 |
 |
 |
| |
COVID-19 BOOSTER VACCINE EFFECTIVENESS IN PEOPLE WITH AND
WITHOUT IMMUNE DYSFUNCTION – in reducing breakthrough, duration of benefit
|
| |
| |
CROI 2022 Feb 11-16
Jing Sun, MD, PhD
Johns Hopkins Bloomberg School of Public Health, Baltimore, MD, USA

2022 CROI, February 12-16 and 22-24, 2022
Mark Mascolini
A booster dose of a SARS-CoV-2 vaccine cut risk of breakthrough infection and chopped odds of hospital admission, invasive ventilation, or death in a 788,792-person analysis of the US National COVID Cohort Collaborative (N3C) [1]. Booster protection against breakthrough infection proved lower but still significant in people with immune dysfunction.
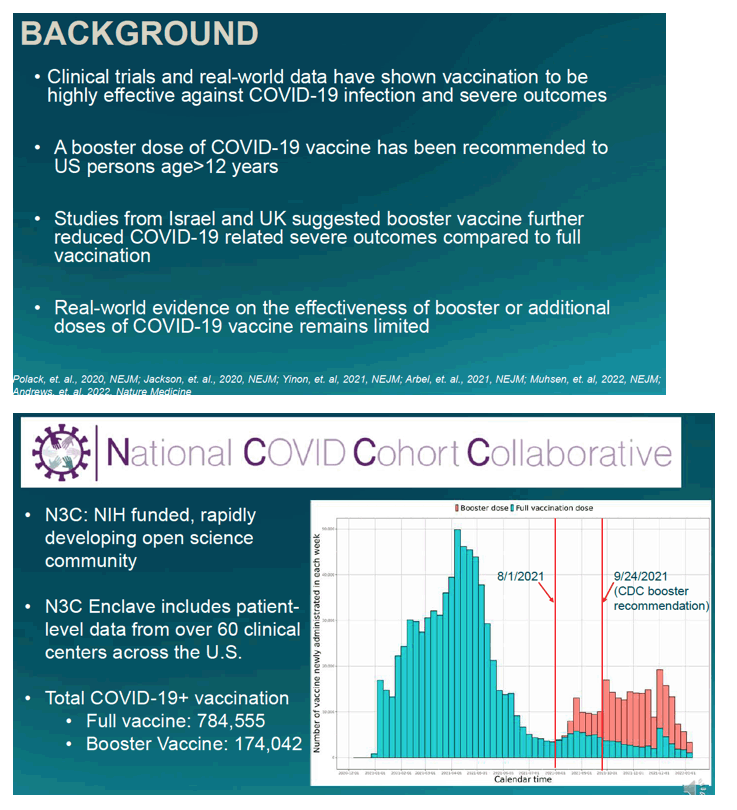
N3C investigators noted that studies in Israel and the UK found evidence that booster vaccination made severe COVID-19 outcomes less frequent than full vaccination without a booster. But until this analysis real-world data on booster impact remained scanty. The National Institutes of Health-funded N3C collects COVID-19 data from more than 60 clinical centers across the United States.
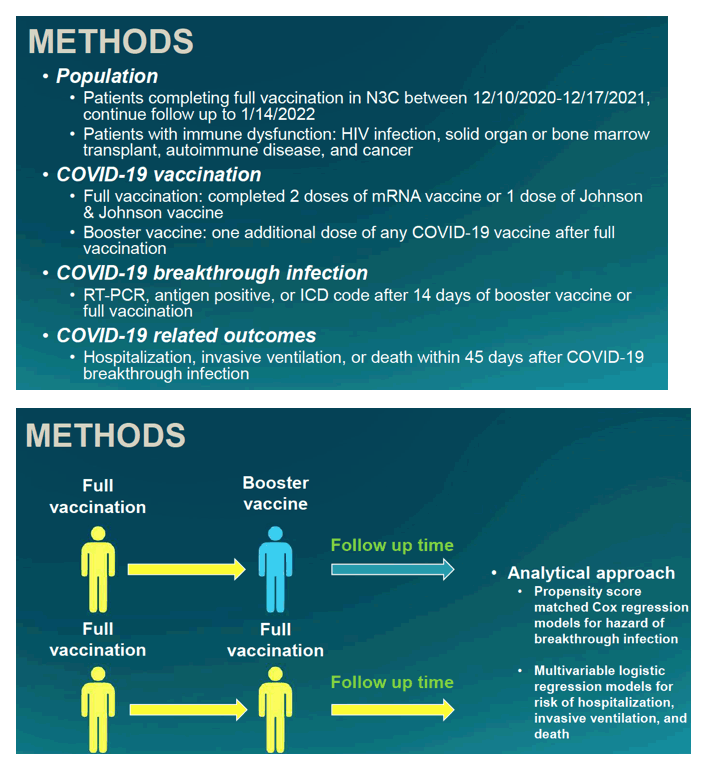
This analysis included people fully vaccinated between December 10, 2020 and December 17, 2021 who continued follow-up through January 14, 2022. Researchers considered people with immune dysfunction those with HIV infection, solid organ or bone marrow transplant, an autoimmune disease, or cancer. Full vaccination meant two doses of an mRNA vaccine (Pfizer or Moderna) or one dose of the Johnson & Johnson vaccine. The investigators defined breakthrough infection as a positive RT-PCR, antigen positivity, or a COVID-19 ICD code more than 14 days after full vaccination or a booster. Outcomes were COVID-related hospital admission, invasive ventilation, or death within 45 days of COVID-19 breakthrough infection.
To gauge the effect of a booster shot on breakthrough infection, the N3C team used propensity score-matched Cox regression models comparing fully dosed people with a booster to fully dosed people without a booster. They used multivariate logistic regression to assess boosting’s impact on hospital admission, invasive ventilation, and death.
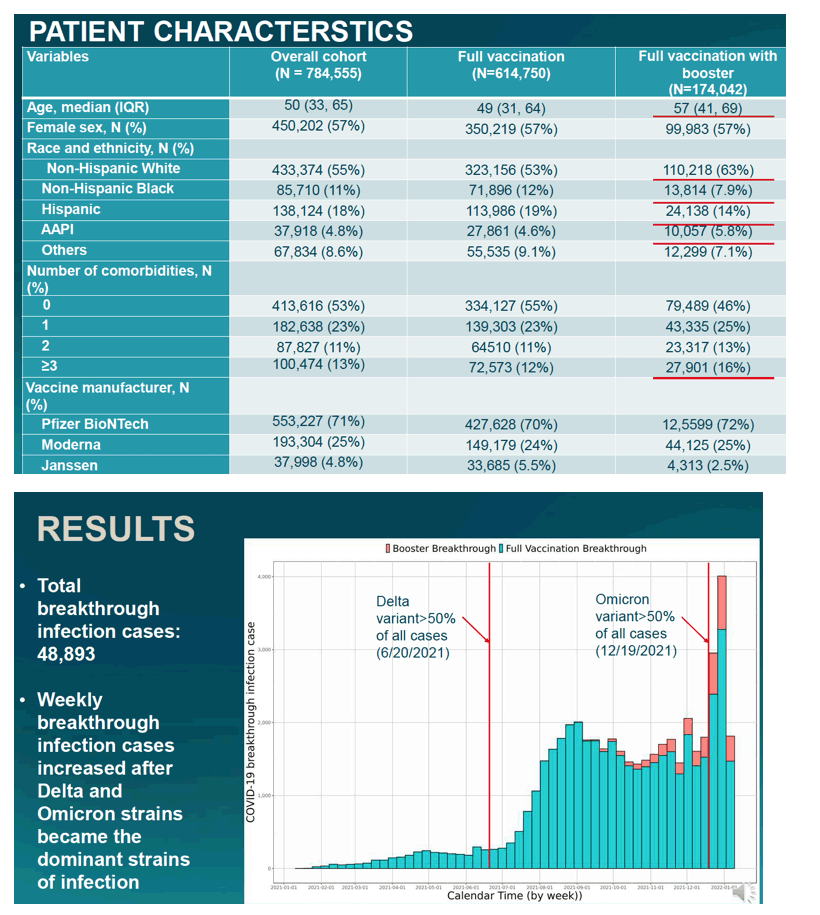
The overall cohort included 614,750 with full vaccination without a booster and 174,042 with full vaccination plus a booster. The booster group was older than the full-vax group (median 57 vs 49) and included a higher proportion of whites (63% vs 53%), a lower proportion of blacks (7.9% vs 12%), a lower proportion of Hispanics (14% vs 19%), a higher proportion of Asians and Pacific Islanders (5.8% vs 4.6%), and a higher proportion with 3 or more comorbidities (16% vs 12%). Most people got the Pfizer vaccine (72% with a booster, 70% without). About 25% of the group got the Moderna shots and about 4% got the Johnson & Johnson’s vaccine.
During follow-up the researchers counted 48,893 COVID-19 breakthrough infections (6% of 788,792), with a rising rate after the Delta and Omicron strains took hold in the United States.
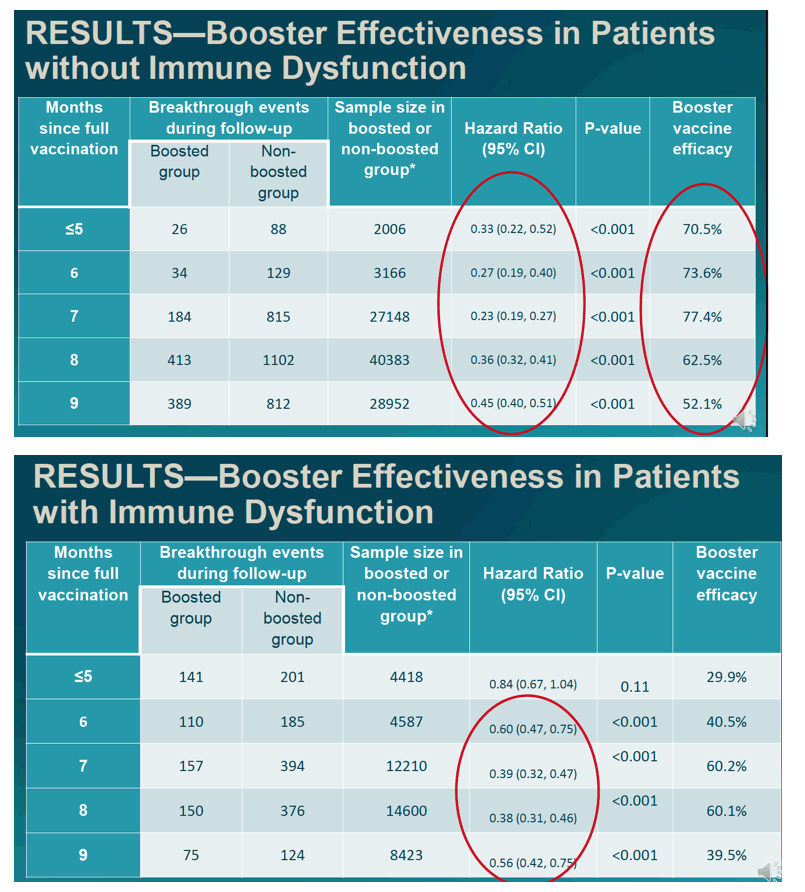
In people without immune dysfunction, booster vaccine efficacy stood at 70.5% within 5 months of full vaccination (hazard ratio [HR] 0.33, 95% confidence interval [CI] 0.22 to 0.52, P < 0.001). Booster efficacy edged up to 73.6% 6 months after full vaccination and to 77.4% 7 months after full vaccination. Then booster efficacy waned to 62.5% at 8 months and to 52.1% at 9 months. A booster dose offered less protection against breakthrough infection in people with immune dysfunction, but efficacy was still significantly greater with than without a booster at 6 months (40.5%), 7 months (60.2%), 8 months (60.1%), and 9 months (39.5%).
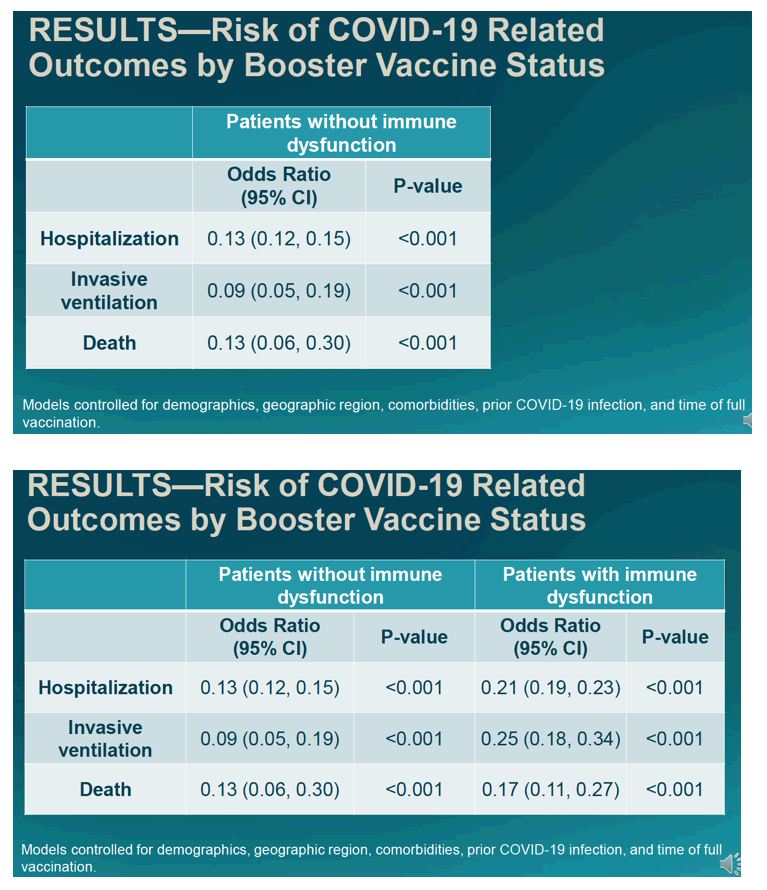
Compared with unboosted fully dosed people, those with a booster shot had significantly lower odds of hospital admission whether they had no immune dysfunction (odds ratio [OR] 0.13, 95% CI 0.12 to 0.15) or had immune dysfunction (OR 0.21, 95% CI 0.19 to 0.23) (P < 0.001 for these two comparisons and all following comparisons.) Boosting also strongly protected against invasive ventilation in people without immune dysfunction (OR 0.09, 95% CI 0.05 to 0.19) and those with immune dysfunction (OR 0.25, 95% CI 0.18 to 0.34). Boosting similarly slashed odds of death in the immune-competent group (OR 0.13, 95% CI 0.06 to 0.30) and the immune-compromised group (OR 0.17, 95% CI 0.11 to 0.27).
The N3C team concluded that a booster dose after full vaccination offered US residents brawny protection against COVID-19 breakthrough infection, hospital admission, invasive ventilation, and death when compared with full vaccination alone.
Reference
1. Sun J, Zheng Q, Anzalone AJ, et al. COVID-19 booster vaccine effectiveness in people with and without immune dysfunction. 2022 CROI, February 12-16 and 22-24, 2022. Abstract 48.
---------------------
program abstract
Background:
SARS-CoV-2 breakthrough infections in vaccinated individuals and in those who had a prior infection have been observed globally, but the transmission potential of these infections is unknown.
Methods:
Leveraging the national databases, effects of vaccination and of prior infection on SARS-CoV-2 infectiousness were investigated by comparing the RT-qPCR cycle threshold (Ct) values (inversely correlated with viral load and culturable virus) in matched cohorts of primary infections in unvaccinated individuals, reinfections in unvaccinated individuals, BNT162b2 (Pfizer-BioNTech) breakthrough infections, and mRNA-1273 (Moderna) breakthrough infections. Pairwise comparisons were conducted assuming linear and non-linear relationships.
Results:
Through analyses of the randomly diagnosed infections, the mean Ct value was higher in all cohorts of breakthrough infections compared to the cohort of primary infections in unvaccinated individuals. The Ct value was 1.3 (95% CI: 0.9-1.8) cycles higher for BNT162b2 breakthrough infections, 3.2 (95% CI: 1.8-4.5) cycles higher for mRNA-1273 breakthrough infections, and 4.0 (95% CI: 3.4-4.6) cycles higher for reinfections in unvaccinated individuals. A sensitivity analysis assuming that infectiousness is non-linearly proportional to viral load ( ) yielded similar results.
Conclusion:
Differences imply that breakthrough infections are at least 50% less infectious than primary infections in unvaccinated individuals. Public health benefits of vaccination may have been underestimated, as COVID-19 vaccines not only protect against acquisition of infection, but also appear to protect against transmission of infection.

|
| |
|
 |
 |
|
|