| |
Effects of Resmetirom on Noninvasive Endpoints in a
36-Week Phase 2 Active Treatment Extension Study in Patients With NASH
|
| |
| |
Download the PDF -- Effects of Resmetirom on Noninvasive Endpoints in a 36-Week Phase 2 Active Treatment Extension Study in Patients With NASH
Resmetirom is in phase 3 with toppling results reported in this press release. There is an Expanded Access program.
04 January 2021
Thyroid axis hormones may be altered in NASH, which is associated with subclinical and clinical hypothyroidism.(15, 16)
Mechanistically, as a targeted hepatic therapeutic acting through THR-β, resmetirom may restore components of liver function that are defective in NASH. Thyroid hormone acting through THR-β is vital to maintain normal lipid regulation and mitochondrial function in the liver.(15) In a large National Health and Nutrition Education Survey database and median follow-up of 23 years, individuals with low thyroid function demonstrated an association with NAFLD.(26) Low thyroid function was associated with a higher risk for all-cause and cardiovascular mortality in individuals with NAFLD and not in those without NAFLD.
Abstract
Resmetirom (MGL-3196), a selective thyroid hormone receptor-β agonist, was evaluated in a 36-week paired liver biopsy study (NCT02912260) in adults with biopsy-confirmed nonalcoholic steatohepatitis (NASH). The primary endpoint was relative liver fat reduction as assessed by MRI-proton density fat fraction (MRI-PDFF), and secondary endpoints included histopathology. Subsequently, a 36-week active treatment open-label extension (OLE) study was conducted in 31 consenting patients (including 14 former placebo patients) with persistently mild to markedly elevated liver enzymes at the end of the main study.
In patients treated with resmetirom (80 or 100 mg orally per day), MRI-PDFF reduction at OLE week 36 was -11.1% (1.5%) mean reduction (standard error [SE]; P < 0.0001) and -52.3% (4.4%) mean relative reduction, P < 0.0001. Low-density lipoprotein (LDL) cholesterol (-26.1% [4.5%], P < 0.0001), apolipoprotein B (-23.8% [3.0%], P < 0.0001), and triglycerides (-19.6% [5.4%], P = 0.0012; -46.1 [14.5] mg/dL, P = 0.0031) were reduced from baseline. Markers of fibrosis were reduced, including liver stiffness assessed by transient elastography (-2.1 [0.8] mean kilopascals [SE], P = 0.015) and N-terminal type III collagen pro-peptide (PRO-C3) (-9.8 [2.3] ng/mL, P = 0.0004 (baseline ≥ 10 ng/mL). In the main and OLE studies, PRO-C3/C3M (matrix metalloproteinase-degraded C3), a marker of net fibrosis formation, was reduced in resmetirom-treated patients (-0.76 [-1.27, -0.24], P = 0.0044 and -0.68, P < 0.0001, respectively). Resmetirom was well tolerated, with few, nonserious adverse events.
Conclusion: The results of this 36-week OLE study support the efficacy and safety of resmetirom at daily doses of 80 mg and 100 mg, used in the ongoing phase 3 NASH study, MAESTRO-NASH (NCT03900429). The OLE study demonstrates a potential for noninvasive assessments to monitor the response to resmetirom from an individual patient with NASH.
Nonalcoholic steatohepatitis (NASH) is a progressive form of nonalcoholic fatty liver disease (NAFLD), defined as the presence of ≥5% hepatic steatosis with inflammation and hepatocyte injury (e.g., ballooning), with or without fibrosis.(1, 2)
NAFLD, including NASH, is associated with a constellation of comorbid conditions that include metabolic syndrome (obesity, type 2 diabetes mellitus, hypertension, dyslipidemia) and hypothyroidism and is associated with increased cardiovascular risk.(3)
Patients with more advanced NASH fibrosis have increased morbidity and mortality from both cardiovascular disease(4) and from progression of their liver disease, including progression to cirrhosis, liver failure, and hepatocellular carcinoma.(5, 6) Diagnosis of NASH is complicated by the requirement for an invasive procedure, liver biopsy, to confirm diagnosis, and there is an unmet need for noninvasive biomarkers and imaging that can diagnose and stage advanced NASH with fibrosis(7, 8) and monitor a patient's response to treatment.
There is no approved therapy for NASH, and its prevalence has increased with increasing world-wide prevalence of obesity.(9, 10)Obeticholic acid, a bile acid analog that activates farnesoid X receptors, improved fibrosis in a phase 3 clinical trial in patients with NASH and F2 or F3 fibrosis.(11) For other agents assessed in patients with NASH, trials with serial liver biopsies did not meet the primary endpoints of fibrosis reduction or NASH resolution.(12-14)
Evidence suggests that NASH may be, in part, a condition of diminished liver thyroid hormone levels or hepatic hypothyroidism, and that the incidence of clinical and subclinical hypothyroidism is higher in patients with NAFLD/NASH relative to age-matched controls.(15, 16)
Resmetirom (MGL-3196) is a liver-directed, orally active agonist of thyroid hormone receptor (THR) that is about 28-fold more selective than triiodothyronine (T3) for THR-β versus THR-α.(17, 18) It is highly protein bound (>99%), has poor tissue penetration outside the liver, and demonstrates specific uptake into the liver. In NASH, selectivity for THR-β may provide metabolic benefits of thyroid hormone that are mediated by the liver, including reduction of excess hepatic fat, atherogenic lipids (low-density lipoprotein-cholesterol [LDL-C], triglycerides), and lipoproteins (apolipoprotein B [ApoB], lipoprotein[a] [Lp(a)], Apo CIII), while avoiding unwanted systemic actions of excess thyroid hormone in heart and bone that are largely mediated through THR-α.(15)
In a 36-week phase 2 serial liver biopsy NASH clinical trial, resmetirom demonstrated statistically significant reductions compared with placebo in MRI-proton density fat fraction (PDFF) (a measure of liver steatosis), liver enzymes, atherogenic lipids, and Lp(a), markers of inflammation and fibrosis.(19) Resmetirom-treated patients also had improvements in NASH on liver biopsy compared with placebo. Patients who were on higher doses of resmetirom (≥80 mg vs. 60 mg), or who had higher exposure to resmetirom and/or demonstrated greater reduction in hepatic fat on week 12 MRI-PDFF, had a higher incidence of NASH resolution and liver fibrosis reduction. An active treatment open-label extension (OLE) study was conducted in a subset of patients completing the 36-week main study, who were predicted to have an incomplete response to either placebo or resmetirom treatment in the main study based on residual minimally to markedly elevated liver enzymes (alanine aminotransferase [ALT] and/or aspartate aminotransferase [AST]) at the end of the main study. The OLE study assessed the impact of 80 and 100 mg daily doses of resmetirom on safety and noninvasive assessments of NASH. Additionally, in both the main and OLE studies, the impact of resmetirom treatment was assessed on a biomarker of net fibrosis formation (N-terminal type III collagen propeptide [PRO-C3]/metalloproteinase-degraded collagen III [C3M]) and a measure of hepatic inflammation (free T3/reverse T3).
MRI-PDFF Outcomes
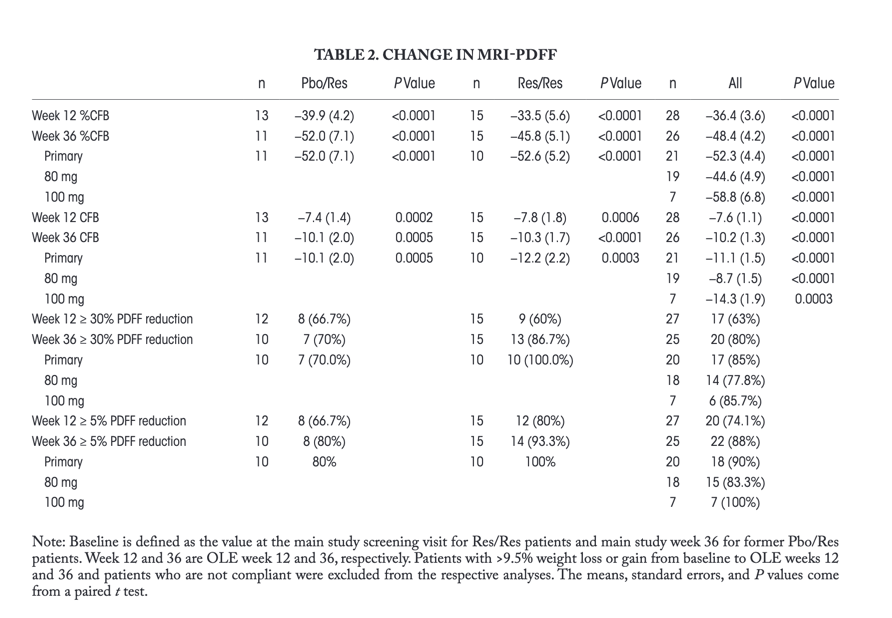
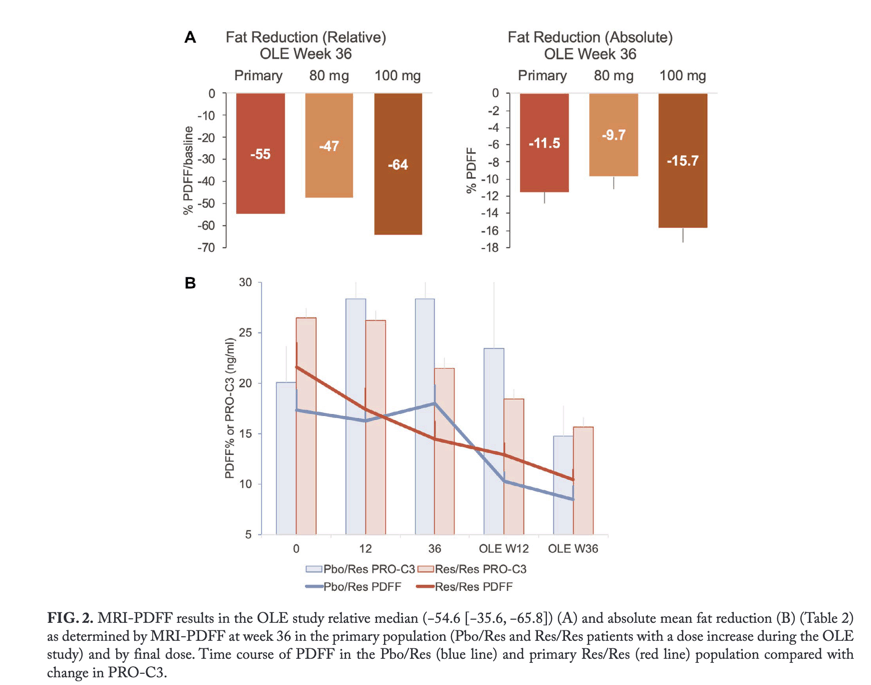
In the Res/Res population, the average reduction in PDFF during the main study at week 36 was 27.9%, and 31.6% at OLE study week 12, and did not change significantly from week 36 of the main study. At OLE week 12, 10/16 Res/Res patients were on the same dose of resmetirom as in the main study; seven additional dose increases were made after week 12, and one additional increase to 100 mg after the initial increase to 80 mg at week 4. At OLE week 36, Pbo/Res patients and Res/Res patients with a dose increase during the OLE study (primary efficacy population) experienced a mean relative reduction of 52.3% (standard error = 4.4%, P < 0.0001) (Table 2 and Figure 2) and absolute reduction of 11.1% (1.5%) in PDFF. Patients receiving 100 mg experienced a mean relative reduction in PDFF of 58.8% (6.8%) and absolute reduction of -14.3% (1.9%). Most of the OLE patients (85%) experienced at least a 30% PDFF relative reduction, and all patients had at least 20% relative reduction. All patients (100%) receiving 100 mg had ≥5% absolute reduction. Two patients with >10% weight gain during the study experienced >20% and <30% relative PDFF reduction.
The CAP score, a component of the FibroScan measurement that is considered a marker of hepatic steatosis,(21) showed no significant correlation with PDFF, at either week 36 (main) or OLE week 36 (R < 0.02, non-significant) and did not decrease significantly with treatment.
Lipids, Lipoproteins, and Liver Enzymes
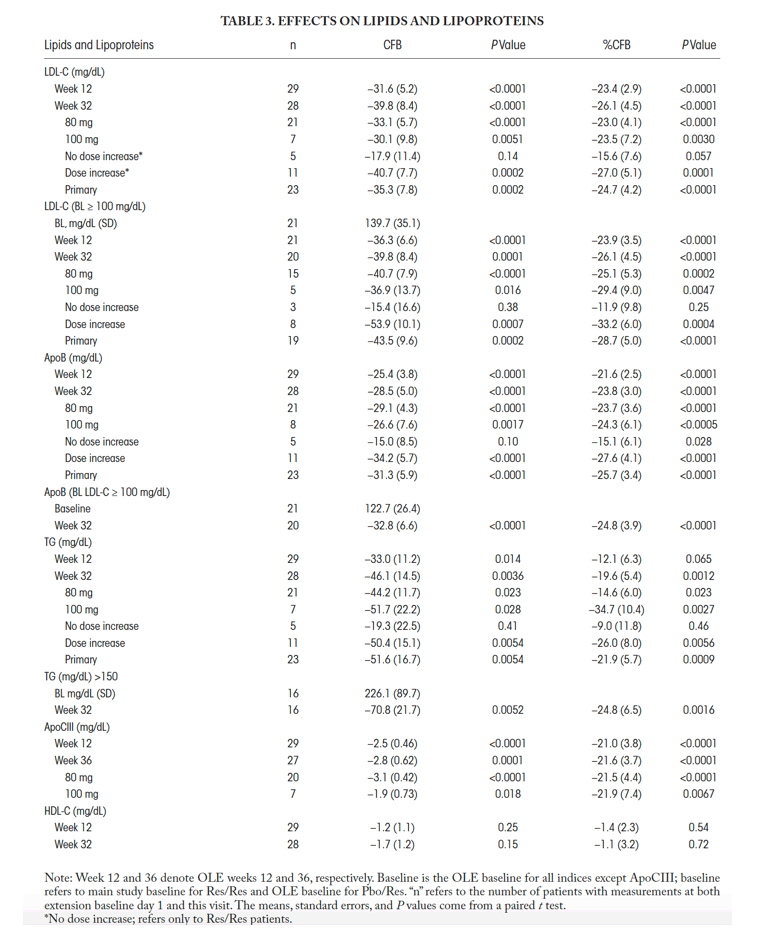
Atherogenic lipids and lipoproteins were reduced in resmetirom-treated patients, including statistically significant reductions in LDL-C (-26.1% [4.5%], P < 0.0001), ApoB (-23.8% [3.0%], P < 0.0001), apolipoprotein CIII (ApoCIII) (-21.6% [3.7%], P < 0.0001), and triglycerides (-46.1 [14.5] mg/dL, P = 0.0036) (Table 3).
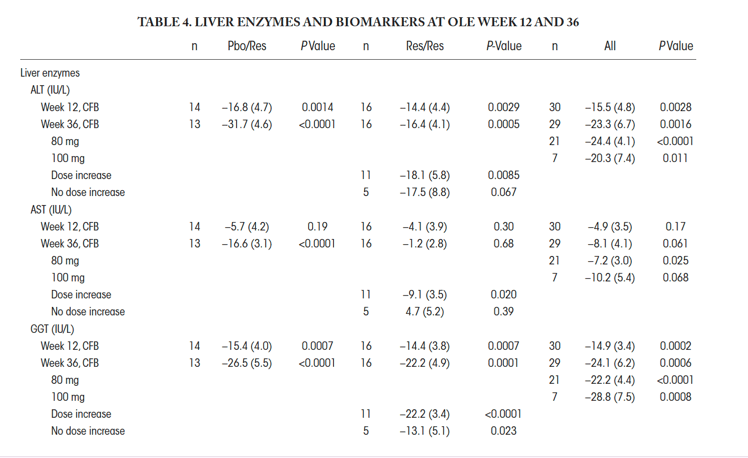
Liver enzymes, particularly ALT (-23.3 [6.7] IU/L, P = 00016) and GGT (-24.4 IU/L, P = 0.0006) (Table 4) declined over time, and sex hormone binding globulin (SHBG), a biomarker of resmetirom activity, increased (Supporting Table S1 and Fig. 3).
Safety
Comparison was made between the OLE study and the placebo group population from the main study (Table 5). Resmetirom at doses of 80 mg and 100 mg in the OLE study was well-tolerated with no serious or severe AEs. There was no increase in gastrointestinal AEs in the OLE study compared with the placebo group in the main study. No changes in vital signs, including body weight, heart rate or blood pressure, were seen (Supporting Table S1).
| |
| |
| |
|
|
|