| |
The 'Viennese epidemic' of acute HCV
in the era of direct-acting antivirals
|
| |
| |
Download the PDF here
11 March 2022
David Chromy1,2,3| David J. M. Bauer1,2| Benedikt Simbrunner1,2|Matthias Jachs1,2| Lukas Hartl1,2| Philipp Schwabl1,2| Caroline Schwarz1,2,4|Armin Rieger2,3| Katharina Grabmeier-Pfistershammer2,5| Michael Trauner1,2|Peter Ferenci1| Mattias Mandorfer1,2| Michael Gschwantler2,4| Thomas Reiberger1,2
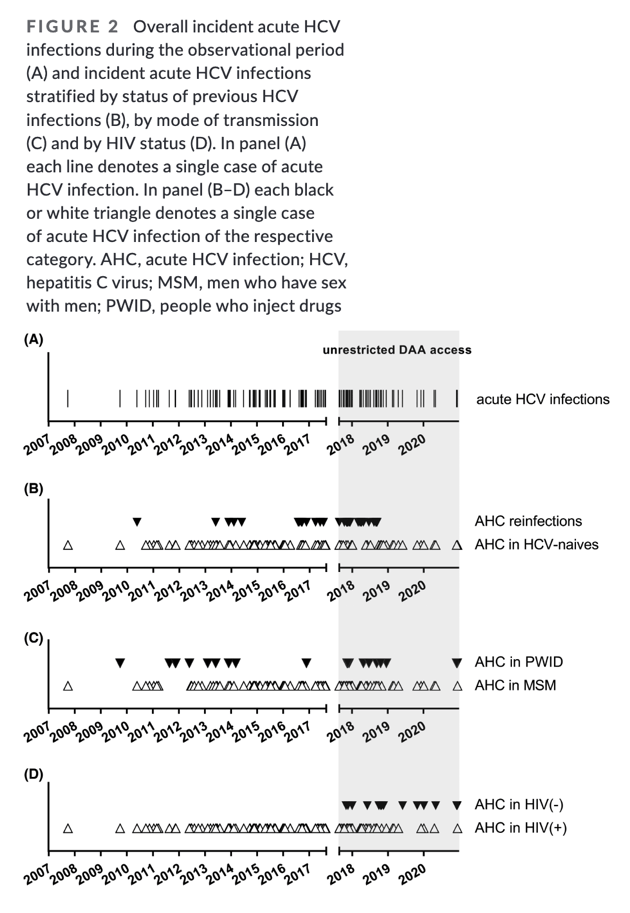
We observed a consistent rise in the numbers of AHC infections - mostly in HIV+ MSM - in Vienna throughout the 13 years (2007–2020) included the study period, with a further aggravation after DAAs became accessible and HIV-negative MSM being increasingly affected. Importantly, we also found a high HCV reinfection rate of 11% during a median follow-up of 1.39 years after HCV clearance/SVR in the DAA era. These findings clearly indicate that Vienna was and remains affected by the ongoing epidemic of AHC infections among HIV+ and HIV-negative MSM.
Another typical marker for increased risk for HCV transmission is positive HIV status.35 However, increasing rollout of PrEP in the recent years may has shifted this paradigm. As PrEP enables sufficient protection against HIV infection,36 individuals engaging in high-risk sex practices likely maintain their HIV-negative status and-in some cases-even over-compensate by scaling their risk behaviour further up.13 A recent meta-analysis by Ong et al.37 on STIs among PrEP-users reported not only extremely high rates of chlamydia and gonorrhoea, but also an HCV prevalence of 2% at PrEP-initiation. In our data, we also noted an increase in acute HCV infections among HIV-negative individuals. Fourteen AHC cases in HIV-negative occurred exclusively in the DAA era, and 56% of the affected MSM were using PrEP. In 2021, PrEP is still not fully covered by the healthcare providers in Austria, and thus, PrEP rollout is strongly hampered in our country.38 Nevertheless, recent HIV-negative cases may reflect the internationally observed shift of the population at risk from HIV+ MSM to HIV-negative MSM on PrEP.11 Fortunately, regular STI screening-including HCV testing-is mandated during PrEP use; hence, PrEP-care might also allow sufficient and regular HCV screening in MSM practicing high-risk behaviour.39
Abstract
The recently reported epidemic of acute hepatitis C virus (HCV) infections -observed predominantly among men who have sex with men (MSM)-may now decline due to wide availability of direct-acting antivirals (DAAs). This study aimed to investigate the current trends of acute hepatitis C in Vienna. Patients presenting with acute hepatitis C between 01/2007 and12/2020 at the Vienna General Hospital were retrospectively enrolled and followed after virologic clearance/eradication. The introduction of unrestricted DAA access after 09/17 defined the 'DAA era', as compared to the 'pre-DAA era' prior to 09/17.
We identified 134 acute hepatitis C cases in 119 patients with a mean age of 39 ± 9 years at inclusion.
The majority of patients were male (92%), HIV-positive (88%) and MSM (85%).
In the DAA era, a history of prior chronic HCV infection at inclusion was found in 24% (11/46) compared to 7% (5/73) in the pre-DAA era (p = .012).
The annual rate of acute hepatitis C cases increased in the DAA era (17.11 per year) compared to the pre-DAA era (7.76 per year). The DAA era included an AHC-genotype-2 cluster and more HIV-negative acute hepatitis C cases (0% (0/73) vs. 30% (14/46), p < .001).
Patients were followed after spontaneous clearance or sustained virologic treatment response (SVR) for a total of 251.88 patient-years (median 1.39 years per patient).
In the DAA era, we recorded 15 acute hepatitis C-reinfections - corresponding to an incidence rate of 5.96 (95% CI: 3.57–9.66) reinfections per 100-patient-years. We continue to observe a high incidence of acute hepatitis C in Vienna in the DAA era-primarily among HIV-positive MSM, but increasingly also in HIV-negative MSM.
During follow-up, we observed 15 acute HCV reinfections in 9% (13/114) of patients whereas one individual presented only with chronic HCV infection. The majority of reinfections during follow-up occurred in MSM (77%, 10/13), including the two individuals with a documented second reinfection.
Interestingly, cases of AHC infection among HIV-negative individuals were exclusively seen in the DAA era: While in the pre-DAA era, all AHC cases (100%, 73/73) were HIV-coinfected, the rate of AHC-HIV coinfection dropped to 70% (32/46; p < .001) once DAAs were readily reimbursable. Nine of the 14 cases among HIV-negative patients were MSM and 56% (5/9) were using PrEP.
| |
| |
| |
|
|
|