 |
 |
 |
| |
UK Survey: Monkeypox Vax Highly Acceptable, but
Less Agreement on Public Health Measures
|
| |
| |
HIV Drug Therapy Glasgow, October 23-26, 2022
Mark Mascolini
A large majority of respondents to a UK survey, 86%, said they would accept a monkeypox vaccine [1]. But basic understanding of the virus and public health measures surrounding it was spotty. For example, well over one third of respondents did not agree that monkeypox originally came from animals.
The Monkeypox (MPXV) Community Survey is a cross-sectional survey created in collaboration with community members and conducted between June 15 and July 27, 2022. Aiming to examine awareness and understanding of the monkeypox outbreak among the most affected communities in the UK, the survey targeted adults via community channels on social media and the gay dating app Grindr.
Among the 1932 respondents, 86% were cis or trans men who have sex with men (MSM). While 1750 respondents identified themselves as men, 88 identified as women, 34 as nonbinary people, 15 as transgender women, and 12 as transgender men. Three quarters of respondents (77%) described their sexual identity as gay or lesbian, 12% as bisexual, 4% as heterosexual, and 3% as queer.
While 71% identified themselves as white, 11% reported "mixed" or "other" heritage groups, 8% Asian, and 2% LatinX. More than one third (39%) were younger than 40, 85% were employed, 79% had completed higher education, and 7% said they were living with HIV.
Half of respondents, 49.5%, said they heard or read a lot about monkeypox, though a similar fraction, 48.8%, had heard or read little. The three most frequently cited sources of monkeypox information were online news (57%), TV or radio news (51%), and printed news (27%). Fair shares of respondents heard about monkeypox on Twitter (21%), dating apps (13%), and even health care providers (11%).
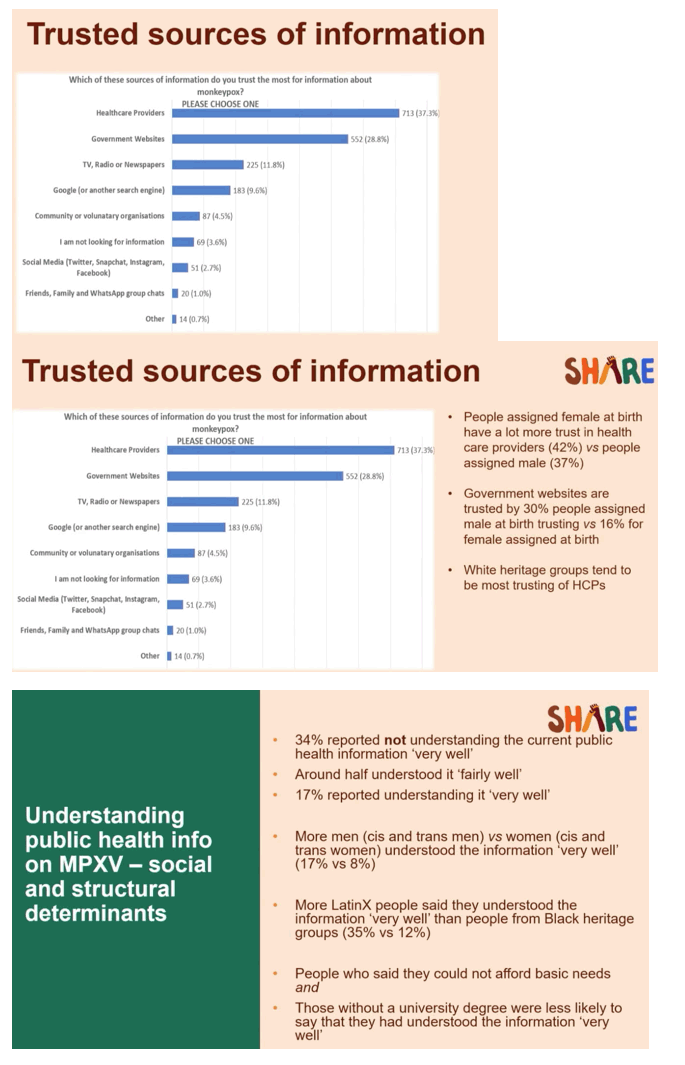
In a question for which surveyed people could list only one response, 37.3% said their most trusted source of monkeypox information was health care providers, followed by government websites (28.8%), TV, radio, or newspapers (11.8%), Google or another search engine (9.6%), community of voluntary organizations (4.5%), social media (2.7%), and friends, family, and WhatsApp group chats (1.0%); 3.6% said they were not looking for information.
A higher proportion of people assigned female than male at birth trusted health care providers for information (42% vs 37%). Conversely, a higher percentage of males than females trusted government websites (30% vs 16%). Overall, people of white heritage tended to trust health care providers for information more than other groups did.
Only 17% of respondents said they understand public health information on monkeypox "very well," compared with half saying they understood things "fairly well" and one third who did not understand monkeypox information very well. More cis and trans men than cis and trans women thought they understood monkeypox very well (17% vs 8%). More LatinX people than black people reported understanding monkeypox very well (35% vs 12%).
Half of respondents (51%) considered themselves at risk for monkeypox infection, while 27% did not and 21% didn't know.
Next respondents answered questions about four key public health messages:
1. When asked if they believe monkeypox originates from animal, 60% agreed or somewhat agreed, 31% neither agreed nor disagreed, and 6% disagreed. People who could not afford basic needs (versus those who could) and people without versus with a higher education degree were less likely to agree or somewhat agree that the virus came from animals. MSM were far more likely than other groups to agree or somewhat agree that monkeypox came from animals.
2. When asked where they would seek care if they got monkeypox, half said they would go to a sexual health clinic, 29% would go to a general practitioner, 6% would visit an emergency care service, and small fractions would go to a pharmacy or a voluntary organization.
3. When asked if they agreed people with monkeypox should self-isolate for 21 days, 62% agreed, 9% disagreed, and 29% weren't sure. Groups more likely to disagree were those without a higher education, the unemployed, people with a disability, or Asians versus whites.
4. When asked if they would accept a monkeypox vaccine, 86% said yes, 6% said no, and 8% weren't sure. MSM were more likely than non-MSM to say they would get the vaccine. Groups with a lower likelihood of accepting a vaccine were bisexuals or heterosexuals, people who could not afford basic needs, and blacks or "other" racial/ethnic groups.
Almost half of all respondents-45%-said they did not feel people who talk about monkeypox in the media represent them.
The researchers concluded that, although monkeypox vaccine acceptability is high, "public health information and advice were neither universally accepted nor correctly understood." They urged greater engagement with "disadvantaged members of affected communities."
A limitation of this kind of survey is that respondents are self-selected rather than scientifically selected to represent a population of interest. The researchers could not verify that all respondents lived in the UK because the survey was completely anonymous. But they assumed respondents lived in the UK because they were recruited via UK social media and they were answering questions that specified the issue was monkeypox in the UK.
Reference
1. Paparini S, Whitcare R, Smuk M, et al. Perceptions and understandings of media and public health messaging about the monkeypox outbreak in the UK: findings from a rapid response, co-produced survey. Including women in the public health response to the monkeypox (MPXV) outbreak in the UK. HIV Drug Therapy Glasgow, October 23-26, 2022. Abstract O418.






|
| |
|
 |
 |
|
|