| |
HIV CVD Guidelines - 2019 - Characteristics, Prevention, and Management of Cardiovascular Disease in People Living With HIV: A Scientific Statement From the American Heart Association
|
| |
| |
Download the PDF here
June 2019 Circulation
Matthew J. Feinstein, MD, MSc, FAHA, Chair, Priscilla Y. Hsue, MD, Vice Chair, Laura A. Benjamin, PhD, Gerald S. Bloomfield, MD, MPH, FAHA, Judith S. Currier, MD, Matthew S. Freiberg, MD, MSc, Steven K. Grinspoon, MD, Jules Levin, MS, Chris T. Longenecker, MD, FAHA, Wendy S. Post, MD, MS, and On behalf of the American Heart Association Prevention Science Committee of the Council on Epidemiology and Prevention and Council on Cardiovascular and Stroke Nursing; Council on Clinical Cardiology; and Stroke Council
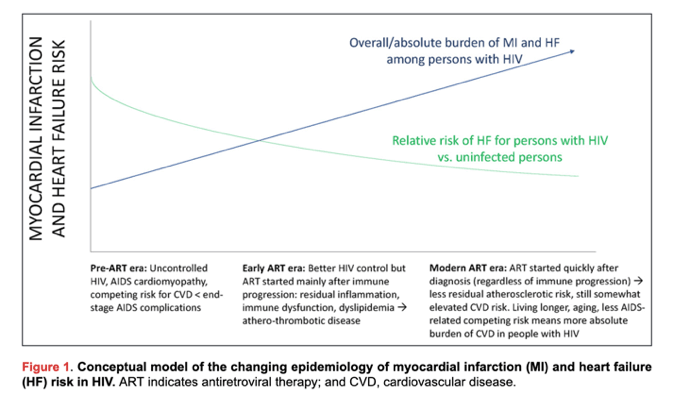
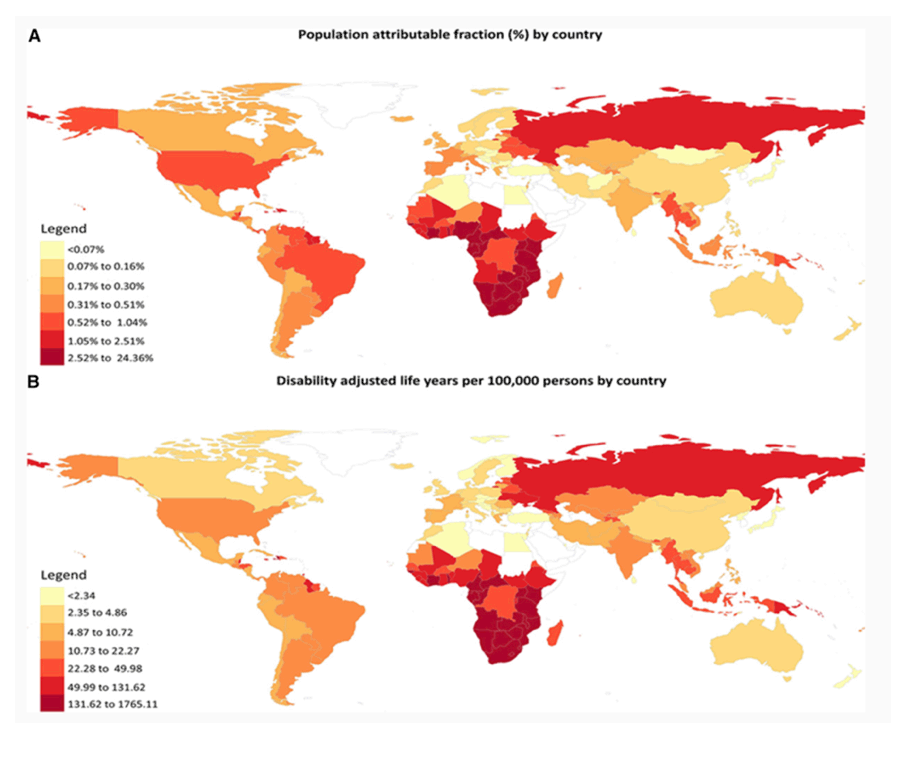
With contemporary antiretroviral therapy (ART), people living with HIV (PLWH) are living longer1 and experiencing a rising burden of cardiovascular diseases (CVDs).2,3 Relative risks of various CVD manifestations are generally 1.5- to 2-fold greater for PLWH compared with uninfected individuals.4 Although the relative risk has decreased with effective ART, there is a large and rising absolute burden of CVD among PLWH (conceptual model in Figure 1).2–4 In a meta-analysis of 793 635 individuals with a total of 3.5 million person-years of follow-up, the global burden of HIV-associated CVD tripled over the past 2 decades and accounted for 2.6 million disability-adjusted life-years per year, with the greatest impact in Sub-Saharan Africa and the Asia-Pacific regions (Figure 2).4 PLWH have an excess risk of myocardial infarction (MI),5,6 ischemic stroke,7,8 heart failure (HF),9,10 pulmonary hypertension,11,12 and venous thrombosis.13,14 Underlying mechanisms likely include an interplay among traditional risk factors, HIV-specific factors (eg, chronic immune activation/inflammation),15,16 ART-related dyslipidemia and other metabolic comorbidities,17,18 behavioral factors (eg, smoking),5,19 and disparities in access to or receipt of care.20–22
Abstract
As early and effective antiretroviral therapy has become more widespread, HIV has transitioned from a progressive, fatal disease to a chronic, manageable disease marked by elevated risk of chronic comorbid diseases, including cardiovascular diseases (CVDs). Rates of myocardial infarction, heart failure, stroke, and other CVD manifestations, including pulmonary hypertension and sudden cardiac death, are significantly higher for people living with HIV than for uninfected control subjects, even in the setting of HIV viral suppression with effective antiretroviral therapy . These elevated risks generally persist after demographic and clinical risk factors are accounted for and may be partly attributed to chronic inflammation and immune dysregulation. Data on long-term CVD outcomes in HIV are limited by the relatively recent epidemiological transition of HIV to a chronic disease. Therefore, our understanding of CVD pathogenesis, prevention, and treatment in HIV relies on large observational studies, randomized controlled trials of HIV therapies that are underpowered to detect CVD end points, and small interventional studies examining surrogate CVD end points. The purpose of this document is to provide a thorough review of the existing evidence on HIV-associated CVD, in particular atherosclerotic CVD (including myocardial infarction and stroke) and heart failure, as well as pragmatic recommendations on how to approach CVD prevention and treatment in HIV in the absence of large-scale randomized controlled trial data. This statement is intended for clinicians caring for people with HIV, individuals living with HIV, and clinical and translational researchers interested in HIV-associated CVD.
In the absence of robust data on the adjunctive value of subclinical imaging and biomarker levels for ASCVD risk stratification among PLWH, it is reasonable to consider selected ASCVD risk enhancers identified in the 2018 ACC/AHA cholesterol clinical practice guidelines as likely ASCVD risk enhancers in HIV (Figure 4).202 These include early family history of MI or stroke (men, age <55 years; women, age <65 years), persistently elevated LDL-C ≥160 mg/dL (≥4.1 mmol/L), chronic kidney disease, preeclampsia or premature menopause, subclinical atherosclerosis on imaging (including CAC), and high levels of selected biomarkers associated with elevated ASCVD risk independently of traditional risk factors (Lp(a) [lipoprotein(a)], hsCRP, and apoB [apolipoprotein B]).202
The presence and extent of subclinical atherosclerosis can be used to refine CVD risk, especially in those considered to be at intermediate risk .19 CAC, measured from noncontrast CT scans, is a potent predictor of coronary heart disease events and has been studied extensively in the general population.20 However, assessment of CAC alone may not reflect underlying coronary artery disease among PLWH because they have more noncalcified plaque than uninfected individuals, and this can be detected only with coronary CT angiography.161CT angiography is not recommended for screening in asymptomatic individuals. The ability of CAC to discriminate risk for coronary heart disease events in PLWH has not been determined; however, those with CAC (particularly if extensive) can be presumed to be at elevated risk. Carotid IMT is also a predictor of future MI and stroke in the general population221 and has been associated with mortality in HIV.222,223
Primary prevention to reduce the risk of ASCVD is an important goal for PLWH. Statins significantly reduce CVD events in patients without HIV with increased inflammation and low levels of LDL-C.240 As discussed, PLWH often present with normal LDL but increased systemic and arterial inflammation72 and persistent immune activation despite successful ART.241 Traditional CVD risk factors, particularly smoking, are also more common and should be targeted in HIV.242
Statin use in HIV is complicated by potential drug interactions, although newer statin and ART therapies appear to have more benign drug-drug interaction profiles.243 Potent cytochrome P450 (CYP) inhibitors such as ritonavir and cobicistat interact with specific statins with significant CYP metabolism.244 Simvastatin and lovastatin are extensively metabolized by the CYP system and can have levels increased >500% when coadministered with CYP inhibitors; accordingly, they should be avoided in HIV.244–246 Pravastatin and pitavastatin are least likely to interact with ART because of minimal CYP metabolism, whereas atorvastatin and rosuvastatin, the 2 highest-intensity statins, with LDL-C lowering of >50% at the highest commonly prescribed doses, have modest interactions with ART.244,245 A comprehensive guide to HIV medications and drug-drug interactions may be found online.247
To address this knowledge gap, the National Institutes of Health launched REPRIEVE, a randomized, placebo-controlled, 7,500-person global trial to test a primary prevention strategy in HIV.261,262 REPRIEVE includes patients at low to moderate risk and assesses whether treatment with pitavastatin will prevent adjudicated major adverse cardiovascular events. REPRIEVE will also assess the degree to which changes in lipids, immune activation, and inflammation contribute to this effect. Furthermore, little is known about the differential effects of statins in women with HIV, but immune activation is higher among women.159 This knowledge gap is being investigated in REPRIEVE, which has enrolled a high percentage of female PLWH.
Although aggressive secondary ASCVD prevention measures are indicated for PLWH, uptake has not been consistent. Compared with uninfected individuals, PLWH are less frequently prescribed high-intensity statin after acute coronary syndrome (15% versus 45%), and LDL reduction 6 months after the acute coronary syndrome event is lower.284
PCSK9 inhibitors are monoclonal antibodies with minimal significant drug-drug interactions identified thus far that reduce LDL-C by ≈60% even in the setting of high-intensity statin therapy.292 Two PCSK9 inhibitors are approved by the US Food and Drug Administration for individuals with heterozygous familial cholesterolemia or clinical ASCVD on maximally tolerated statins who require additional LDL-C lowering. Among uninfected people with ASCVD, PCSK9 inhibitor therapy in addition to statin therapy reduced clinical events by 15% (P<0.001).292
Lifestyle Optimization
As in the general population,200–202 adherence to a healthy lifestyle is an essential first step for primary and secondary prevention of CVD among PLWH. Smoking cessation is of paramount importance given the high prevalence of smoking among PLWH143 and the clear role of smoking in atherosclerosis and MI.144,145 (An extensive library of resources for patients and providers to approach smoking cessation can be found online.227,228) Limiting alcohol consumption is likewise important given the potential disproportionate contribution of alcohol to CVD in HIV.19 Regular physical activity is also an essential aspect of lifestyle optimization in HIV given the associations of physical inactivity with poor health and adherence in HIV and, conversely, the improvement in inflammation and cardiometabolic health with increasing physical activity in HIV.226,234,235
Although it is clear that heavy alcohol consumption has adverse effects on CVD and other disease end points,229there is debate about whether a "healthy" level of alcohol consumption exists; some large analyses suggested a cardioprotective effect of light to moderate alcohol consumption (<100 g/wk [<7 drinks/wk]),230,231 whereas others found no benefit and perhaps elevated HF and stroke risks for light to moderate alcohol consumption.232,233
No amount of alcohol is good for the heart, new report says, but critics disagree on science - (01/20/22)
One Alcohol Drink A Day Increases Cancers Risk - (01/20/22)
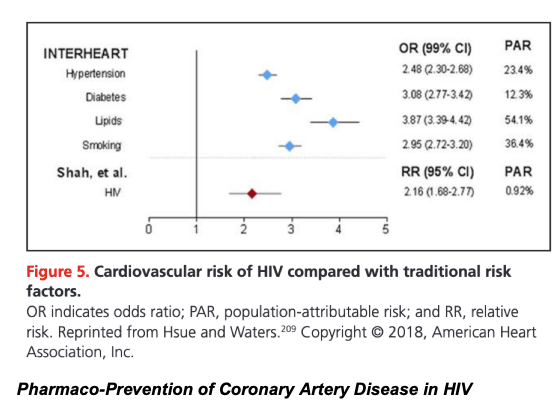
Traditional ASCVD risk factors such as age, diabetes mellitus, current smoking, hypertension, and dyslipidemia are associated with elevated ASCVD risk among PLWH just as they are in the general population.5,24,34 Similar to traditional ASCVD risk factors, HIV infection is associated with elevated ASCVD risk (Figure 5),209 particularly for PLWH with low current or nadir CD4 count (especially <200 cells/mm3)5,25,26,210 or a history of sustained untreated HIV.5,210
Risk Factors
• HIV infection is associated with metabolic complications, including dyslipidemia, insulin resistance, and body composition changes, which can contribute to CVD.
• Insulin resistance and diabetes mellitus are also seen with increasing frequency in HIV.104 Prevalence estimates range up to 26% and 47% in Sub-Saharan Africa for diabetes mellitus and prediabetes mellitus, respectively.99
• Diabetes mellitus has been linked to ASCVD in HIV such that PLWH with diabetes mellitus have a 2.4-fold increased risk of coronary heart disease events.106
• Body composition changes are common in HIV. Patients presenting in the initial era of ART often demonstrated relative loss of subcutaneous fat and gain in abdominal visceral fat.107
• The changes in fat distribution were often heterogeneous and frequently were associated with insulin resistance and deposition of ectopic adipose in the liver and muscle. Multiple factors contributed to these changes, including effects of ART. Use of specific thymidine NRTIs is associated with subcutaneous fat loss and deposition of ectopic adipose tissue in the liver and muscle, as well as arterial inflammation.108 Early PI therapy was associated with increased abdominal fat gain.
• In the modern ART era, this phenotype has changed, and recent work has focused on dysfunctional subcutaneous fat, related in part to the effect of HIV on peroxisome proliferator-activated receptor-γ and Dicer, as well as other mechanisms.109,110 With increasingly effective ART, gains in both subcutaneous and visceral fat are often seen with the initiation of ART, regardless of regimen,111 and rates of generalized obesity are increasing among PLWH.112 Changes in body composition, including excess visceral adipose tissue, have been linked to overall mortality.113 These changes have been associated with increased coronary plaque, including both noncalcified and calcified plaque.114,115
• Other traditional risk factors, including hypertension and cigarette smoking, play an important role in the pathogenesis of ASCVD in PLWH. A meta-analysis of 63 554 participants from studies published from 2011 to 2016 estimated hypertension prevalence to be 35% for PLWH on ART and 13% for ART-naïve PLWH.136Although untreated HIV is typically associated with lower blood pressure, resulting perhaps from uncontrolled inflammation and periseptic states of vascular permeability,136–138 studies are inconsistent on whether individuals with treated HIV have a higher prevalence of hypertension compared with uninfected individuals.139–141
• On a population-level scale, smoking may be the most important modifiable CVD risk factor among PLWH. Smoking is highly prevalent among PLWH (42% were current smokers and 20% were former smokers in a nationally representative US sample143) and is strongly associated with coronary artery plaque and MI.144,145
• Heavy alcohol use, although not generally considered a traditional atherosclerotic risk factor, may contribute disproportionately to CVD among PLWH.19 In addition to (and often in conjunction with) substance use disorders, mood and anxiety disorders are quite common among PLWH146–148 and may contribute to elevated CVD risk (including MI149 and HF36). PLWH also have low levels of physical and cardiorespiratory fitness, which are associated with vascular dysfunction, inflammation, and risk for CVD, as well as all-cause mortality, in patients with HIV (and in the general population).150–153
• Although it is clear that heavy alcohol consumption has adverse effects on CVD and other disease end points,229 there is debate about whether a "healthy" level of alcohol consumption exists; some large analyses suggested a cardioprotective effect of light to moderate alcohol consumption (<100 g/wk [<7 drinks/wk]),230,231 whereas others found no benefit and perhaps elevated HF and stroke risks for light to moderate alcohol consumption.232,233
No amount of alcohol is good for the heart, new report says, but critics disagree on science - (01/20/22)
One Alcohol Drink A Day Increases Cancers Risk - (01/20/22)
|
|
| |
| |
|
|
|