 |
 |
 |
| |
Prevalence, risk factors and the impact of antiretroviral treatment in SARS-CoV-2 infection in people with HIV: A cross-sectional study
|
| |
| |
One Fifth With HIV in Barcelona Got COVID-No Protection From ART or TDF
HIV Drug Therapy Glasgow, October 23-26, 2022
Mark Mascolini
Nearly 1 in 5 people in a 4400-person Barcelona HIV group got COVID from late 2020 to mid-2021 [1]. Young women and men, including men who have sex with men (MSM), and people with active syphilis ran the highest risk of COVID. Antiretroviral therapy (ART) and tenofovir disoproxil fumarate (TDF) did not lower COVID risk, as they appeared to in earlier reports [2,3].
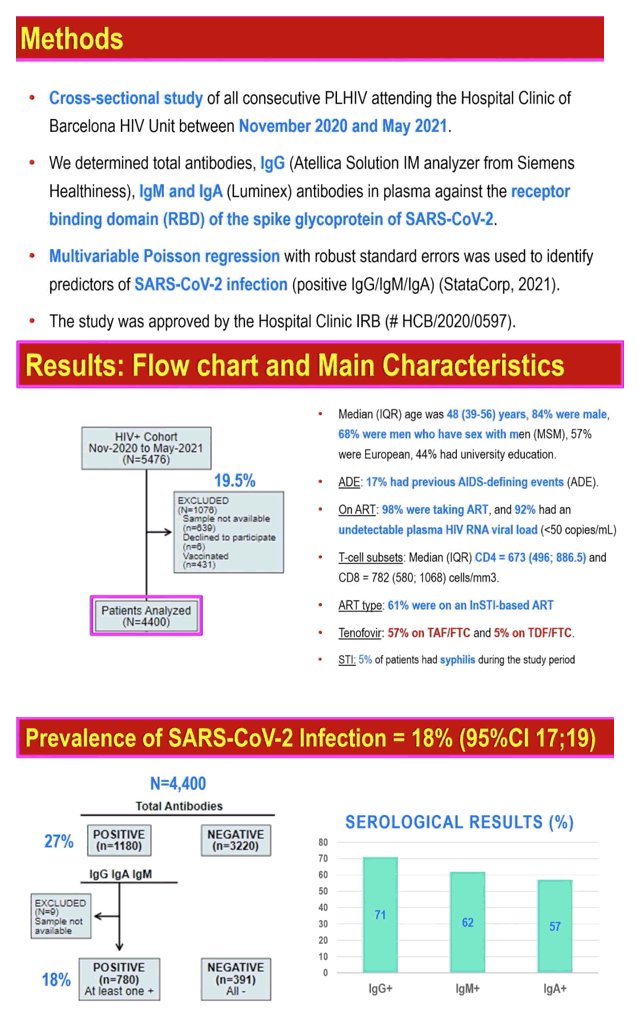
The new study aimed to figure prevalence and risk factors for SARS-CoV-2 infection in people with HIV cared for at the Hospital Clinic of Barcelona in Spain. This cross-sectional analysis considered all consecutive adults with HIV who came to the clinic between November 2020 and May 2021. The researchers used multivariable Poisson regression to find independent predictors of SARS-CoV-2 infection.
The study excluded people already vaccinated against the coronavirus. The 4400 people considered had a median age of 48 (interquartile range [IQR] 39 to 56), 84% were male, 68% were MSM, 57% were European, and 44% had a university education. Median CD4 count stood at 673 (IQR 496 to 886.50). Most people in the study group, 61%, were taking an integrase inhibitor regimen, while 57% were using tenofovir alafenamide/emtricitabine (TAF/FTC) and 5% TDF/FTC. One in 20 people (5%) had syphilis during the study period.
Antibody testing indicated SARS-CoV-2 prevalence of 18% (95% confidence interval [CI] 17 to 19). Specifically, of the 4400 participants, 780 (18%) tested positive for at least one antibody-IgA, IgG, or IgM.
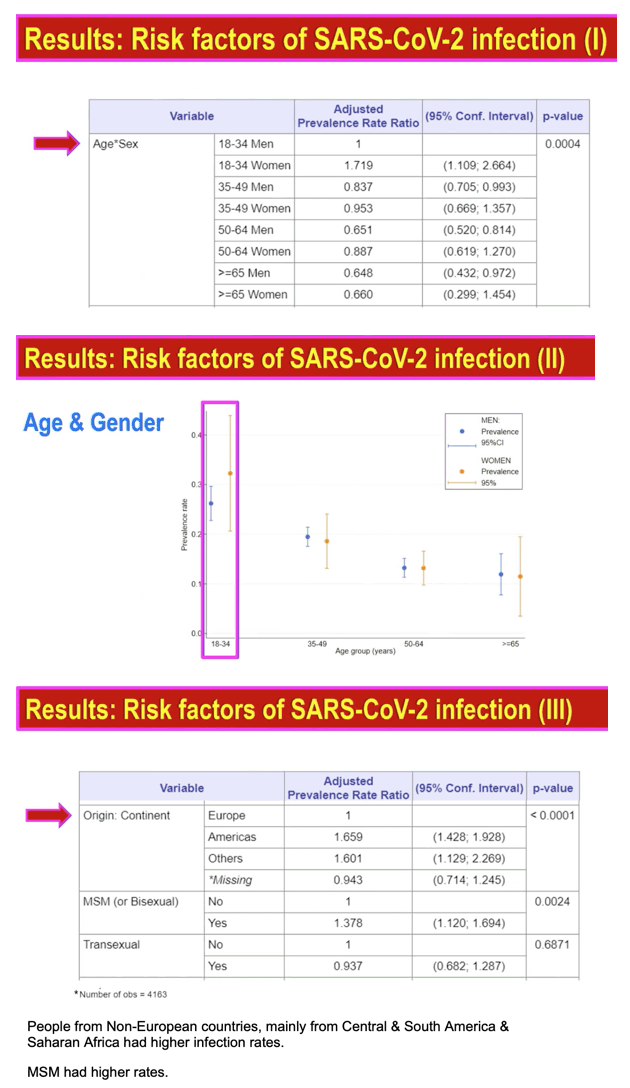
Compared with 18-to-34-year-old men, women that age had a 70% higher rate of SARS-CoV-2 infection (adjusted prevalence rate ratio [aPRR] 1.719, 95% CI 1.109 to 2.664). All older groups of men or women had lower aPRRs than 18-to-34-year-old men (P = 0.0004 overall).
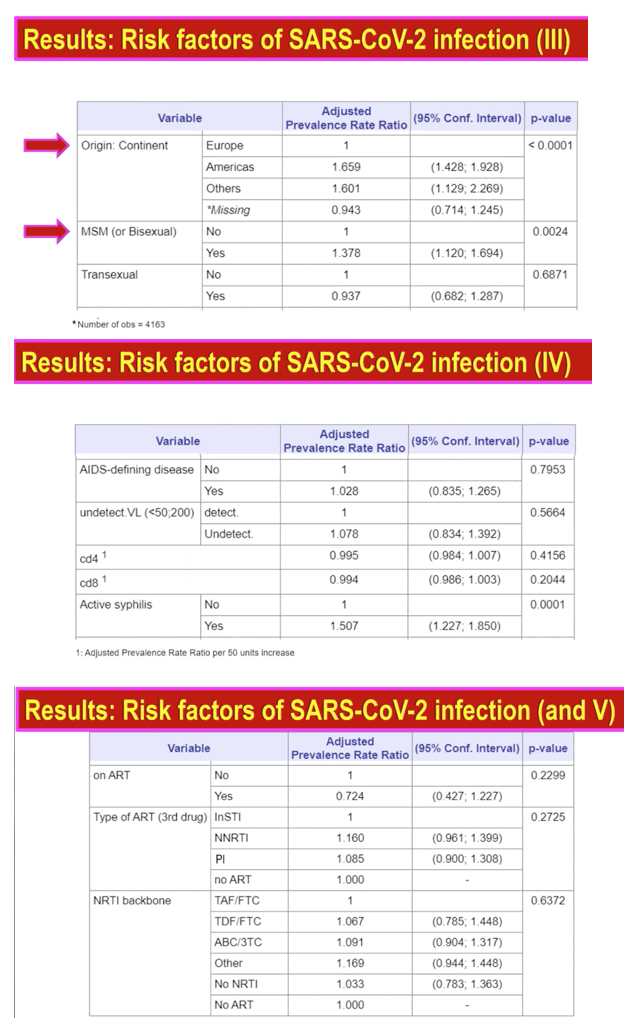
Compared with people born in Europe, those born in the Americas had a 66% higher risk of COVID and those born on other continents had a 60% higher risk. MSM ran almost a 40% higher risk of SARS-CoV-2 infection than non-MSM (aPRR 1.378, 95% CI 1.120 to 1.694, P = 0.0024). Transsexuals did not run a higher COVID risk than people who weren't transsexual.
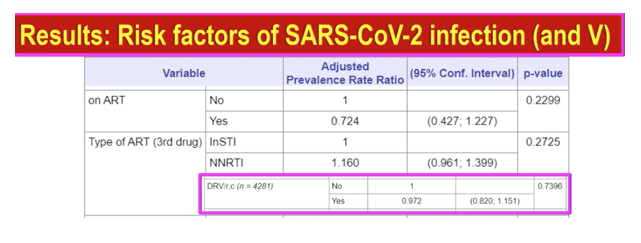
Having an AIDS-defining illness, an undetectable viral load, or a lower CD4 or CD8 count did not affect coronavirus risk. No antiretroviral factor affected SARS-CoV-2 risk-taking or not taking ART, anchor drug in regimen, or NRTI backbone, including TDF/FTC (compared with TAF/FTC). But people with active syphilis ran a 50% higher risk of SARS-CoV-2 infection (aPRR 1.507, 95% CI 1.227 to 1.850, P = 0.0001).
The Barcelona team listed several limitations to their study: low number of people with a CD4 count below 200 because they were among the first vaccinated against the coronavirus, no comorbidity data, no clinical severity data, and no data comparing this HIV group to the general population.
References
1. Miro JM, de Lazzari E, Blanco JL, et al. Prevalence, risk factors and the impact of antiretroviral treatment in SARS-CoV-2 infection in people with HIV: a cross-sectional study. HIV Drug Therapy Glasgow, October 23-26, 2022.
2. Del Amo J, Polo R, Moreno S, et al. Incidence and severity of COVID-19 in HIV-positive persons receiving antiretroviral therapy: a cohort study. Ann Intern Med. 2020;173:536-541. doi: 10.7326/M20-3689. https://www.acpjournals.org/doi/full/10.7326/M20-3689
3. Nomah DK, Reyes-Urueña J, Díaz Y, et al. Impact of tenofovir on SARS-CoV-2 infection and severe outcomes among people living with HIV: a propensity score-matched study. J Antimicrob Chemother. 2022;77:2265-2273. doi: 10.1093/jac/dkac177. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9384242/


|
| |
|
 |
 |
|
|