| |
Emerging therapeutic approaches for the treatment
of NAFLD and type 2 diabetes mellitus - NASH pipeline, phase 3
|
| |
| |
Download the PDF here
Teamorelin
Clinical Predictors of Liver Fibrosis Presence and Progression in HIV-Associated Nonalcoholic Fatty Liver Disease
Clinical Predictors of Liver Fibrosis Presence and Progression in Human Immunodeficiency Virus-Associated Nonalcoholic Fatty Liver Disease
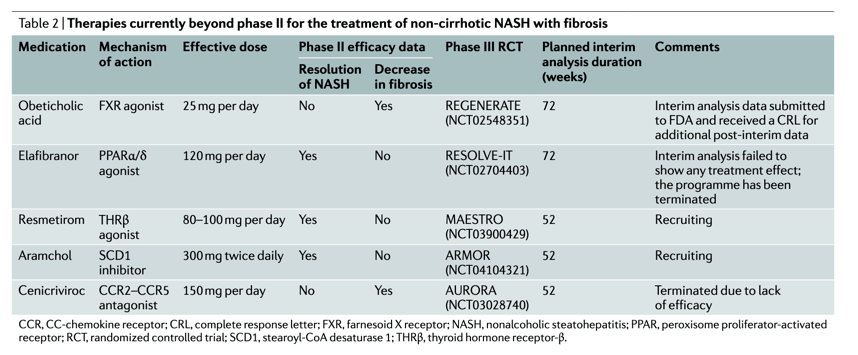
In Phase 3 now:
Aramchol in NASH Phase 3; Expanded Access - (06/01/22)
Positive Topline Phase 3 MAESTRO-NAFLD-1 Data Demonstrate Resmetirom was Safe, Well-Tolerated and Provided Statistically Significant Improvements in Key Measures of Liver and Cardiovascular Health - Expanded Access Program - (06/01/22)
Abstract
Non-alcoholic fatty liver disease (NAFLD) has emerged as the most prevalent liver disease in the world, yet there are still no approved pharmacological therapies to prevent or treat this condition. NAFLD encompasses a spectrum of severity, ranging from simple steatosis to non-alcoholic steatohepatitis (NASH). Although NASH is linked to an increased risk of hepatocellular carcinoma and cirrhosis and has now become the leading cause of liver failure-related transplantation, the majority of patients with NASH will ultimately die as a result of complications of type 2 diabetes mellitus (T2DM) and cardiometabolic diseases. Importantly, NAFLD is closely linked to obesity and tightly interrelated with insulin resistance and T2DM. Thus, targeting these interconnected conditions and taking a holistic attitude to the treatment of metabolic disease could prove to be a very beneficial approach. This Review will explore the latest relevant literature and discuss the ongoing therapeutic options for NAFLD focused on targeting intermediary metabolism, insulin resistance and T2DM to remedy the global health burden of these diseases.
Introduction
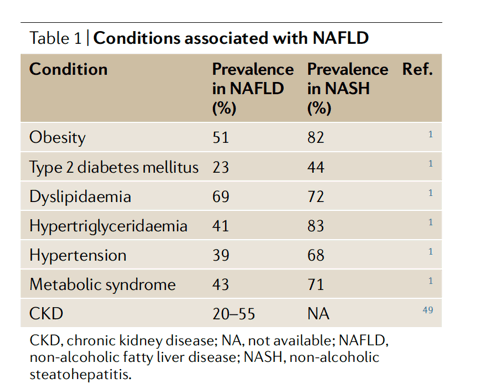
Non-alcoholic fatty liver disease (NAFLD) is defined as ectopic lipid accumulation in the liver in the absence of excessive alcohol intake or other attributable cause; 25% of the world's population might have NAFLD and direct costs are estimated at US$100 billion annually in the USA alone1,2. NAFLD is tightly linked to obesity and, while diet and exercise have proven to be effective in the treatment of NAFLD3, the long-term sustainability of these interventions is poor. Furthermore, there is no licensed drug therapy for non-alcoholic steatohepatitis (NASH) and there is a critical need for the development of effective treatments for this global health problem.
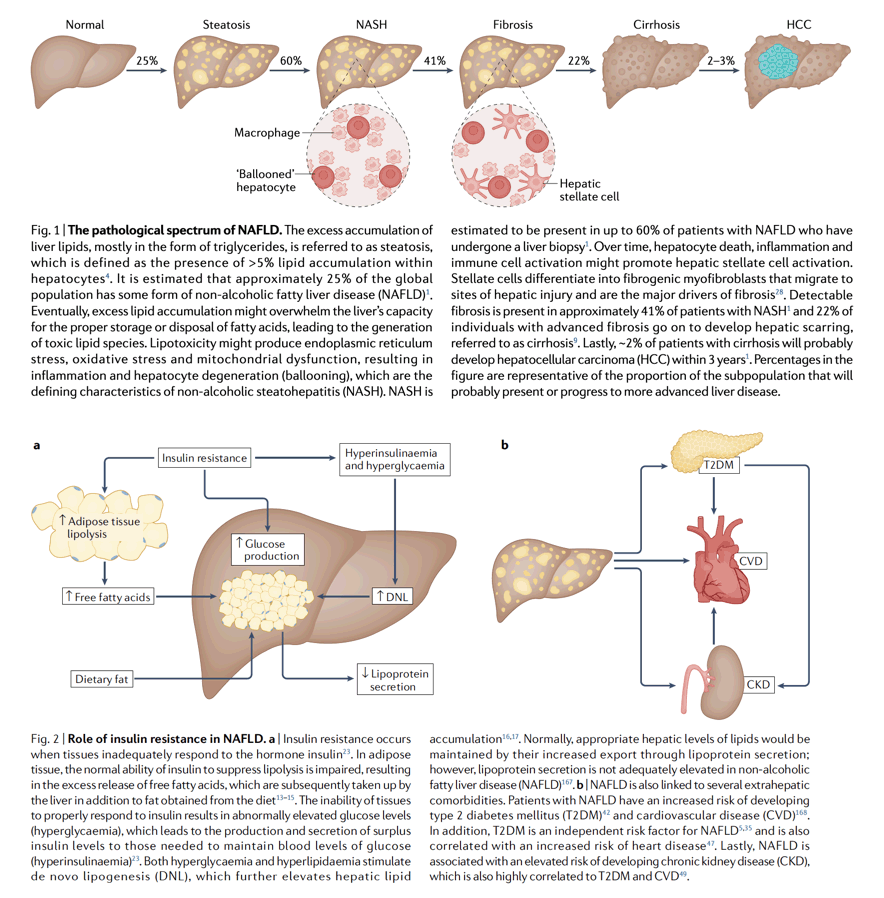
NAFLD encompasses a spectrum of disease severity (Fig. 1) ranging from simple steatosis to more advanced disease characterized by hepatocyte death, inflammation and the development of fibrotic lesions (NASH). Simple steatosis is characterized by lipid accumulation in hepatocytes with minimal hepatocellular injury but is associated with an increased risk of other metabolic disorders, including insulin resistance, type 2 diabetes mellitus (T2DM), dyslipidaemia and hypertension4,5. Epidemiological studies show that NAFLD is more prevalent in men than in premenopausal women6 and premenopausal women are less likely to develop fibrosis than men7,8. By contrast, the protective effect of the female sex is not observed after menopause. It is estimated that NASH is present in ∼60% of patients with NAFLD who undergo a liver biopsy and 41% of patients with NASH exhibit considerable fibrosis1. In patients with advanced fibrosis, ∼22% go on to develop cirrhosis and ∼2% of patients with cirrhosis develop hepatocellular carcinoma (HCC) within 3 years1,9 (Fig. 1). HCC and cirrhotic liver failure can only be cured with an extreme treatment - liver transplantation. Liver disease secondary to NASH has become a leading cause for liver transplantation in the USA due to increasing rates of obesity-related NASH and the increasing availability of alternative curative therapies for other diseases, such as hepatitis C virus infection10,11. Unfortunately, most patients with liver failure will ultimately not receive a transplant and will die while waiting for a donor organ12. Further, the majority of patients with NASH will die from cardiometabolic disease rather than from a liver-related cause due to the tight relationship between NAFLD and T2DM. Thus, therapeutics that target NAFLD, T2DM and cardiometabolic risk factors might be the most effective treatment.
Thiazolidinedione insulin sensitizers
Pioglitazone and rosiglitazone treat T2DM by sensitizing the body to the effects of insulin and are identifiable by their thiazolidinedione ring. Pioglitazone and rosiglitazone are potent activators of the nuclear receptor PPARγ, which is most highly expressed in adipose tissue and has a critical role in adipocyte differentiation and lipid and glucose metabolism as well as in suppressing inflammation69. Thiazolidinediones probably improve peripheral insulin sensitivity by stimulating the release of adipokines, promoting triglyceride storage in adipose tissue and enhancing the suppressive action of insulin on lipolysis, resulting in reduced plasma levels of free fatty acids and decreased hepatic lipid accretion70. Additionally, thiazolidinedione treatment directly reduces hepatic stellate cell activation and fibrosis in rats71. Thus, thiazolidinediones might improve hepatic and peripheral insulin sensitivity to attenuate NASH and might also have direct effects on hepatic pathophysiology. However, the use of thiazolidinediones in people is now limited by PPARγ-driven adverse effects, including weight gain, oedema and the risk of bone fracture72. In addition, a meta-analysis published in 2007 found that rosiglitazone use was associated with an increased risk of myocardial infarction and cardiovascular death compared with placebo73, resulting in a black-box warning and restriction of rosiglitazone use by the FDA. However, the warning and restriction were later removed after additional studies failed to replicate the findings regarding cardiovascular risks74. Nonetheless, at present, rosiglitazone is used very rarely to treat patients with T2DM.
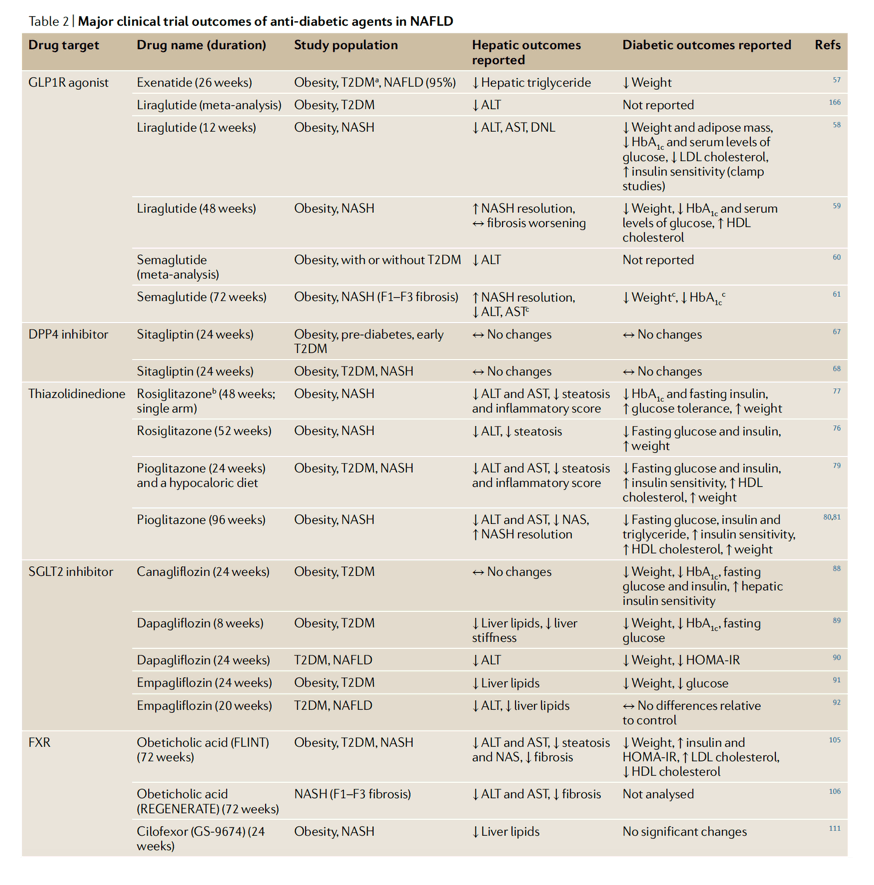
Of the two approved thiazolidinediones, rosiglitazone is the most potent activator of PPARγ75. Studies have demonstrated that patients with NASH receiving rosiglitazone had enhanced insulin sensitivity and reduced hepatic steatosis; however, considerable weight gain and oedema in the lower extremities were reported (Table 2)76,77. As the clinical use of rosiglitazone as an insulin sensitizer has largely been discontinued, there has been very little further evaluation of the drug for the treatment of NASH subsequent to the studies conducted almost 15 years ago. Pioglitazone is also an effective insulin sensitizer but is a less potent PPARγ agonist and is associated with fewer adverse effects than rosiglitazone75,78. Treatment with pioglitazone in patients with T2DM and NASH resulted in improved insulin sensitivity and reduced inflammation and hepatocyte degeneration as well as in reduced fibrosis relative to pretreatment measurements, yet there was no difference in the resolution of fibrosis compared with the placebo group79. Additionally, patients with NASH but no T2DM receiving pioglitazone had improved fasting glucose levels and a greater resolution of NASH, though with no improvement in fibrosis, and increased weight gain versus patients receiving placebo80,81. A meta-analysis of randomized controlled trials using the thiazolidinediones, either pioglitazone or rosiglitazone, demonstrated that thiazolidinedione treatment led to improved liver histology, including reduced steatosis, inflammation and degeneration82. However, a statistically significant decrease in fibrosis was only seen in studies using pioglitazone versus placebo, suggesting that pioglitazone might be more efficacious than rosiglitazone for the resolution of fibrosis. Further examination demonstrated that responders to pioglitazone had increased plasma concentrations of pioglitazone83 and genetic analysis identified a variant of CYP2C8 (the gene that encodes the predominant pioglitazone-metabolizing enzyme) that was associated with fibrosis score84. Collectively, these studies indicate the usefulness of pioglitazone in the resolution of NASH and highlight the importance of pharmacogenetics, which can drastically alter drug metabolism and response to treatment.
Given the greater efficacy of pioglitazone than rosiglitazone, despite a markedly lower affinity for PPARγ, it seems reasonable to explore whether the therapeutic pharmacology of thiazolidinediones might not be entirely dependent on PPARγ activation. Indeed, other molecular targets of thiazolidinediones have been identified85 and one will be discussed in greater detail in subsequent sections.
SGLT2 inhibitors
SGLT2 is a sodium-dependent glucose transporter primarily expressed in the proximal tubule epithelium of the kidney and is responsible for the majority (>90%) of filtered glucose reabsorption86. Inhibitors of SGLT2 (canagliflozin, dapagliflozin, empagliflozin and ertugliflozin) lead to the increased urinary excretion of glucose and are approved anti-hyperglycaemic agents for T2DM. In addition, SGLT2 inhibitors induce weight loss in many people and reduce the risk of major cardiovascular events86. In a mouse model of T2DM, SGLT2 inhibition significantly reduced levels of liver enzymes, steatosis, hepatocyte damage and fibrosis87.
Several trials have tested the efficacy of SGLT2 inhibitors in human NAFLD and T2DM. Patients treated with either canagliflozin, dapagliflozin or empagliflozin showed reduced hyperglycaemia and improvements in hepatic lipid content, liver enzymes and liver stiffness (Table 2)88,89,90,91,92. Notably, as with GLP1R agonists, SGLT2 inhibitors caused weight loss, which strongly correlated with the decrease in hepatic lipid content88. However, a large retrospective study comparing canagliflozin, dapagliflozin, liraglutide or sitagliptin added to previous T2DM treatment (insulin, metformin or sulfonylurea), demonstrated that only the SGLT2 inhibitors canagliflozin and dapagliflozin resulted in significantly improved levels of liver enzymes independently of body-weight loss and HbA1c (ref.93). As with GLP1R, SLGT2 is not expressed in the liver86 and treatment-induced weight loss or metabolic improvements might indirectly result in reduced liver lipid content. However, SGLT2 inhibitor use is associated with an increased risk of lower limb amputation and diabetic ketoacidosis compared with GLP1R agonist treatment94. Overall, SGLT2 inhibitors are effective in managing glycaemic control and lowering hepatic lipid content but histological analyses are needed to evaluate their usefulness in NASH.
Weight gain and peripheral edema were reported commonly with pioglitazone and lanifibranor-side effects attributed to the PPAR-γ effects of these agents. Increased risk of cardiovascular events and bladder cancer were reported with pioglitazone, whereas reversible increase in serum creatinine was reported with elafibranor.
Saroglitazar magnesium, a dual PPAR-α/γ agonist, was designed to have a weaker PPAR-γ effect to reduce untoward side effects related to PPAR-γ agonism.(22) Through its PPAR-α agonism, saroglitazar increases hepatic oxidation of fatty acids, lowers synthesis and secretion of triglycerides (TGs), and produces favorable changes in circulating lipoproteins. Through its PPAR-γ agonism, saroglitazar regulates transcription of insulin-responsive genes, increases insulin sensitivity, and reduces blood glucose and glycosylated hemoglobin A1c (HbA1c) levels.(23) Saroglitazar was granted marketing authorization in India in 2013 for management of diabetic dyslipidemia and hypertriglyceridemia in those with T2DM not controlled by a statin alone.
In mice with choline-deficient high-fat diet or Western diet-induced NASH,(24, 25) saroglitazar significantly decreased alanine aminotransferase (ALT) and improved hepatic steatosis, hepatocellular ballooning, and lobular inflammation. These changes were accompanied by a decrease in expression of fibrosis and inflammation biomarkers. Saroglitazar was also associated with reduction in homeostasis model assessment-insulin resistance (HOMA-IR), TGs, total cholesterol, and metabolically active lipid species, including diglycerides, ceramides, and sphingomyelins, in mice with Western diet-induced NASH.(25)
Experimental PPAR agonists
The PPAR family of nuclear receptor transcription factors (PPARα, PPARδ and PPARγ) are characterized by large, promiscuous ligand-binding pockets and are known to regulate numerous aspects of metabolism through gene transcription. Whereas PPARγ is adipocyte enriched and tends to regulate lipid storage, PPARα and PPARδ are expressed most highly in oxidative tissues and regulate genes encoding enzymes involved in mitochondrial biogenesis and metabolism, fatty acid oxidation, ketogenesis, fatty acid uptake, and triglyceride turnover21. Numerous natural and synthetic PPAR agonists have been studied for therapeutic efficacy, including agonists that can activate two or three PPAR isoforms21.
Elafibranor (GFT505), a dual PPARα-PPARδ agonist, reduced hepatic steatosis, inflammation and fibrosis in both mouse and rat models of NAFLD113. Patients with obesity who were treated with elafibranor had reduced levels of liver enzymes and improved insulin sensitivity114. In a phase IIb clinical trial (GOLDEN-505), elafibranor promoted moderate resolution of NASH; however, some patients developed elevated serum levels of creatinine and renal impairment115. A larger phase III trial is under way but interim results showed no statistically significant improvement in histological NASH endpoints compared with placebo116. The use of lanifibranor (IVA337), a pan-PPAR agonist, improved glucose metabolism, steatosis and hepatocyte injury in multiple mouse models of NASH117. A phase II trial might demonstrate that lanifibranor was effective in promoting the resolution of NASH with improved fibrosis in patients with T2DM and NASH118; however, the peer-reviewed publication for this work is yet to be published. A dual PPARα/γ agonist, saroglitazar, reduced hepatic steatosis and inflammation and prevented fibrosis in mice119 and improved insulin sensitivity in patients with T2DM120. Trials in patients with NASH are ongoing (NCT03061721 and NCT03863574). Collectively, experimental PPAR agonists demonstrate some efficacy in NAFLD but their use might be hobbled by adverse effects attributable to PPARγ and PPARδ activation.
Conclusions
NAFLD is the most common form of liver disease yet there are no drugs licensed for its treatment. Due to the close association between NAFLD and T2DM, many agents that are currently prescribed for hyperglycaemia have yielded positive results on NASH biomarkers. Experimental agents that target aspects of intermediary metabolism have also proven beneficial to varying degrees but adverse effects might limit their use. The overall benefit of metabolic-targeted therapies for NAFLD and NASH is attractive as these drugs might also reduce other cardiometabolic risk factors that contribute to CVD and complications of T2DM, which are the leading cause of mortality in patients with NAFLD and NASH.
The treatment of patients with T2DM with either exenatide, liraglutide or semaglutide has demonstrated efficacy in reducing hepatic lipid content as well as levels of liver enzymes and inflammatory markers, an effect associated with improved HbA1c levels and body-weight loss (Table 2)57,58,59,60. Furthermore, compared with control individuals given placebo, a greater percentage of patients with NASH who were treated with semaglutide achieved resolution of NASH with no worsening of fibrosis61. Additionally, semaglutide is being tested in patients with NASH and compensated cirrhosis (NCT03987451) to determine its efficacy in the reduction of fibrosis score without a worsening of NASH.
CVD - the leading cause of mortality in patients with NAFLD - a loss of body weight is also effective in resolving the features of NASH3.
In addition to CVD-related macrovascular complications, patients with NAFLD are at increased risk of developing microvascular disease, particularly chronic kidney disease, which is also highly associated with CVD and T2DM. An increased histological severity of NAFLD correlates with progressively lower renal function, which is independent of other comorbidities, including T2DM, hypertension, dyslipidaemia and adiposity49. Patients with NASH who had improvements in fibrosis and/or a resolution of NASH due to lifestyle interventions also had a statistically significant increase in renal function50.
In the past few years, the term 'metabolic-associated fatty liver disease' has been proposed to more accurately describe patients who have liver disease coincident with metabolic dysfunction. For example, a patient with hepatic steatosis in combination with obesity and/or T2DM or an individual with a normal BMI who has at least two metabolic risk factors51. Although not yet universally accepted, this new terminology seeks to include a larger population of patients than the term NAFLD, who probably share many underlying and possibly undiagnosed comorbidities, to help expand the collaboration between hepatologists and diabetologists to advance growth in our understanding and treatment of this population of patients51,52,53. Due to the interplay between NAFLD, NASH and T2DM, it is likely that targeting insulin sensitivity and hyperglycaemia and adopting a holistic attitude towards the treatment of metabolic disease in patients with NAFLD might prove advantageous.
In addition to CVD-related macrovascular complications, patients with NAFLD are at increased risk of developing microvascular disease, particularly chronic kidney disease, which is also highly associated with CVD and T2DM. An increased histological severity of NAFLD correlates with progressively lower renal function, which is independent of other comorbidities, including T2DM, hypertension, dyslipidaemia and adiposity49. Patients with NASH who had improvements in fibrosis and/or a resolution of NASH due to lifestyle interventions also had a statistically significant increase in renal function50.
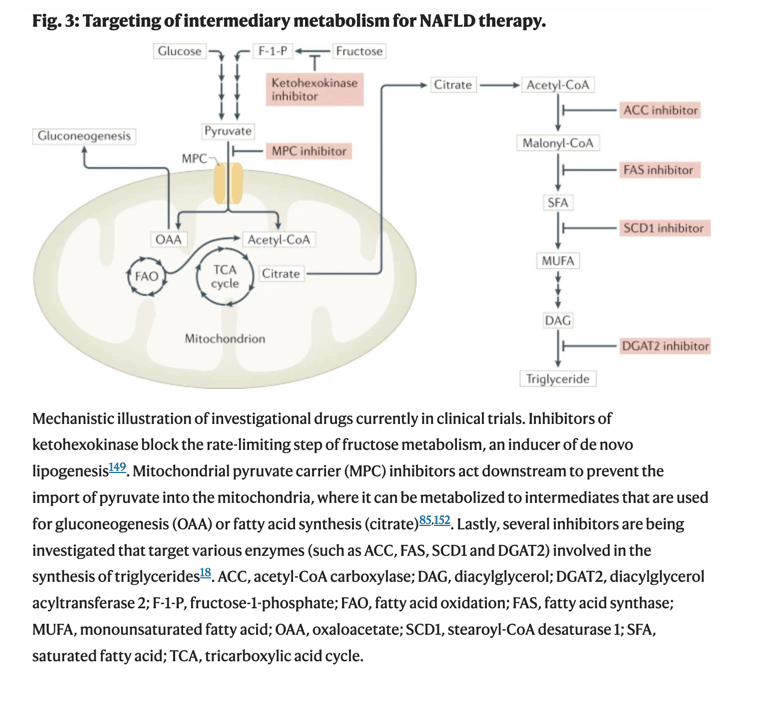
Although impairments in the mitochondrial metabolism of fatty acids could also contribute to lipid accumulation, mitochondrial dysfunction seems to happen only in the later stages of NASH progression19. Nevertheless, compounds that stimulate mitochondrial oxidative metabolism, including thyroid hormone receptor agonists20, ligands for nuclear receptors that control the expression of mitochondrial genes21 and inhibitors of mitochondrial pyruvate import22, have shown efficacy in the treatment of NASH.
The pathological spectrum of NAFLD. The excess accumulation of liver lipids, mostly in the form of triglycerides, is referred to as steatosis, which is defined as the presence of > 5% lipid accumulation within hepatocytes4. It is estimated that approximately 25% of the global population has some form of non-alcoholic fatty liver disease (NAFLD)1. Eventually, excess lipid accumulation might overwhelm the liver's capacity for the proper storage or disposal of fatty acids, leading to the generation of toxic lipid species. Lipotoxicity might produce endoplasmic reticulum stress, oxidative stress and mitochondrial dysfunction, resulting in inflammation and hepatocyte degeneration (ballooning), which are the defining characteristics of non-alcoholic steatohepatitis (NASH). NASH is estimated to be present in up to 60% of patients with NAFLD who have undergone a liver biopsy1. Over time, hepatocyte death, inflammation and immune cell activation might promote hepatic stellate cell activation. Stellate cells differentiate into fibrogenic myofibroblasts that migrate to sites of hepatic injury and are the major drivers of fibrosis28. Detectable fibrosis is present in approximately 41% of patients with NASH1 and 22% ofindividuals with advanced fibrosis go on to develop hepatic scarring, referred to as cirrhosis9. Lastly, ∼2% of patients with cirrhosis will probably develop hepatocellular carcinoma (HCC) within 3 years1. Percentages in the figure are representative of the proportion of the subpopulation that will probably present or progress to more advanced liver disease.
| |
| |
| |
|
|
|