 |
 |
 |
| |
Low Use of Preventive CVD Measures - Use of Preventive Measures
for Cardiovascular Disease in People Living with HIV
|
| |
| |
Glasgow 2022 Oct 23-26
N. Jaschinski, B. Neesgaard, F. Wit, M. Van der Valk, H. Günthard, M. Stöckle, E. Wallner, J. Kowalska, A.L. Ridolfo, P. Nowak, A. Castagna, A. d'Arminio Monforte, N. Chkhartishvili, K. Petoumenos, J. Hoy, S.

Program Abstract
Background: While cardiovascular disease (CVD) contributes significantly to morbidity and mortality in people living with HIV (PLWHIV), data on the uptake of preventive measures for CVD are limited.
Materials and methods: We included participants from the multinational RESPOND cohort in whom an estimated 10-year D:A:D CVD risk could be calculated. We determined the annual prevalence (1 July 2012 to 1 July 2019) of preventive measures use for those with a very high (>10%) estimated CVD risk and eligible for each specific measure. Binomial regression with robust standard errors assessed factors associated with the uptake of each preventative measure.
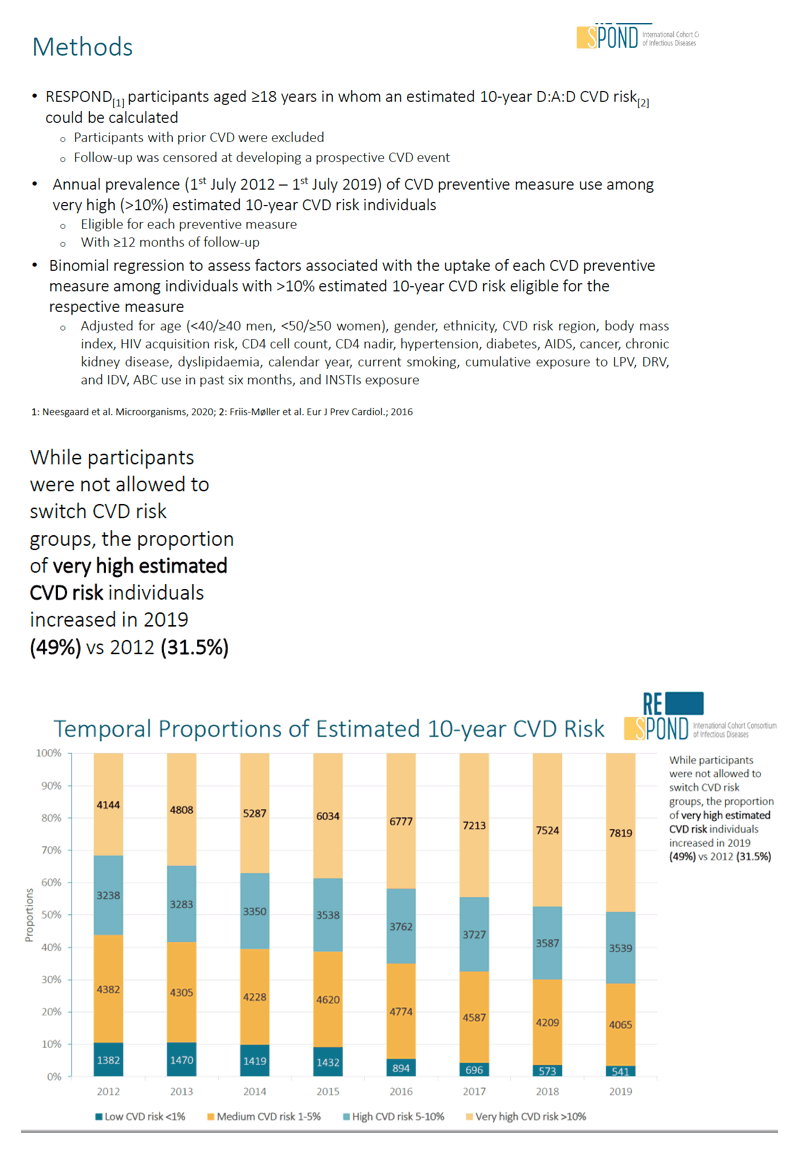
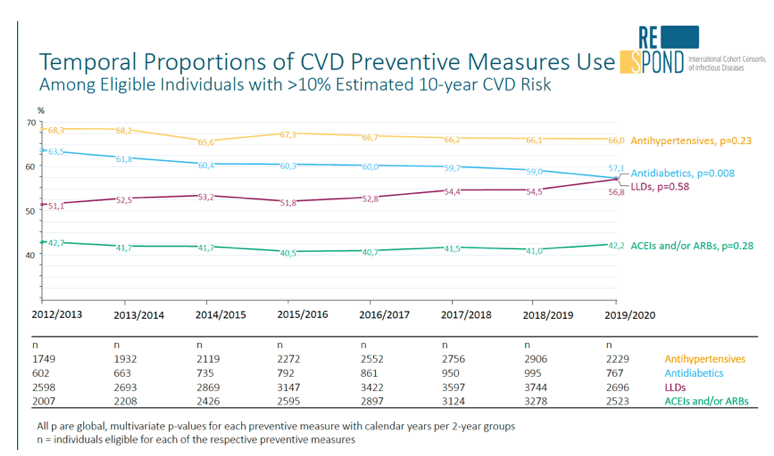
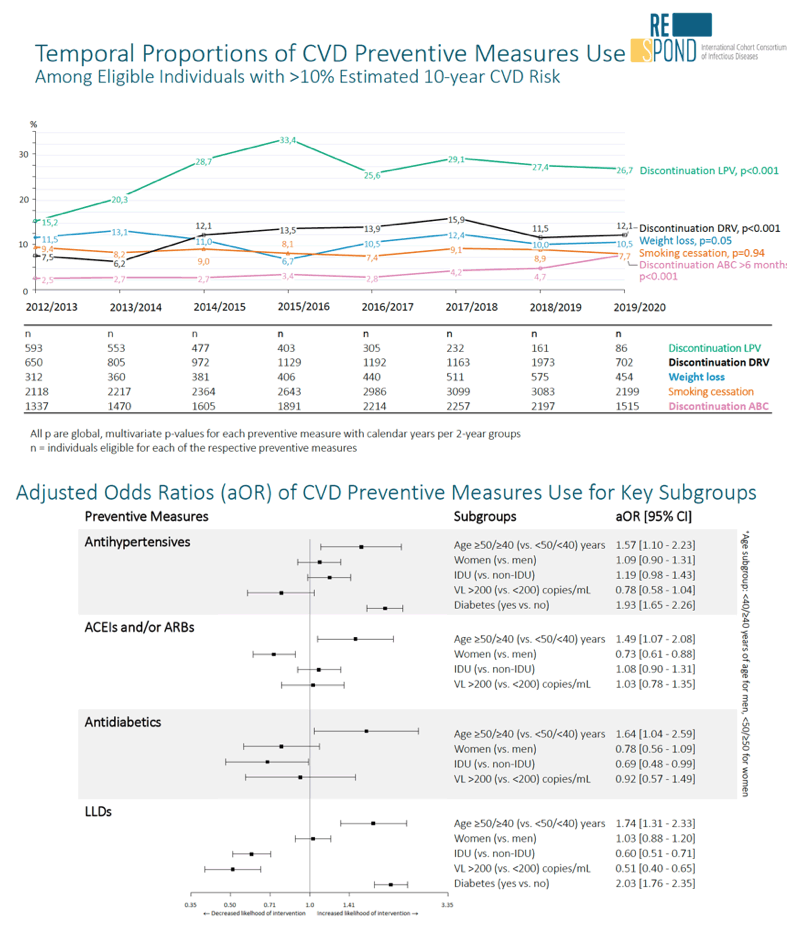
Results: The crude proportion with >10% estimated 10-year CVD risk increased from 31.5% (4144/13 146) in 2012 to 45.0% (7187/15 964) in 2019 (p < 0.0001). In 2019, in those at very high risk, 65.6% (1462/2229) with hypertension received antihypertensives, 56.4% (1520/2696) with dyslipidaemia received lipid-lowering drugs (LLDs) and 41.8% (1055/2523) with diabetes/hypertension used angiotensin-converting enzyme inhibitors (ACEIs)/angiotensin receptor blockers (ARBs). Equally, 8.1% (178/2199) of smokers ceased smoking and 10.6% (48/454) with BMI >30 kg/m2 lost ≥7% bodyweight. We found no significant changes over time in the use of any of these measures (2012 to 2019; all multivariate p > 0.05). While fewer diabetics received antidiabetics in later years (2012; 63.5% [382/602] vs 2019; 56.7% [435/767]), discontinuation of darunavir (7.5% [49/650] vs 12.1% [85/702]), lopinavir (15.2% [90/593] vs 26.7% [23/86]) and abacavir (2.5% [34/1337] vs 7.9% [120/1515]) increased among individuals using these drugs (all multivariate p < 0.01). In multivariable analyses (Figure 1), older individuals (≥40 years for men, ≥50 for women vs <40/<50) were more likely to use antihypertensives, ACEIs/ARBs, antidiabetics and LLDs.
Individuals with diabetes (vs those without) were also more likely to use antihypertensives, LLDs and cease smoking. In contrast, LLD use and smoking cessation were less likely in those with a viral load ≥200 copies/mL (vs <200) and intravenous drug use (IDU) as HIV acquisition risk (vs non-IDU). Besides women being less likely to receive ACEIs/ARBs, the use of preventive measures was similar between genders.
Conclusions: Despite an increased proportion of individuals at very high estimated CVD risk, CVD preventive measures were underused in RESPOND. Our findings call for greater awareness of management guidelines for CVD risk factors in PLWHIV.




|
| |
|
 |
 |
|
|