Health Research and Innovation Program of Catalonia (PADRIS) to obtain COVID-19 diagnosis related data and other comorbidities. Only patients with microbiologically confirmed SARS-CoV-2 infection (NAAT, antigen detection or antibodies) were included in the analysis. Factors associated with COVID-19 diagnosis and severe outcomes were assessed using multivariate Cox regression models. We estimated the impact of immunosuppression on severe outcomes (hospital admission or death) using survival analysis.
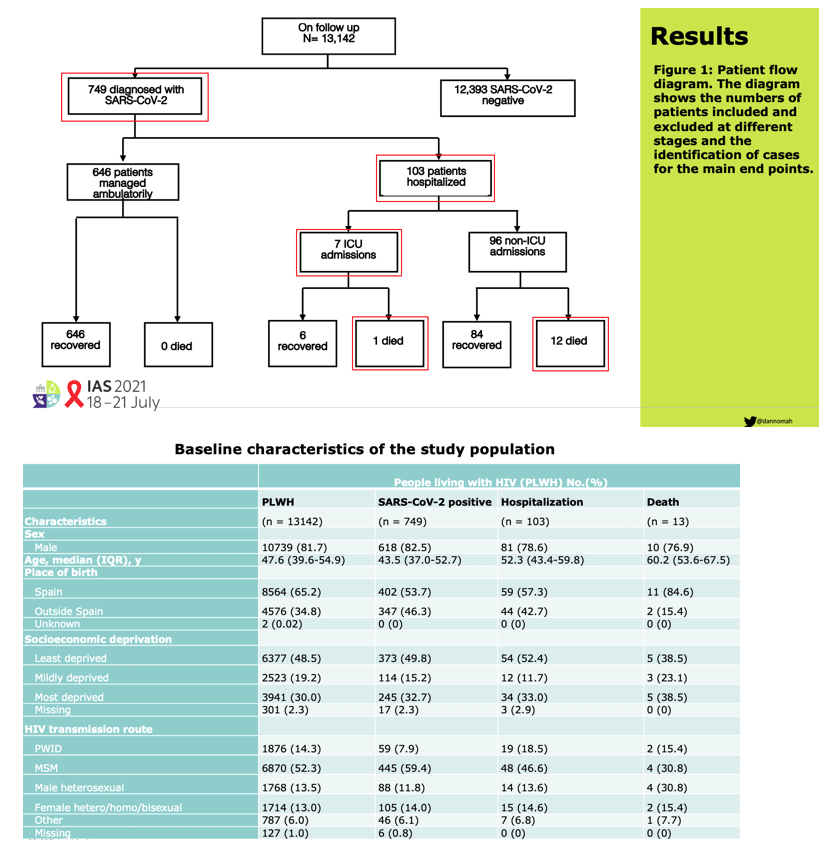
Results
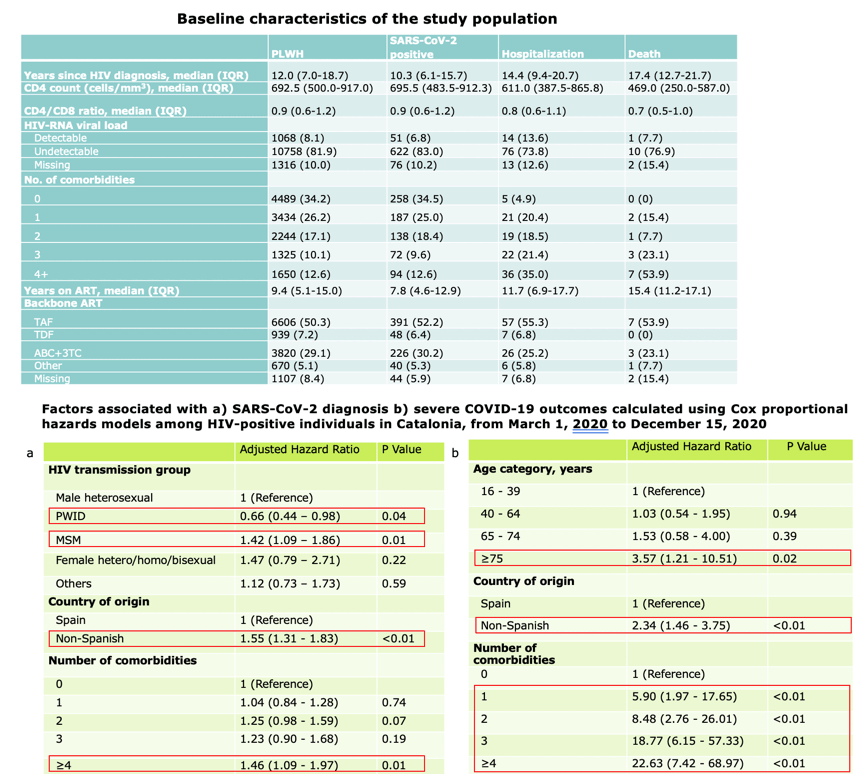
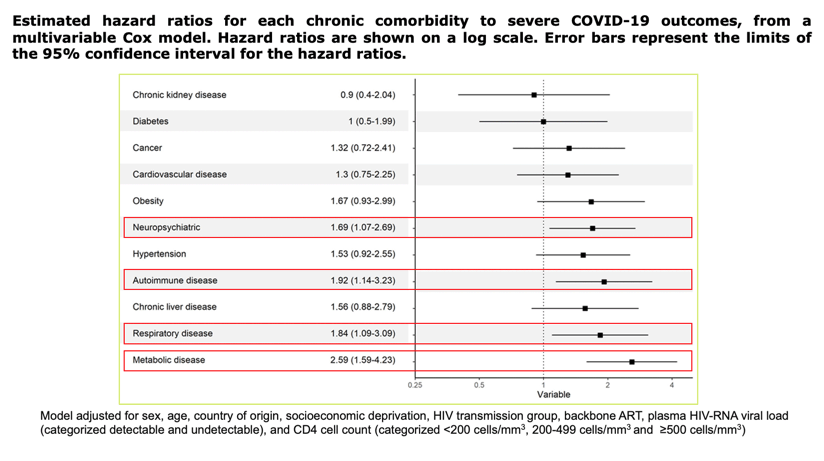
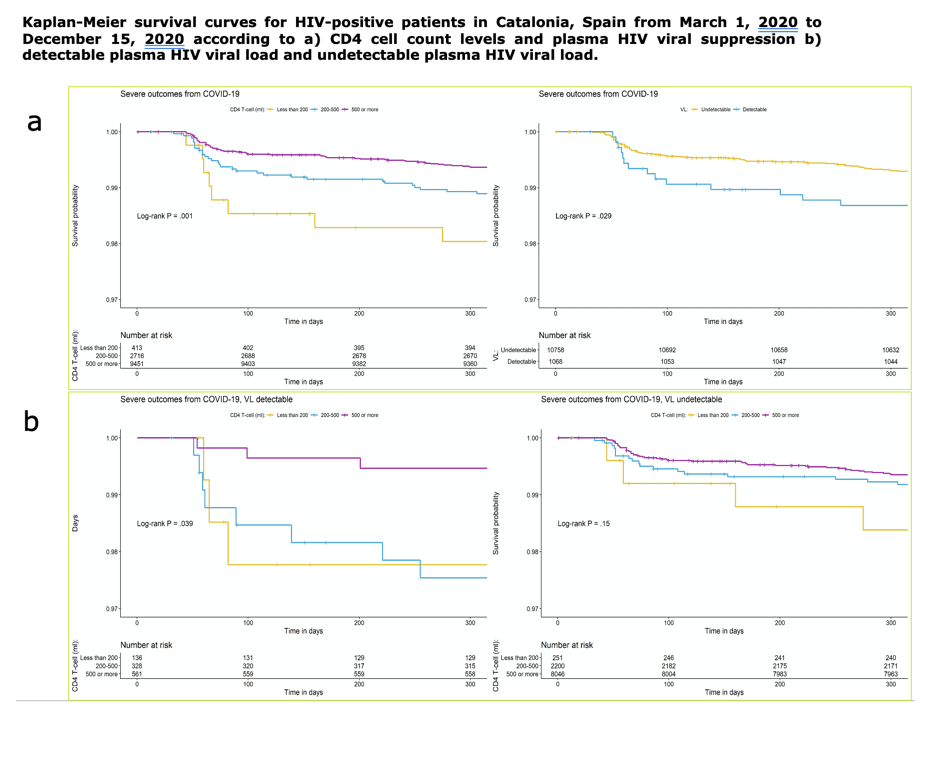
Of 13,142 PLWH on follow-up, 749 (5.7%) were diagnosed with SARS-CoV-2. Among them, 618/749 (82.5%) were males and the median age was 43.5 years ([IQR] 37.0-52.7). 103 (13.8%) were hospitalized, 7 (0.9%) were admitted to the ICU and 13 (1.7%) died. SARS-CoV-2 diagnosis was more common among migrants (aHR, 1.55 [95% CI, 1.31-1.83]), MSM (aHR, 1.42 [95% CI, 1.09-1.86]) and those with ≥4 comorbidities (aHR, 1.46 [95% CI, 1.09-1.97]). Age ≥75 years (aHR, 5.2 [95%CI:1.8-15.3]), non-Spanish origin (aHR, 2.1 [95%CI:1.3-3.4]) and chronic comorbidities (neuropsychiatric aHR, 1.69 [95% CI, 1.07-2.69], autoimmune disease aHR, 1.92 [95% CI, 1.14-3.23] respiratory disease aHR, 1.84 [95% CI, 1.09-3.09] and metabolic disease aHR, 2.59 [95% CI, 1.59-4.23]) were associated with higher risk of severe outcomes. A Kaplan-Meier estimator showed differences in the risk of severe outcomes according to CD4 levels in patients with detectable HIV viral load (P<0.039) but no differences were observed in patients with undetectable HIV viral load (P=0.15)
Conclusion
SARS-CoV-2 diagnosis in PLWH was more common among migrants, those with ≥4 comorbidities and MSM. Among co-infected patients, those with detectable HIV viral load, older age, chronic comorbidities and migrants had higher risks of severe outcomes. Of note, lower CD4 cell counts was a risk factor to severe COVID-19 only among patients with detectable viral load in stratified analysis.



|
| |
|
 |
 |
|
|