| |
CDC - HIV+ Black Adults More Social Vulnerabilty; Higher Mortality; More Commorbidites
|
| |
| |
Download the PDF here

Media Statement
For immediate release: Thursday, Feb. 3
Contact: National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention
(404) 639-8895 | NCHHSTPMediaTeam"at"cdc.gov
Despite overall progress in reducing HIV transmission in the United States, HIV continues to affect some groups more than others due to longstanding and ingrained barriers. Black or African American (hereafter referred to as Black) people account for a higher proportion of new HIV infections, compared to other races and ethnicities. Black people accounted for 13% of the U.S. population but 40% of people with HIV in 2019, according to CDC estimates.
HIV disparities can and must end. Racism, longstanding systemic inequities, social and economic marginalization, residential segregation, unequal reach of HIV prevention and treatment, and higher levels of HIV in some communities are among the factors that have contributed to these troubling and persistent disparities.
A CDC report published today, ahead of National Black HIV/AIDS Awareness Day on February 7, finds 52% of Black adults with diagnosed HIV resided in areas in the country with higher Social Vulnerability Index (SVI) scores-often residentially segregated communities comprised predominately of Black people. The report underscores the continuing, urgent need to address the social determinants that contribute to disparities and better deliver HIV prevention and care to people who need it most.
A separate report by New York State health officials and CDC found, in the state of New York, that COVID-19 vaccination coverage was lower among adults with HIV than the general adult population; and that Black people with HIV were among the groups with the lowest COVID-19 vaccination coverage. People engaged in care were more likely to be vaccinated than people not engaged in HIV care. The report emphasizes the need for interventions to help people with HIV get into and stay in HIV care, get vaccinated, and stay up-to-date on COVID-19 vaccines according to CDC guidelines.
To achieve health equity and end the HIV epidemic, the nation must overcome barriers that, for far too long, have stood between some people and highly effective HIV prevention and treatment tools. CDC is working with partners on many fronts, and through the federal Ending the HIV Epidemic in the U.S.external icon initiative, to focus resources to communities that could most benefit from key, science-based HIV treatment and prevention strategies that are scaled up in innovative ways to reach populations equitably.
Please attribute the following quote to Demetre Daskalakis, MD, MPH, Director of CDC's HIV Prevention Program
"Despite tremendous progress in reducing HIV transmission since the height of the epidemic, HIV continues to disproportionately affect Black people in America. HIV disparities are not inevitable and can be addressed. The advanced, highly effective HIV prevention and treatment tools and COVID-19 vaccines that that have been accessed by some must be accessible to all. While there is no simple solution to equity, our nation must finally tear down the wall of factors-systemic racism, homophobia, transphobia, HIV-related stigma, and other ingrained barriers-that still obstructs these tools against HIV and COVID-19 from equitably reaching the people who could benefit from them."
----------------------------------------------

Weekly / February 4, 2022
Summary
What is already known about this topic?
In 2018, Black persons accounted for nearly one half of all new diagnoses of HIV infection in the United States. The annual diagnosis rate among Black persons was four times the rate among all other racial or ethnic groups combined.
What is added by this report?
Rates of new HIV diagnoses among Black adults were higher in communities with the highest social vulnerability. Approximately one half of Black adults with diagnosed HIV reside in the upper quartile of socially vulnerable U.S. Census tracts in the United States.
What are the implications for public health practice?
Intensified prevention efforts are needed to reduce HIV transmission among Black persons in communities with the highest social vulnerability.
During 2018, Black or African American (Black) persons accounted for 43% of all new diagnoses of HIV infection in the United States (1). The annual diagnosis rate (39.2 per 100,000 persons) among Black persons was four times the rate among all other racial/ethnic groups combined, indicating a profound disparity in HIV diagnoses (1,2). Community-level social and structural factors, such as social vulnerability, might help explain the higher rate of HIV diagnoses among Black persons. Social vulnerability refers to the potential negative health effects on communities caused by external stresses (3). CDC used National HIV Surveillance System (NHSS)* and Social Vulnerability Index (SVI)†data to examine the association between diagnosed HIV infections and social vulnerability among Black adults aged ≥18 years. Black adults in communities in the highest quartile of SVI were 1.5 times (rate ratio [RR] = 1.5; 95% CI = 1.4-1.6) as likely to receive a diagnosis of HIV infection as were those in communities in the lowest quartile. Because of a history of racial discrimination and residential segregation, some Black persons in the United States reside in communities with the highest social vulnerability (4,5), and this finding is associated with experiencing increased risk for HIV infection. The development and prioritization of interventions that address social determinants of health (i.e., the conditions in which persons are born, grow, live, work, and age), are critical to address the higher risk for HIV infection among Black adults living in communities with high levels of social vulnerability. Such interventions might help prevent HIV transmission and reduce disparities among Black adults.
During 2018, the rate of new HIV diagnoses per 100,000 population among Black adults was higher in communities with the highest SVI (Quartile 4; 52.1) than in communities with the lowest SVI (Quartile 1; 33.7). Approximately one half (52.2%) of Black adults with newly diagnosed HIV infection resided in the most socially vulnerable census tracts, which are often racially segregated communities comprising predominately Black persons (5,7). The social and economic marginalization of Black persons, including residential segregation, is correlated with factors associated with higher social vulnerability and higher rates of HIV diagnosis (7). Residential segregation contributes to higher rates of HIV diagnosis and poor health outcomes among Black persons because isolation limits access to important resources and affects neighborhood quality; populations residing in lower-income and relatively more isolated areas experience vulnerability to negative health outcomes, including HIV infection (5,7,8). In addition, persons lacking basic economic and social support in communities with higher social vulnerability are more likely to be overwhelmed by routine life demands (e.g., addressing issues with unstable housing or unable to take time off from minimum-wage job because of lack of paid leave (9). Although social vulnerability does not explain all the disparity in HIV diagnosis (5), Black adults in communities with the highest social vulnerability might find it harder to obtain HIV prevention and care services because of various factors, such as poverty, limited access to health care, substance use disorder, transportation to services, housing insecurity, HIV stigma, racism, discrimination, and high rates of sexually transmitted diseases (7,10). These factors directly and indirectly affect the health of Black adults with HIV infection and those who experience risk for infection (10).
------------------------------------
Excess Black Deaths PLWH & Higher Morbidity- (12/23/21)
HRSA Aging/HIV Medicare Paper - "need for personalized care & maximizing functional status....training medical professionals....increased coordination & integration of services, geriatric services " - (09/08/21)
"we found that older people with HIV have a higher overall hazard of mortality as well as a higher odds of having depression, chronic kidney disease, COPD, osteoporosis, colorectal cancer, lung cancer, hypertension, ischemic heart disease, diabetes, chronic hepatitis, and end-stage liver disease compared to those without HIV ......minorities and dual Medicaid enrollees overall had higher hazards of mortality as well as higher odds and incidence of many conditions"
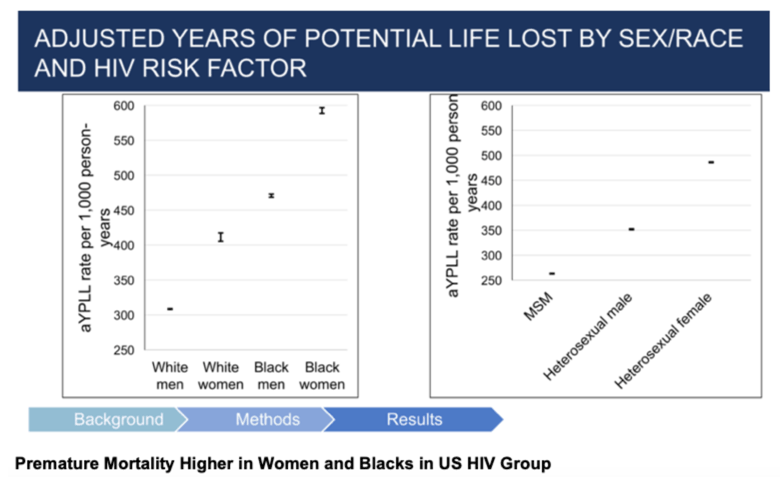
Sex and race disparities in premature mortality among people with HIV: a 21-year observational cohort study - Premature Mortality Higher in Women and Blacks in US HIV Group- (10/01/21)
|
|
| |
| |
|
|
|