 |
 |
 |
| |
Oral TDF/FTC Provides Early Mucosal Protection In Both On- Demand And Daily Regimen
|
| |
| |
CROI 2022 Feb 11-16
Sylvain Chawki1, Audrey Gabassi1, Mayssam El Mouhebb2, Milad Taouk1, Lambert Assoumou2, Iris Bichard1, Skander Benothmane1, Ali Amara3, Rhonda Brand4, Aaron Siegel4, Lauriane Goldwirt1, Ian McGowan5, Dominique Costagliola2, Jean-Michel Molina1, Constance Delaugerre1 for the ANRS-PREVENIR Research Group
1Hôpital Saint-Louis, Paris, France, 2Institut Pierre Louis d'Epidémiologie et de Santé Publique, Paris, France, 3Institut National de la Santé et de la Recherche Médicale, Paris, France, 4University of Pittsburgh, Pittsburgh, PA, United States, 5Orion Biotechnology, Ottawa, Canada

Program abstract
Background: Oral pre-exposure prophylaxis (PrEP) with TDF/FTC is efficacious in preventing HIV acquisition in MSM, both with ON-DEMAND and the DAILY regimens. Whether a PrEP effect occurs at the mucosal level after the recommended pre-exposure dose remains uncertain. We aimed to study TDF/FTC PrEP mucosal efficacy against HIV in an ex vivo rectal tissue model with either PrEP dosing regimen.
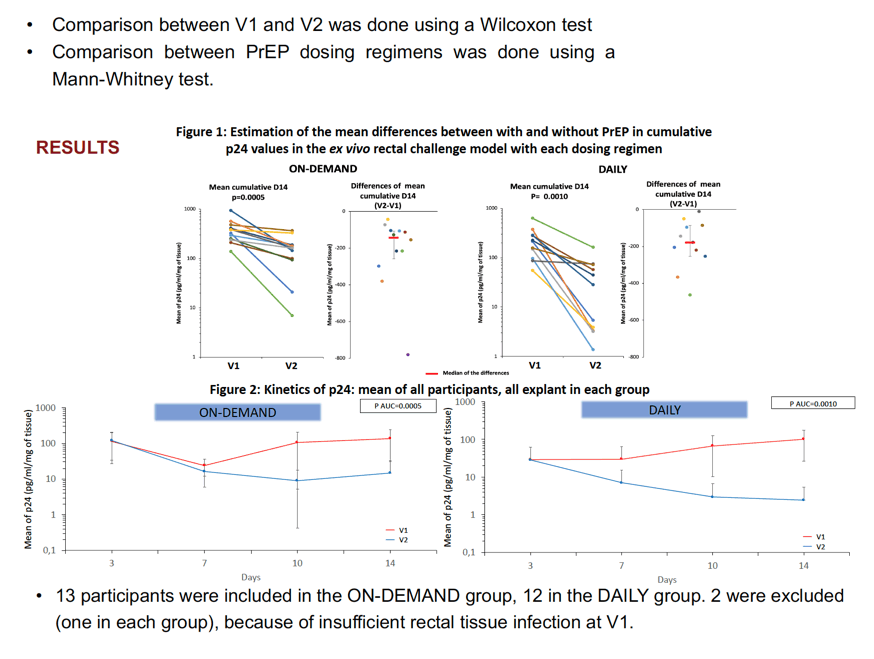
Methods: We designed a substudy of the ANRS-PREVENIR study (NCT 03113123) of participants taking either ON-DEMAND or DAILY PrEP. We used an ex vivo infection challenge model to evaluate rectal tissue susceptibility to HIV infection before and after PrEP exposure, where each participant was his own control, thus estimating the level of protection provided by TDF/FTC. Rectal explants were collected at baseline and 2 hours after a double dose of TDF/FTC or 7 days after one pill a day in the ON-DEMAND and DAILY arms, respectively. HIV infectability was evaluated by measuring rectal explant supernatant p24 secretion over 14 days of culture. Levels of p24 were standardized by the weight of each explant (ng/ml/mg of tissue). Mean D14 cumulative p24 level differences (After-Before PrEP) reflect overall infectability of explants in each patient. Comparison between before and after PrEP was done using a paired-Wilcoxon test. Comparison between PrEP dosing regimens was done using a Mann-Whitney test.
Results: We included 13 individuals in the ON-DEMAND group and 12 in the DAILY group. All participants were self-identifying MSM and gave written consent. We excluded 2 individuals (one in each group) for insufficient infection of rectal tissue before PrEP. The median of mean D14 cumulative p24 difference after-before PrEP was -144ng/ml/mg (IQR[-259;-108]) for the ON-DEMAND group (P=.0005, n=12) (Figure). The median of mean D14 cumulative p24 difference after-before PrEP was -179ng/ml/mg (IQR[-253;-86]) for the DAILY group (P=.001, n=11) (Figure). There was no statistical difference in the median cumulative p24 differences between the groups, for a sample of 23 participants analyzed (P=0.93).
Conclusion: ON-DEMAND and DAILY PrEP with TDF/FTC both showed efficacy to reduce HIV infection, as soon as 2 hours for the ON-DEMAND arm, in rectal tissue. PrEP efficacy in rectal tissue might be a good marker of clinical efficacy that needs to be evaluated for future PrEP agents or dosing strategy candidates.





|
| |
|
 |
 |
|
|