| |
Fall & Frailty Increase Mortality in Older PLWH - Frailty Assessments In Routine Care
|
| |
| |
Download the PDF here
Middle-aged HIV-infected adults have high fall risk. Multiple comorbidities, medications, and functional impairment were predictive of falls, but surrogate markers of HIV infection or an HIV-specific multimorbidity index were not. Fall risk should be assessed routinely as part of the care of HIV-infected persons.
With increasing age, however, many PWH experience an increased burden of some comorbidities and impairments including difficulties with balance, slow gait, weakness, and cognitive impairment 4-6. The increased burden of comorbidities, combined with physical and cognitive impairments has contributed to a higher prevalence of falls in PWH compared to demographically similar HIV-uninfected adults 7-9.
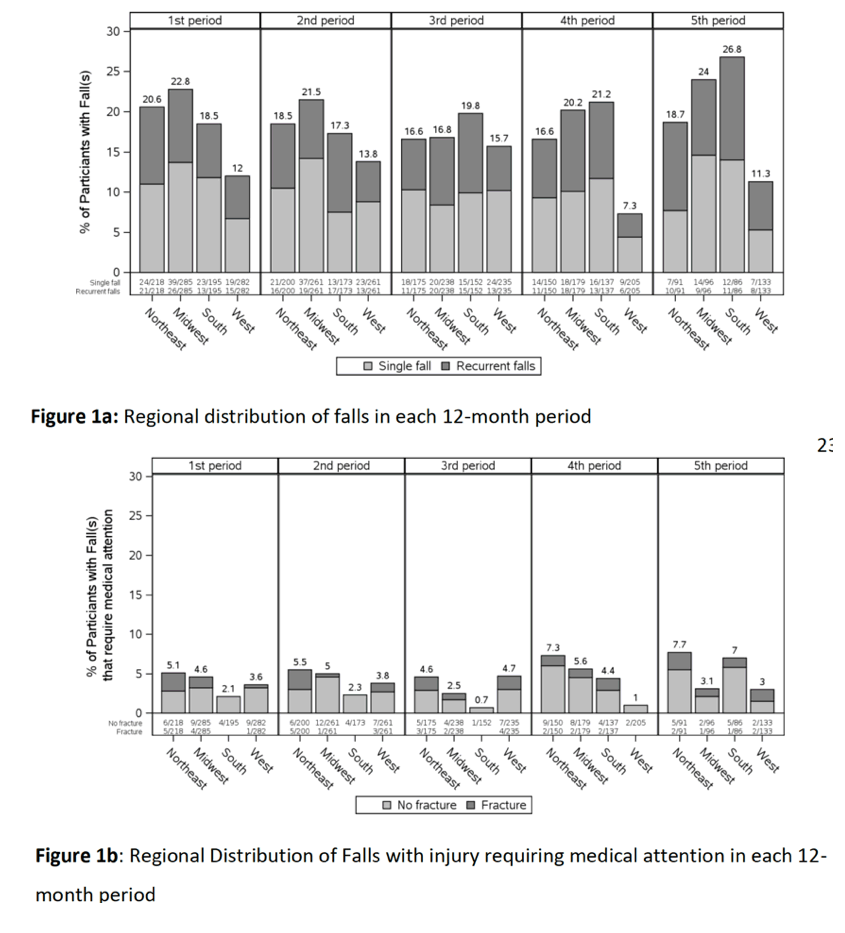
We found significant differences in the risk of recurrent falls across U.S. geographic regions among older PWH, despite accounting for numerous fall risk factors, with higher odds of recurrent falls among PWH in the Midwestern and Southern region compared to those in the Western region.
Falls are a major cause of mortality and morbidity globally, with fall-related injuries increasing with age. Every year in the U.S., one in four older adults (65+) has a fall, resulting in over 800,000 fall-related hospitalizations and more than 27,000 fall-related deaths 10. Risk factors for falls among older adults include age, medications and comorbidities, gait and balance disorders, functional impairment, and cognitive impairment 11,12. Among PWH, HIV-related risk factors including ART, toxicity of prior ART, and HIV-1 replication may further contribute 13,14.
ACTG - Frailty is an independent risk factor for mortality, cardiovascular disease, bone disease and
diabetes among aging adults with HIV
Baseline frailty was associated with multiple adverse health outcomes (incident
CVD, DM and bone disease), while increase in frailty score was associated with mortality among
PWH engaged in care. Incorporation of frailty assessments into the routine care of PWH may
assist in improvement of functional status and risk stratification for age-related chronic diseases.
Frailty and the Risk of Falls in HIV-Infected Older Adults in the ACTG A5322 Study
49% who were frail had a fall; 21% who were pre-frail had a fall; and, 12% who were not frail had a fall.
---------------------------------
Risk Factors for Falls in HIV-Infected Persons
Background: The incidence of and risk factors for falls in HIV-1-infected persons are unknown.
Methods: Fall history during the prior 12 months, medical diagnoses, and functional assessments were collected on HIV-infected persons 45-65 years of age receiving effective antiretroviral therapy. Fall risk was evaluated using univariate and multivariate regression analyses.
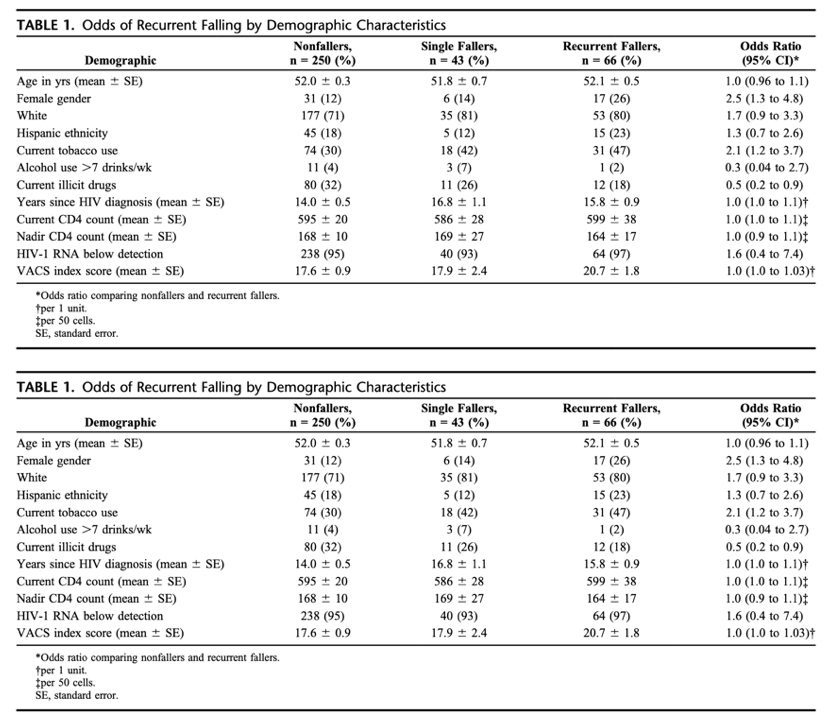
Results: Of 359 subjects, 250 persons (70%) reported no falls, 109 (30%) had >/=1 fall; and 66 (18%) were recurrent fallers. Females, whites, and smokers were more likely to be recurrent fallers (P /= 0.09); didanosine recipients were more likely to be recurrent fallers (P = 0.04).
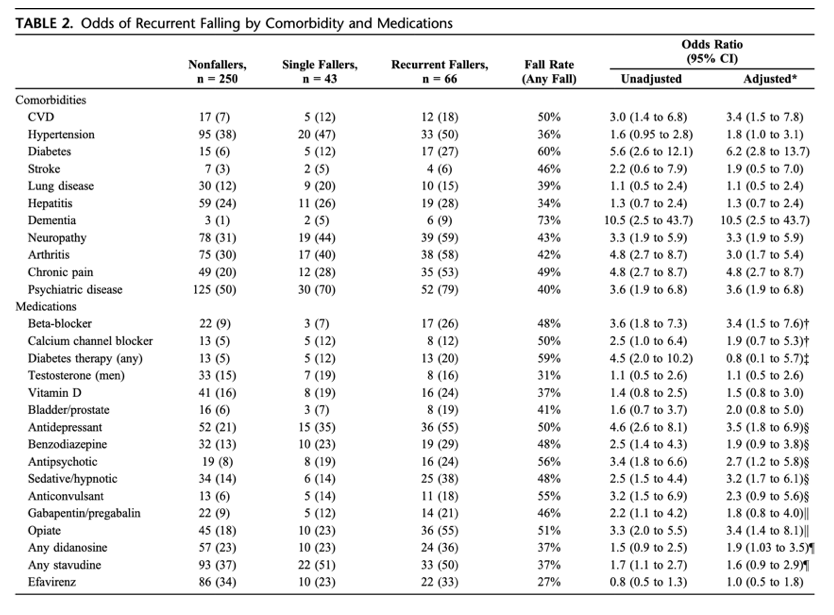
The odds of falling increased 1.7 for each comorbidity and 1.4 for each medication (P < 0.001) and were higher in persons with cardiovascular disease, hypertension, dementia, neuropathy, arthritis, chronic pain, psychiatric disease, frailty, or disability [all odds ratio (OR) >/= 1.8; P
Beta-blockers, antidepressants, antipsychotics, sedatives, and opiates were independently associated with falling (all OR >/= 2.7; P
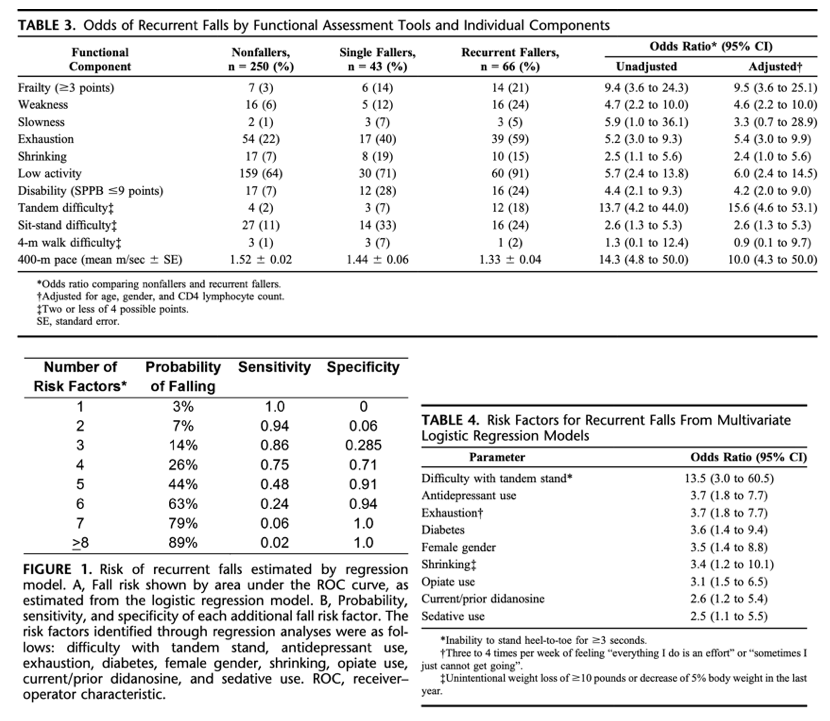
Female gender, diabetes, antidepressants, sedatives, opiates, didanosine, exhaustion, weight loss, and difficulty with balance were the most significant predictors of falls in logistic regression (all OR > 2.5; P
Conclusions: Middle-aged HIV-infected adults have high fall risk. Multiple comorbidities, medications, and functional impairment were predictive of falls, but surrogate markers of HIV infection or an HIV-specific multimorbidity index were not. Fall risk should be assessed routinely as part of the care of HIV-infected persons.
Polypharmacy was associated with increased odds of falls, with each additional prescribed medication associated
with an incremental increase of 1.4 in the odds of falls (CI: 1.3 to 1.6; P <0.001).
In functional assessments, both frailty and disability were associated with falls (P< 0.001
------------------------

Mona Abdo1, Xingye Wu2, Anjali Sharma3, Katherine K. Tassiopoulos4, Todd T. Brown5, Susan L. Koletar6, Michael T. Yin7, Kristine M. Erlandson8, for the ACTG A5322 Study Team.
Abstract
Background: We examined regional variation in falls in a geographically diverse cohort of older people with HIV (PWH), and explored whether physical activity, sex, or BMI modified these associations.
Setting: PWH enrolled in ACTG A5322 HAILO (HIV Infection, Aging and Immune Function Long-Term Observational Study). Methods: Participants who reported falls in the 6 months prior to each semiannual visit with ≥1 consecutive pair of falls assessments were included. We examined associations between geographic region with recurrent falls (≥2) over each 12-month period using repeated measures multinomial logistic regression models, and assessed effect modification by adding an interaction term between geographic region and each potential effect modifier.
Results: A total of 788 men and 192 women with median age at study entry of 51 years contributed up to 240 weeks of data. U.S. region included Northeast (22%), Midwest (29%), South (20%), and West (29%).
In multivariable analyses, compared to Western region, greater risk was seen among Midwestern region (OR=2.35[95% CI=1.29,4.28]) and Southern region (2.09[1.09,4.01]). Among those with higher physical activity, Midwestern region had higher odds of recurrent falls than Western region. Among obese individuals, Southern region had higher odds of recurrent falls than Western region. Sex did not modify the association between region and recurrent falls.
Conclusion: Fall risk varied by geographic region and associations between geographic region and recurrent falls appeared to be modified by physical activity and obesity. This may help identify subgroups of older PWH for targeted falls screening/interventions.
Education level, health insurance, smoking status, current substance use, physical activity, average NPZ-4, neurocognitive impairment, and prescription opioid use changed the age-adjusted model effect estimate by more than 10% and were included in the multivariable model, with one exception; due to collinearity, NPZ-4 but not neurocognitive impairment was included in the multivariable model.
Introduction
Antiretroviral therapy (ART) has been effective in extending survival and narrowing the gap in life expectancy between people with HIV (PWH) and HIV-uninfected individuals 1-3
With increasing age, however, many PWH experience an increased burden of some comorbidities and impairments including difficulties with balance, slow gait, weakness, and cognitive impairment 4-6. The increased burden of comorbidities, combined with physical and cognitive impairments has contributed to a higher prevalence of falls in PWH compared to demographically similar HIV-uninfected adults 7-9.
Falls are a major cause of mortality and morbidity globally, with fall-related injuries increasing with age. Every year in the U.S., one in four older adults (65+) has a fall, resulting in over 800,000 fall-related hospitalizations and more than 27,000 fall-related deaths 10. Risk factors for falls among older adults include age, medications and comorbidities, gait and balance disorders, functional impairment, and cognitive impairment 11,12. Among PWH, HIV-related risk factors including ART, toxicity of prior ART, and HIV-1 replication may further contribute 13,14. Two separate studies among PWH have also suggested that geographic location might be a risk factor for falls 13,15. In the Women's Interagency HIV Study (WIHS), a study of risk factors for falls in women with and without Interagency HIV Study (WIHS), a study of risk factors for falls in women with and without HIV, significant differences in fall occurrences were seen between study sites, with a higher prevalence of falls in the San Francisco site compared to the New York City site 15. Investigators hypothesized that the differences observed might have been due to reasons such as mode of transportation, weather conditions, seasonality, or physical activity 15. Similarly, in the Multicenter AIDS Cohort Study (MACS), the odds of a fall were twice as high in the Chicago and Pittsburgh sites compared to the Baltimore site, and lowest in the Los Angeles site.
|
|
| |
| |
|
|
|