| |
Long-term HIV Pre-exposure Prophylaxis Trajectories
Among Racial & Ethnic Minority Patients: Short, Declining, & Sustained Adherence
|
| |
| |
Download the PDF here
Pyra, Maria MPH, PhDa,b; Brewer, Russell MPH, DrPHb; Rusie, Laura MSca; Kline, Jeanelle MSWa; Willis, India MSN MPH FNP-BCa; Schneider, John MD, MPHa,b
JAIDS Feb 2022
Abstract
Background:
HIV pre-exposure prophylaxis (PrEP) requires continued use at an effective dosage to reduce HIV incidence. Data suggest early PrEP drop-off among many populations. We sought to describe PrEP use over the first year among racial and ethnic minority patients in the US.
Setting:
Racial and ethnic minority patients initiating PrEP at a federally qualified health center in Chicago, IL.
Methods:
Using electronic health records, we determined the adherence (≥6 weekly doses) trajectories over the first year of PrEP use and compared baseline and time-varying patient characteristics.
We included electronic health record (EHR) data from all Howard Brown Health (HBH) patients who started PrEP 2015–2018 and self-identified as Latinx, Asian, or Black. HBH is a large, federally qualified health center with locations in diverse community areas within Chicago, IL, specializing in sexual health, particularly among sexual and gender minorities.
Results:
From 2159 patients, we identified 3 PrEP use trajectories.
Sustained use was the most common (40%) trajectory, followed by short use (30%) and declining use (29%).
In adjusted models, younger age, Black race, as well as gender, sexual orientation, insurance status at baseline, and neighborhood were associated with trajectory assignment; within some trajectories, insurance status during follow-up was associated with odds of monthly adherence (≥6 weekly doses).
Conclusion:
Among racial and ethnic minorities, a plurality achieved sustained PrEP persistence. Access to clinics, insurance, and intersectional stigmas may be modifiable barriers to effective PrEP persistence; in addition, focus on younger users and beyond gay, cismale populations are needed.
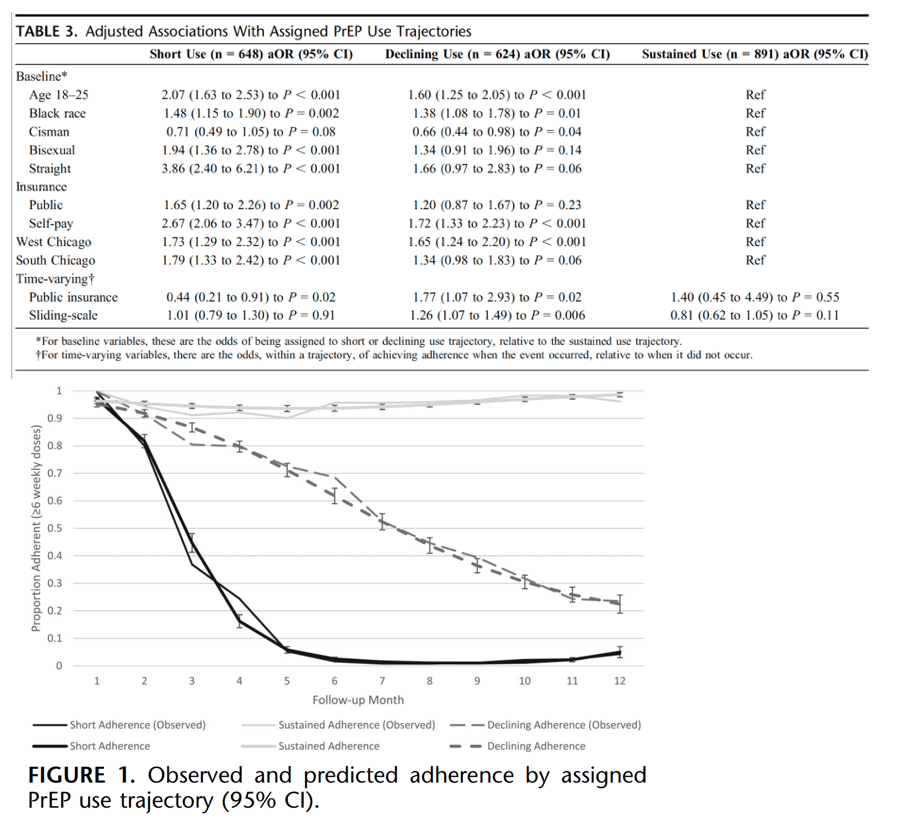
In the final model (Table 3), younger age (18–25) was associated with increase odds of being assigned to the short PrEP use vs sustained PrEP use trajectory {aOR 2.07, 95% confidence interval (CI): [1.63 to 2.63]} and declining vs sustained PrEP use trajectory [aOR 1.60, 95% CI: (1.25 to 2.05)]. Black race was associated with increased odds of short or declining PrEP use vs sustained PrEP use trajectory [aOR 1.48, 95% CI: (1.15 to 1.90); aOR 1.38, 95% CI: (1.08 to 1.78) respectively]. Cismen had lower odds of short or declining PrEP use trajectories, relative to sustained use [aOR 0.71, 95% CI: (0.49 to 1.05); aOR 0.66, 95% CI: (0.44 to 0.98)]. Both bisexual and straight sexual orientations were associated with higher odds of short vs sustained PrEP use trajectories [aOR 1.94, 95% CI: (1.36 to 2.78); aOR 3.86, 95% CI: (2.40 to 6.21), respectively]. Public insurance and self-pay at baseline were associated with increased odds of short vs sustained PrEP use trajectories [aOR 1.65, 95% CI: (1.20 to 2.26); aOR 2.67, 95% CI: (2.06 to 3.47), respectively]; self-pay was also associated with lower odds of declining PrEP use vs sustained [aOR 1.73, 95% CI: (1.29 to 2.32)]. West and Southside residence increased odds of short PrEP use vs sustained trajectories [aOR 1.73, 95% CI: (1.29 to 2.32); aOR 1.79, 95% CI: (1.33 to 2.42), respectively]; Westside was also associated with short vs sustained PrEP use trajectories. During follow-up, among the short PrEP use group, public insurance use decreased odds of adherence [aOR 0.44, 95% CI: (0.21 to 0.91)], whereas public insurance increased the odds of adherence among the declining trajectory [aOR 1.77, 95% CI: (1.07 to 2.93)]. Sliding-scale use (a specific subset of self-pay) was also associated with increase adherence among the short PrEP use group only, aOR 1.26, 95% CI: (1.07 to 1.49). Results were similar when the lower adherence threshold (average ≥4 weekly doses per month) was used.
|
|
| |
| |
|
|
|