 |
 |
 |
| |
Gilead to Present Latest Data From Across Liver Disease Development Programs at the International Liver Congress™ 2022
|
| |
| |
- Two Oral Presentations and 22 Posters Will Be Presented Across HDV, HCV, HBV, NASH and PSC -
- Oral Presentations of Latest Phase 3 Hepcludex ® (bulevirtide) Efficacy and Safety and Patient-Reported Outcomes Data Reinforce the Clinical Importance of the First-in-Class Treatment for HDV -
June 21, 2022
FOSTER CITY, Calif.--(BUSINESS WIRE)-- Gilead Sciences, Inc. (Nasdaq:GILD) today announced that more than 80 abstracts will be presented at the International Liver Congress™ (ILC) 2022, taking place from June 22-26, 2022. Key oral presentations will include Week 48 primary endpoint data from the Pivotal Phase 3 program of Hepcludex® (bulevirtide) evaluating its efficacy and safety for the treatment of hepatitis delta virus (HDV) and the impact of the treatment on patient-reported outcomes. Gilead will also present real-world data on global efforts to support the World Health Organization's (WHO) goal of hepatitis C (HCV) elimination, long-term results from studies in the treatment of chronic hepatitis B (HBV) and ongoing research in nonalcoholic steatohepatitis (NASH) and primary sclerosing cholangitis (PSC).
"We are very proud to share such a broad range of research and progress at this year's International Liver Congress as we continue to pursue solutions to some of the greatest unmet needs for people living with liver disease," said Merdad Parsey, MD, PhD, Chief Medical Officer, Gilead Sciences. "As a leader in liver disease, with more than two decades of experience in HCV and HBV, we are applying our expertise to develop treatments for HDV and pioneering research into NASH, PSC and HBV cure."
Driving Innovation in HDV Research
Gilead will present the latest data from the Phase 3 MYR301 study on the safety and efficacy (Oral 0509) of bulevirtide in chronic HDV at Week 48 and patient-reported outcomes (Oral 3237) in adults with chronic HDV and compensated liver disease. These results underscore the utility of bulevirtide as the first-in-class treatment for chronic HDV.
In addition to advancing scientific innovation in HDV, Gilead is working in partnership with the liver community to increase understanding of the burden and impact of HDV for patients and health systems. At ILC 2022, nine studies will be presented further characterising the HDV burden, prevalence, epidemiology, patient characteristics and resulting economic impact on health systems. This includes an analysis of the U.S. All-Payer Claims Database (Posters 1436 and 1326) which found that 4.8% of the adults with HBV also had an HDV diagnosis. Adults with HDV also had high rates of baseline comorbidities, liver disease severity and experienced significantly greater overall healthcare resource utilization and costs. These findings highlight the need for more effective strategies to screen, diagnose and treat HDV, which may also translate into cost savings for the healthcare system.
Bulevirtide was granted Conditional Marketing Authorization by the European Commission and is an investigational agent in the U.S. and outside of the European Economic Area. In these regions, health authorities have not established the safety and efficacy of bulevirtide. A Biologics License Application (BLA) has been submitted to the U.S. Food and Drug Administration (FDA) for bulevirtide for injection (2 mg) to treat HDV in adults with compensated liver disease.
Impact of Treatment in Viral Hepatitis
Data presented on HCV will further explore the benefit of treatment with direct-acting antivirals (DAAs) on clinical markers, quality of life, cost effectiveness and progress toward the WHO goal of HCV elimination. Of note, Gilead will present data from two analyses in Spain which found that scaling up testing and treatment with DAA's reduced the prevalence and incidence of HCV over time (Poster 3205) and over five years, treatment with Epclusa® (sofosbuvir/velpatasvir) significantly reduced morbidity and mortality (Poster 3201).
Real-world evidence from the Kaiser Permanente Southern California healthcare system will also be presented (Poster 2954), showing a reduction in HCV-related morbidity and mortality, and a significant improvement in quality-adjusted life-years (QALYs) in patients treated with DAAs like sofosbuvir/velpatasvir. Furthermore, the use of DAAs in this setting resulted in cost savings within the healthcare system.
These data provide additional support for the effectiveness of utilizing testing and treatment of HCV with DAAs within key populations as a promising strategy to not only reduce the clinical and economic burden of HCV, but as strategies to ultimately achieve the WHO's goal of viral hepatitis elimination by 2030.
In HBV, data presented will highlight the long-term results of switching to Vemlidy® (tenofovir alafenamide 25 mg, TAF) for HBV prophylaxis in post-liver transplant patients with chronic kidney disease, providing sustained improvements in bone and renal safety parameters (Poster 0832). In addition, Gilead will present results from a study in which a new multiplex imaging method was used to quantify HBV hepatocyte burden, demonstrating a substantial reduction in HBV liver burden with anti-viral treatment (Poster 0660).
Advancing Liver Fibrosis Monitoring and Treatment
Five presentations will include a range of early data from the company's broader liver disease research and development program as Gilead continues its work to pursue new approaches in the potential treatment and monitoring of NASH and PSC.
Non-invasive measures of treatment response that avoid the need for liver biopsy remain a significant unmet need in NASH clinical research and patient care. New data will be presented assessing the associations between treatment-induced changes in the MRI-aspartate aminotransferase (MAST) Risk score, and noninvasive and histologic measures of fibrosis in patients with advanced fibrosis due to NASH (Poster 1403). The study found the MAST Risk score is correlated with noninvasive and histologic measures of fibrosis and may be a useful marker of treatment response beyond conventional histologic methods.
In addition, Gilead will present a proof-of-concept study, evaluating the safety and efficacy of escalating doses of investigational cilofexor (GS-9674) in patients with compensated cirrhosis due to PSC (Poster 1405). The study found escalating doses of cilofexor over 12 weeks were well tolerated and showed improved markers of cholestasis and liver biochemistry. Cilofexor is undergoing evaluation in the ongoing Phase 3 PRIMIS study of PSC patients without cirrhosis.
Key abstracts being presented at ILC 2022 include:
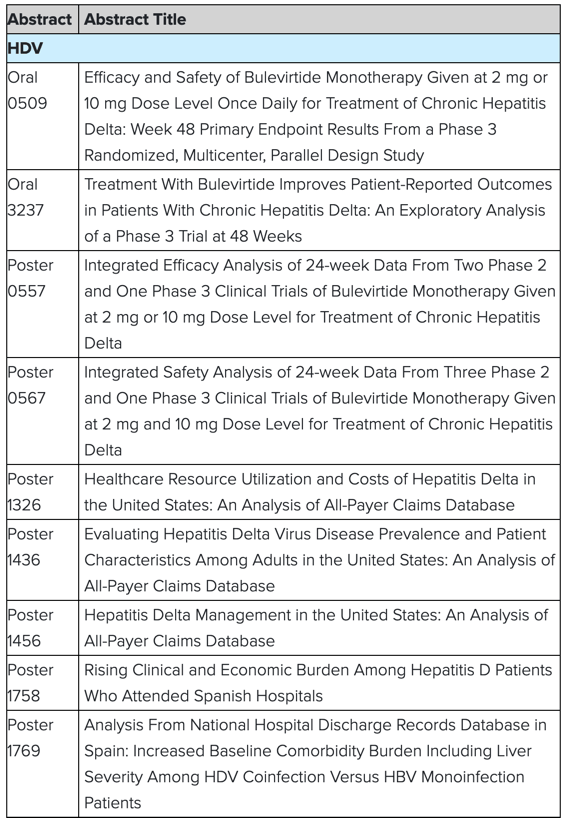
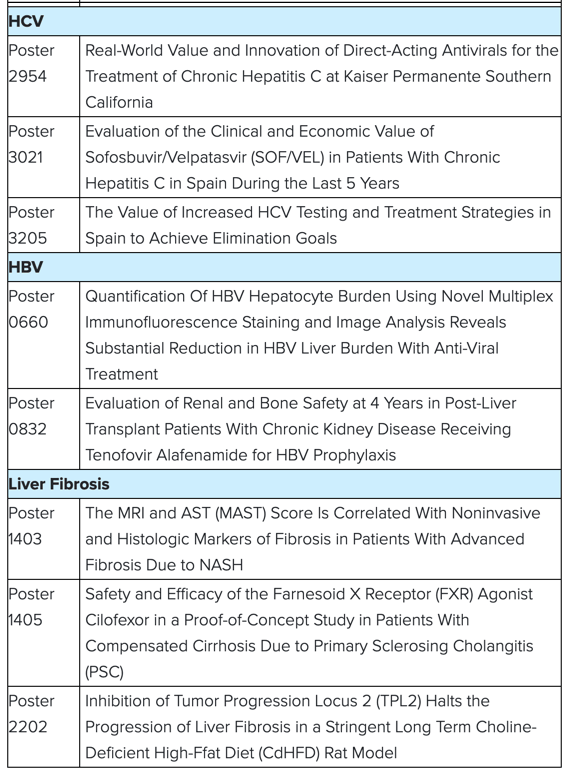
or more information, including a complete list of abstract titles being presented at the meeting, please visit
https://easl.eu/wp-content/uploads/2022/05/ILC-2022-List-of-accepted-abstracts-FINAL.pdf
.
Cilofexor, firsocostat, inarigivir, selgantolimod and bulevirtide are investigational compounds and are not approved by the FDA or any other regulatory authority; their safety and efficacy have not been established.
Please see below for the U.S. Indications and Important Safety Information, including BOXED WARNINGS, for Epclusa and Vemlidy.
U.S. Important Safety Information And Indication for Epclusa
BOXED WARNING: RISK OF HEPATITIS B VIRUS REACTIVATION IN HCV/HBV COINFECTED PATIENTS
Test all patients for evidence of current or prior hepatitis B virus (HBV) infection before initiating treatment with EPCLUSA. HBV reactivation has been reported in HCV/HBV coinfected patients who were undergoing or had completed treatment with HCV direct acting antivirals (DAAs) and were not receiving HBV antiviral therapy. Some cases have resulted in fulminant hepatitis, hepatic failure, and death. Cases have been reported in patients who are HBsAg positive, in patients with serologic evidence of resolved HBV, and also in patients receiving certain immunosuppressant or chemotherapeutic agents; the risk of HBV reactivation associated with treatment with HCV DAAs may be increased in patients taking these other agents. Monitor HCV/HBV coinfected patients for hepatitis flare or HBV reactivation during HCV treatment and post-treatment follow-up. Initiate appropriate patient management for HBV infection as clinically indicated.
Contraindications
• If EPCLUSA is used in combination with ribavirin (RBV), all contraindications, warnings and precautions, in particular pregnancy avoidance, and adverse reactions to RBV also apply. Refer to RBV prescribing information.
Warnings and Precautions
• Serious Symptomatic Bradycardia When Coadministered with Amiodarone: Amiodarone is not recommended for use with EPCLUSA due to the risk of symptomatic bradycardia, particularly in patients also taking beta blockers or with underlying cardiac comorbidities and/or with advanced liver disease. A fatal cardiac arrest was reported in a patient taking amiodarone who was coadministered a sofosbuvir containing regimen. In patients without alternative, viable treatment options, cardiac monitoring is recommended. Patients should seek immediate medical evaluation if they develop signs or symptoms of bradycardia.
• Risk of Reduced Therapeutic Effect Due to Use with P-gp Inducers and/or Moderate to Strong Inducers of CYP2B6, CYP2C8 or CYP3A4: Rifampin, St. John's wort and carbamazepine are not recommended for use with EPCLUSA as they may significantly decrease sofosbuvir and/or velpatasvir plasma concentrations.
Adverse Reactions
• The most common adverse reactions (≥10%, all grades) with EPCLUSA in adults and pediatric patients 6 years of age and older were headache and fatigue; and when used with RBV in adults with decompensated cirrhosis were fatigue, anemia, nausea, headache, insomnia and diarrhea. The most common adverse reactions (≥10%, grade 1 or 2) in pediatric patients less than 6 years of age were vomiting and spitting up the drug.
Drug Interactions
• Coadministration of EPCLUSA is not recommended with topotecan due to increased concentrations of topotecan.
• Coadministration of EPCLUSA is not recommended with proton-pump inhibitors, phenobarbital, phenytoin, rifabutin, rifapentine, efavirenz, and tipranavir/ritonavir due to decreased concentrations of sofosbuvir and/or velpatasvir.
Consult the full Prescribing Information for EPCLUSA for more information on potentially significant drug interactions, including clinical comments.
Indication
EPCLUSA is indicated for the treatment of adult and pediatric patients 3 years of age and older with chronic hepatitis C virus genotype 1, 2, 3, 4, 5, or 6 infection without cirrhosis or with compensated cirrhosis and in combination with ribavirin for those with decompensated cirrhosis.
U.S. Important Safety Information and Indication for Vemlidy
BOXED WARNING: POST TREATMENT SEVERE ACUTE EXACERBATION OF HEPATITIS B
Discontinuation of anti-hepatitis B therapy, including VEMLIDY, may result in severe acute exacerbations of hepatitis B. Hepatic function should be monitored closely with both clinical and laboratory follow-up for at least several months in patients who discontinue anti-hepatitis B therapy, including VEMLIDY. If appropriate, resumption of anti-hepatitis B therapy may be warranted.
Warnings and Precautions
https://www.gilead.com/news-and-press/press-room/press-releases/2022/6/gilead-to-present-latest-data-from-across-liver-disease-development-programs-at-the-international-liver-congress-2022
|
| |
|
 |
 |
|
|