 |
 |
 |
| |
Metabolic Comorbidities Tied to Shorter HCC-Free Survival With HBV
|
| |
| |
AASLD-The Liver Meeting, November 4-8, 2022, Washington, DC
Mark Mascolini
Each of four metabolic comorbidities was linked to shorter hepatocellular carcinoma (HCC)-free survival in a retrospective study of people with HBV infection in the Netherlands [1]. While having a single metabolic comorbidity was associated with almost a 3-fold risk of shorter HCC-free survival in an adjusted analysis, having 2 or more metabolic comorbidities meant almost a 6-fold higher risk of shorter survival.
Researchers from Rotterdam's Erasmus University Medical Center reminded AASLD attendees that chronic HBV infection boosts risk of HCC and liver-related death. Metabolic comorbidities-in this study overweight, diabetes, hypertension, and abnormal lipids-may spur progression of fibrosis and HCC development.
The Erasmus team conducted this study to explore associations between these four comorbidities and HCC or death in people with chronic HBV monoinfection. This retrospective single-center study used chart review to gather relevant demographic and clinical details of people with chronic HBV infection. The primary endpoint was HCC-free survival, defined as time until HCC diagnosis, liver transplant, or death.
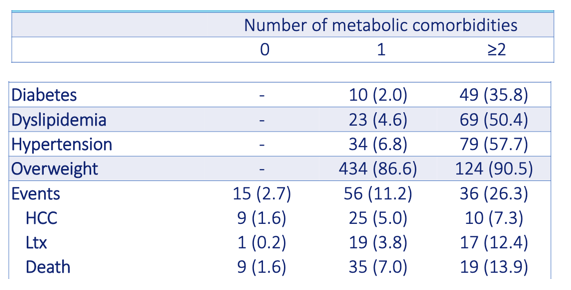
Among 1194 people with chronic HBV, 638 (53%) had at least one metabolic comorbidity-overweight in 46.7%, hypertension in 9.5%, abnormal lipids in 7.7%, and diabetes in 4.9%. While 501 people had 1 comorbidity, 137 had 2 or more. Median ages in the groups with 0, 1, and 2 or more comorbidities were 31, 36, and 46, so this was a young study group. The proportion of men rose across the three comorbidity groups-from 50.5% with 0 comorbidities, to 65.5% with 1, to 70.8% with 2 or more. Across those three groups, proportions of whites and Asians were 43.7% and 36.8%, 51.4% and 26.9%, and 60.5% and 24.0%.
Through a median follow-up of 6.6 years, researchers counted 107 first events (44 HCCs, 38 liver transplants, and 25 deaths). Proportions of people with an endpoint event were 2.7% in people with 0 comorbidities, 11.2% in people with 1 comorbidity, and 26.3% in people with 2 or more comorbidities.
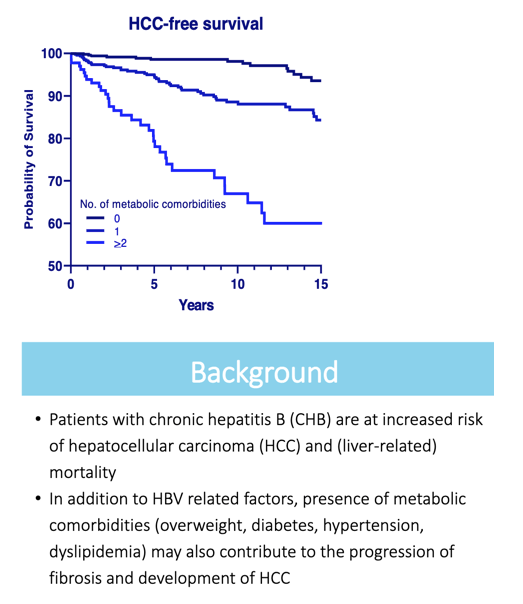
Each comorbidity was significantly associated with lower HCC-free survival: overweight hazard ratio (HR) 1.6 (P = 0.013), abnormal lipids HR 3.7 (P < 0.001), diabetes HR 6.7 (P < 0.001), and hypertension HR 9.98 (P < 0.001). Having more comorbidities heightened the risk of reaching an endpoint: for 1 comorbidity HR 3.8, while for 2 or more comorbidities HR 12.7 (P < 0.001).
When the researchers used multivariable Cox regression to adjust these calculations by HCC risk score (age-male-ALBI-platelet or aMAP score), more comorbidities remained independently associated with reaching an endpoint: for 1 comorbidity adjusted HR 2.7, while for 2 or more comorbidities, adjusted HR 5.8 (P < 0.001). When the Erasmus team divided participants into low, intermediate, and high HCC risk groups by aMAP score (75.7%, 17.3%, and 7% of the cohort), hazard ratios for 1 and 2 or more comorbidities were 3.0 and 9.4 for the low-risk group (P = 0.001), 2.1 and 6.3 for the intermediate-risk group (P < 0.001), and 2.3 and 3.8 for the high-risk group (P = 0.04).
The Erasmus investigators concluded that individual metabolic comorbidities are associated with shortened HCC-free survival in people with chronic HBV infection-and 2 or more comorbidities are tied to shorter disease-free survival than a single comorbidity.
Reference
1. Patmore L, Katwaroe WK, Van Der Spek D, et al. Presence of metabolic comorbidities is associated with reduced HCC-free survival in patients with chronic hepatitis B. AASLD-Th


|
| |
|
 |
 |
|
|